The Case: Worsening Skin Infection in a Cat
Sandra R. Merchant, DVM, DACVD, Louisiana State University
Filbert, a 10-year-old neutered domestic short-haired cat, presented for worsening skin condition previously diagnosed as ringworm infection.
History
Filbert lived in a large colony of cats segregated into smaller living groups. All cats were under the care of various veterinarians, with most receiving heartworm prevention and flea control therapy.
Many cats in the colony had been presumptively or definitively diagnosed with Microsporum canis infection, although not all had been tested or treated for ringworm. After definitive diagnosis of ringworm infection was confirmed with a positive culture result, Filbert had undergone 2.5 months of terbinafine treatment at 30 mg/kg PO q24h. In addition, he had been bathed weekly in ketoconazole-containing shampoo during the first month and then every other week thereafter.
The scaling and hair loss had improved significantly until about 1 month before presentation, at which time it had started to worsen.
Examination
On examination, all vital signs were within normal limits and Filbert’s weight was stable at 4.1 kg. No abnormalities were noted on thoracic auscultation or abdominal palpation. Papules surmounted by crusts, consistent with miliary dermatitis and self-inflicted alopecia, were noted bilaterally on the lateral, medial, and caudal thighs and the ventral abdomen.
Ask Yourself: What is an appropriate plan for Filbert?
A. Increase the terbinafine dose to 45 mg/kg and bathe Filbert weekly with a miconazole-containing shampoo.
B. Replace terbinafine with itraconazole and bathe Filbert q1–2wk with either a chlorhexidine- or miconazole-containing shampoo.
C. Consider other causes of worsening skin condition and perform a skin scraping, especially looking for Demodex gatoi.
D. Perform a dermatophyte brush culture and continue current ringworm therapy until desired results are obtained.
Correct Answer
C. Consider other causes of worsening skin condition and perform a skin scraping, especially looking for Demodex gatoi.
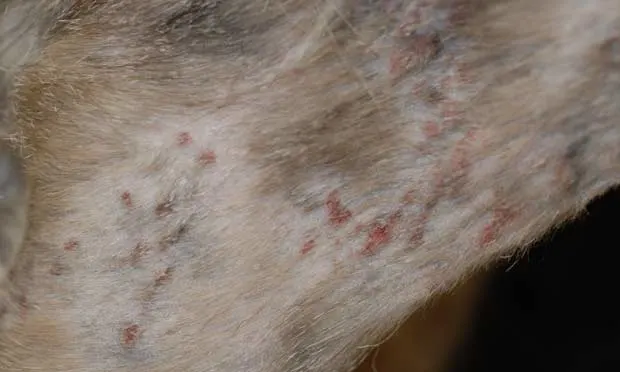
Because terbinafine treatment was ongoing, it seemed unlikely that self-inflicted alopecia and miliary dermatitis evident on examination (Figure 1) were the result of ringworm infection. Terbinafine was chosen because it has been shown to be effective and had recently become affordable.1,2 The skin scraping performed was negative. Of note, continuing exposure to ringworm-positive cats is a factor in performing repeat dermatophyte brush cultures (see Answer D: Brush Culture & Ringworm Therapy). The brush culture performed during this visit was reported as negative 3 weeks later, but terbinafine treatment was continued until the second negative brush culture was obtained.


Figure 1: Hair loss and miliary dermatitis on Filbert’s (A) lateral abdomen and thigh and (B) ventral abdomen were consistent with excessive licking and scratching related to flea allergy.
Other Causes of Miliary Dermatitis
In areas where fleas are present, the most common cause of self-inflicted alopecia and miliary dermatitis in cats is flea allergy.3 With Filbert, the initial skin disease—based on positive ringworm culture—was fungal-inflicted alopecia with scaling, which had been improving until about a month before presentation. In addition, although Filbert had been receiving monthly flea control, not all of the cats in the colony were under flea control. Furthermore, a new cat had been added to Filbert’s living group for 2 weeks but was removed shortly before his skin condition had worsened. Whether this cat played a role remained unknown, but it is likely if the transient was not on flea prevention.
Flea Control in Feline Colonies
All cohabitating animals should receive flea control therapy at minimum on a monthly basis. Frequency of shampooing may need to be considered when choosing topical flea control. In most flea-allergic cats, twice-monthly topical flea control therapy can help control clinical signs, although weekly flea control with an approved product may be needed. Even then, it can take 4 to 6 weeks (or more) before new or improved flea control measures alleviate or resolve signs associated with flea allergy. Antihistamines may relieve some of the itching, but oral and injectable glucocorticoids should be avoided in cats testing positive for ringworm.
Outcome
Flea control therapy for Filbert was increased to twice-weekly topical administration, and reduced contact between cat groups was beneficial in resolving his self-inflicted alopecia and miliary dermatitis. Flea control therapy was decreased to once monthly after his clinical signs had resolved.
Despite the negative skin scraping, if clinical signs had not improved after implementation of complete flea control measures, treatment for D gatoi would be a consideration, especially in multicat households and colonies.
Take-Home Messages
In multicat households and catteries, consider ringworm, D gatoi, and flea allergy as likely differentials for skin disease.
It is quite common to find no evidence of fleas or flea feces on cats with flea allergy dermatitis, as they are excellent at removing evidence during grooming. If small flecks of dirt are seen, especially comma-shaped flecks, moisten them; flecks that turn red while dissolving are confirmed flea feces.
If a cat tests positive for ringworm infection, continue treatment (terbinafine) until the results of two or three consecutive brush cultures are negative. Environmental cleaning is also important to minimize the potential for reexposure via infected hair in the environment.
For cats with flea allergy, implement flea control twice monthly (sometimes weekly, depending on product and bathing protocol) for 4 to 8 weeks or until clinical signs resolve. All cohabitating animals need to remain on good flea control therapy.
If a cat’s skin condition worsens, evaluate whether the original presenting signs are similar to or the same as the worsening signs.
If flea infestation is suspected in multicat facilities but clinical signs of pruritus and/or miliary dermatitis do not resolve, consider treatment for possible D gatoi infection (lime sulfur dips weekly for 4 to 6 treatments; monthly topical imidacloprid/moxidectin for cats).
Brush Culture & Ringworm Therapy
Of note, Answer D—perform a dermatophyte brush culture and continue current ringworm therapy until desired results are obtained—also applies in this case. However, although ringworm infection had been responsible for the initial fungal-inflicted alopecia, it was not as likely responsible for the subsequent miliary dermatitis and self-inflicted hair loss.
Even in single-cat households, ringworm therapy should be continued until a brush culture is negative. In large cat populations or catteries, it is ideal to continue therapy until two or three brush cultures performed 1 month apart are negative.
Ideally, all cohabitating cats should be examined for ringworm and any cats with positive brush culture results need to be housed separately. Environmental cleaning1 and topical therapy are important to minimize environmental reexposure and zoonotic transmission.
Some controversy remains concerning total body clipping of ringworm-infected cats, as it may initially worsen clinical signs; however, improved environmental control and decreased zoonotic risk also need to be considered.
Note:
This article was originally published in Clinician's Brief with the title "Skin Disease in Cats: It Isn’t Always What It Seems" in May 2012.