Staging & Management of Feline Chronic Kidney Disease
ProfileDefinitionLoss of functional renal tissue (nephrons) due to a chronic (> 2 month) disease process
Systems. Renal
Genetic Implications. Medullary amyloidosis in Abyssinians and polycystic kidney disease in Persians are examples of heritable feline CKD.
Incidence/Prevalence. 1% to 3% of all cats; in geriatric populations at referral institutions, CKD may affect up to 35% of cats.
Geographic Distribution. Worldwide
SignalmentSpecies. Feline
Breed Predilection. See the heritable examples listed above.
Age and Range. All ages can be affected; however, most CKD is acquired and therefore more common in geriatric cats (> 8 years).
Gender. No difference has been reported.
Causes & Risk FactorsCauses are often difficult to determine since the structural and functional endpoint of irreversible nephron damage is the same. Renal diseases that have been associated with the development of CKD in cats include amyloidosis, glomerulonephritis, primary tubulointerstitial disease, ascending urinary tract infections (bacterial pyelonephritis), nephrolithiasis, polycystic kidney disease, feline infectious peritonitis, and neoplasia.
Typical gross appearance of chronic kidney disease. Note the irregular borders and "lumpy-bumpy" surface.
PathophysiologyNephron damage associated with CKD is usually irreversible and can be progressive (stage I and early stage II CKD may not be progressive, but later stage II to IV is almost always progressive). Renal failure results when three quarters or more of the nephrons of both kidneys are not functioning. Whether the underlying CKD primarily affects glomeruli, tubules, interstitial tissue, or renal vasculature, irreversible damage to any portion of the nephron renders the entire nephron nonfunctional. Healing of irreversibly damaged nephrons occurs by replacement fibrosis.
Progressive diseases that destroy nephrons at a slow rate allow intact nephrons to undergo compensatory hypertrophy which can delay the onset of renal failure. When renal failure finally occurs, the nephron hypertrophy can no longer maintain adequate renal function and < 25% of the original nephrons are functional.
The pathophysiology of CKD can be considered at both the organ and systemic level. At the level of the kidney, the fundamental pathology of CKD is loss of nephrons and decreased glomerular filtration. Reduced glomerular filtration results in increased plasma concentrations of substances that are normally eliminated from the body by renal excretion (eg, creatinine, urea nitrogen, and phosphorus). In addition to excretion of metabolic wastes and maintenance of fluid and electrolyte balance, the kidneys also function as endocrine organs and catabolize several peptide hormones. Thus, hormonal disturbances also play a role in the pathogenesis of CKD. Examples include decreased production of erythropoietin, which contributes to the nonregenerative anemia of CKD, decreased metabolism, and excretion of parathyroid hormone and gastrin, which contribute to osteodystrophy and gastritis, respectively.
Finally, part of the pathophysiology of CKD is brought about by compensatory mechanisms. For example, osteodystrophy occurs secondary to hyperparathyroidism, which develops in an attempt to maintain normal plasma calcium and phosphorous concentrations. Similarly, the individual glomerular filtration rate of intact nephrons increases in CKD in an attempt to maintain adequate renal function; however, proteinuria and glomerulosclerosis may be consequences or "trade-offs" of this hyperfiltration.
SignsHistory. Dependent on the stage of CKD (see Table 1). History is often unremarkable in stage I and early stage II. In later stage II and beyond, history may include anorexia, weight loss, vomiting, polydipsia, and polyuria.
Physical examination**. Dependent on the stage of CKD (see Table 1**). Physical exam may be normal in stage I and early stage II. In later stage II and beyond, findings may include dehydration; poor body condition; uremic breath; oral ulcers; and small, firm, irregularly-shaped kidneys. Hypertensive retinopathy is possible.
Pain IndexIn general, the kidneys of cats with CKD are not painful (exceptions may include lymphosarcoma causing renal swelling and the presence of nephroliths or ascending infections). Gastrointestinal irritation can result in mild to moderate pain; oral ulcers may be quite painful.
Diagnosis
Definitive DiagnosisDefinitive diagnosis is traditionally based on loss of > 75% of the patient's nephrons, resulting in persistent azotemia superimposed on an inability to concentrate urine (USG < 1.035 to 1.040) along with chronic clinical signs of weight loss and polydipsia/polyuria. Preazotemic CKD may also be diagnosed in cats with persistent renal proteinuria, urine concentrating deficits, increases in serum creatinine over time even if the values remain in the normal range (eg, serum creatinine that increases from 0.6 to 1.2 mg/dl could indicate a 50% reduction in GFR), or renal abnormalities noted on palpation or ultrasound. The International Renal Interest Society (IRIS) has developed a staging system for feline CKD; it is based primarily on serum creatinine concentrations in stable, well-hydrated cats (Table 1).
Ultrasound image of kidney demonstrating pyeloectasia, which may indicate an ascending urinary tract infection.
Serum creatinine concentrations should always be interpreted in light of the patient's USG, muscle mass, and physical examination findings in order to rule out pre- and postrenal causes of azotemia. The stages are further classified by the presence or absence of proteinuria and systemic hypertension in Table 2.
Differential DiagnosesHyperthyroidism, diabetes mellitus, FeLV-associated disease, primary gastrointestinal disease, neoplasia
Laboratory Findings/ImagingIn addition to the azotemia and inability to concentrate urine, nonregenerative anemia, hypokalemia, metabolic acidosis, and hyperphosphatemia are frequently observed. Small and irregularly shaped kidneys are often observed on radiographs and renal ultrasound findings may include increased cortical echogenicity with loss of the corticomedullary junction. Ascending infections may result in pyeloectasia on ultrasound and calcium oxalate nephroliths may be observed by radiographs and/or ultrasound.
Urinary tract infections are common in cats with CKD (especially female cats); therefore, urine cultures should be part of the initial and follow-up diagnostics. Fundic examination may reveal changes consistent with systemic hypertension (vessel tortuosity, hemorrhage, retinal detachment).
Postmortem FindingsGastrointestinal tract irritation (mucosal ulceration); small, fibrotic kidneys; evidence of renal secondary hyperparathyroidism (soft tissue mineralization and osteodystrophy)
Renal histology: Morphologic heterogeneity between nephrons exists in CKD with changes ranging from severe atrophy to marked hypertrophy. Histologic changes are not process specific and, therefore, an etiologic diagnosis is frequently not possible.
TreatmentInpatient or Outpatient
Depends on the severity of the patient's clinical signs. Many cats with CKD are better suited to outpatient treatment versus hospitalization.
ActivityUnrestricted
Client EducationCKD in cats is irreversible and often progressive. Frequent rechecks of the patient's body weight, hydration status, blood pressure, and laboratory parameters are often necessary. Medications and diet therapy require a high level of owner/patient compliance.
SurgeryUsually indicated only for obstructive uropathy
Medications & Nutritional AspectsIn early to mid-stage CKD, specific treatment aimed at the primary underlying disease is important and may include antibiotics for ascending urinary tract infections, chemotherapy for lymphosarcoma, and surgery to relieve ureteral obstruction. Renoprotective treatments aimed at stabilizing any renal functional decline are also important in early to mid-stage CKD and may include renal diets (protein and phosphorous reduction, alkalinization, omega-3 fatty acid supplementation), enteric phosphate binders, antihypertensive drugs (eg, calcium channel antagonists and ACE inhibitors), and antiproteinuric drugs (ACE inhibitors).
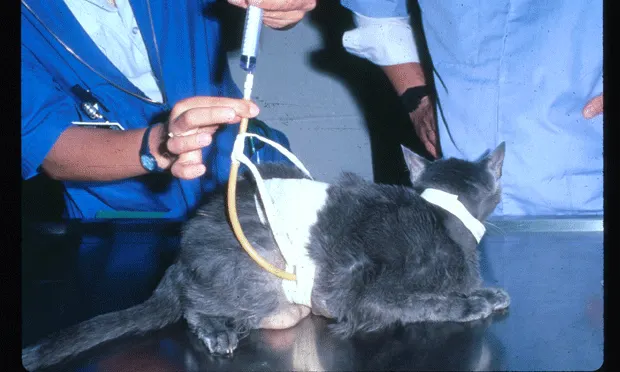
Cat with gastrostomy feeding tube.
In the latter stages of CKD, treatments designed to relieve clinical signs become more important; examples include SC or IV fluids to correct dehydration, potassium supplementation, recombinant erythropoietin, antiemetics/antacids/gastrointestinal protectants, and feeding tube placement.
ContraindicationsPotentially nephrotoxic drugs, glucocorticoids
PrecautionsTry to avoid sudden dietary change and stressful hospitalization.
InteractionsDiuretics, especially furosemide, may potentiate the effects of potential nephrotoxicants
Alternative TherapyRenal replacement therapy (eg, dialysis and renal transplantation)
Follow-UpPatient MonitoringMay range from 2 to 4 times/year in early stage CKD to several times per week in latter stage CKD.
PreventionAnnual wellness exams are recommended to diagnose early stage CKD; this is the time when disease-specific and renoprotective treatments have the best opportunity for success.
ComplicationsAscending infections, nephroliths, hypertension, proteinuria, gastrointestinal tract irritation, nonregenerative anemia, metabolic acidosis, potassium depletion
CourseStage I and early Stage II CKD may be stable or progressive; later Stage II through Stage IV CKD is often progressive.
In GeneralRelative Cost
Initial diagnosis and staging $$ (relatively speaking, the earlier the stage, the less expense for diagnosis and treatment)
Disease specific treatment ranges from $ for antibiotic treatment to $$$ for surgery for relief of obstructive uropathy
Renoprotective treatment and follow-up $$ (on an annual basis)
Treatment for clinical signs and follow-up $$ to $$$ (on an annual basis)
PrognosisGuarded, as CKD is irreversible and in many cases progressive.
Future ConsiderationsEnteric dialysis may play a role in relieving clinical signs in later stage CKD.
STAGING & MANAGEMENT OF FELINE CHRONIC KIDNEY DISEASE • Gregory Grauer
Suggested ReadingAssessment and management of proteinuria in dogs and cats: 2004 ACVIM Forum Consensus Statement (small animal). Lees GE, Brown SA, Elliott J, et al. J Vet Intern Med 19:377-385, 2005.Chronic renal disease in cats. Krawiec D, Gelberg H. In RW Kirk (ed): Current Veterinary Therapy X-Philadelphia: WB Saunders, 1989, pp 1170-1173.Comparison of conventional urine protein test strips and a quantitative ELISA for the detection of canine and feline albuminuria. Grauer GF, Moore LE, Smith AR, et al. J Vet Intern Med 18:418A-419A, 2004.Effect of dietary phosphate restriction on renal secondary hyperparathyroidism in the cat. Barber PJ, Rawlings LM, Markwell PJ, Elliott J. J Small Anim Pract 40:62-70, 1999.Effects of the angiotensin-converting enzyme inhibitor benazepril in cats with induced renal insufficiency. Brown SA, Brown CA, Jacobs G, et al. Am J Vet Res 62, 375-383, 2001.Effects of the calcium channel antagonist amlodipine in cats with surgically induced hypertensive renal insufficiency. Mathur S, Syme H, Brown CA, et al. Am J Vet Res 63:833-839, 2002.Feline hypertension: Clinical findings and response to antihypertensive treatment in 30 cases. Elliott J, Barber PJ, Syme HM, Rawlings JM. J Small Anim Pract 42:122-129, 2001.Hypertension in cats with chronic renal failure or hyperthyroidism. Kobayashi DL, Peterson ME, Graves TK, et al. J Vet Intern Med 4:58-62, 1990.Incidence and prevalence of bacterial urinary tract infections in cats with chronic renal failure. Barber PJ, Rawlings JM, Markwell PJ, et al. J Vet Intern Med 13:101A, 1999.Prevalence of systolic hypertension in cats with chronic renal failure at initial evaluation. Syme HM, Barber PJ, Markwell PJ, Elliott J. JAVMA 220:1799-1804, 2002.Relation of survival time and urinary protein excretion in cats with renal failure and/or hypertension. Syme HM, Elliott J. J Vet Intern Med 17:405A, 2003.Survival of cats with naturally occurring chronic renal failure: Effect of dietary management. Elliott J, Rawlings JM, Markwell PJ, Barber PJ. J Small Anim Pract 41:235-242, 2000.Update: Conservative medical management of chronic renal failure. Polzin DJ, Osborne CA. In Kirk RW (ed): Current Veterinary Therapy IX-Philadelphia: WB Saunders, 1986, pp 1167-1173.Urinary protein excretion in cats with renal failure and/or hypertension. Syme HM, Elliott J. J Vet Intern Med 17:405A, 2003.
ResourcesInternational Renal Interest Society: www.iris-kidney.com