What to Do With a Positive Lyme Test Result
What should I do when a patient has a positive result on a Lyme serologic test?
Although there is no absolute right or wrong answer, logical and practical options are available. Canine Lyme disease, with its causative agent, Borrelia burgdorferi, has become an extremely common tick-borne disease in many areas of the United States and Europe over the past 20 years in both humans and dogs.1 Despite the large number of clinical and nonclinical cases of Lyme disease in small animal practice in Lyme-endemic areas and excellent available diagnostic tests, veterinary practitioners still face many unanswered questions. One of the most basic questions is what to do with a positive result on a Lyme serologic test; this is not a trivial question for either clinical or nonclinical dogs.
What Tests Do We Have to Diagnose Lyme Disease?
Culture & Polymerase Chain Reaction
Culture or polymerase chain reaction (PCR) isolate and identify the organism. Unfortunately, these tests are not practical tools to identify B burgdorferi. Because this organism is not often found in the blood of infected dogs, results of these tests are usually negative, even in dogs with active disease.
Serologic Testing
Due to the limitations of culture and PCR, we must rely on serologic testing to identify B burgdorferi infection. Two types are widely commercially available:
Nonspecific or kinetic enzyme-linked immunosorbent assay (ELISA): This very sensitive test identifies antibodies produced against Borrelia whole-cell antigen. It does not differentiate between antibodies produced in reaction to Lyme infection and those produced against Lyme vaccination, and it will yield positive results in both instances. Because we can usually never be sure of infection status or, at times, vaccination status, a positive, nonspecific ELISA result should be followed with an additional test, such as a Western blot2 or a C6 antibody test.3
C6 antibody testing: Two types of tests are available for canine antibodies against the Lyme C6 peptide. This peptide is expressed only during infection; therefore, results of these tests are meant to be positive only in the event of natural exposure and negative only in naive dogs or dogs vaccinated against Lyme disease.4 These tests include the in-house SNAP 3Dx or SNAP 4Dx tests and the quantitative C6 antibody test (idexx.com). These tests can be used in the following situations:
The SNAP tests are excellent tools for screening dogs for Lyme infection and common co-infections. This can be done as part of a screening program for nonclinical dogs or when Lyme disease is suspected. A positive result indicates active Lyme infection.5
The C6 antibody test looks for similar antibodies as the SNAP tests but in a quantitative fashion. We still have a lot to learn about the value of knowing the quantitative C6 titer in all cases of Lyme infection, but we do know that the quantitative C6 titer does decrease with therapy.6 In addition, the titer correlates with circulating antiLyme immune complexes.7 In my opinion, it is likely a useful tool in treatment decisions of nonclinical dogs.
The Western blot is smeared with Lyme antigens located in known areas. This is a relatively expensive and labor-intensive test, and interpretation of the result requires expertise. Therefore, this will never be in-house technology. SNAP tests and quantitative C6 assays have usurped some of the role of the Western blot as a confirmatory assay. At this time I would recommend using the Western blot only when the vaccinal status is important to the veterinarian.
Lyme Disease in Sick Dogs
Clinical Signs
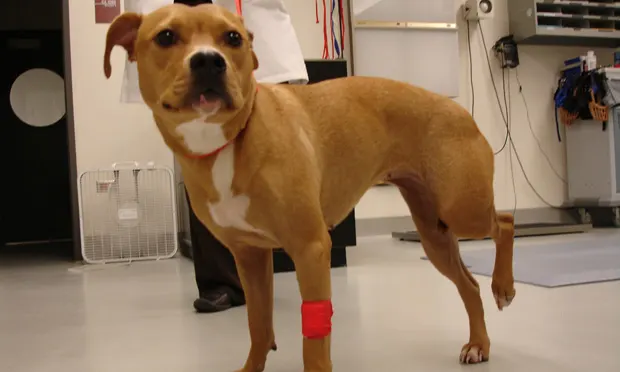
The lack or apparent lack of clinical signs in most dogs with active Lyme infection makes both the diagnosis and the study of this disease very difficult. Overt clinical signs are observed only in approximately 5% to 10% of infected dogs.8 These signs tend to occur 2 to 5 months after the experimental infection and include lameness, monoarthritis or polyarthritis (Figure 1), lymphadenopathy, lethargy, and fever.9 Unlike in humans with acute infections, skin lesions are uncommon in dogs.
The classic Lyme signs of arthritis, pain, fever, and lethargy typically resolve within approximately 3 days, in some cases only with antibiotic therapy.1 Renal disease (Lyme nephritis) appears to be a life-threatening, rare sequela of B burgdorferi infection in a small subset of dogs. Some questions remain about other, more serious, less common syndromes associated with Lyme infection in dogs, including cardiac disease (myocarditis) and neurologic disease. Another question yet to be answered is whether some dogs develop the devastating chronic recurrent disease, as seen in some infected humans; hopefully future studies can provide data that can help answer this question.

Typical presentation of acute non–weight-bearing monoarthritis in a dog with clinical Lyme disease
Diagnosis
What is a rational approach to a sick dog suspected of having Lyme disease? If the clinical signs are classic and the result of the Lyme test (SNAP test or Western blot) is positive for infection, then the additional recommended tests include:
Complete blood count and serum biochemical profile
Urinalysis to assess for proteinuria (this is very important)
Determine possible coinfections based on region (eg, anaplasmosis, Rocky Mountain spotted fever, babesiosis)
Treatment
After testing, treat with doxycycline (10 mg/kg Q 24 H) for 1 month. This dose is considered the standard of care and has been shown to be sufficient in treating clinical disease;10 however, it is not based on extensive experimental dosage studies in dogs. If the clinical signs resolve within a day or two of therapy, as expected, and do not recur during or soon after stopping therapy, it is reasonable to assume that the dog did have Lyme disease.
Response to therapy alone does not prove Lyme as an etiologic agent—coinfection, response to the nonantimicrobial properties of doxycycline, and coincidental improvement are all possible. In such circumstances, Lyme disease is a reasonable diagnosis. However, if the clinical signs are not classic and the signs do not resolve within a day or two of therapy, or if they return during or soon after cessation of therapy, the clinician should assume that this is not Lyme disease. A thorough workup should then be aggressively pursued.
Screening in Nonclinical Dogs
Annual Screening
There are many advantages to annually screening nonclinical dogs with a 4Dx SNAP test:
Testing is necessary for assessment of Lyme prevalence in a given practice area.
Being Lyme-positive is a marker for tick exposure and increases awareness of coinfection.
Testing can be used to measure the success of Lyme prevention strategies, including tick control and vaccination.
Testing provides a marker of possible risk for human exposure.
Positive Tests
What should you do when a dog tests positive? No definitive study has proved that treating nonclinical Lyme-positive dogs prevents future clinical disease. We do know, however, that treatment does cause a decrease in C6 antibody titers and circulating immune complexes in most dogs. The C6 titer and circulating immune complexes are positively correlated; the higher they are, the more likely they are to decrease with therapy. There are 3 main approaches to this practical clinical question, and one could argue that none have been proven right or wrong:
Many veterinarians treat all positive nonclinical dogs. The reasons not to treat (global resistance to doxycycline, expense of treatment, and side effects) may not convince many veterinarians and owners not to err on the side of treating all positive dogs.
Some veterinarians do not treat any positive nonclinical dogs. Because treatment has not been proven to prevent disease, this approach is obviously acceptable as well.
Although an approach that is not definitively proven, some veterinarians attempt to treat dogs that may be more likely to benefit from therapy. This assessment can be based on the following:
Lyme-positive dogs should be tested for proteinuria with a dipstick. A positive result should be confirmed with urinalysis and, ideally, a protein–creatinine ratio. Such dogs should thus be considered “clinical” and treated appropriately (see Treatment under Lyme Disease in Sick Dogs).
In a dog without proteinuria, a quantitative C6 titer can be used to aid in treatment decisions. In my opinion, if the titer exceeds 30, it seems reasonable to treat the dog, although some would argue that it is also reasonable not to treat. The titer will most likely decrease after treatment and probably reflects a similar decrease in circulating immune complexes. This approach has not been proven to be beneficial but appears reasonable on the basis of the partial knowledge currently available (Figure 2)

Suggested algorithm for a positive result on a SNAP 4Dx or 3Dx test in a nonclinical dog. Reprinted with permission from Lyme. Goldstein RE. In Ettinger SJ, Feldman EC (eds): Textbook of Veterinary Internal Medicine, 7th ed—Saunders Elsevier, 2010.