Top 5 Keys to Successful Management of Otitis Externa
Erin E. Aufox, DVM, University of Tennessee
Elizabeth R. May, DVM, DACVD, University of Tennessee
We sat down with Dr. Aufox to further discuss otitis externa management. Listen to her episode of Clinician's Brief: The Podcast here.
Otitis externa is a common inflammatory condition that affects 15% to 20% of dogs and 4% to 7% of cats.1 Dogs and cats of breeds predisposed to otitis externa may have pendulous ears, canal hypertrichosis, and familial seborrhea or cerumen gland hyperplasia.2,3
Although some patients may have irreversible external ear canal changes necessitating surgical management, many cases can be managed medically. Incorporating steps early in the disease course may help prevent chronic changes (eg, proliferation, fibrosis, mineralization of the external ear canal) and recurrence.
Following are the authors’ top 5 steps to manage otitis externa.
1. Classification
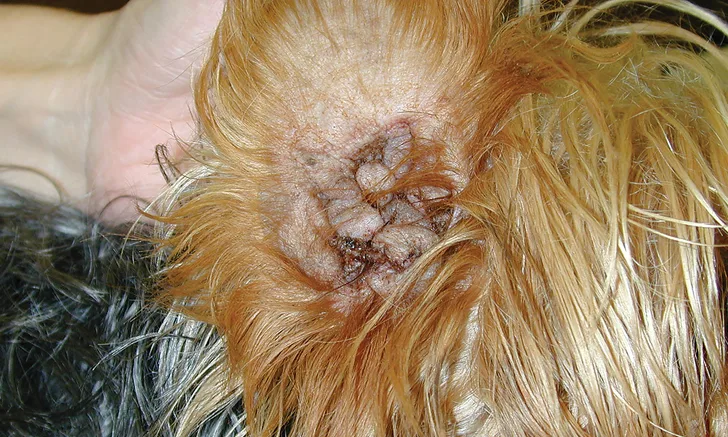
Successful treatment of otitis externa should begin with clinical assessment of the patient (ie, ear canal palpation, otoscopic examination, cytology). Palpating the ears can aid in determining whether a patient is best managed medically with antimicrobial drugs and glucocorticoids or surgically. Normal ear canals should be pliable. Surgical management should be considered for ear canals that are firm due to fibrosis and calcification and/or ossification (Figure 1).4

FIGURE 1 Severe vertical canal epithelium and ceruminous gland hyperplasia impeding medical management of otitis externa. Surgical management is recommended in this case.
Otoscopic examination of both ears using a standard handheld otoscope with 2×/4× magnification and a reusable 0.75-inch cone includes assessment of the exudate type (eg, ceruminous, purulent), degree of stenosis, and integrity of the ear canal (eg, presence of ulceration, mass, polypoid changes, ceruminous gland hyperplasia) and tympanic membrane. In patients with stenotic ear canals (and those exhibiting signs of pain with comorbid diseases for which sedation or anesthesia may be initially contraindicated), otoscopy may be delayed and topical and/or oral steroid treatments prescribed to manage patient discomfort.1 If a sample for cytology can be obtained at the time of initial presentation, topical antimicrobial therapy should be initiated simultaneously with steroid therapy to address the infectious disease component. In patients with severely stenotic ear canals, daily oral steroid therapy may be the best treatment option until the patient is comfortable and a cytology sample can be obtained.
Otic cytology is an essential test used to diagnose and characterize otitis externa.1,5 Type of organism present (eg, cocci, rods, yeast), relative numbers of organisms (1-4+ scale), and presence or absence of inflammatory cells (typically, neutrophils) should be recorded. Purulent exudate and ulcerative lesions in the canal are typically associated with Pseudomonas spp infection (Figure 2) or reaction to a topical medication. Inflammatory cells are not routinely observed when there is ceruminous discharge containing yeast organisms with or without bacteria.

Ulcerative ear pinnal lesions with profuse green discharge characteristic of Pseudomonas spp otitis
Cytologic presence of neutrophils (with or without rods) and appropriate clinical findings may suggest Pseudomonas spp otitis or contact reactions, both of which should prompt aerobic culture; culture should also be performed if bacterial otitis does not respond to appropriate empiric treatment.1,6 Diagnosis of infectious otitis using culture results without cytology can be misleading. The ear canal hosts various species of bacteria in the healthy state, and bacterial organisms, including methicillin-resistant Staphylococcus spp, can be recovered from culture samples of healthy ears of dogs or cats.7,8 Misdiagnosis and inappropriate therapy are possible if otic cytology results are not considered when culture results are interpreted. Culture results should parallel cytology findings, allowing for selection of the appropriate pathogen-specific therapy. Susceptibility data are not used initially to select treatment because topical medications achieve higher local concentrations than those achievable in plasma, upon which susceptibility interpretation is determined. Susceptibility data are used for refractory cases unresponsive to standard treatment protocols.
2. Treatment
Ear canals should first be opened, as ear canal epithelial inflammation and stenosis hinder effective topical treatment, and most cases therefore require topical and/or systemic corticosteroid treatment.2
Ears should be cleaned by flushing, which removes dried medication and cerumen that may interfere with examination and treatment. Sterile saline flushing should be selected when tympanic membrane status is unknown to minimize concern for ototoxicity.9 Squalene is an effective ceruminolytic agent with demonstrated safety in the middle ear and is an alternative option when perforation is suspected.10 During treatment, at-home flushes containing salicylic acid or other mild ceruminolytics should be administered 2 to 3 times per week to maintain ear canal cleanliness.
Treatment selection is based on pathogen identification (yeast vs Pseudomonas spp vs other bacteria), exudate characteristics, and chronic ear canal changes. Because external ear canal volume varies among dog breeds (eg, brachycephalic breeds, 0.47 mL; mesaticephalic and dolichocephalic breeds, up to 5.86 mL),11 extra-label dosing (0.5-1 mL) of most topical ear medications should be used for each affected ear to allow medication to sufficiently coat the ear canals. Antimicrobial medications, excluding long-acting, FDA-approved florfenicol otic medications, are applied twice daily (extra-label) to ensure maintenance of adequate antimicrobial concentrations and inflammation reduction. For stenotic canals, a solution is preferred over an ointment.
Topical antibiotics (eg, fluoroquinolones, amikacin, tobramycin, silver sulfadiazine, ceftazidime) are frequently used to treat Pseudomonas spp. Due to drug inactivation, gentamicin and neomycin are ineffective against Pseudomonas spp otitis, seemingly more so than other aminoglycosides such as amikacin and tobramycin, which have been effective for treatment of Pseudomonas spp otitis in the authors’ experience.12,13 Florfenicol is also ineffective against Pseudomonas spp otitis due to its spectrum limitations.12,13 Using a tris-EDTA–containing flush, which serves as a calcium-chelating agent, can help the effectiveness of topical antimicrobial treatment. These flushes are commercially available and increase the medication permeability of gram- negative organisms by damaging the outer cell wall membrane. The calcium-chelating flush should be applied as pretreatment in conjunction with topical therapy for improved treatment efficacy against Pseudomonas spp otitis.14
Systemic antibiotics should be reserved for the treatment of otitis media and are ineffective in the treatment of otitis externa.2,15
3. Monitoring
The patient should first be assessed 2 to 3 weeks after initiating treatment to determine if the treatment plan is effective based on otoscopic examination and cytology. Otoscopic examination and cytology should also be performed at each follow-up visit to document changes, including resolution. A successful outcome is dependent on timely recheck examinations with diagnostics, including sedation if needed for effective examination.
4. Maintenance
Otitis can cause changes to the ear canal, predisposing the patient to future infections.1,16 Ear flushing is required long-term unless return of self-cleaning mechanisms of the canal epithelium are documented. In addition, controlling ongoing low-level inflammation should decrease disease recurrence. Once–to–twice-weekly treatments with topical steroid formulations (ie, the least potent form to control clinical signs) are effective when an underlying cause cannot be identified or adequately controlled by other means. Systemic absorption of topical steroids should be considered when performing endocrine testing and, when used long-term, necessitates monitoring clinical signs and performing minimum database testing for adverse effects.17
5. Identification
After otitis has resolved, the primary cause should be identified to help prevent recurrence, although identification is less useful in cases in which chronic ear canal changes become a perpetuating cause of disease or cases in which recurrence can be prevented by a simple maintenance regimen. Aural conformation, allergic conditions (especially atopy), and endocrinopathies (eg, Cushing’s disease, hypothyroidism) are common causes of otitis externa, with neoplasia and/or foreign bodies considered for patients with unilateral otitis.2
Conclusion
Otitis externa is a common disease of dogs and cats presented for veterinary care. Most patients can be treated quickly, and recurrence can be prevented by incorporating these fundamentals early in the course of disease, which can help patients avoid chronic pain and pathology to the external ear canals.