Smoke Inhalation
Selena L. Lane, DVM, DACVECC, University of Georgia
Background & Pathophysiology
Smoke inhalation is a significant cause of morbidity and mortality in patients involved in a fire and can cause severe respiratory compromise and acute lung injury, although this is uncommon.1 Patients with smoke inhalation are often presented with upper airway obstruction, bronchospasm, secondary pneumonia, and even respiratory failure.2 In instances of fire exposure, patients may have concurrent injuries (eg, thermal burn injury) and should be assessed for respiratory difficulty and hemodynamic stability on presentation.
Smoke inhalation often leads to severe respiratory injury, including airway obstruction, hypoventilation, acute respiratory distress syndrome, and pneumonia.3,4 Direct heat injury and release of inflammatory mediators in the upper airway can result in damage to the upper respiratory tract, which can cause further swelling and edema of local tissue in the tongue, oropharynx, and epiglottis and can lead to airway obstruction.5 Injury to the lower airway is generally caused by inhalation of irritants, including soot (ie, particulate matter produced by fire).5 Soot adheres to the tracheal mucosa and disrupts standard defense mechanisms, allowing other chemical and physical irritants to become trapped in the mucosal surface.6 Injury in the respiratory tract mirrors the pathophysiology of injuries caused by thermal burns, including upregulation of inflammation and release of reactive oxygen species, edema formation, fluid exudation into the airway, and bronchoconstriction.5-8 Sloughing of bronchial epithelial cells and damage to the ciliary mucosa can cause disruption of the lower airways, which can lead to plugging of the bronchioles and alveoli and increase the risk for secondary infection.5 Airway plugging results in hypoxemia secondary to atelectasis and ventilation-perfusion mismatch.2,5
Patients with smoke inhalation often have systemic effects of carbon monoxide (CO) and cyanide (CN) toxicity.1,6,9 CO is the most commonly inhaled gas associated with complications in these patients and can lead to an inability to offload oxygen to tissues due to hemoglobin’s increased affinity for CO as compared with oxygen.2,6 CN toxicity results in tissue hypoxia secondary to inhibition of oxidative phosphorylation that affects the respiratory, neurologic, and cardiovascular systems.2 Inhalation of toxic gases can lead to acute and delayed neurologic signs.10-12 Few reports exist regarding the neurologic and respiratory effects of smoke inhalation in companion animals; however, results suggest that treatment for multiple major complications secondary to smoke inhalation has been successful.10-14 Patients may die from hypoxia or CO or CN toxicity if not treated promptly.
History
Patients with smoke inhalation were typically involved in a fire that occurred in an enclosed space (eg, residential home or apartment). It is important to ask the pet owner (if available) for a complete medical history and how long the patient was exposed to the fire. The owner or rescue personnel can also be asked whether other relevant clinical signs (eg, excessive cough, dyspnea, collapse, neurologic dysfunction, known burn injuries) were noted prior to presentation.
Clinical Signs
The patient may smell strongly of smoke on presentation. Significant signs of airway damage (eg, upper airway obstruction, respiratory distress) may not be present shortly after exposure to fire; however, life-threatening complications can develop quickly, and the patient should be closely monitored.
The extent of physical examination abnormalities will depend on the severity and duration of smoke inhalation, as well as any treatment administered prior to presentation (eg, oxygen supplementation by rescue personnel). Initial findings may include thermal burn injury to the skin, singed hair or whiskers, soot in the oral cavity or on the fur, oromucosal burns, and/or edema. More significant respiratory signs (eg, oral or facial edema, stridor, wheezing, dyspnea, cyanosis or cherry-red mucous membranes, wheezes, crackles, open-mouth breathing, orthopnea) may be seen in patients with severe respiratory injury or concurrent CO or CN toxicity. The patient may have altered mentation (ranging from a dull to comatose appearance) and/or other neurologic signs, including ataxia or seizures. Delayed neurologic signs have been reported in dogs up to 6 days after smoke inhalation.11,15 Cats are most often presented with signs of lethargy.16
Respiratory signs can take >24 hours to develop, as airway edema usually progresses in the first 72 hours.5 Endotracheal intubation is indicated if there are signs of airway obstruction (eg, progressive swelling, stridor, dyspnea). Mechanical ventilation may be required in cases of severe pulmonary damage. The patient should be evaluated repeatedly during hospitalization, particularly in the first 72 hours, to ensure early signs of airway obstruction are not missed. Indications for intubation are airway obstruction, neurologic decline, or crucial burn injury that affects the face, airway, or oropharynx.17 The literature suggests dogs and cats not presented with signs of respiratory abnormalities at admission often do not develop substantial complications.13,16
Other clinical signs are directly related to the severity of hemodynamic compromise and concurrent burn injuries. Rectal temperature may vary.13,18 Ophthalmologic examination with fluorescein staining is warranted to rule out corneal ulcers or burn injury to the eye. The mucous membranes or skin may appear cherry red if the patient is concurrently experiencing CO or CN toxicity. Patients with smoke inhalation often have normal to hyperemic mucous membranes with hyperemia secondary to carboxyhemoglobinemia, distributive shock, and systemic vasodilation.13
Diagnosis
Smoke inhalation is diagnosed in patients that have a history of exposure to smoke and fire events. The index of suspicion for smoke inhalation injury is increased with identification of burns associated with the oral cavity or face, soot in the oral cavity, or soot particles on cytology of saliva. Patient history, physical examination, and clinical findings can confirm diagnosis.
Measures of hypoxemia (eg, arterial blood gas analysis, pulse oximetry) and thoracic radiography can also support a definitive diagnosis. Arterial blood gases allow identification of hypoxemia (partial pressure of oxygen [PaO2], <60 mm Hg) and impaired ventilation (partial pressure of carbon dioxide [PaCO2], >60 mm Hg). Pulse oximetry is often used during the initial examination; however, if the patient has CO or CN toxicity, the oxygen saturation of peripheral blood may appear normal due to the inability of the device to differentiate between carboxyhemoglobin and oxyhemoglobin. If available, co-oximeters can be used to measure specific hemoglobin species and oxygenation status and may be more useful than pulse oximetry alone in patients with both pulmonary injury and CO or CN toxicity. Patients may also have metabolic acidosis (predominated by hyperlactatemia secondary to systemic hypoxia) or respiratory acidosis (associated with hypoventilation).
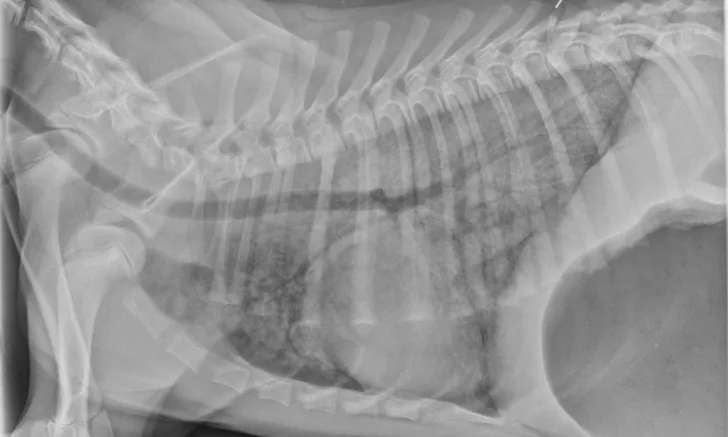
Thoracic radiographs can appear normal initially, but changes to the pulmonary parenchyma may become more apparent within 24 to 72 hours as respiratory injury progresses. Evidence of patchy pulmonary edema with bronchial, interstitial, or alveolar patterns may be observed [Figures 1 and 2].6,13,16,19 Right middle lung lobe consolidation and pleural effusion in cats have been reported.6,13,16 An alveolar pattern may be seen on serial radiographs in patients that develop secondary bacterial pneumonia.6

A severe, diffuse patchy interstitial-to-alveolar pattern, more severe in the mid-to-caudodorsal lung fields, in a dog with smoke inhalation injury after a house fire

A severe, patchy interstitial-to-alveolar pattern, more severe in the left hemithorax and caudodorsal lung fields, in a dog with smoke inhalation injury after a house fire
Treatment & Management
Oxygen supplementation should be immediately administered to all patients with smoke inhalation injury, as this will help stabilize patients with CO or CN toxicity. Continued oxygen supplementation should be provided in case of deteriorating respiratory status. In humans, hyperbaric oxygen therapy has shortened recovery from CO poisoning, but this is often unavailable routinely in veterinary hospitals, and intubation and ventilation with 100% oxygen is a reliable alternative.4,18 Mechanical ventilation may be required in patients that do not maintain normoxemia.7 Duration of mechanical ventilation is variable, as resolution of concurrent injuries, neurologic dysfunction, and severity of pulmonary injuries are all factors associated with requiring ventilation. Patients that require intubation and are candidates for prolonged mechanical ventilation may need referral to a tertiary care facility. Temporary tracheostomy may be required in cases of severe laryngeal edema that lead to upper airway obstruction.
An IV catheter should be placed, ideally in an area of skin unaffected by thermal burn injury. Although IV fluids may not be necessary for patients with mild smoke inhalation and subsequent respiratory complications, they are essential in managing patients with concurrent burn injury, as signs of hypovolemia and distributive shock are not uncommon with severe burns. Fluid therapy should aim to address maintenance fluid requirements and replace any ongoing losses using balanced isotonic crystalloids while avoiding volume overload, as this may increase the risk for pulmonary edema formation in patients with increased pulmonary vascular permeability secondary to smoke inhalation. In patients presented with signs of shock, fluid resuscitation with balanced isotonic crystalloids (dogs, 20-30 mL/kg IV boluses, up to a total of 90 mL/kg shock dose; cats, 10-15 mL/kg IV boluses, up to 60 mL/kg shock dose) should be administered, and the patient should be reassessed after each fluid bolus to identify resolution of signs of shock (eg, improvement to normalization of mentation, heart rate, pulse quality, blood pressure, or other identified endpoints). In patients with signs of lower airway inflammation or bronchoconstriction, treatment may include terbutaline (0.01 mg/kg IV or IM), aminophylline (dogs, 5-10 mg/kg IV; cats, 4 mg/kg IV), or albuterol via metered-dose inhaler. Sedation or analgesia may be required on presentation, depending on the extent of CO or CN toxicity and burn injury. Sedation with opioids (eg, butorphanol, 0.2-0.4 mg/kg IV or IM; methadone, 0.1-0.2 mg/kg IV or IM; or fentanyl, 2-5 µg/kg/hour IV CRI) can help manage anxiety related to both dyspnea and pain associated with burns. Acepromazine (0.01-0.1 mg/kg IV or IM) can be considered in a normotensive patient with signs of dyspnea and airway obstruction. Empiric antibiotic therapy is not generally recommended for patients with smoke inhalation unless secondary bacterial pneumonia is suspected. Antibiotics are ideally selected based on culture and susceptibility testing results obtained from airway sampling via endotracheal wash or bronchoalveolar lavage.
Prognosis & Prevention
Prognosis depends on the duration of exposure, severity of clinical signs, and extent of concurrent severe burn injury. Dogs and cats with smoke inhalation are reported to have a satisfactory survival rate of up to 90%.6,13,16 There is not much literature on prognostic factors and mortality in small animals with smoke inhalation. Two case series evaluating smoke exposure in dogs and cats reported an increased risk for death or euthanasia and prolonged hospitalization in patients exhibiting worsening respiratory signs 2 days after hospitalization.13,16 Retrospective studies support findings that progressive respiratory decline or neurologic dysfunction may result in worse outcomes.13,15,18 In a case series on cats affected by smoke inhalation, none of the cats died from smoke exposure, but 2 were euthanized because of the severity of respiratory and neurologic signs.16 Generally, the prognosis for survival to discharge is likely favorable if the patient recovers from CO or CN toxicosis in the acute hospitalization period or has minimal respiratory or neurologic signs in the first 24 to 72 hours. The long-term prognosis for respiratory and neurologic function following hospital discharge in recovered patients is excellent, and a gradual return to normalcy can be expected.