Top 5 Emergencies Requiring Anesthesia
Kate Cummings, DVM, DACVAA, MedVet
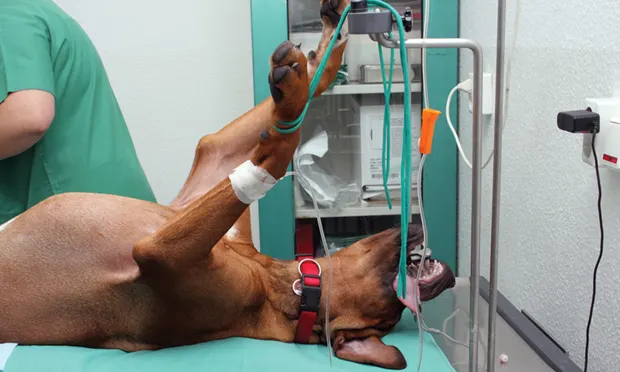
Before administration of anesthetic agents, critical patients should be evaluated and stabilized; patient history, cardiovascular and respiratory stability, pain level, and available laboratory results must be considered. Replacement fluids (eg, crystalloids, colloids, blood products) are often required to restore volume status and correct electrolyte abnormalities.1 Therefore, appropriate ECG, SpO2, blood pressure, and end-tidal CO2 monitoring is essential. Readily accessible intravascular catheters are strongly recommended, and emergency drug doses should be calculated and be available before anesthetizing.
1. Gastric dilatation–volvulus
At presentation, patients with gastric dilatation–volvulus (GDV) are often hypovolemic and require aggressive fluid resuscitation (~50 mL/kg; actual endpoint is patient specific until patient heart rate is <150 bpm and systolic blood pressure is >90 mm Hg1,2). Gastric decompression by trocarization or stomach tube is recommended to improve ventilation before anesthesia is initiated. Electrolyte abnormalities and acid–base imbalances should be corrected, and cardiac arrhythmias (early and late in the disease process) should be identified by ECG and treated.
An opioid (see Common Emergency Anesthesia Protocols, for dosing instructions) can be used alone or with a benzodiazepine to sedate for gastric decompression and may serve as premedication. Opioids may decrease GI motility, but this is of minimal relevance in GDV patients. Although opioids are advantageous, they can cause vomiting3; fentanyl, methadone, and buprenorphine IM or IV or hydromorphone or oxymorphone IV are less likely to induce vomiting.3 Ketamine in combination with a benzodiazepine is recommended for induction in most fluid-resuscitated patients,4,5 whereas poorly stabilized patients that must be taken to surgery immediately can be administered a fentanyl–midazolam–ketamine (lower dose) combination; this is often reserved for patients that are depressed and recumbent before anesthesia. Propofol should be avoided and can cause hypotension following IV administration.
Anesthetic maintenance can be achieved with inhalants, although GDV patients may not tolerate them because of their vasodilatory effects; therefore, intraoperative fentanyl constant-rate infusion (CRI) or intermittent hydromorphone doses allow use of reduced inhalant concentrations to minimize associated hypotension. Dopamine may be required for additional blood pressure support in adequately volume-resuscitated patients, and poor response to a positive inotrope may suggest insufficient fluid resuscitation or abnormal blood pH. Lidocaine and ketamine CRIs6 will provide intraoperative multimodal analgesia and lidocaine may be useful if ventricular arrhythmias develop. Intraoperative analgesics should be continued postoperatively, based on postextubation patient comfort.
2. Urethral obstruction
Cats with urethral obstruction (UO) often require immediate and rapid urethral catheterization. Before sedation and analgesia are initiated, the patient’s hydration status, electrolyte values (particularly potassium), and mentation must be assessed. Treatment for dehydration and severe electrolyte abnormalities should begin with IV fluids, particularly 0.9% NaCl, which (with dextrose) may aid in resolving hyperkalemia. Calcium gluconate and dextrose (± regular insulin) can provide further stabilization in cats with significant hyperkalemia (potassium >7.5 mEq/L) and bradycardia. Although calcium gluconate does not alter potassium values, it does stabilize cell membranes, allowing time to reduce potassium levels and minimize the cardiotoxic effects of hyperkalemia.2,7,8 To promote intracellular translocation of potassium, dextrose can be used alone (which stimulates endogenous insulin release and lessens risk for hypoglycemia) or in combination with regular insulin (which requires close patient monitoring for hypoglycemia).2,7,8 Unblocking the patient can also facilitate resolution of hyperkalemia and acid–base disturbances. Anesthetic protocols for cats with UO vary, based on preanesthetic blood work and patient condition at presentation.
An IV catheter should be placed in all cats. Cats with no additional medical conditions should receive chemical restraint9 with ketamine and a benzodiazepine and buprenorphine for analgesia before urinary catheter placement. Although buprenorphine has a slow onset (~30 min) following IV administration, it is long lasting, ideal for mild-to-moderate pain, and generally well tolerated by cats. In cats with a pathologic murmur, or history of UO requiring previous catheterization (resulting in a potentially more challenging catheterization because of scarring or chronic inflammation), oxymorphone or hydromorphone (± a benzodiazepine) should be given as premedication, followed by propofol for anesthetic induction. Critically ill, recumbent cats may not require chemical restraint for catheterization, but analgesic support with a previously mentioned opioid is recommended.
Dogs with UO often require general anesthesia for catheter placement, as blockage commonly occurs from cystic or urethral calculi. Hydromorphone or any available mu-agonist opioid should be given IM or IV, followed by propofol induction and inhalant anesthesia. In intubated patients, intermittent positive pressure ventilation (IPPV) to normocapnea (arterial PCO2 38–42 mm Hg) prevents the development of respiratory acidosis, a condition that increases blood potassium, worsening hyperkalemia.7 In dogs and cats without evidence of acute or chronic kidney disease, NSAIDs can be administered for pain management and to decreases urethral inflammation.

Successful pup recovery following dystocia
3. Dystocia
In patients undergoing cesarean section, anesthetic requirements are reduced (decreased minimum alveolar concentration) because of increased progesterone levels. Functional residual capacity is also reduced because the intraabdominal volume of the fetuses increases the possibility for atelectasis resulting in hypoxemia.10 In calm patients, IV catheter placement and initial abdominal clipping and prepping should be completed before anesthetic agents are administered. Premedication is not recommended, but a low dose of an opioid can be given if necessary to facilitate a smoother induction. α2-Adrenergic agonists, particularly xylazine, should be avoided as they have been linked to decreased survival in the neonate.11 Propofol, the induction agent of choice, crosses the placenta, but there is rapid clearance and minimal fetal depression occurs.7 Because of altered GI motility, pregnant patients are at increased risk for regurgitation and aspiration; care should be taken to protect the airway via intubation immediately after induction.
Presurgical injection of lidocaine and bupivacaine along the linea alba can lessen responses to the abdominal incision and can also provide some intra- and postoperative analgesia. Maintenance can be achieved with isoflurane or sevoflurane, and, if needed, occasional small boluses of propofol. Following delivery (Figure 1. Successful pup recovery following dystocia), buprenorphine should be administered IV to the dam. Although lower doses of full-agonist opioid IM or IV are acceptable, buprenorphine results in fewer postoperative adverse effects (ie, respiratory and cardiovascular depression, sedation) allowing the dam to quickly return to her offspring. Alternatively, a post-surgical morphine epidural7 can provide analgesia without significant postoperative depression for dam and neonates.7,10 If preoperative blood work is normal and mean blood pressure was maintained at or above 60 mm Hg during surgery, a single postoperative dose of carprofen or meloxicam can be administered to the dam. An opioid and postoperative NSAID combination is often adequate analgesia and is associated with minimal adverse behavioral effects in the dam and no adverse consequences in the newborn.
4. Proptosis
Proptosis is often caused by trauma; assessment for concurrent life-threatening injuries (ie, head trauma) is crucial. Because of the possibility for coexisting injuries, use of short-acting and/or reversible drugs is recommended. Premedication should include an opioid (one less likely to induce vomiting; see Gastric dilatation–volvulus) in combination with a benzodiazepine and anti-cholinergic (eg, glycopyrrolate, atropine) IM or IV. Anticholinergics are included in premedication of ocular patients for two reasons: 1) they reduce the risk that the surgeon may initiate the oculocardiac reflex, and 2) brachycephalic patients, a population with a high resting vagal tone, often present with proptosis. Induction with propofol allows smooth, rapid intubation. Maintenance can be achieved with isoflurane or sevoflurane. If head trauma has occurred, IPPV to maintain an end-tidal CO2 of 40 mm Hg is recommended to prevent increased intracranial pressure.2,7 Heart rate should be monitored closely while the patient is anesthetized. With onset of bradycardia or sinus arrest (because of the oculocardiac reflex), the procedure should be discontinued and atropine administered. Following enucleation, patients that are dysphoric during recovery should be sedated to reduce trauma to the surgical site. Low-dose acepromazine or dexmedetomidine allows a smoother recovery. Use of α2-adrenergic agonists is often reserved for recovery to avoid interference with anticholinergic administered before surgery. Postoperative pain management includes an opioid and an NSAID to reduce swelling and pain at the surgical site.

Surgical approach to hemoabdomen
5. Hemoabdomen
The hemoabdomen patient (Figure 2 Surgical approach to hemoabdomen) often presents in hypovolemic shock. Although definitive treatment is stopping the bleeding, hypovolemia should be treated preoperatively, and goals should include heart rate below 150 bpm, systolic blood pressure above 90 mm Hg, and, if possible, PCV at or above 20% and total solids at or above 4 g/dl.1,2 Treatment is based on hemorrhage cause (ie, trauma, neoplasia, rodenticide [nonsurgical]). Blood loss from trauma or a bleeding tumor requires surgery to stop hemorrhage before complete fluid resuscitation. Because hypovolemic patients have simultaneous RBC and protein loss, colloids and/or blood products are often required perioperatively. If blood loss exceeds 20% of the patient’s estimated blood volume or the PCV drops below 20%, whole or packed RBC transfusion is required. The anesthetic protocol and support measures outlined for GDV patients apply.