Shockwave Therapy as a Treatment Option
Kristin Kirkby Shaw, DVM, MS, PhD, DACVS, DACVSMR, Aratana Therapeutics, Kansas City, Kansas
Extracorporeal shockwave therapy (ESWT), an acoustic energy modality, has become an accepted treatment modality for musculoskeletal injuries, osteoarthritis (OA), and wound healing in horses.1 There is, however, limited awareness of its use in companion animals.
Mechanism of Action
Shock waves, high-energy sound or pressure waves (like thunder following lightening or a small, focused explosion), have little to do with electric shock. Shock waves can be generated in many ways, but electrohydraulic devices have the greatest capacity to produce and project high energy to a deep focal depth. ESWT can be highly focused and can achieve a focal point beyond 10 cm into deeper tissues, depending on the treatment head used. ESWT differs from radial pressure wave therapy, which does not deliver focused energy at the target; instead, acoustic waves spread eccentrically from the applicator tip.2
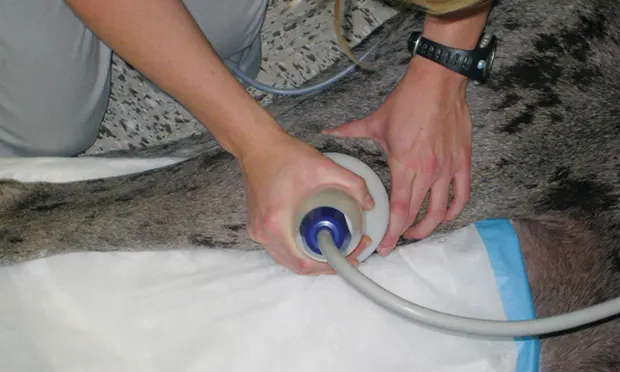
ESWT is applied superficially, with waves entering tissue and being absorbed or reflected. Energy is released when a wave meets an area of high acoustic impedance (eg, bone–tendon interface). Compressive and tensile forces cause cavitation and mechanical microstress in cells and tissues, resulting in modulation of inflammatory, angiogenic, and osteogenic proteins that assist the natural healing process. Shockwave therapy applied to an area of chronic, nonhealing tissue (Figure 1) may enable acute cytokines to be released and stimulate healing. The mechanism behind the pain-relieving function may result from increased serotonin activity in the dorsal horn and descending inhibition of pain signals.3

Figure 1 ESWT on a 4-year-old castrated English pointer for a partial Achilles tendon rupture (managed nonsurgically). Full recovery was achieved after 9 months of physical rehabilitation, ESWT, and a custom brace.
Indications
Bone Healing
Several clinical studies in humans have investigated the use of ESWT to treat complex fractures and delayed bone union. In humans with high-energy fractures of the long bones, ESWT immediately following surgical repair resulted in significantly faster fracture healing and decreased incidence of nonunion compared with the control group.4 Similarly, one treatment of ESWT resulted in bony consolidation in 75% of patients with previous delayed or nonunion fractures.5
Of 4 dogs treated for fracture nonunion, 3 showed significant progression in bone healing following treatment.6 Furthermore, in a canine model of distal radial fracture nonunions, all dogs that received ESWT showed complete bony union after 12 weeks, whereas no dogs in the control group achieved complete bone healing.7
Related Article: Stem Cells: New Therapy for Old Diseases
Indications for Bone Healing
Delayed union and trophic nonunion fractures
In conjunction with surgical repair of highly comminuted fractures and/or anticipated slow fracture healing
In conjunction with external coaptation for nonsurgical management of digital, metacarpal, or metatarsal fractures
Tendon & Ligament Healing
Tendinopathies, often a result of repetitive activity or overuse injuries, commonly cause pain and loss of full function. They are typically noninflammatory; degeneration of tendon fibers and insufficient vascular supply to the area can lead to loss of the tendon’s mechanical properties. Treatment has typically relied on rest and/or surgery along with medications (eg, NSAIDs, steroid injections), but treatments (including ESWT) aimed at increasing blood supply and stimulating the regeneration of tendon tissue are gaining recognition.
For instance, one study has demonstrated improvement in 88% of dogs with lameness attributable to soft tissue shoulder conditions (eg, supraspinatus/biceps tendinopathy) following treatment with ESWT without surgical intervention.8 Shockwave therapy was also shown to significantly reduce distal ligament thickening in dogs with patellar ligament desmitis following tibial plateau leveling osteotomy.9 Finally, significantly increased neovascularization at the bone–tendon interface in a canine model of the Achilles tendon has demonstrated healing with the use of ESWT.10
Indications for Tendon & Ligament Healing
Supraspinatus tendinopathy
Biceps tendinopathy
Medial shoulder instability
Achilles tendinopathy (in addition to surgery if indicated)
Patellar tendinopathy
Iliopsoas strain
Osteoarthritis
Shockwave therapy has been shown to modulate the osteoarthritic disease process in animal models by reducing nitric oxide production in the joint and inhibiting chondrocyte apoptosis. Shockwave therapy can also be valuable for managing arthritic pain.
Several studies have demonstrated positive results in joint range of motion and peak vertical force—as measured using force plate analysis—in dogs with stifle (Figure 2), hip, and elbow arthritis. For example, in dogs with unilateral elbow OA treated with ESWT, improvement in lameness and peak vertical force was equivalent to that expected with NSAIDs.11

Figure 2 ESWT on a 5-year-old spayed Great Dane with arthritic stifle joint.
Chronic Wounds
Shockwave therapy has been shown to enhance skin flap survival and prevent ischemia-reperfusion injury in rodent models, and studies are currently investigating ESWT for treating diabetic ulcers in humans. Currently, there are only experimental studies on equine wounds and unpublished case reports of ESWT for treating chronic wounds in small animals.12,13 However, based on its mechanism of action, ESWT may be a valuable adjunctive therapy in managing skin flaps and difficult wounds.
Contraindications
Shockwave therapy should not be used over a neoplastic lesion, thorax or abdomen, potential vascular thrombi, or in place of stabilization of fractures and traditional wound management.
Clinical Use
Because ESWT can be loud and acutely painful, sedation is required. Medications used with ESWT vary. Shockwave therapy is commonly used in conjunction with traditional surgical management; therefore, patients may already be anesthetized at treatment. Treatment time depends on the amount of energy delivered and number of locations treated. A common dose of 800 pulses per joint requires fewer than 4 minutes to deliver.
Patients typically begin experiencing pain relief benefits of ESWT within 24 hours; however, oral pain management should be considered. Tramadol at 2 to 4 mg/kg PO q8–12h and/or deracoxib at 1 to 2 mg/kg PO q24h is typically prescribed.
Treatment of musculoskeletal conditions is recommended q2–3wk for 1 to 3 treatments or until clinical improvement or resolution has been achieved (eg, bone union). Wounds are typically treated once a week; depending on the wound size, more than 3 treatments may be required. When ESWT is used to manage OA, disease resolution is not expected; thus treatment is typically repeated q6–12mo as needed. Treatment protocols may vary, depending on the ESWT equipment used; most ESWT manufacturers have suggested protocols for common indications.
ESWT should be used in conjunction with a physical rehabilitation program that will likely include activity modification and therapeutic exercises to optimally return the patient to full activity.