Top 5 Topical Dermatologic Therapies
Elizabeth A. Layne, DVM, DACVD, BluePearl Pet Hospital, Midvale, Utah; Montana Veterinary Dermatology, Bozeman, Montana; Unleashed Veterinary Dermatology, Stratford, Connecticut
Douglas J. DeBoer, DVM, DACVD, University of Wisconsin–Madison
Topical therapy is of renewed interest in veterinary dermatology, both as primary short-term treatment and as an intervention that can prevent or reduce the frequency of severe flares of recurrent infection or allergic inflammation. In some cases, topical therapy, either alone or with systemic treatments, can be more effective than systemic therapies alone. Careful selection of products that are conducive to client compliance is critical to long-term success. The increasing variety of product formulations gives veterinary practitioners and pet owners more options for managing dermatologic problems.
The following 5 ingredient descriptions can aid veterinarians and their teams in tailoring dermatologic treatment plans.
1. Chlorhexidine as Pyoderma Treatment

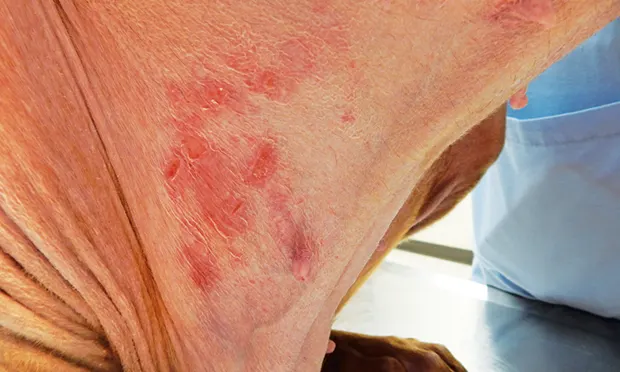
Superficial bacterial folliculitis on the ventral neck of a dog; this would be amenable to daily topical chlorhexidine therapy without systemic antibiotics.
Superficial bacterial folliculitis (typically staphylococcal pyoderma) commonly affects patients secondary to underlying disease, such as allergy or endocrine disease1 (Figure 1). With the rise of methicillin-resistant Staphylococcus spp (eg, S pseudintermedius [MRSP], S aureus [MRSA], S schleiferi [MRSS]) as well as other antibiotic-resistant organisms, dermatologists are looking at treatment differently. Topical antibacterial therapy should be used in all cases; for some patients, it might be the sole therapy.1,2 Chlorhexidine is an excellent topical antibacterial for treatment of superficial pyoderma and prevention of recurrence. It is economical and involves low risk for adverse effects. The authors prescribe daily topical chlorhexidine as primary treatment for mild-to-moderate superficial pyoderma—without antibiotics—for 2 to 4 weeks. For preventing recurrence, chlorhexidine is used 2 to 3 times per week long-term. Chlorhexidine is available in shampoos, sprays, leave-on mousse, and wipes. Individual pet and owner preferences can result in selection of 1 form over another; for instance, daily application of 2% to 4% chlorhexidine spray with weekly 2% to 4% chlorhexidine shampoo baths is feasible for many clients. Wipes are useful for face or tail folds, interdigital areas, and the perineum. Topical chlorhexidine therapy can reduce or eliminate the need for systemic antibiotics.1-3
2. Topical Corticosteroids for Preventing Atopic Flares

Cutaneous atrophy and ulcerations in a dogs inguinal region caused by prolonged frequent application of betamethasonegentamicin spray.
Topical corticosteroid application can provide the benefits of systemic corticosteroids with lower risk of adverse effects.4 Topical corticosteroids can prevent flares of atopic dermatitis and, in some cases, can perform as well as systemic antipruritic medications.5,6 Product selection is critical. Long-term use of betamethasonegentamicin sprays (ie, more than a week) should be avoided because of cutaneous corticosteroid adverse effects and development of antimicrobial resistance (Figure 2).7,8 Betamethasone valerate is a potent corticosteroid that can induce epidermal atrophy and ulceration.7,9 Systemic absorption of topical corticosteroids can induce systemic adverse effects, such as suppression of the hypothalamicpituitaryadrenal axis and sensitization of the endocrine pancreas.10 A simple alternative to steroid and antibiotic combinations is chlorhexidine to control infection and a steroid-only product to control inflammation, facilitating tailored steroid and antibiotic treatment to the clinical condition. There are few veterinary-specific corticosteroid-only topical products. A 0.015% triamcinolone acetonide spray (Genesis, virbacvet.com) is moderate-potency and low concentration; this is useful for localized inflammation and pruritus. Outside of the United States, hydrocortisone aceponate spray 0.584 mg/mL (Cortavance, virbac.ca) is available; this soft steroid is metabolized by the epidermis and provides a moderately potent anti-inflammatory effect. However, this product has a lower risk for adverse effects than other products because of unique biochemistry in the epidermis.4
Preventing recurrence of signs is part of the emerging concept of proactive therapy for atopic dermatitis.
There are many widely available and affordable generic topical corticosteroids for humans; hydrocortisone 2.5% cream and triamcinolone 0.1% cream are short-term options. Optimal dosing and duration of these products have not been published for veterinary patients, and adverse effects are possible. The lowest frequency of application that controls clinical signs should be used. Preventing recurrence of signs is part of the emerging concept of proactive therapy for atopic dermatitis. This involves preventing flares of inflammation and infection when the skin appears normal; intermittent topical corticosteroid application is an important component of this therapy.11
3. Otic Corticosteroids as Maintenance Therapy
Just as topical corticosteroids can proactively reduce flares of atopic dermatitis6 and minimize the need for systemic medication, otic corticosteroids administered as part of maintenance therapy for inflammatory ear disease can manage otic pruritus, minimize chronic inflammatory changes, and possibly reduce the occurrence of secondary infections.12 Recurrent infectious otitis externa typically involves an underlying skin disease; atopic dermatitis and primary seborrhea are the most common. Once an infection is successfully treated, it is necessary to attempt to prevent recurrence because neither atopic dermatitis nor primary seborrhea are curable conditions. As with topical or systemic corticosteroids, it is necessary to use the lowest effective frequency of application that prevents recurrence of inflammation and infection while minimizing adverse effects. The authors generally find that once the primary infection has been successfully treated, instillation of the steroid-only drop once or twice a week is sufficient to control inflammation and prevent relapsing infection (see Corticosteroid-Only Otic Preparation). It is wise to advise concurrent weekly cleaning with an antiseptic ear cleaner to remove debris, which makes the ear less hospitable to microorganisms.
Corticosteroid-Only Otic Preparation
Synotic Otic Solution (zoetis.com) is approved to relieve pruritus and inflammation from acute and chronic otitis externa in dogs. It is labeled for twice-daily application for no more than 14 days. According to the Synotic Otic Solution package insert, fluocinolone acetonide is approximately 100 times more potent than hydrocortisone. Dimethyl sulfoxide enhances systemic absorption. For animals that require potentially lifelong otic corticosteroids, twice-daily administration has the potential to result in iatrogenic hyperadrenocorticism.10 It is not known if less frequent administration would provide anti-inflammatory benefits while minimizing adverse effects.
The authors use a solution of 1 mg/mL dexamethasone in propylene glycol for longer-term ear care. This compounded moderate-potency steroid formulation is applied daily for 7 to 14 days until clinical signs of pruritus and erythema are controlled; it then is used once or twice a week for longterm maintenance. Be aware of federal and state regulations regarding veterinary compounding.
For preparation, see uwveterinarycare.wisc.edu/wp-content/uploads/2017/01/ear_formulary.pdf
4. Antiseborrheic Topicals

Excessive scale and follicular casts typical of primary seborrhea. Frequent topical treatment can provide long-term control.
Primary seborrhea (Figure 3) involves increased keratinocyte turnover with altered maturation in the absence of an identifiable underlying cause. Because this is a heritable disorder,13 cure is not possible; however, long-term control can be achieved using topical therapy. A variety of topical ingredients can be useful for decreasing skin cell turnover, increasing desquamation of keratinocytes, and normalizing sebaceous secretions. Sulfur, salicylic acid, and benzoyl peroxide have been available for many years in a variety of forms. Phytosphingosine is a relatively new ingredient in veterinary products. It is in the family of sphingolipids that comprise the normal epidermal lipid barrier. Application of phytosphingosine shows promise in normalizing the epidermal lipid barrier and modifying the production of sebum.14 It is available in shampoo, spray, and leave-on mousse formulations. A key principle in antiseborrheic topical treatment is frequent (at least twice a week) application of the medicated product. Because most owners are unable to bathe their dogs this frequently long-term, the spray and mousse products are very helpful.
5. Azole Antifungals
Overgrowth of the cutaneous yeast Malassezia pachydermatis is recognized as a flare factor for atopic dermatitis (Figure 4).14,15 Some dogs are additionally hypersensitive to the yeast itself.<sup15 sup> Because M pachydermatis is part of normal canine skin flora, dogs with yeast hypersensitivity can be challenging to manage. Although oral antifungal medications may be typically required initially, topical antifungals are an excellent addition to short- and long-term management and, in some cases, might be sufficient to prevent recurrence.2 There are a variety of products available containing either an azole alone (eg, miconazole, clotrimazole, ketoconazole, climbazole) or an azole combined with chlorhexidine for dogs affected by concurrent bacterial and yeast overgrowth.


(A) Dog with yeast dermatitis. (B) Photomicrograph with yeast (arrow) and cocci bacteria (arrowheads) compared.