Vulvovaginal Hemorrhagic Discharge in the Dog: Caudal Reproductive Tract
John P. Verstegen III, DVM, MSc, PhD, DECAR, University of Florida
Karine J. Onclin, DVM, PhD, DECAR, University of Florida
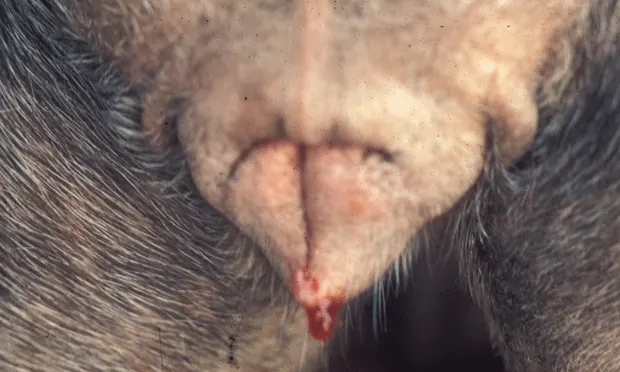
Proestrual vulvar bleeding in the bitch
Profile
Definition
Vaginal bleeding, which is a misused term, should instead be called vulvovaginal hemorrhagic discharge (VVHD). Indeed, VVHD refers to the clinical observation of blood leaking from the vulvar opening, while vaginal bleeding should theoretically refer only to a bleeding vagina.
VVHD is a normal physiologic observation during proestrus and estrus, which occurs on average every 7 months starting at puberty (range varying from 4 to more than 12 months). During the estrous cycle, bleeding is of uterine origin and is elicited by estrogens produced by the ovarian follicles (Figure 1).
Pathologic VVHD is complex and may find its origin from various parts of the female reproductive tract, from the vulva itself to the ovaries. In some instances the urinary tract may be involved or the bleeding may be caused by systemic problems such as coagulopathies (eg, disseminated intravascular coagulation). This article will cover only pathologic bleeding originating from the caudal reproductive tract even if the cause may stem from other areas.
Causes
The causes of VVHD vary greatly. Discharge originating from the vulva and the vagina can be traumatic, infectious, hormonal, or neoplastic. The discharge may be associated with an externally normal or abnormal vulva or the presence of lesions and/or protruding masses. Congenital abnormalities of the external reproductive tract (eg, recessed vulva) and vagina (eg, fibrous band, stricture, ectopic urethra, or hypolastic development) can often be primary causes of VVHD.
Trauma can be linked to licking, biting, fighting, or inappropriate breeding of animals with anatomic abnormalities (eg, strictures, septum, fibrous bands, persistent hymen, etc) or when vaginal rupture occurs as a result of attempts to separate dogs in a breeding ‘tie'. Vulvovaginal hematomas may manifest with bleeding and can be caused by trauma. Improperly obtained samples for vaginal smear or vaginal endoscopy may be associated with secondary bleeding. Trauma can also be associated with foreign bodies such as broken vaginal cytology swabs.
Infectious causes may involve the vulva or vagina or both, mostly by extension from one to the other. Infectious VVHD is rarely primary, but most often secondary to acquired abnormalities (particularly vulvar and/or vaginal hypoplasia as observed in some early-spayed animals) or congenital anatomic abnormalities (strictures, fibrous bands, urine pooling, ectopic urethra). Tumors of the urinary/reproductive tract and local skin diseases are also leading causes.
Prepubertal vulvovaginitis is rarely infectious but generally caused by an underlying etiology (ie, congenital abnormalities/hormonal imbalance) that leads to irritation/inflammation and impairment of local immune defenses. Prepubertal vulvovaginitis is most often associated with mucous or mucopurulent discharge. However, hemorrhagic discharges are sometimes observed. Bacteria, if present, are generally nonspecific and of no real significance. Prepubertal vaginitis often resolves spontaneously after the first estrus. It should not be treated with antibiotics until the primary cause has been identified and cured. If clinical signs persist after primary treatment, antibiotics may be considered to control bacterial growth. However, antibiotic treatments will never cure the vaginitis if the primary cause is not corrected.
Adult vaginitis is more often infectious with numerous, often specific bacteria (Escherichia coli). Specific infectious agents such as herpesvirus or Brucella canis may be associated with vaginal and perivulvar lesions that induce bleeding. Adult vaginitis may be secondary to a congenital or acquired anatomic vaginal abnormality (vaginal atrophy after OHE) or urinary tract abnormality (ectopic urethra). Systemic diseases such as diabetes mellitus may also promote development of vaginitis. Bleeding observed (Figure 2. Necrotic (A) and hemorrhagic (B) vaginitis as detected by vaginoscopy in the dog) is generally secondary to inflammation and development of ulcerations. In adult vaginitis, bacteria are generally significant and should be treated at the onset, even before the underlying cause has been identified. When herpes vesicles (Figure 3) rupture, some spotting and/or bleeding may be observed.

Figure 3. Herpes vesicles seen during vaginoscopy in an adult dog with VHD
Figure 4. Vaginal hypertrophy with bleeding (A) and vaginal prolapse (B)
Ovarian hormonal disorders (eg, tumors, cysts, irregular or prolonged estrus) or individual hypersensitivity to estradiol in otherwise normal animals may lead to prolonged physiologic VVHD, development of vaginal prolapse (Figure 4), or masses including vaginal hyperplasia and tumors. Administration of exogenous hormones such as androgen may promote the development of clitoral abnormalities.
Vaginal hyperplasia/prolapse complex is not directly responsible for bleeding, unless tissue is also traumatized. Estrogens first induce vaginal hyperplasia, which is associated with tissue relaxation and development of edema. Edema promotes prolapse of the vagina. It is common for vaginal hyperplasia to lead to prolapse when it originates in the dorsal vagina. There is no clear breed predisposition, but vaginal prolapse is commonly observed in breeds such as boxers (or boxer crosses), some sheepdogs, and rottweilers. Some hereditary influence has been described.
Vulvar or vaginal tumors are associated with vulvar discharge or the sudden appearance of a mass protruding from the vulva (most often seen in diestrus). These conditions are mainly observed in senior, sexually intact animals with an average onset of 7 to 10 years of age. Tumors of the vulva are rare. They are sometimes observed as tumors of the Bartholin's glands and perivulvar glands but most often are an extension of neoplasia of the vagina or urethra. Tumors of the vagina are relatively uncommon in dogs and most often benign (> 70%) and, except for transmissible venereal tumors (TVT, Sticker's sarcoma), are of smooth muscle or fibrous tissue origin (leiomyoma or fibroma).
Leiomyomas are estrogen-dependent. They develop mostly during estrus and are observed during early diestrus when vaginal hyperplasia disappears, promoting exteriorization/visualization of the tumor. Leiomyomas generally do not bleed except when ulcerated.
Leiomyosarcomas are invasive and, even if they do not metastasize through the lymphatic or vascular pathway, tend to extend throughout the vagina and sometimes even into the urethra. Hormonal dependency of this tumor is less obvious. Leiomyosarcomas are often associated with significant continuous or discontinuous bleeding. Infiltrative vulvar and vestibulovaginal hemangiosarcomas have also been described, and are associated with intermittent VVHD.
Figure 5. A TVT vulvovaginal lesion in a female poodle before vincristine treatment (A) and one week after the start of treatment (B)
TVT or Sticker's sarcoma is also a common tumor in the dog (Figure 5), affecting the external genitalia and other mucous membranes (mouth, nose, respiratory mucosa, eyes), including the caudal reproductive tract. Traditionally seen in tropical and subtropical regions, this condition is now found worldwide as a result of increased exchange between countries and pet travel. In the female, lesions are typically observed in the vulva and vagina after a few weeks to a month of incubation. Reddish-gray friable tumors develop; initially small nodules, they rapidly grow and gain a papillary and pedunculated, cauliflower-like appearance.
The pathogenesis of this tumor is not clear. Viruses have been hypothesized but none has been identified. TVT neoplastic cells have a chromosomal number of 59 +/- 5, which differs from the normal 78 in the dog. Transmission occurs during coitus but may also be from close contact or licking.
Enlargement of clitoral tissue (Figure 6) can also be associated with VVHD. The condition is most often either congenital, as in some cases of hermaphroditism, or the result of endogenous or exogenous androgens (mibolerone administration to control cycle or to treat cystic endometrial hyperplasia).
Figure 6. Clitoral hypertrophy in a racing dog before (A) and after surgical correction (B)
Clinical Signs
Clinical signs of underlying causes of VVHD are scarce, but include: inflammation of the vulvar and perivulvar tissues; changes in perineal hair color due to licking; erosion or ulceration; dysuria, anuria, or stranguria, either due to pain during micturition or secondary to associated urinary tract infection and compression; tenesmus/constipation caused by compression of the rectum by an intravaginal mass; and pain.
The discharge may vary from light and intermittent without any other clinical signs to continuous bleeding with multiple other signs. When due to systemic disease, such as coagulation disorders, the discharge is often associated with general health changes including prostration, inappetence, and fever.
Hyperplasia/prolapse complex and tumors are most often associated with protrusion of a mass from the vulva. Tumors are usually localized to one side of the vulvar opening while prolapse generally involves the entire opening of the vulva.
Risk Factors
Aging (cycling irregularities)
Genetic (vulvovaginal anatomic abnormalities)
Early OHE (6-12 weeks of age, vaginal hypoplasia and recessed vulva)
Iatrogenic (unwarranted antibiotic treatment for secondary caudal reproductive tract abnormality and chronic vaginitis, estrogen or androgen administration)
Pain Index
Except in long-term and/or complicated infectious/traumatic problems, pain is not considered severe and generally results from multiple inflammatory processes. NSAIDs are generally efficient for controlling pain and inflammation; opiates may be needed in some chronic and severe cases.
Diagnosis
Definitive Diagnosis
History: To characterize nature of discharge (physiologic or not; continuity; severity; presence of trauma, infection, or toxicosis; etc)
Local examination: To identify origin of discharge (vulvar only or involving reproductive and/or urinary tract). Vulvovaginal palpation is always recommended for detection of caudal vaginal abnormalities (stricture, fibrous band, hymen) and masses. Localized delimited tumors are most often leiomyoma, hyperplasia, or prolapse while invasive, friable tumors are most likely leiomyosarcoma or TVT
Vaginal smears: To identify stage of estrous cycle, presence of estrogenic influence (superficial cornflake-like cells), and inflammatory or multinucleated giant tumor cells. Superficial cornified cells in high numbers (> 70%) indicate presence of significant estrogens of exogenous or ovarian origin (Figure 7).
Vaginoscopy: To confirm the stage of the estrous cycle, visualize lesions (tumor, trauma, TVT, herpes vesicles), identify bleeding from the vagina or cervical os. Vaginoscopy can be performed using either a human pediatric proctoscope or an endoscope
Vaginal cultures: To establish the predominant organism(s) associated with vaginal discharge and as a guide for selection of a therapeutic agent
Ultrasonography: To identify uterine or ovarian lesions
CBC (anemia, toxemia) and serum biochemical profile (coagulopathy, diabetes mellitus): To evaluate extent of lesions and possible systemic complications
Treatment
Depends on cause and origin of the hemorrhagic discharge. Surgical treatment ranges from vulvoplasty in cases of hypoplastic and recessed vulva (Figure 8) to vaginal tumor ablation for localized benign vaginal tumor or even total vaginal ablation for infiltrative malignant vaginal tumors. OHE is not advised for prepubertal vaginitis as it has been associated with continuation of the clinical signs and further resistance to treatment.
Medical treatments vary (see Table). If bleeding is due to estrous cycle abnormalities and if dog is being bred, hormonal treatment is warranted. Hormonal strategies range from hCG injections to induce ovulation to ergot derivatives and prostaglandins or oxytocin to treat subinvolution of the uterus and placental sites occurring in the immediate postpartum period.
Treatment for vaginitis in prepubertal bitches is justifiably conservative as most will recover spontaneously, but analgesics may be warranted, as with adult vaginitis. Antibiotics are generally not justified in prepubertal vaginitis and may induce development of bacterial resistance.
Chronic vaginitis in adult bitches is often associated with identifiable abnormalities of genitalia (35%) or urinary tract (26%) and resolution is directly related to their resolution. In older animals, if an infectious cause is underlying, it should be treated for 4 to 6 weeks with an appropriate dose of antibiotic, with selection based on culture and sensitivity testing.
Chemotherapy with vincristine is still the best therapeutic choice for TVT. It may be used in combination with surgical removal of the main lesions. Vincristine may affect fertility.
Table: Selected Causes of Hemorrhagic Vulvovaginal Discharge & Possible Therapy
In General
Relative Cost
Cost of treatment will range from a few dollars for an injection of hCG to thousands of dollars for total vaginal ablation.
Prognosis
Generally good but obviously depends on the cause. Anatomic abnormalities have a good prognosis; primary infectious chronic adult vaginitis a more guarded prognosis; and invasive leiomyosarcoma a poor prognosis.