Top 5 Bone & Joint Antibiotics to Consider Before Culture Results
Mary Sarah Bergh, DVM, MS, DACVS, DACVSMR, Midwest Veterinary Specialists, Milwaukee, Wisconsin
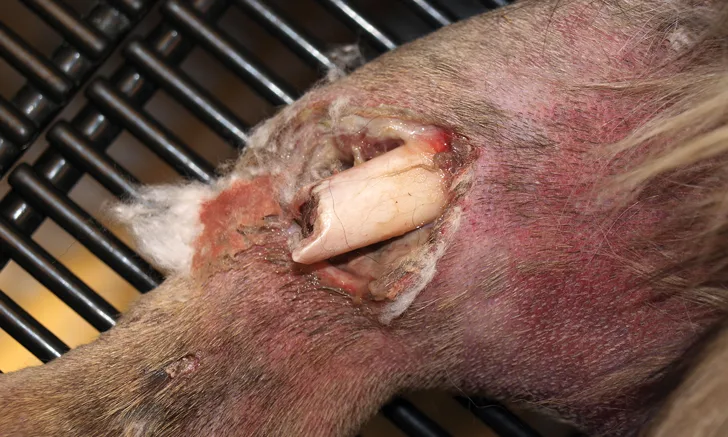
Bone and joint infections may arise from direct inoculation (eg, a penetrating wound or surgery), extension from soft tissue infection, or, less commonly, hematogenous spread.1,2 In most cases, the result is a painful and debilitating condition that warrants aggressive therapy to alleviate discomfort and promote musculoskeletal health. Necrotic bone, soft tissue, and fibrinous material—as well as biofilms and implants—are often associated with these infections and can complicate treatment. Thus, joint lavage and/or wound debridement are often necessary in combination with oral, IV, or even local antibiotic delivery.3-5
Antibiotic therapy optimally should be based on bacterial culture and susceptibility testing of specimens from the suspected infected area. When antibiotics are initiated before culture results are available, the drug should be empirically chosen based on the suspected organism type, infection location, and patient factors.5 The most common bacteria isolated from bone and joint infections include Staphylococcus spp, Streptococcus spp, Escherichia coli, and Pasteurella spp (Table).1-8
Table: Common Bacteria in Bone & Joint Infections
Most antibiotics achieve acceptable levels in synovial fluid and bone, and some achieve higher levels in inflamed or infected bone or joint tissue.8-11 Based on principles of good antimicrobial stewardship, it is important to select an antibiotic that will minimize the impact on public health. Antibiotics—including some fluoroquinolones, third- or fourth-generation cephalosporins, carbapenems, glycopeptides, and oxazolidinones—are used to treat antimicrobial-resistant organisms in humans. Their use in veterinary medicine should be justified by the absence of alternatives.
Appropriate choices for empiric therapy depend on the inciting source of bacterial contamination and could include cephalexin, clindamycin, amoxicillin–clavulanic acid, enrofloxacin, and cefpodoxime. Other antibiotics may be appropriate based on culture and susceptibility testing of the bone or joint tissue.
1. Cephalexin
Cephalexin is a good first-line choice for treating many bone and joint infections because it is bactericidal, is effective against the most common skin pathogens, and achieves good penetration in both normal and osteolytic bone.12,13 Cephalexin is a first-generation cephalosporin that kills bacteria by disrupting peptidoglycan synthesis in the bacterial cell wall. It is predominantly effective against gram-positive bacteria such as Staphylococcus spp and Streptococcus spp.
Cephalexin has generally poor activity against gram-negative bacteria. Most anaerobes are susceptible to first-generation cephalosporins, with the exception of Bacteroides spp. First-generation cephalosporins can also be efficacious against gram-negative organisms such as Proteus mirabilis, some E coli, and Klebsiella spp.
There is no activity against Pseudomonas spp or Enterococcus spp. Cephalexin is FDA-approved for dogs (22 mg/kg PO q12h) and is typically used extra-label in cats.13
2. Clindamycin
Clindamycin has great bone penetration; however, as a lincosamide antibiotic, it is bacteriostatic and, therefore, should not be given in combination with a bactericidal drug. Clindamycin affects bacteria via inhibition of protein synthesis of the bacterial ribosome and has excellent activity against most pathologic anaerobic bacteria; most aerobic gram-positive cocci (eg, staphylococci, streptococci) are also susceptible. This drug is often effective against Corynebacterium spp, Nocardia asteroides, and Mycoplasma spp. It is FDA-approved for treating osteomyelitis (Figure) in dogs (11-33 mg/kg PO q12h) and cats (11-33 mg/kg PO q24h).13

Craniocaudal radiograph of a postoperative (8 weeks) open tibial fracture with tibial/fibular osteomyelitis. Note the large degree of soft tissue swelling, spiculated periosteal response (yellow arrows), sequestrum (blue arrows), and loose transfixation of the pin on the external skeletal fixator (orange arrow). Successful treatment of this patient’s infection required a multimodal approach including removal of the sequestrum, debridement of necrotic material and biofilm, removal and replacement of the loose transfixation pin, and antibiotics based on culture and susceptibility testing of deep wound tissue.
3. Amoxicillin–Clavulanic Acid
Amoxicillin–clavulanic acid is a potentiated penicillin with β-lactamase–inhibiting effects, which are induced by the clavulanic acid. It is effective against gram-positive and gram-negative aerobic and anaerobic bacteria (ie, Staphylococcus aureus, Staphylococcus pseudintermedius, Staphylococcus spp, other Streptococcus spp, E coli, Pasteurella spp) and is the antibiotic of choice for treating infections caused by bite wounds of cats or dogs.14 Amoxicillin–clavulanic acid is not effective against Pseudomonas spp or Enterobacter spp. It is FDA-approved for dogs (13.75 mg/kg PO q12h) and cats (62.5 mg PO q12h).13
4. Enrofloxacin
Enrofloxacin is a bactericidal fluoroquinolone only available in the veterinary market. It is effective against a broad spectrum of gram-negative and gram-positive bacteria but is not effective against anaerobes. Its mechanism of action is believed to be through inhibition of bacterial DNA gyrase, which prevents bacterial DNA supercoiling and synthesis. Enrofloxacin is effective against most Pseudomonas spp, Klebsiella spp, E coli, Enterobacter spp, Campylobacter spp, Proteus spp, and Staphylococcus spp, among others. This antibiotic should be avoided in juvenile dogs, as it may induce abnormalities in cartilage development. It is FDA-approved for dogs (5-20 mg/kg PO q24h) and cats (5 mg/kg PO q24h).13
5. Cefpodoxime
Cefpodoxime is a third-generation cephalosporin. It is less effective than cephalexin against gram-positive bacteria but has a broader effect on gram-negative organisms, including Enterobacteriaceae (eg, Proteus spp, E coli, Klebsiella spp). However, it is not effective against Pseudomonas aeruginosa, Enterococcus spp, or Bacteroides fragilis. In addition to good musculoskeletal penetration, cefpodoxime has good CNS penetration. It is FDA-approved for dogs (5-10 mg/kg PO q24h) and is typically used extra-label in cats.13
Conclusion
Antibiotic therapy plays an important role in the comprehensive treatment of bone and joint infections in cats and dogs. Successful identification of the underlying cause of infection, isolation of the pathologic bacteria, and debridement of the wound to remove necrotic tissue and biofilm-covered material are often needed to resolve the infection. Empiric therapy should be based on the cause of the infection and the suspected bacterial organisms. Bacterial culture results may indicate the need to change antibiotic therapy.
When antimicrobial susceptibility results indicate that several antibiotic choices are efficacious against the pathologic organism, antibiotic selection should be based on the efficacy of the drug, the degree of tissue penetration, side effects, route of administration, and cost. Great care should be taken to select antibiotics that minimize the ongoing development of antibiotic resistance in human and animal medicine.