Recurrent Pyoderma in a Golden Retriever
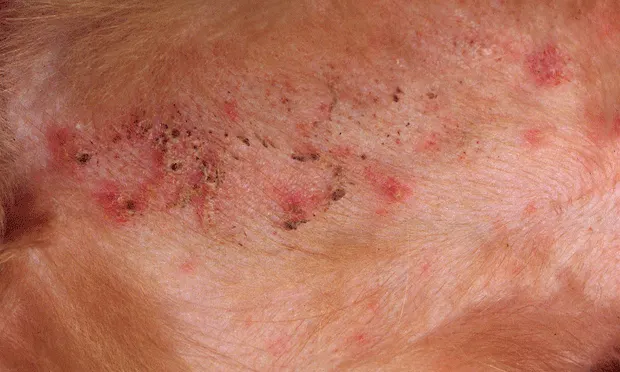
Briggs, a 5-year-old golden retriever, presented with superficial pyoderma that was unresponsive to antimicrobial therapy.
History. The dog had a history of recurrent superficial pyoderma as well as nonseasonal pruritus of the ventral trunk, groin, and feet since 1.5 years of age. The dog had been treated on numerous occasions with cephalexin (and twice with enrofloxacin) for 10 to 14 days and concurrent corticosteroids (injectable and oral), which usually led to significant improvement in the lesions and the pruritus. Five weeks prior to this presentation the dog had been treated with cephalexin (20 mg/kg Q 12 H PO) for 14 days, which did not result in any improvement in the skin lesions. A sample from a pustule containing many Staphylococcus intermedius organisms was then collected for bacterial culture and susceptibility testing. Based on the results of this antibiogram, the cephalexin dose had been increased to 30 mg/kg Q 8 H. The skin lesions persisted and the dog was referred for further evaluation.
Physical Examination. The dog was in good health apart from the dermatologic abnormalities. A moderate papular to pustular dermatitis with associated crusts was present on the trunk, the groin, and the medial thighs (Figure 1, above). There was moderate interdigital and axillary erythema.
ASK YOURSELF ...
What could have been done differently in the past to prevent recurrence of superficial pyoderma?
What is the error in the bacterial culture and susceptibility results?
What do you tell owners if they ask whether there is any health risk for themselves from this infection?
What are the most important diagnostic procedures to perform?
Diagnosis: Methicillin-resistant Staphylococcus intermedius (MRSI) infection of the skin
Until recently, MRSI was rare in canine superficial pyoderma but recent reports indicate that these highly resistant bacteria are an emerging problem in dermatology.1,2
It is likely that the dog has recurrent pyoderma associated with an underlying allergic dermatitis. As the pruritus is nonseasonal and affects the ventral trunk, axilla, and feet, food allergy and atopic dermatitis are the most likely underlying diseases.
Treatment. The dog was administered doxycycline 10 mg/kg Q 12 H and was bathed twice weekly with a 2% chlorhexidine shampoo. At reevaluation after 4 weeks of treatment, the pyoderma (papules, pustules, and crusts) had resolved but there was still moderate pruritus of the axilla, groin, and feet. There was no improvement in the pruritus after an 8-week hypoallergenic food trial (IVD Potato and Rabbit diet; Royal Canin, www. royalcanin.com). A diagnosis of underlying atopic dermatitis was made based on suggestive historical information, supportive clinical signs, and rule out of major differential diagnoses (eg, food allergy).
DID YOU ANSWER ...
Treatment with 10 to 14 days of antibiotics will significantly improve pyoderma but typically not resolve the infection. Always treat superficial pyoderma for a minimum of 3 weeks or until all lesions have totally resolved. I rarely use fluoroquinolones for superficial staphylococcal pyoderma except where bacterial culture and susceptibility testing has demonstrated that they are the only orally administered antimicrobials available to which the bacterium is susceptible. Staphylococcal pyoderma is a secondary problem and prevention of recurrence depends on identifying and controlling the underlying disease, which had not been achieved in this dog.
As the S intermedius isolated was resistant to methicillin, it must be reported as resistant to all β-lactam antibiotics irrespective of the apparent in vitro susceptibility. Corrected antibiogram results are shown below.
If methicillin-resistant S aureus (MRSA) had been cultured, there would be concern for zoonotic infection for the owners.3 MRSI has not been reported to infect humans to date and the potential for zoonotic infection is currently unknown.
Diagnostic Tests
Cytology of pustule contents to confirm pyoderma (detection of cocci) and rule out other nonbacterial causes of pustular dermatitis (such as dermatophytosis or pemphigus foliaceus).
Deep skin scrapings for Demodex mites as the dog has a history of corticosteroid administration, which predisposes it to development of adult-onset generalized demodicosis.
Cytology of nail folds and interdigital skin to assess whether yeast (Malassezia) dermatitis may be present in these areas and contributing to the pedal pruritus. No yeast organisms were seen on cytology, thus ruling out yeast dermatitis.
Bacterial culture and susceptibility testing of pustule contents. The organism is resistant to multiple drugs (including methicillin) and the dog had been treated with further antibiotics without clinical response since the first culture/sensitivity tests 3 weeks earlier. Thus, the susceptibility may have changed.
RECURRENT PYODERMA IN A GOLDEN RETRIEVER • Andrew Hillier
References
1. Comparison of tests to detect oxacillin resistance in Staphylococcus intermedius, Staphylococcus schleiferi and Staphylococcus aureus isolates from canine hosts. Bemis DA, Jones RD, Hiatt LE, et al. J Clin Micro 44:3374-3376, 2006.2. Screening of Staphylococcus aureus, Staphylococcus intermedius, and Staphylococcus schleiferi isolates obtained from small companion animals for antimicrobial resistance: A retrospective review of 749 isolates (2003-04). Morris DO, Rook KA, Shofer FS, Rankin SC. Vet Dermatol 17:332-337, 2006.3. Methicillin-resistant Staphylococcus aureus: An emerging pathogen in small animals. Weese JS. JAAHA 41:150-157, 2005.