Surgical Treatment for Aural Hematoma
Karen M. Tobias, DVM, MS, DACVS, University of Tennessee
Rachel Seibert, DVM, University of Tennessee
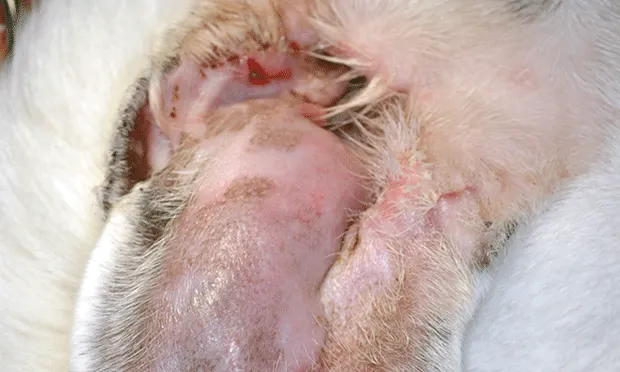
Branches of the caudal auricular artery passing from the convex to the concave surface of the pinna through tiny channels within the cartilage provide blood to the auricular cartilage. Normally, the concave surface of pinna cartilage is firmly attached to the skin, but trauma may create dead space between the cartilage and skin that fills with blood. Hemorrhage from the penetrating vessels continues, ultimately forming an out-pouching (ie, aural hematoma). If untreated, granulation tissue replaces aural hematomas; subsequent contraction and fibrosis of this tissue can result in pinnal deformity and, in cats, obstruction of the external acoustic opening.
Aural hematomas can be caused by direct damage (eg, bite wounds, vehicular trauma) but are more common from head shaking and ear scratching associated with otitis externa or atopy. Affected animals should undergo thorough dermatologic and otoscopic examinations, and any underlying disease should be treated to facilitate resolution and prevent recurrence.
Treatment
Aural hematomas can be treated surgically or nonsurgically. Therapeutic goals include removal of contents, maintenance of apposition between skin and cartilage, and appropriate treatment for the source of head shaking or scratching. Drainage should be performed expeditiously to prevent contracture, fibrosis, and subsequent deformity.
Surgical options include placement of an active or passive drain or fenestration on the concave skin of the pinna, using either a single long incision or multiple small incisions, to empty the pocket and prevent recurrence of fluid accumulation. Apposition of skin to cartilage is maintained by placement of sutures between skin and cartilage, application of a compressive bandage, or both. Drains are removed within 1 week, but bandaging may be required for 2 additional weeks.
Nonsurgical treatment involves needle drainage and flushing of the hematoma cavity. Recurrence is common with needle drainage alone, even if bandages are applied, but treatment with systemic or intralesional steroids reduces recurrence. For needle drainage, the concave surface of the pinna should be clipped and aseptically prepared. A 14- or 16-gauge needle or 19- or 21-gauge butterfly catheter is inserted into the dependent portion of the hematoma and directed into the pocket (Figure 1). For floppy-eared dogs, the needle is inserted into the end of the hematoma near the pinna apex so fluid draining from the needle hole does not enter the ear canal.

A butterfly catheter used to remove fluid from the hematoma cavity.
Fluid is drained, and the pocket is flushed with sterile saline to remove clots. Steroids can be injected into the hematoma cavity before bandage placement. Because of the antiinflammatory effects of glucocorticoids, local steroid injection can predispose abscess formation; use of sterile technique is extremely important with intralesional infusion. Successful resolution has been reported in 90% of animals with drainage followed by injection of intralesional triamcinolone acetonide (10 mg/mL; 0.1–1 mL q7d for 1–3 treatments) or dexamethasone (0.2–0.4 mg diluted to 0.5–1.8 mL, infused q24h for 1–5 days).1-3 Bandaging is still recommended to prevent damage during continued head shaking or scratching. Resolution of hematomas with drainage followed by IV administration of immunosuppresive dose of glucocorticoids has also been described1; however, this treatment is not recommended because of potential adverse events.
Closed-Suction Drains
Closed-suction drainage using a butterfly catheter and vacutainer tube may inexpensively prevent or resolve SC fluid accumulation. In active patients, the tube and catheter must be carefully secured to prevent accidental needle dislodgement. The owner can be taught to change the vacutainer tube when it has filled or lost negative suction and to monitor fluid production. Drains are usually removed within 5 to 7 days of placement; the ear can be bandaged for another week to prevent disruption from head shaking or scratching. Closed-suction drainage works for acute or chronic hematomas that have fluid accumulation, as long as the underlying cause is treated. Most patients show resolution in 7 to 10 days with minimal pinna distortion. Recurrence rates are 22%, with recurrence reported in animals with uncontrolled allergic dermatitis.3
Step-by-Step: Continuous Suction Drainage
What You Will Need
#40 clipper blade
Chlorhexidine scrub and solution
Butterfly catheter (19- or 21-gauge)
Mayo scissors
Sterile gloves
Needle drivers
#11 or #15 surgical blade
2-0 or 3-0 monofilament suture
Tongue depressors
White adhesive tape
Bandage material
Vacutainer blood tubes (bd.com)

Step 1
Cut the syringe adaptor from the butterfly catheter (A). Fold over the tubing near the cut end, and snip off the corner of the fold with Mayo scissors to create a fenestration (B). Add several fenestrations to the terminal 1.5–2 cm of the tubing, making sure that fenestrations are less than half the diameter of the tubing to prevent accidental breakage (C).
Author Insight
Leave some fluid in the hematoma to permit stab incision into the fluid pocket.

A
Step 2
Clip and vacuum the pinna, and place cotton or gauze in the ear canal to prevent fluid accumulation. Aseptically prepare the surgical site with chlorhexidine scrub and solution. If desired, drain some fluid from the hematoma with a needle and syringe. With the tip of a #11 blade, make a small stab incision into the hematoma cavity; alternatively, use a large-gauge–needle or small-skin–punch that is the same diameter as or slightly larger than the drain tubing. The incision should only be large enough for tube placement. If desired, flush the hematoma through the incision to remove any clots or fibrin.

Step 3
Using a needle holder or hemostat, insert tubing into the hematoma cavity. Ensure all fenestrations are located within the cavity. Place a purse string suture in the skin around the tubing exit site to maintain negative pressure.

Step 4
Secure the tube to the ear with a finger trap suture pattern. Use surgeon’s throws where the suture crosses the tubing. Tie these carefully so they grip the tubing without kinking or compressing it. After tying off the finger trap pattern, take a final bite through the skin to finish securing the tube.

Step 5
Insert the needle end of the butterfly tubing into the vacutainer tube to create a closed seal and active drainage. Once the tube has partially filled, the vacuum on the drain will be lost. Kink off the drain, remove the needle from the vacutainer tube, and place it in a new tube to reestablish active suction. The vacutainer tube may need to be changed 2 or 3 times immediately after drain placement. After, it can be changed q24h or when the tubes are half full.

Step 6
Position the pinna apex dorsally to expose the external ear canal and concave surface of the pinna. Place a long strip of white adhesive tape along the haired surface of each pinna margin (adhesive side facing outward); carefully wrap each strip around the neck or chin and back to the ear margin and stick it to the exposed adhesive. Use tongue depressors to prevent the tape from sticking together during placement. Tape should be loose enough to prevent neck constriction.

Step 7
If desired, place a padded, full-head bandage, leaving an opening over the ear canal for topical medications. Bandage around the exposed, unaffected ear to prevent slippage and allow treatment of that ear as well. Make sure the bandage is loose enough to avoid facial swelling or respiratory compromise. Tape the vacutainer tube to the bandage or neck collar for easy changes. Have the caretaker label each vacutainer tube with the date and time. The fluid volume should decrease over several days.
