Practice Life
Explore practical perspectives from peers and experts for navigating the social and professional challenges veterinarians face in the practice and beyond.
18m:06s
Ep. 317
In this episode, Dr. Alyssa and Dr. Beth explore the potential addition of two new specialties to the American Board of Veterinary Specialties and examine how the continued growth of specialized care is transforming the field.
Topics In Practice Life
Poll
Brought to You by Bionote

Quiz
Brought to You by Bionote

New in Practice Life
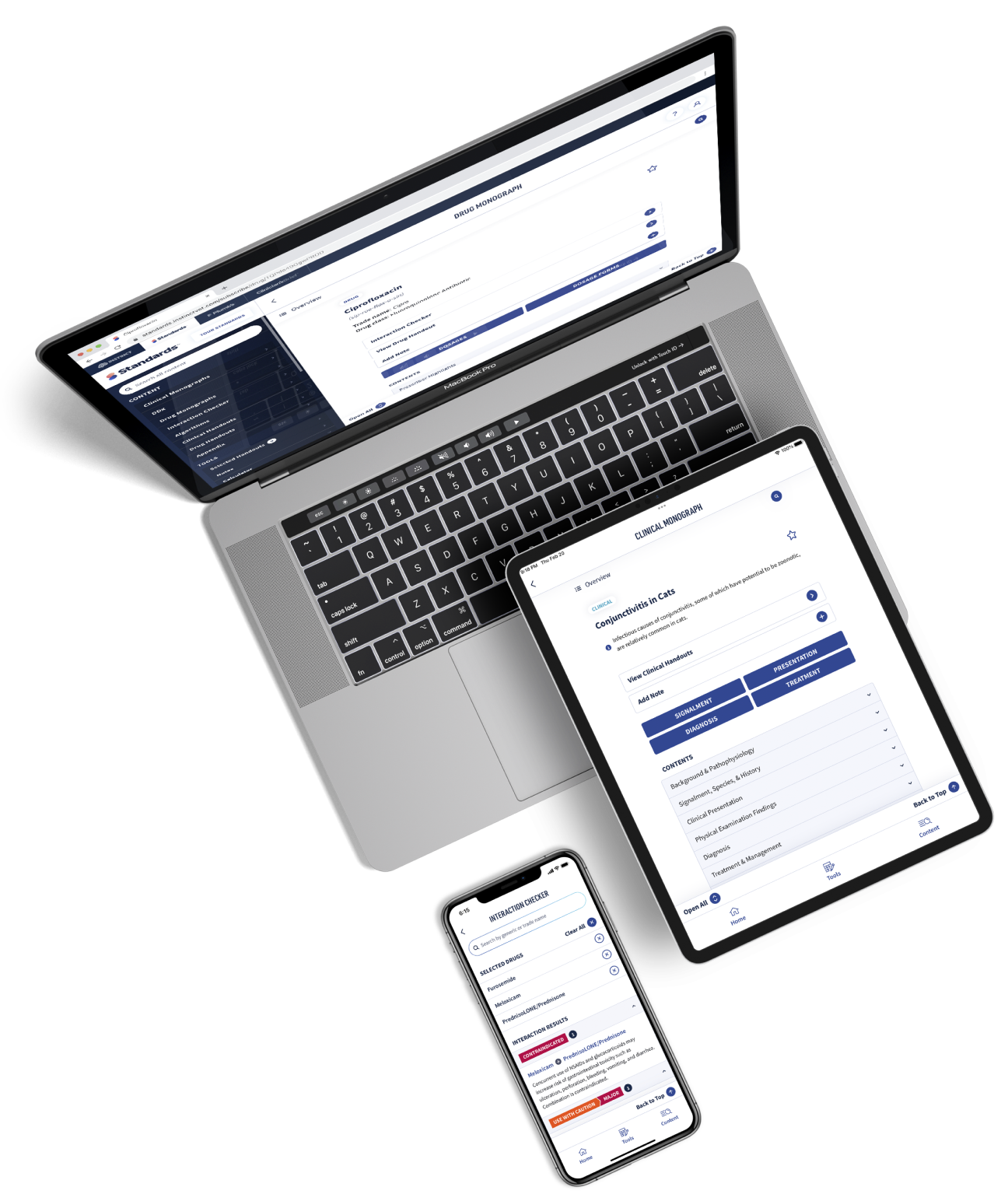
Get more clinical guidance with Standards of Care™
From the team that brings you Clinician’s Brief, extend your knowledge with expert-written, peer-reviewed diagnostic and treatment guidance as well as pet owner education and all the reliable drug information you love in Plumb’s.