Zinc-Responsive Dermatosis in Dogs
Darren Berger, DVM, DACVD, Iowa State University
Zinc is a vital micronutrient, and mammalian metabolic zinc requirements must be met via constant dietary intake. It is a fundamental component of many metalloenzymes involved in cellular functions, metabolic pathways, nucleic acid synthesis, and protein synthesis. Zinc is an essential component for cell replication, specifically in rapidly dividing cells required for regeneration of intestinal mucosa, wound healing, and the continual turnover of epithelial cells in skin, hair, and claws.1,2
How should zinc-responsive dermatosis be diagnosed and treated in canine patients?
Zinc-responsive dermatosis is an uncommon skin disease in dogs and is normally associated with 1 of 2 recognized clinical syndromes.
Syndrome 1 is seen almost exclusively in Nordic breeds (eg, Siberian husky, Alaskan malamute). It is considered hereditary and arises in part due to a diminished capability to absorb zinc from the GI tract.3
Syndrome 2 is seen in rapidly growing, usually large-breed puppies receiving either a diet deficient in zinc, a diet high in plant phytates, or a diet excessively supplemented with other minerals (specially calcium). Phytates and other minerals can impair zinc absorption from the GI tract. Water with elevated iron levels can also be a potential source of impaired zinc absorption.2
Clinical Signs
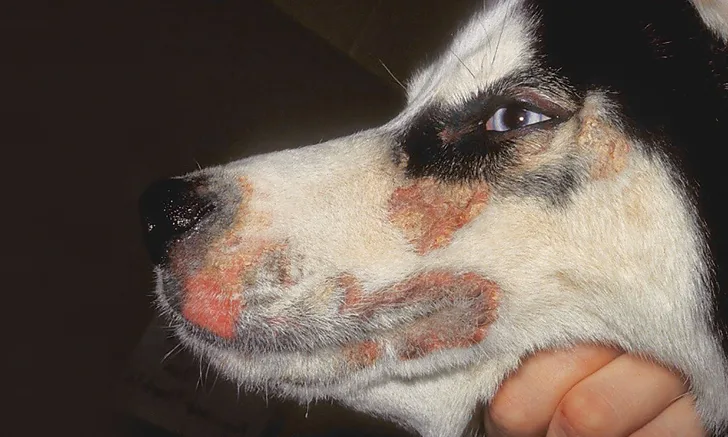
Cutaneous lesions are similar for both syndromes, but those associated with Syndrome 2 are typically more severe and occur at a younger age. Clinical signs usually develop in early adulthood, with the mean age of onset ≈3 years. Initial lesion development, however, has been identified in dogs as old as 11 years.4 Cutaneous lesions exhibit erythema, variable degrees of alopecia, scaling, crusting, and lichenification, which are commonly symmetric and most often affect the head (periocular, perioral, and pinnae; Figures 1 and 2).

FIGURE 1
Symmetric periocular hypotrichosis, erythema, and crusting in a 1.5-year-old male Siberian husky with zinc-responsive dermatosis. Image courtesy of J.O. Noxon, DVM, DACVIM, Iowa State University
Other areas often involved include pressure points (eg, elbows, stifles), other mucocutaneous junctions (eg, prepuce, vulva, anus), scrotum, and distal extremities (Figure 3). The paw pads and nasal planum may also become hyperkeratotic (Figure 4). Pruritus is commonly associated with the condition and may result from secondary bacterial or Malassezia spp infection. Exacerbation of clinical signs has been observed with periods of stress, estrus cycle, and time of year (worse in winter months).2
Differential Diagnoses
Diseases that clinically resemble zinc-responsive dermatosis in dogs can be differentiated by age at onset of clinical signs. Demodicosis, dermatophytosis, and pyoderma are the most likely differentials in younger patients. As the age of onset of clinical signs increases, additional possibilities (eg, pemphigus foliaceus, cutaneous lupus variants, hepatocutaneous syndrome) should be considered.
Diagnosis
Diagnosis should be made based on presenting signalment, history, and physical examination findings for both syndromes. A dermatologic database (ie, skin scrape, trichogram, cytology) and fungal culture should be used to rule out possible differential diagnoses. Once initial diagnostics have eliminated the more common causes of skin lesions seen in zinc-responsive dermatosis, skin biopsies with histopathology can confirm diagnosis. Biopsy samples should be taken from more severely affected areas with scaling and crusting (biopsy directly through the crusts). Care should be taken to avoid areas of ulceration; an intact epidermis is needed for diagnosis. The most consistent histopathologic change is diffuse parakeratotic hyperkeratosis that extends to involve the superficial portion of hair follicles.4 This microscopic change corresponds to scale and crusts seen on clinical examination, confirming the importance of sampling from these areas. Although it may seem intuitive to sample blood or hair to determine zinc concentrations in affected patients, this is not routinely performed because of technical issues with sampling and the variable results reported.2
Current Treatment Recommendations
Treatment of Syndrome 2 involves correction of the dietary deficiency or elimination of excessive mineral supplementation interfering with normal zinc absorption. Many times, skin lesions resolve within 6 weeks following dietary modification.2 Zinc supplementation might shorten recovery time and is required for several weeks. Treatment of Syndrome 1 typically requires lifelong zinc supplementation.
Zinc is available in several forms for oral supplementation, including zinc methionine, zinc gluconate, and zinc sulfate (Table). The most commonly used forms are zinc sulfate or zinc methionine, the latter of which has better oral bioavailability and causes less GI upset.2 Dosing recommendations may cause confusion, as some are based on the amount of elemental zinc in a product whereas others are based on the amount of zinc salt or the amino acid complex. Significant clinical improvement should be observed within 4 to 6 weeks of starting appropriate oral supplementation.
Table: Recommended Oral Zinc Dosages3,5
*This dose should be divided in half and given q12h with food to help prevent GI upset.
Failure to Respond to Initial Treatment
When dogs do not respond as expected, the first step is to ensure no secondary infections (Malassezia spp or bacterial) are complicating the lesions. Failure to address these may slow or prevent clinical resolution. The next option is to try an alternative oral zinc supplement or concurrent fatty acid supplementation. If these modifications do not provide further benefit, the addition of low-dose glucocorticoid therapy (eg, prednisone 0.25-0.5 mg/kg PO q48h, potentially long-term) may help alleviate clinical signs.2,5 Glucocorticoids can benefit patients with zinc-responsive dermatosis by enhancing zinc absorption from the GI tract. In some patients, the use of sterile zinc sulfate solution (10-15 mg/kg IV or IM) may be required; injections are initially administered weekly for a month then given every 1 to 6 months as needed. When zinc sulfate is administered IV, it should be diluted with sterile saline and given slowly over 10 to 15 minutes to prevent cardiac arrhythmias.5