Sarcoptic Mange
Adam P. Patterson, DVM, DACVD, Texas A&M University
Profile1-7
Definition
Sarcoptic mange (ie, sarcoptic acariasis) is a transmissible dermatosis caused by the burrowing acarid mite Sarcoptes scabiei.
Infestation, referred to as scabies, often results in acute and intense pruritus.
Common in domestic dogs and rare in cats, sarcoptic mange can affect other mammalian species (eg, foxes, rabbits, guinea pigs, ferrets, sheep, goats, cattle, pigs, Spanish ibex, humans).
Scabies occurs worldwide but is more prevalent in some regions because of environmental conditions.
Signalment
No age, sex, or breed predilections
Young patients may be at increased risk because of exposure in overcrowded areas (eg, shelter, kennel, pet store, breeding mill, boarding or training facility).
Related Article: Sarcoptic Mange
Causes
S scabiei is an obligate parasite that spends its entire 14–21-day life cycle on the host.
Scabies mites are named as variants of their preferred host species.
S scabiei var canis (dog)
S scabiei var vulpis (red fox)
S scabiei var ovis (sheep)
S scabiei var bovis (cattle)
S scabiei var suis (pig)
Variants tend to infect certain hosts but can cause disease in other species.
Feline scabies is caused by Notoedres cati; however, S scabiei has reportedly caused disease in cats (rare).1
Location of the mite anus helps distinguish between S scabiei var canis and N cati (terminal in the former, dorsal in the latter).
Risk Factors
While not always necessary, direct contact with an infested animal, especially in an overcrowded area, increases the risk for transmission.
Other risk factors include fox-dense regions and immunosuppression.
Pathophysiology
Clinical disease can develop when an affected animal’s mites are transmitted to the skin of another animal.
After the mites penetrate the skin, they burrow, feed, and reproduce in superficial skin layers, often in areas with little hair.
Pruritus occurs
When mite population increases
Through suspected hypersensitivity reaction to mite antigens
Because S scabiei and house dust mites share similar antigens, antibody cross-reactivity (influencing allergy test interpretation) and cosensitization are possible.
History
Historical clues suggestive of scabies may include
Acute and severe nonseasonal pruritus
Exposure to roaming foxes
Recent history of adoption or boarding
Cohabitation with multipleanimals, several of which may be pruritic
Lack of acaricidal therapy in monthly ectoparasite preventives
Fair-to-poor response to previously administered antiinflammatory glucocorticoids and/or cyclosporine
Humans in the household may be pruritic and have erythematous papules.
Clinical Signs

Dogs
Pruritus
Moderate to extreme
Observable at physical examination
Distribution

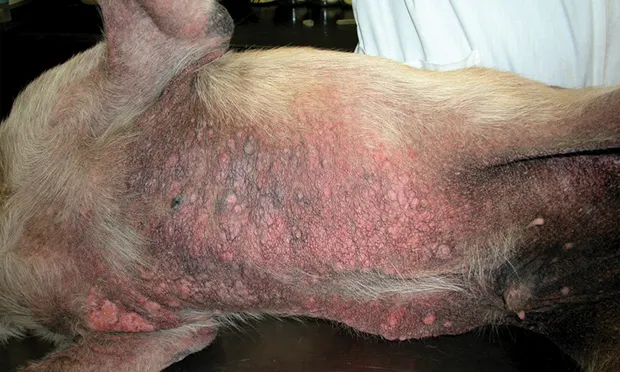
Sparsely haired body regions: Pinnal margins (not otic canals), periocular skin, elbows (Figure 1. Sarcoptic mange presenting as crusting excoriation along the left caudolateral elbow of a dog) hocks, and ventral trunk (Figure 2. Pruritic papular rash with lichenification on ventral trunk of a dog with sarcoptic mange.)
May become widespread as alopecia becomes more severe
Dorsum and paws are often spared (Figure 3. Distribution pattern of disease for canine scabies.2).
Lesions
Peracute: Lesional pruritus that may mimic allergic skin disease
Acute: Erythematous maculopapular eruptions that eventuate into crusted papules with excoriations and alopecia
Chronic: Diffuse exfoliation with hyperpigmented lichenification and hyperkeratotic calluses on elbows and hocks
Aural hematoma can occur at any disease stage.
Some dogs may not develop skin lesions despite intense pruritus (ie, scabies incognito), while others (ie, immunosuppressed) have widespread lesions with minimal pruritus (ie, crusted or Norwegian scabies).
Secondary skin infection
Superficial pyoderma and/or Malassezia spp dermatitis are common sequelae.
Extracutaneous signs
Lethargy
Depression
Inappetence
Weight loss
Peripheral lymphadenomegaly
Nonclinical carriers may exist.
Cats
Pruritus is nonexistent to moderate.
Distribution on bridge of nose, face, pinnae, paws, and tail
Lesions include crusted papules and alopecia.
Extracutaneous signs include poor body condition and peripheral lymphadenomegaly.
Related Article: Pruritus & Pinnal Hair Loss in a Beagle
Diagnosis1-4
Definitive

Definitive evidence involves microscopic finding of scabies mites, mite eggs, or mite feces (Figure 4. Sarcoptic acariasis mite) on superficial broad skin scrapings from representative nonexcoriated lesions or fecal flotation findings.
Circumstantial evidence includes history, signs, and positive pinnal–pedal response (uncontrollable scratching/thumping with a pelvic limb when the ipsilateral pinnal margin is scratched).
Clinical resolution following appropriate scabicidal therapy also indicative
Paucity of S scabiei exists when dogs are hypersensitive to mite antigens, so negative skin scrapings and/or fecal examination do not exclude scabies.
Mites are usually numerous and easy to find on skin scrapings from immunosuppressed dogs (crusted scabies).
Differential
Dogs
Folliculitis (eg, superficial pyoderma, demodicosis, dermatophytosis)
Malassezia spp dermatitis
Pelodera spp mange
Allergic skin disease
Contact dermatitis
Ear margin dermatosis
Zinc-responsive dermatosis
Pemphigus foliaceus
Neoplasia
Cats
Demodex gatoi infestation
Otodectic mange
Cheyletiellosis
Notoedric mange
Herpesvirus dermatitis
Allergic skin disease
Laboratory Testing
Indicated
Skin surface cytology to exclude concurrent bacterial and/or fungal infection
May be Indicated
ELISA serologic testing for IgG against Sarcoptes spp antigens
Available in some countries, but false-positive (eg, cross-reactivity with house dust mite) and negative (eg, dogs receiving glucocorticoids) results can occur.
Skin biopsy to exclude other differentials
CBC, serum chemistry panel, urinalysis, and feline retroviral testing when other comorbidities are suspected as based on history and physical examination
Before extralabel macrocyclic lactone therapy
Testing for heartworms when status is unknown or questionable
ABCB1Δ genetic testing to screen for avermectin sensitivity in ivermectin-sensitive dogs (eg, herding dogs, sight hounds) before the use of extralabel macrocyclic lactone therapy
Treatment1-4,8,9
Dogs with unexplained pruritus, particularly unresponsive to glucocorticoids (eg, prednisone 1 mg/kg q24h) should receive trial therapy for scabies before making a diagnosis of allergy.
Duration of scabicidal therapy should encompass at least two mite life cycles (at least 4–6 weeks) regardless of the product prescribed.
S scabiei can be transmitted to other close-contact animals and humans; all close-contact animals (notably dogs) should be treated concurrently.
In general, systemic scabicidal therapy (including correctly applied systemic spot-on) is more effective than topical treatment for scabies because of improved compliance.
Assuming all close-contact animals are treated, environmental decontamination is not typically needed, unless scabies outbreak occurs in an overcrowded facility.
Scabies-infested dogs and cats can be treated as outpatients; use of topical amitraz dips (dogs) should be reserved for in-hospital use.
Supportive Medical Care (see Medications)
Antiseborrheic shampoo can facilitate removal of excessive surface scale and crusting.
Concurrent pyoderma and/or Malassezia spp dermatitis must be treated.
In dogs, systemic azole therapy (inhibitor of P-glycoprotein) cannot be given concurrently with extralabel (high-dose) macrocyclic lactones such as ivermectin (substrate of P-glycoprotein), as doing so may cause signs of ivermectin-sensitivity.
Sole topical therapy directed against yeast may be needed to avoid potential drug interactions.
Worsening pruritus is normal during the first days of treatment, so systemic glucocorticoids (dogs, prednisone 1 mg/kg PO q24h 3–7d; cats, prednisolone 2 mg/kg PO q24h 3–7d) or oclacitinib (dogs, 0.4–0.6 mg/kg PO q12h 3–7d) are often indicated.
Aural hematomas should be decompressed.
Nutritional Aspects
The patient should receive an age-appropriate balanced diet.
Client Education
Humans who develop itchy skin (± lesions) should contact their physician.
Medications1-7, 9-12
Note: Recommended treatments are mostly considered extralabel as described.
Canine Sarcoptic Mange
Systemic
Ivermectin: 0.2–0.4 mg/kg SC q14d 3–4 doses or 0.2–0.4 mg/kg PO q7d 4–6 doses
Doramectin: 0.2–0.6 mg/kg SC q7d 4–6 doses
Moxidectin: 0.2–0.3 mg/kg SC q7d 3–4 doses or 0.2–0.3 mg/kg PO q7d 4–6 doses
Moxidectin 2.5% + imidacloprid 10% topical spot-on: Applied q2–4wk 2–4 doses (based on manufacturer’s established body weight range)
Selamectin topical spot-on: Applied q2–4wk 3–4 doses (based on manufacturer’s established body weight range)
Dermatologists have safely used this protocol in herding canine breeds.
Topical
Amitraz: 0.025%–0.03% solution applied to entire skin surface q1–2wk 4–6 doses
Do not rinse.
May need to clip coat to facilitate contact
Lime sulfur: 2%–3% solution applied to entire skin surface q7d 4–6 doses
Do not rinse.
May need to clip coat to facilitate contact
Fipronil spray: 3 mL/kg applied as fine mist to entire skin surface q2–3wk 3 doses or 6 mL/kg sponged on the skin q7d 4–6 doses
May be better reserved for subclinical close-contact dogs
Feline Sarcoptic Mange
Systemic
Ivermectin: 0.2–0.3 mg/kg SC q2wk 3–4 doses
Doramectin: 0.2–0.3 mg/kg SC as a single dose or repeated in 2 weeks
Moxidectin 2.5% + imidacloprid 10% topical spot-on: Applied q2wk 3–4 doses (based on manufacturer’s established body weight range)
Selamectin topical spot-on: Applied q2wk 3–4 doses (based on manufacturer’s established body weight range)
Topical
Lime sulfur: 2%–3% solution applied to entire skin surface q7d 4–6 doses
Do not rinse.
May need to clip coat to facilitate contact
Precautions & Drug Interactions
Dogs with an ivermectin-sensitive genotype (eg, herding dogs, sight hounds) should not receive extra-label macrocyclic lactone therapy (eg, ivermectin, doramectin, moxidectin) because of risk for neurotoxicosis signs.
Neither spinosad-containing flea preventives nor systemic azole therapy (eg, ketoconazole, itraconazole) can be given concurrently with extralabel macrocyclic lactones in any dog (neurotoxicosis).
Amitraz dip treatment should be used cautiously in small dogs and should not be used for Chihuahuas.
Do not administer concurrently with monoamine oxidase inhibitors in any dog.
Whether amitraz is optimal should be strongly considered; in-hospital application is recommended, and administrative personnel are at risk for adverse effects.
For nonclinical dogs, fipronil spray may be cost-effective in a multidog household.
Follow-up
Patient Monitoring
Pruritus should be significantly improved after the first two doses of scabicidal therapy (within 3 weeks), but mild pruritus may linger for several weeks.
If skin lesions fail to improve after 3–4 weeks of therapy, skin culture and/or biopsy may be indicated.
Complications
Treatment failure may occur if
Using topical spot-on for patients with body weights nearing the upper limit of the manufacturer’s recommended body weight range (ie, underdosed therapy)
All close-contact animals (especially dogs) or secondary infections are not concurrently treated
In General
Relative Cost
Canine sarcoptic mange: $–$$
Feline sarcoptic mange: $–$$
Sarcoptic mange in multipet household: $$$–$$$$
Prognosis
Good
Prevention
Routine use of flea preventives containing acaricides may lessen chances for scabies after casual exposure to an infested animal.