Clinical Skills
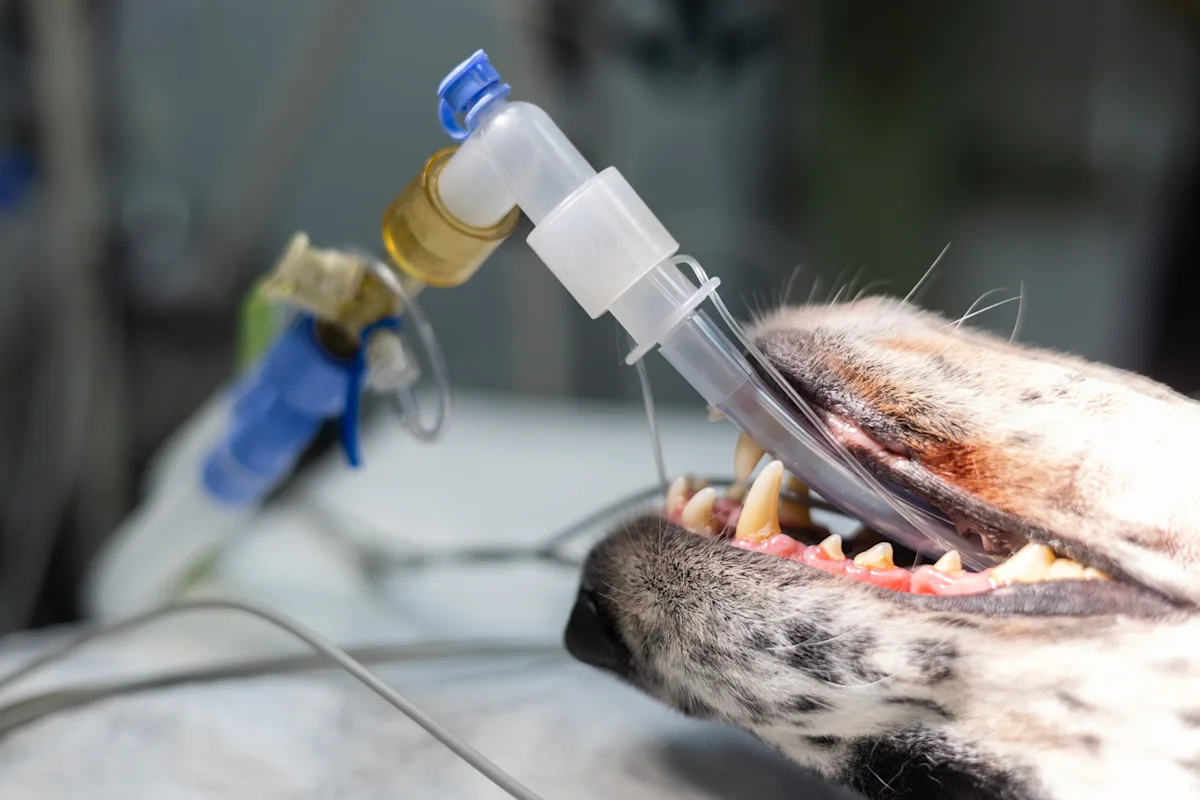
Discover guidance for assessing patients, diagnostic testing, and surgical procedures through expert-led articles and videos. Perfect for general practitioners, veterinary students, and residents looking to refine their skills.
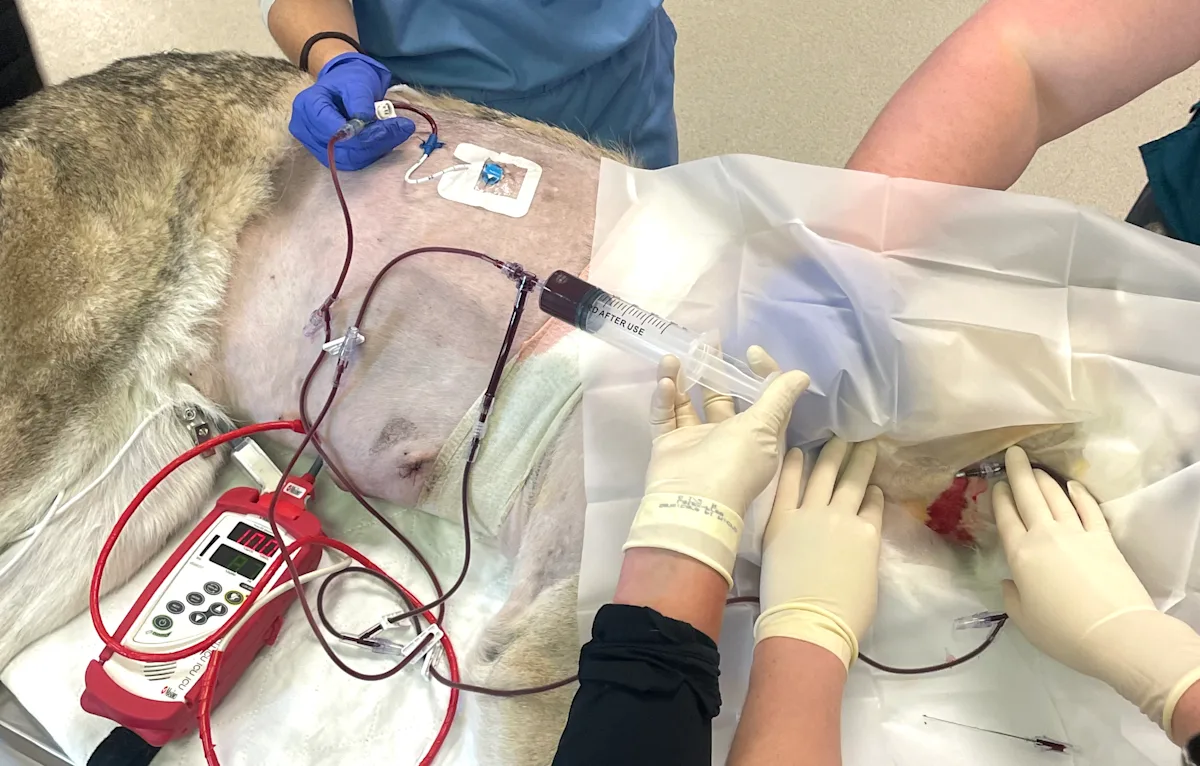
Autotransfusion can be a lifesaving option when donor blood is unavailable or incompatible. This step-by-step guide reviews indications, equipment, technique, and key precautions for safe use.
Topics In Clinical Skills
Featured in Clinical Skills
Poll
Quiz
New in Clinical Skills
Sponsored byHill's Pet Nutrition
1h:07m:24s
Ep. 357
Sponsored byPRN® Pharmacal
Sponsored byPRN® Pharmacal
Sponsored byCeva Animal Health, LLC
26m:58s
Ep. 355
Sponsored byHill's Pet Nutrition
Get more clinical guidance with Standards of Care™
From the team that brings you Clinician’s Brief, extend your knowledge with expert-written, peer-reviewed diagnostic and treatment guidance as well as pet owner education and all the reliable drug information you love in Plumb’s.