Laryngeal Paralysis Diagnosis
Kelley Thieman Mankin, DVM, MS, DACVS (Small Animal), Texas A&M University
Laryngeal paralysis (LP) is an important cause of upper airway obstruction in dogs. It can lead to the inability of the arytenoid cartilages to abduct during inspiration, which may result in dyspnea. Idiopathic acquired laryngeal paralysis is the most common form, but congenital laryngeal paralysis, specific traumatic events, iatrogenic nerve damage, and neoplasia may also be seen.<sup1 sup>
Older, large-breed dogs are most commonly affected with idiopathic acquired laryngeal paralysis. The disease typically manifests around 11 to 12 years of age.2-5 Any breed can be affected, but Labrador retrievers are over-represented.2-5
Idiopathic acquired LP is believed to be part of a polyneuropathy complex.2,3,6 Specifically, idiopathic acquired LP is thought to occur because of degeneration of the recurrent laryngeal nerve, although multiple nerves are affected.
The recurrent laryngeal nerve originates from the vagus nerve and runs a long course; it branches off of the vagus nerve in the thorax and runs up the neck to terminate as the caudal laryngeal nerve in the larynx. It is responsible for innervation of most of the laryngeal muscles, including the cricoarytenoideus dorsalis muscle; contraction of this muscle causes abduction of the arytenoid cartilages.
Signs
The most dramatic clinical signs occur secondary to degeneration of the recurrent laryngeal nerve. Many dogs affected by idiopathic laryngeal paralysis are presented for acute onset of dyspnea, but most nerves in the body are typically affected so a variety of signs can be present.2,3 In addition to respiratory signs, animals affected by idiopathic laryngeal paralysis may have difficulty rising, proprioceptive deficits, dysphagia, esophageal dysmotility, aspiration pneumonia, and muscle atrophy.2,3
Progression of the disease is often slow, and subtle clinical signs may go unnoticed. Many affected dogs eventually have an episode of dyspnea, stridorous breathing, or cyanosis. Excitement or exercise may exacerbate clinical signs, and the dog may require emergency treatment.
A physical examination and thorough palpation of the neck can detect any masses that may be present that would cause clinical signs similar to those associated with LP.
Examination & Evaluation
In a stable dog with suspected LP, a thorough evaluation should be performed. A physical examination and thorough palpation of the neck can detect any masses that may be present that would cause clinical signs similar to those associated with LP. A complete neurological examination should be performed to evaluate for signs of polyneuropathy, and a minimum database should be established before administration of anesthetic agents.
Related Article: The Case: Acute Respiratory Distress
Related Article: Respiratory Distress: Diagnosis & Treatment at a Glance
The work-up should include a CBC, serum chemistry panel, urinalysis, and thoracic radiographs. CBC and serum chemistry panel are often normal but are important in identifying concurrent disease in older dogs. Radiographs of the neck may be indicated if a neck mass is suspected or to rule out other causes of dyspnea. Thoracic radiographs are important to detect conditions that may cause LP (eg, thoracic masses damaging the vagus or recurrent laryngeal nerves), or concurrent diseases that may be present.
Dogs with LP are also predisposed to aspiration pneumonia and megaesophagus, so a preoperative diagnosis of megaesophagus—if present—is imperative, as it will likely change the surgical recommendations.
If megaesophagus is present on thoracic radiography, the dog is likely to develop aspiration pneumonia. A cricoarytenoid lateralization procedure is not recommended in dogs with megaesophagus, as the presence of megaesophagus after cricoarytenoid lateralization has been associated with a high rate of complications and death.7
Instead, a tracheostomy may be considered to relieve the upper airway obstruction. If megaesophagus is not present on thoracic radiography, an esophagram may be considered. Dogs with idiopathic laryngeal paralysis can also have or can develop esophageal dysfunction.2 Dogs that have poor esophageal motility are more likely to develop aspiration pneumonia postoperatively.2
Most dogs will develop clinical signs of generalized neuropathy within 1 to 2 years.2,3 Therefore, it is important that owners know LP is a progressive disease.
Neurologic status should be thoroughly discussed with the client, who must be aware that LP is a progressive disease. Some dogs may be presented for LP without clinical signs of neurologic dysfunction, but most dogs will develop clinical signs of generalized neuropathy within 1 to 2 years.2,3
Diagnosis
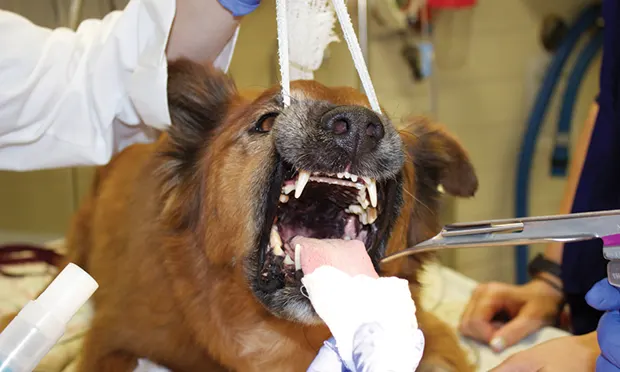
Following the pre-anesthetic work-up, a laryngeal examination is necessary to diagnose LP. Completing a diagnostic laryngeal examination and minimizing false positives is important but difficult.
Direct observation of the larynx per os is an effective diagnostic tool.8 Laryngeal examination would ideally be performed in a conscious patient because of the effect of anesthetic agents on laryngeal function; however, this method is often not feasible in a conscious patient. Instead, a light plane of anesthesia is required.
Anesthetic premedication is necessary in some dogs. Acepromazine or butorphanol are good options for premedication, as laryngeal function is maintained with these drugs.9 After premedication, the anesthetic agent is administered. Administration of different anesthetic agents may have varying effects on laryngeal motion.
Although thiopental was historically regarded as the best anesthetic agent for evaluation of laryngeal function,9 it is no longer manufactured; different anesthetic agents are now recommended.
Currently, many dogs are administered propofol slowly, to effect,10 to undergo laryngeal examination. If the dog becomes overly sedate, the clinician can wait until the dog is at a lighter plane of anesthesia and attempts to swallow or gag. The clinician must know which phase of respiration is occurring to accurately diagnose LP.
In some dogs, paradoxical motion of the arytenoid cartilages may appear to be normal laryngeal motion. In dogs with paradoxical motion, the arytenoid cartilages are adducted during inspiration by the negative pressure in the airway. At exhalation, the arytenoids are forced open by the air rushing past. Therefore, the arytenoid cartilages appear to be moving, but their motion is the opposite of what would be expected in a normal dog.
An assistant can help the clinician to identify paradoxical motion by calling out the dog’s inspirations. Doxapram can be administered to stimulate maximal respirations in dogs with absent or shallow respirations.<sup11 sup>
Related Article: Acute Respiratory Distress: The Blue Patient
Related Article: Respiratory Support for Acute Intensive Care
Step-by-Step: Laryngeal Paralysis Diagnosis
What You Will Need
Examination gloves
Anesthetic drugs/propofol ± pre-anesthetic agents
Doxapram
Laryngoscope
Assistant
Gauze (4 × 4 in [101 x 101 mm]) for holding tongue
Long-handled, cotton-tipped applicator
Tongue depressors
Endotracheal tube for intubation
Oxygen
Patent IV catheter
Roll gauze
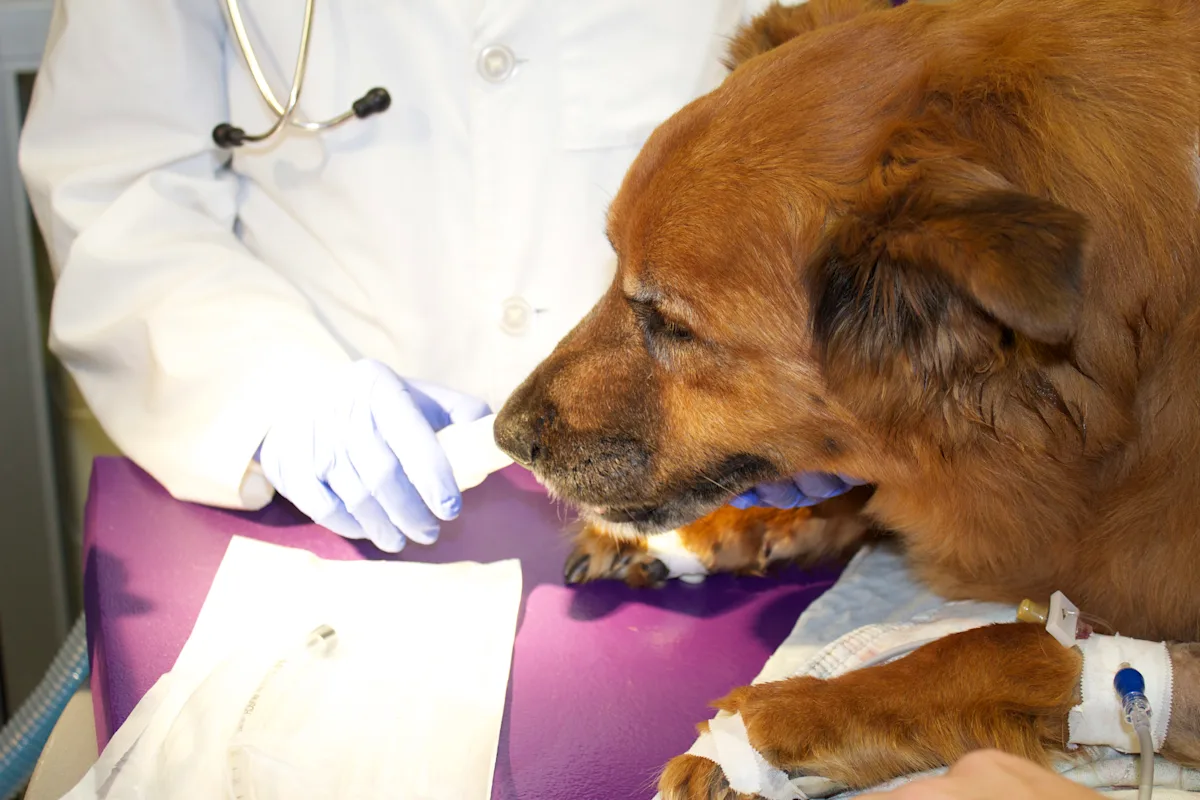
STEP 1
Place patient in sternal recumbency. Administer flow-by oxygen for pre-oxygenation. The flow-by oxygen should be administered for approximately 5 minutes before administration of the anesthetic agent. Check the IV catheter for patency. If patent, administer the anesthetic agent to effect.
Diagnostic Insights
Be patient. The dog must be in a light plane of anesthesia to avoid misdiagnosis of LP.
Tell the assistant to indicate when the dog inspires. This will help the identification of paradoxical motion of the larynx (and avoid false-negative results).
Elevate the dog’s head by gauze under the maxilla, not by putting pressure on the ventral aspect of the larynx.
Have an endotracheal tube nearby. Some dogs require intubation due to poor respirations or paradoxical laryngeal motion.
Every time an animal is intubated, take a few seconds to watch arytenoids move to become familiar with what is normal and to better recognize what is abnormal.
LP = laryngeal paralysis