Top 6 Conditions Found During Canine Rectal Examination
Christopher R. Lea, DVM, DABVP (Canine & Feline), CCAT, Auburn University
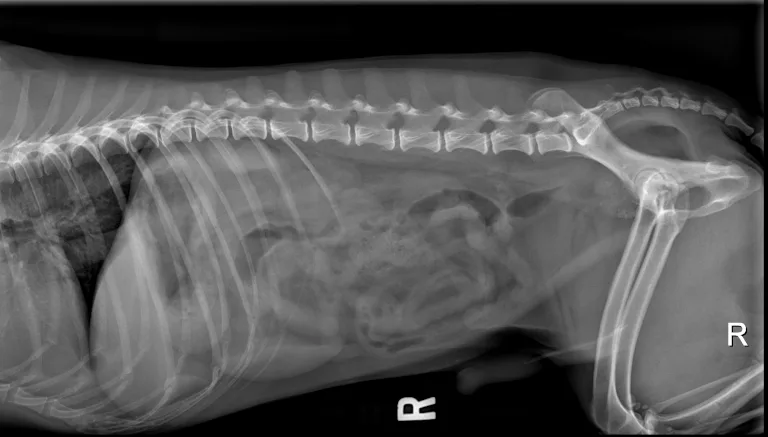
Radiograph of an enlarged and mineralized prostate (arrow) in a dog diagnosed with prostatic carcinoma based on DNA urine testing. Image courtesy of Merrilee Holland, DVM, DACVR
Rectal examination is an important part of the physical examination, especially in aging dogs,1 as detection of clinical diseases and subclinical disorders may otherwise be missed. Patient temperament and size can make rectal examination difficult, and patients with clinical signs of perianal or prostatic disease may require additional care (eg, sedation).
Following are the top disorders identified during rectal examination in dogs, according to the author.
1. Anal Sac Tumors
Anal sacs are sphere-shaped structures on each side of the rectum between the internal and external anal sphincter muscles and are lined with sebaceous and apocrine glands.2 Each sac communicates directly into the rectum with a single duct and expresses a fluidlike material into the stool after defecation and muscle contraction.2
The most common anal sac tumor is apocrine anal gland adenocarcinoma, which comprises ≈17% of all perianal tumors.3,4 Approximately 47% of apocrine anal gland adenocarcinomas are detected incidentally on rectal examination.3 These tumors are more common in spaniels, dachshunds, and German shepherd dogs, as well as in middle-aged to older dogs3; ≈16% to 53% of patients also demonstrate paraneoplastic hypercalcemia.3 Fine-needle aspiration and cytology results are typically suggestive of neuroendocrine-like cells (Figure 1).3 Recommended treatment is surgical removal of the anal sac and any affected lymph nodes after metastatic surveillance.3,4

Fine-needle aspirate from a dog with apocrine anal gland adenocarcinoma. Image courtesy of Pete Christopherson, DVM, PhD, DACVP
2. Nonneoplastic Anal Sac Disease
Nonneoplastic anal sac disease can be categorized as impaction, inflammation with or without infection, or abscessation and is more common in small-breed dogs (<33 lb [15 kg]).5 The cause of nonneoplastic anal sac disease is generally unknown; theories include changes in anal sac secretory activity, obesity, and changes in muscle tone.5,6 Clinical signs include excessive licking and dragging of the perianal region.6
On rectal examination, anal sacs can be thickened on palpation and may be difficult to express. Common treatment includes expression, flushing, and infusion of a corticosteroid/antimicrobial directly into the gland with the patient under sedation.5,6 This treatment can be an effective alternative to oral antibiotics.5
Anal sacculectomy is another treatment option, particularly in chronically recurrent cases, but is a delicate procedure with the potential to damage the anal sphincter muscles and caudal rectal nerve; referral to a board-certified surgeon may therefore be considered.7
3. Lumbosacral Disease
Many conditions (eg, disk protrusion/herniation, thickening of fibrous joint capsules, osseous proliferation of lumbar endplates) can contribute to pain in the lumbosacral area (ie, lumbosacral disease).8,9 Localizing lumbosacral pain that contributes to nerve root compression can be challenging, especially in the absence of other neurologic signs (eg, urinary incontinence, fecal incontinence).8 Deep external lumbar palpation, dorsiflexion of the tail, and rectal examination may aid in localization.8 During rectal examination, digital pressure can be applied dorsally to the lumbosacral spine to examine for pain and discomfort.
Lumbosacral disease is more common in large-breed dogs.8 Radiographs can help rule out other conditions (eg, spondylosis deformans, facet arthritis, disk narrowing); however, MRI is necessary for evaluation of soft tissue pathology (eg, nerve root compression).8,9 Medical and surgical treatment options depend on several factors but should be based on the severity and chronicity of clinical signs.8,9
4. Urethral Neoplasia
Transitional cell carcinoma is the most common neoplasia in the urinary system of dogs.10 These tumors are commonly found at the trigone of the bladder and/or urethra, in which a thickening or mass may be palpable at the pelvic urethra during rectal examination.11 Further diagnostics (eg, abdominal ultrasonography) may be warranted if clinical signs and examination abnormalities are found (Figure 2). Imaging results suggestive of a mass indicate the need for further evaluation with molecular urine testing.12,13

Ultrasound of the urethra (dashed arrow) of a dog with transitional cell carcinoma. A mixed echogenic mass within the lumen of the urethra can be seen (solid arrow). Image courtesy of Merrilee Holland, DVM, DACVR
5. Prostatic Disease
Other organs (eg, prostate in males) may be palpable depending on patient size. Intact males commonly have benign prostatic hypertrophy or bacterial prostatitis. Additional testing (eg, radiography, ultrasonography, urinalysis, urine culture) may be needed. As with transitional cell carcinoma, molecular tests can be submitted for diagnosis of prostatic carcinoma. DNA-based diagnostics are highly sensitive and specific, making these tests noninvasive and useful for diagnosis of transitional and prostatic carcinoma (Figure 3).12,13

Radiograph of an enlarged and mineralized prostate (arrow) in a dog diagnosed with prostatic carcinoma based on DNA urine testing. Image courtesy of Merrilee Holland, DVM, DACVR
6. Miscellaneous Conditions
Dogs presented with clinical signs such as pollakiuria, perianal swelling, or tenesmus require rectal examination.14 Urethral stones, perineal hernias, rectal strictures, hemorrhoids, lymphadenopathy, and neoplasia may also be identified.14
Conclusion
Rectal examination can provide valuable information about the overall health of a patient and be a useful screening tool for a variety of conditions associated with the rectum or vital structures in similar anatomic areas. Sedation may be required to facilitate examination; sedation for another procedure can also provide an effective opportunity to complete the rectal examination.
Listen to the Podcast
Listen as Dr. Lea reviews his checklist for rectal examination findings and shares some of the next steps when you’ve found an abnormality.