Clinical Skills
Discover guidance for assessing patients, diagnostic testing, and surgical procedures through expert-led articles and videos. Perfect for general practitioners, veterinary students, and residents looking to refine their skills.
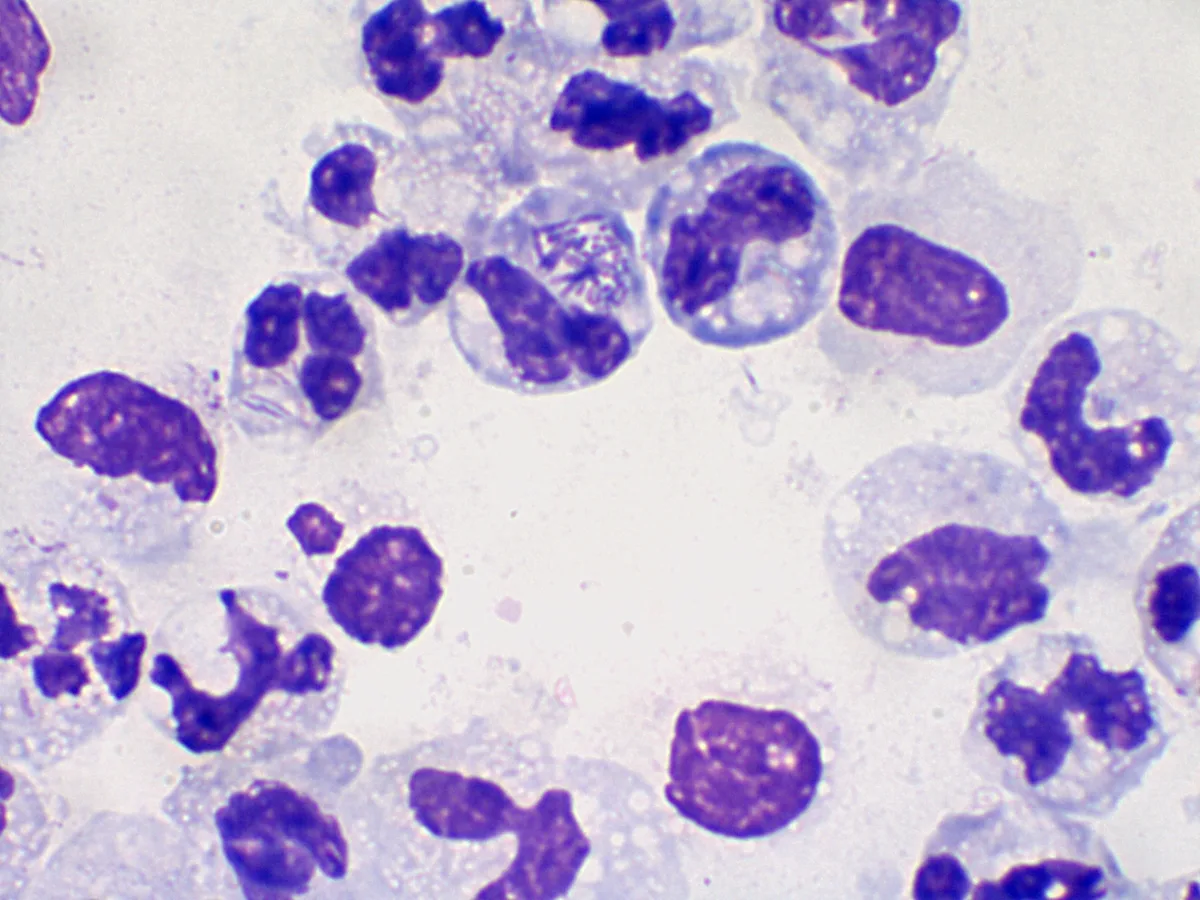
Biomarkers help diagnose, monitor, and predict response to therapy across a range of conditions. This article focuses on acute-phase proteins, which are key indicators of inflammation that every small animal practitioner should know how to interpret and apply.
Topics In Clinical Skills


New in Clinical Skills
Get more clinical guidance with Standards of Care™
From the team that brings you Clinician’s Brief, extend your knowledge with expert-written, peer-reviewed diagnostic and treatment guidance as well as pet owner education and all the reliable drug information you love in Plumb’s.