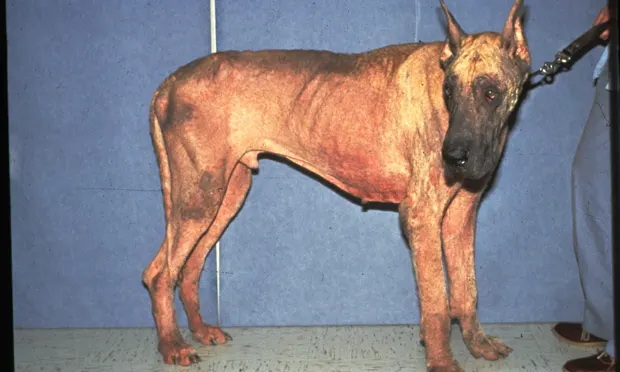
Profile
Definition
Highly contagious, nonseasonal, pruritic parasitic skin disease caused by Sarcoptes scabiei.
Signalment
Almost all mammalian species are affected by a variant of this species.
Occurs commonly in dogs.
No age, sex, or breed predilection.
Sarcoptes scabiei infestation is rare in cats but may be underdiagnosed; Notoedres species infestation in cats is considered the "contagious mange" of cats.
Causes & Risk Factors
Infestation caused by mites of the family Sarcoptidae, including the feline mange mite Notoedres cati.
Infestation in dogs is caused by Sarcoptes scabiei var. canis. Mites are small (200 to 400µm) and oval, with two pairs of anterior legs and two pairs of rudimentary hind legs that do not extend beyond the body (Figure 1).

Disease is highly contagious and easily transmitted. Mite is not host-specific, and all in-contact animals are at risk for infestation.
Infestation can occur from direct contact with an affected animal or indirect contact via a fomite. Cool, damp conditions favor survival of mite in the environment; female mites have been reported to survive off the host for 4 to 21 days.1
Contact with a large number of other animals is a risk factor: boarding kennels, grooming facilities, dog day-care centers, communal dog parks, and competitions.
Canine reservoirs of infestation in populated areas include feral, stray, and/or dogs that are allowed to roam free; foxes; and coyotes.
Mite life cycle is 17 to 21 days; they copulate in burrows in the skin and lay eggs in tunnels in the superficial skin; they prefer thinly haired areas of body.
Pruritus is caused by mechanical burrowing of mites; there are strong indications that clinical disease is caused by a complex hypersensitivity reaction. Inapparent canine carriers can be seen.
History & Clinical Signs2
Acute onset of intense pruritus usually occurs within 3 to 4 weeks of exposure.
Dogs that scratch incessantly during examination should raise clinical suspicion.
Lesions initially start on thinly haired areas of the body; distribution pattern is ventral. Ear margins, elbows, and ventrum are good sample sites.
The primary early lesion is a pruritic, papular, crusted, erythematous eruption.
Lichenification, crusting, erythema, and self-excoriation are common. Alopecia develops as disease progresses. Lymphadenopathy is common (Figures 2 and 3).


Disease typically spares dorsum but can become generalized.
Two atypical presentations of scabies are clinically normal dogs with only intense pruritus ("scabies of the cultivated") and dogs with severe crusting in which large numbers of mites are easily found ("Norwegian scabies").
"Norwegian scabies" is most common in immunosuppressed patients.
Clinical signs vary in cats and include pruritic pinnae, facial papules, pododermatitis with or without nail abnormalities, scaling, and pruritus. Self-trauma without skin lesions can occur.
Immunosuppression is common in affected cats.
Disease is zoonotic; owners may complain of pruritic papules on arms, chest, and abdomen.
Pain Index
Unquestionably one of the most severely pruritic skin diseases of mammals.
Affected animals incessantly scratch, rub, and self-mutilate, leading to irritability, anxiety, and sleep deprivation (according to owners).
Weight loss can occur.
Severe excoriations and secondary microbial infections are common.
Diagnosis
Definitive Diagnosis
Infestation with sarcoptic mange mite should be considered in the differential diagnosis of pruritic dogs, especially severe cases. The disorder is highly contagious, and a history of contagion and/or zoonosis may help narrow the potential diagnoses. Uncomplicated scabies is characterized by papular eruption; bacterial pyoderma brings pustules, crusted pustules, epidermal collarettes, and scales entrapping hairs.
Definitive diagnosis: Finding mites and/or mite eggs on skin scrapings.
Demonstration of mites is difficult if patient has been bathed or dipped or is severely excoriated. Estimated that mites are found in fewer than 20% of cases.2
Multiple skin scrapings of the ears flaps, ear margins, elbows, and papular nonexcoriated areas of the ventrum and/or lateral thorax enhance finding of mites.
Large amount of mineral oil applied to site and collected for examination: Mite visible at 10×. One egg or mite is diagnostic. Using a spatula for skin scraping enhances techniquea (Figure 4).

Mites and eggs may be found on fecal examination.
ELISA test for circulating anti-Sarcoptes IgG may be helpful in infections lasting longer than 5 weeks but is not available in the United States.3
Response to therapy is most common "diagnostic test."
The pinnal-pedal reflex (vigorous rubbing of an ear flap results in hind leg scratching) is positive in 75% to 90% of affected dogs.4 Test may be negative in dogs with no ear lesions.
Differential Diagnosis
Most common differential diagnoses are contact allergies, atopic dermatitis, food hypersensitivity, and bacterial or yeast pyoderma. Much less commonly, Pelodera infestation or hookworm dermatitis may be found.
Contact allergies have ventral distribution, are uncommon, have no evidence of contagion, and are slow to develop in contrast to scabies.
Atopic dermatitis includes facial, pedal, and ventral pruritus. No history of acute onset. This disorder is corticosteroid-responsive, whereas scabies is incompletely responsive. The pruritus of atopic dermatitis is usually less intense than that of scabies.
Food hypersensitivity may have gastrointestinal component (vomiting, diarrhea, frequent soft stools); pruritus is less intense; no history of acute onset.
Combined bacterial and yeast pyoderma can cause pruritus as intense as that of scabies. Pelodera is easily diagnosed by skin scraping and finding nematodes.
Hookworm dermatitis is ventral in distribution, often with severe predominant pedal pruritus. Hookworm dermatitis is seasonal in northern climates, but can occur year-round in warm climates; scabies can occur year-round.
Laboratory Findings
Fine-needle aspirates of lymph nodes are reactive; eosinophilic infiltrate can be seen. Histologic findings diagnostic if mites are found; perivascular to diffuse eosinophilic dermatitis is a typical finding.
Treatment
Due to contagious nature, treat patients as outpatients.
Clip dogs with dense hair coat if treating topically.
Bathe patients with antiseborrheic shampoo to remove crusts and scales.
Bathe patients before any whole-body treatment.
Opinions vary widely on efficacy of various drugs (e.g., fipronil, selamectin)5; therapy with any drug can fail.
Variations in efficacy may be related to prior use of parasiticidal agents (e.g., flea control) or regional variation in mite susceptibility.
Response-to-Therapy Trials
Rule of thumb: "If you suspect scabies, treat for it."
Secondary complicating bacterial and/or Malassezia infection can cause an incomplete response to therapy; treat concurrently or rule out before treatment.
Glucocorticoid use for humane relief can complicate concurrent treatments for microbial infections and/or response to therapy trials. Use with caution.
Use only drugs with consistent scabicidal efficacy.
Based on anecdotal reports of treatment failures in known cases of Sarcoptes, selamectin is often recommended only for treatment of known cases.5
Complete remission of clinical signs on completion of treatment is diagnostic. Lack of response is an indication for reassessment of diagnosis or change of scabicidal therapy.
Pruritus usually decreases within first 2 weeks of therapy; treat for at least 6 weeks as some dogs do not show improvement until after 4 weeks of therapy.
Treatment of Confirmed Cases
Treat all in-contact animals.
Treat with lime sulfur, amitraz, ivermectin, fipronil, milbemycin oxime, or selamectin for at least 6 weeks.
Fipronil spray may be used in severely debilitated animals.5
Glucocorticoids 0.5 mg/kg PO Q 24 H for 7 to 10 days or a topical steroid spray may be needed for humane relief of pruritus.
Client Education
Disease is highly contagious; all in-contact animals need treatment.
Contact with other animals should be avoided until conclusion of therapy and complete resolution of pruritus.
Disease is zoonotic; affected humans should seek medical therapy.
Topical applications may increase risk for contagion due to close contact with pet; wear protective clothing.
Mites can live off host; routine cleaning should eliminate mites from home environments. Wash all items that have come in contact with an infected animal (e.g., bedding, collars).
Environmental pesticides may be needed in kennels/multiple-animal facilities.
Aqueous ivermectin solution can be formulated and used as an environmental parasiticidal spray.b Use after thoroughly cleaning environment; allow solution to wet the surface; does not stain surfaces. Do not use around chelonians or collies.b
Medications
Drugs
Selamectin, lime sulfur, and fipronil are currently the only nonorganophosphate drugs licensed for the controlled and/or treatment of scabies.
Lime sulfur (4 to 8 oz/gal once or twice weekly for 6 weeks) is safe and effective. Can stain hair coat; higher concentration may be drying to skin. Good option for collies and ivermectin-sensitive breeds.
50% of dogs treated with selamectin responded to one treatment, and 90% responded to two treatments. Some have found it to be very effective; however, there are anecdotal reports of lack of efficacy.5 Recommended for use in confirmed cases at 6 to 12 mg/kg Q 30 days for two treatments.6 May be more effective if used biweekly. Good option for collies and ivermectin-sensitive breeds.
Amitraz (1 bottle/2 gal water) Q 2 weeks for 6 weeks. Less labor-intensive topical therapy. Possible adverse effects include bradycardia, sedation, transient hyperglycemia, PU/PD. Not recommended in Chihuahuas or pregnant, nursing, or diabetic dogs.5 Exposure to solution is not recommended in pregnant or diabetic owners or persons taking monoamine oxidase inhibitors. Good option for collies and ivermectin-sensitive breeds. The manufacturer does not recommend this product be used for the treatment of scabies due to lack of data supporting efficacy; reports of efficacy are anecdotal.
Fipronil spray and spot-on products are labeled as an aid in the control of scabies in dogs when used as labeled: 1 to 2 pumps per pound, thoroughly wetting the coat. Other recoommendations found to be effective include 3 ml/kg applied as pump spray or 6 ml/kg applied as whole-body dip. Efficacy still unclear as manufacturer recommends several monthly treatments are needed to eradicate infestation. May be an option in severely debilitated, pregnant, or young animals. Treatment concentration may be irritating to inflamed skin.<sup7, 8sup> Good option for ivermectin-sensitive breeds.
Milbemycin oxime (2 mg/kg Q 7 days for 3 to 5 treatments) reported as effective. Alternatively, 2 mg/kg twice weekly also effective. More expensive than ivermectin but well-tolerated and safer for ivermectin-sensitive breeds. Collies can be sensitive at higher doses.9-11
Moxidectin (0.2 to 0.25 mg/kg PO or SC weekly for 3 to 6 weeks) reported to be effective.12 Adverse effects include edema, angioedema, and ataxia. Not recommended for use due to limited information on efficacy.
Nutritional Aspects
No specific nutritional changes needed.
All patients should be fed a complete and balanced maintenance diet.
Performance diets may benefit severely debilitated patients with weight loss.
Follow-up
Complete resolution of clinical signs may take 4 to 6 weeks.
Initial worsening of pruritus is common; may be caused by hypersensitivity to dying mites.
Incomplete resolution of pruritus indicates treatment failure or misdiagnosis.
Selamectin may prevent reinfestation in patients at risk.
Individuals applying topical therapies at risk for infestation due to close contact; protective clothing should be worn.
Topical or oral glucocorticoids may be needed for humane relief of pruritus. Stop humane relief during last 10 to 14 days of treatment in patients undergoing therapeutic trial.
In General
Relative Cost
< $100 to $150-$250
Number of in-contact animals needing treatment influences cost.
Presence or absence of secondary microbial infections requiring therapy influences cost.
Prognosis
Excellent.
Future Considerations
Dogs at risk for reinfestation and/or exposure due to lifestyle may benefit from year-round selamectin treatment.
Currently considered a disease of dogs, but there is evidence that cats may be affected.13
TX at a Glance...
Patient Preparation
Treat all in-contact animals. Clip heavy-coated animals. Bathe to remove crusts, scales.
Humane Relief in Confirmed Cases
Short-term use of prednisone 0.5 mg/kg PO Q 24 H or topical steroid spray (e.g., Genesis Spray-Virbac)
Treatment Length
6 weeks
Drugs
Confirmed cases: Treat all in-contact animals with any of the following methods:
Selamectin (Revolution-Pfizer): 6-12 mg/kg 2× at 30-day intervals or Q 2 weeks for 3 treatments
Ivermectin (Ivomec-Merial Animal Health): 100 µg/kg PO as test dose; if no neurologic signs seen, proceed next day with 200 µg/kg Q 2 weeks for 3 treatments
Lime sulfur (LymDyp-DVM): 4-8 oz/gal 1-2× a week for 6 weeks
Milbemycin oxime (Interceptor-Novartis Animal Health): 2 mg/kg Q 7 days for 3-5 weeks with or without lime sulfur. Note: Milbemycin oxime can also be used at 2 mg/kg twice weekly
Amitraz (Mitaban-Pharmacia Animal Health): Label dilution; Q 2 weeks for 3 treatments
Fripronil (Frontline Plus Spray-Merial Animal Health): 2 pumps/lb minimum; spray must thoroughly wet coat/contact skin
Therapeutic trials: If positive response, treat all in-contact animals with any of the following methods:
Author's choice in non-at-risk breeds: Ivermectin or lime sulfur (see above)
Author's choice in at-risk breeds or dogs failing ivermectin test dose: Lime sulfur, milbemycin oxime with concurrent lime sulfur, or amitraz alone (see above)
Debilitated, pregnant, or very young: Lime sulfur, fipronil (Frontline-Merial Animal Health)
Environmental Cleaning
Routine cleaning of home and bedding of single animals
Can use products labeled as effective for flea control in kennel environment.
Take-home point: If you suspect scabies treat for it-even if the dog was treated with a product known to be scabicidal. Not all drugs work all the time in all patients!