Top 5 Causes of Splenomegaly in Dogs
Todd Archer, DVM, MS, DACVIM (SAIM), Mississippi State University
Alyssa Sullivant, DVM, MS, DACVIM, Mississippi State University
The spleen is a complex organ composed of 2 distinct parenchymal areas (red pulp and white pulp), each with important hematologic and immunologic functions.
The red pulp filters blood and removes senescent or damaged blood cells, aids in the metabolism and subsequent recycling of iron, and serves as a site for hematopoiesis, producing leukocytes, platelets, and RBCs when demand is increased. Regions of white pulp consist of lymphoid tissue that produces and stores immune cells (eg, lymphocytes, macrophages), which provide immune surveillance of blood for “foreign” material (eg, cells harboring infectious organisms, antibody-coated cells that are targeted for destruction and removal from circulation). The spleen also acts as a reservoir of blood, storing up to 20% of the total RBC mass and up to 30% of the platelet mass in the body. The spleen releases RBCs and platelets readily to meet physiologic demand.
Splenic disorders are common in middle-aged and older dogs, with clinical signs ranging from vague signs of illness to life-threatening hemoabdomen. In these disorders, splenomegaly is often present, regardless of disease severity. Splenomegaly is typically caused by discrete nodule(s) or diffuse enlargement.1 Although splenomegaly can be present in the absence of clinical signs, patients with chronic splenic disease may exhibit lethargy, inappetence, vomiting, abdominal enlargement, and weight loss. Patients presented with hemoabdomen are often collapsed and in hypovolemic shock. Arrhythmias are common with splenic diseases, especially hemangiosarcoma.2 Splenomegaly may be detected on abdominal palpation or through imaging modalities such as radiography, ultrasonography, or advanced imaging. Imaging is useful for differentiating a splenic mass from diffuse splenomegaly and is important in narrowing the possible causes of splenomegaly.
The “two-thirds/two-thirds”2 and “fifty/fifty”3 rules are often cited regarding the incidence of splenic malignancy. In a study of 325 dogs, 66% of dogs with splenomegaly were diagnosed with splenic malignancy, and 65% of those malignancies were hemangiosarcoma.2 An earlier study of 1480 dogs found that approximately 50% of splenic samples represented malignancy, with hemangiosarcoma accounting for approximately 50% of malignancies.3 However, in a study of 105 dogs with nonruptured splenic masses, 70.5% had benign splenic lesions and 29.5% had malignant neoplasia, with hemangiosarcoma accounting for 58% of malignancies.4 Although splenic neoplasia is a common cause of splenomegaly, it is impossible to differentiate between malignant and benign lesions grossly. A definitive diagnosis should be obtained before considering euthanasia. Fine-needle aspiration of the spleen is safe, and cytologic diagnoses correspond to histologic diagnoses in at least 50% of cases.5-7 Submission of the entire spleen for histopathology is recommended to increase the likelihood of distinguishing between benign and malignant processes, particularly between hemangiosarcoma and hematoma.1
Following are the authors’ top 5 causes of splenomegaly seen most often in veterinary practice.
1. Hemangiosarcoma
Hemangiosarcoma is the most common malignant disease of the spleen, representing one-half to two-thirds of all malignant splenic tumors. It is more prevalent in older medium- and large-breed dogs (eg, German shepherd dogs, golden retrievers, Labrador retrievers, standard poodles).2,8 Hemangiosarcoma arises from the vascular endothelium and often develops into a large cavitary mass in the spleen (Figure 1). Approximately 25% of dogs with splenic hemangiosarcoma may have concurrent hemangiosarcoma affecting the right side of the heart.9 Clinical signs are typically related to anemia, which may be mild to severe and life-threatening, and include pale mucous membranes, tachycardia, lethargy, and abdominal distention.8 Intra- and extrasplenic hemorrhage may occur and can cause marked hemoabdomen and acute anemia with subsequent hypovolemia and collapse. Although hematomas and, less commonly, other benign splenic lesions may cause hemoabdomen, hemangiosarcomas are more likely to cause hemoabdomen.8 Blood study findings can include schistocytosis, thrombocytopenia, and, possibly, disseminated intravascular coagulation.

Hemangiosarcomas are the most common splenic malignancy in dogs.3 Lesions are often cavitary, and hemoabdomen is common.
Initial testing and staging should include CBC, serum chemistry profile, coagulation testing (prothrombin time and partial thromboblastin time), 3-view thoracic radiography, abdominal ultrasonography, and cardiac ultrasonography. Splenic aspirates may disclose malignant cells or evidence of nonspecific hemorrhage only, and a definitive diagnosis requires histopathology. Dogs with Stage I hemangiosarcoma have a solitary primary tumor less than 5 cm in diamter, and dogs with Stage II have a primary tumor that is ruptured, is greater than 5 cm in diameter, or has lymph node involvement.8 Stage III dogs have splenic rupture or lymph node involvement and evidence of distant metastasis.8 Survival times do not differ markedly between stages.8 Splenectomy alone yields a median survival time of 86 days, whereas dogs receiving adjunctive doxorubicin-based chemotherapy have a longer median survival time of 172 days if no evidence of gross disease is present after surgery.10
2. Extramedullary Hematopoiesis
Extramedullary hematopoiesis (EMH; ie, hematopoiesis occurring outside the bone marrow) causes diffuse uniform symmetric enlargement of the spleen (because of “work hypertrophy”) with increased activity of the mononuclear phagocytic system and increased blood cell production.10 Hypoxia is the main stimulus for splenic EMH in an adult animal11 and can be seen with any disease that undermines the ability of the bone marrow to function properly.
Because EMH is a benign condition that occurs in response to an underlying hematologic abnormality, diagnostic efforts are directed at the disease process driving the EMH. Mild EMH occurs with many splenic and nonsplenic disorders11 and can be seen with both immune-mediated hemolytic anemia and immune-mediated thrombocytopenia, as the spleen is a major site of removal and destruction of antibody-coated cells and a site for extramedullary production of blood cells. EMH can also be associated with a variety of splenic neoplasms. In patients with EMH, ultrasonography typically shows focal or diffuse, heterogenous nodules or masses within the spleen.4,6
Fine-needle aspiration of lesions yields a predominance of small lymphocytes.11 Myeloid and erythroid precursors may be seen, particularly in anemic patients (Figure 2).10 A concurrent CBC analysis is recommended to determine which hematologic abnormality is responsible for splenic EMH.11 Frequently, increased numbers of immature cells (eg, nucleated RBCs) may be seen in the circulation due to splenic EMH.11

Erythroid (arrow) and myeloid (arrowhead) precursors are common cytologic findings in splenic extramedullary hematopoiesis, particularly in response to anemia.11 Lymphocytes (asterisk) are also commonly seen.
3. Multicentric Lymphoma
Lymphoma is a systemic disorder of uncontrolled proliferation of neoplastic lymphoid cells. Multicentric lymphoma is the most common form of lymphoma in dogs, and the liver and/or spleen are frequently involved (Stage IV).12 Infiltration of neoplastic lymphoid cells often causes a diffuse enlargement of the spleen that results in a characteristic “honeycomb” or “moth-eaten” appearance on ultrasonography (Figure 3),13 which has a sensitivity of 100%, specificity of 23.3%, positive predictive value of 64.7%, negative predictive value of 100%, and accuracy of 68.1% for diagnosis of splenic lymphoma.13

Numerous, variably sized, sharply defined, hypoechoic nodules with a “honeycomb-like” appearance are characteristic of splenic lymphoma.
In one study, fine-needle splenic aspirate findings confirmed lymphoma in all multicentric lymphoma patients with a moth-eaten appearance of the spleen.13 Further differentiating lymphoma type (B-cell vs T-cell) using flow cytometry helps with prognosis. Treatment with chemotherapy is considered standard of care and is associated with 80% to 90% remission rates with median survival times of 10 to 12 months, depending on the chemotherapy protocol used.12
4. Nodular Hyperplasia/ Hematoma
Nodular hyperplasia and hematoma are thought to be a continuum of the same process, which starts as nodular hyperplasia and possibly results in formation of a hematoma.10 Hyperplastic nodules are benign masses that typically cause discrete abnormal areas in the spleen. During ultrasonography, hyperplastic nodules appear as focal or diffuse discrete hyperechoic, hypoechoic, or isoechoic masses—which may or may not cause shadowing—in the spleen. They may cause an irregular splenic border, but rarely do hyperplastic nodules distort, or bulge, the splenic capsule. These nodules cannot be distinguished from neoplasia by ultrasonography alone.14,15 They consist of a benign accumulation of cells normally found in the spleen, including lymphoid, hematopoietic, and plasmacytic cellular infiltrates, and develop in response to antigenic stimulation from a variety of inflammatory or neoplastic conditions.11 One study suggested that a hematoma may develop when blood flow (out of the spleen) is disrupted by hyperplastic nodules.3
Hematomas consist of hemorrhage and organized fibrin and are the most common benign splenic lesion (Figure 4).2,3 Although uncommon, some hyperplastic nodules, especially large hyperplastic nodules, may distort or bulge the splenic capsule. Hemoabdomen may also occur, but the incidence is markedly lower than in hemangiosarcoma.2 Surgical excision is indicated for hematomas and hyperplastic nodules large enough to cause splenomegaly, with excision being curative. Because hematomas may develop in neoplastic tissue, submission of the entire spleen for histopathology is crucial to minimize the risk for misclassifying a malignant neoplasm as a hematoma.16

Splenic hematomas are the most common benign splenic mass. They may be quite large and are grossly indistinguishable from hemangiosarcoma.
5. Congestion
Splenic congestion has numerous causes, including sedation, anesthesia, thrombosis, right-sided congestive heart failure, splenic torsion, and portal hypertension. Splenic congestion may cause severe splenomegaly and clinical signs, as the spleen is capable of pooling up to 30% of blood volume.10 Smooth muscle relaxation may be responsible for drug-induced splenic congestion, which is transient and may be limited to certain drugs (eg, phenothiazine sedatives, ultrashort-acting barbiturates).17 Administration of acepromazine, thiopental, or propofol produces marked splenomegaly.18 Severe hepatic disease may lead to portal hypertension and subsequent splenomegaly. Increased systemic hydrostatic pressure from right-sided congestive heart failure or increased splenic vein hydrostatic pressure because of thrombosis may cause splenic congestion.
Treatment of the underlying disease in these conditions may relieve or reduce splenomegaly. In cases of splenic torsion (Figures 5 and 6), splenectomy is the recommended treatment, with approximately 90% of dogs surviving to discharge.19


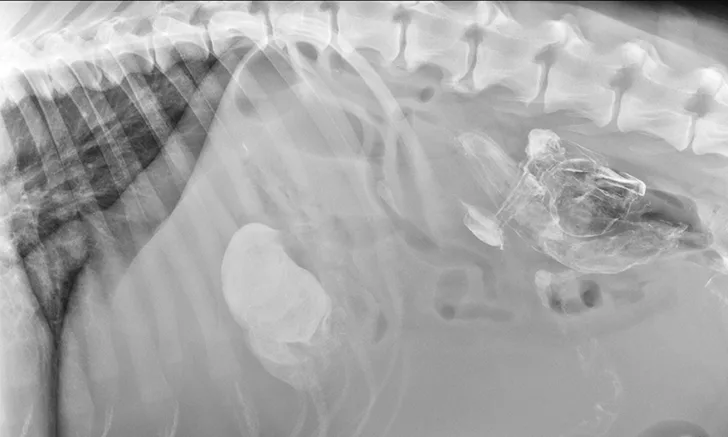
Splenic torsion appears as a large soft-tissue opacity that displaces the GI tract caudally and peripherally (A). The splenic head is obscured caudal to the left margin of the stomach (B). The metallic opacity seen in the stomach and intestines is caused by recent barium administration.

The spleen is markedly enlarged, hypoechoic, and lacy, with hyperechoic patches surrounding the hilus. A perivenous hyperechoic triangle at the splenic hilus is continuous with the mesentery, and no flow is present on Doppler. These findings are often associated with splenic torsion.20