Recognition & Management of Animal Sexual Abuse
Nancy Bradley, DVM, MNM, Arizona Humane Society
Karyn Rasile, RN, BSN, MAEd, CFN, SANE-A, AFN-BC, Scottsdale Healthcare Forensic Nurse Examiner Unit
This inaugural installment of a series of case studies involving forensic veterinary medicine reviews the approaches and goals for suspected sexual abuse cases.
Two 3-month-old, 4-lb, female shih tzu siblings were presented to different clinics with severe rectal trauma.
History
One puppy was presented to a private practice and died on admission. The second puppy was presented to an emergency clinic in lateral recumbency and barely conscious. Its rectal temperature was obtained, and the rectal area was lavaged with dilute chlorhexidine solution. The puppy was started on IV fluids but died soon after treatment.
Examination
At presentation, both puppies had severe rectal trauma. The outer rectal lining was significantly dilated and lacerated in each puppy (Figure 1) with contusions in the perianal (Figure 2A) and ventral abdominal (Figure 2B) regions. Both bodies were transferred to the local humane society for further investigation.
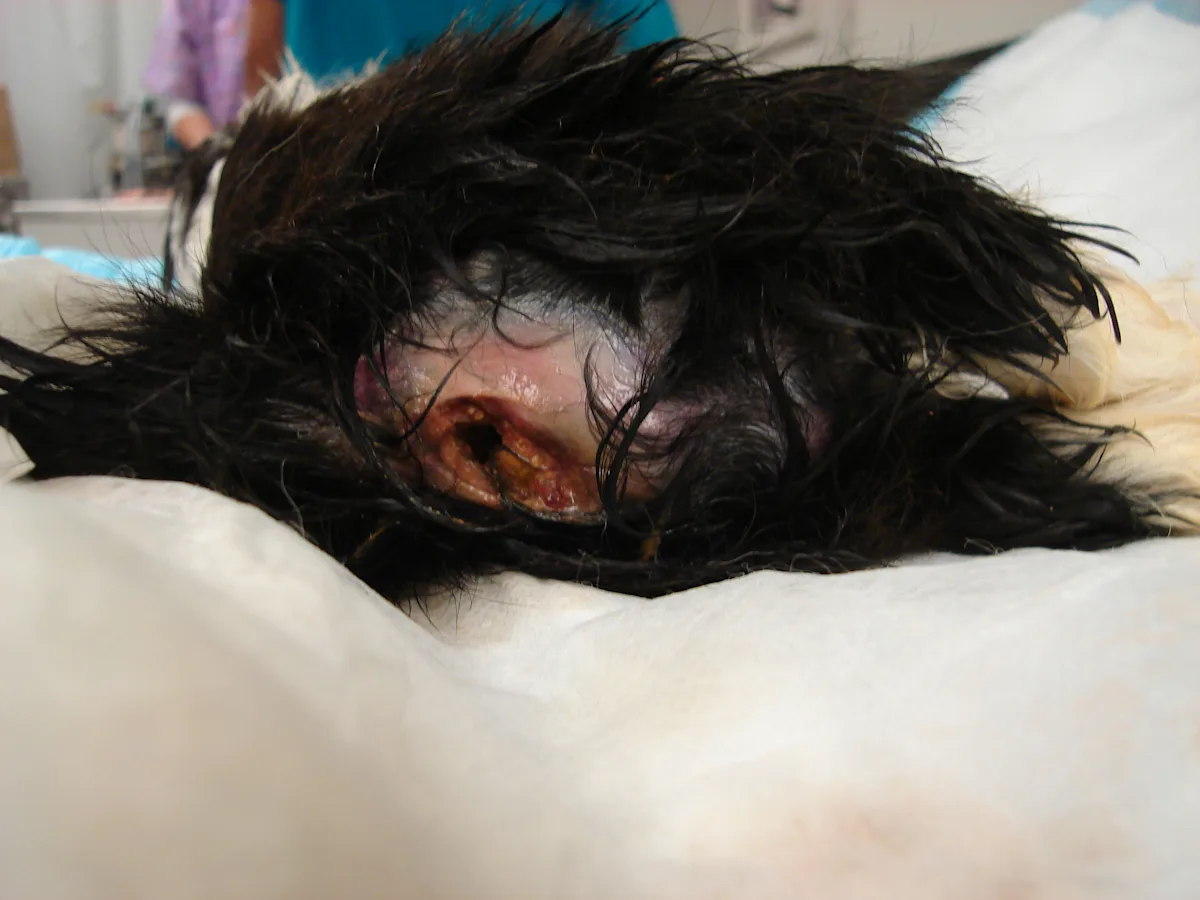
FIGURE 1 Dilation and laceration of the anorectal area
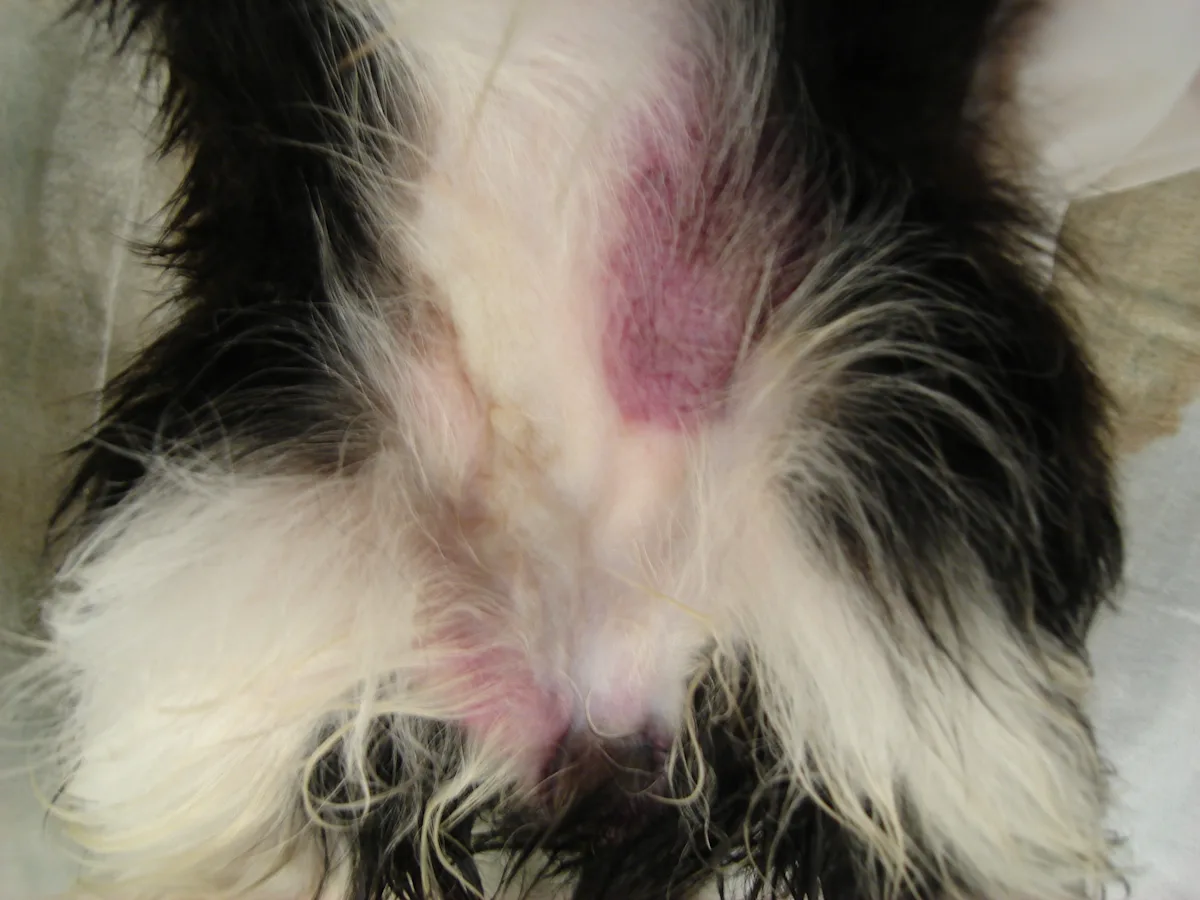
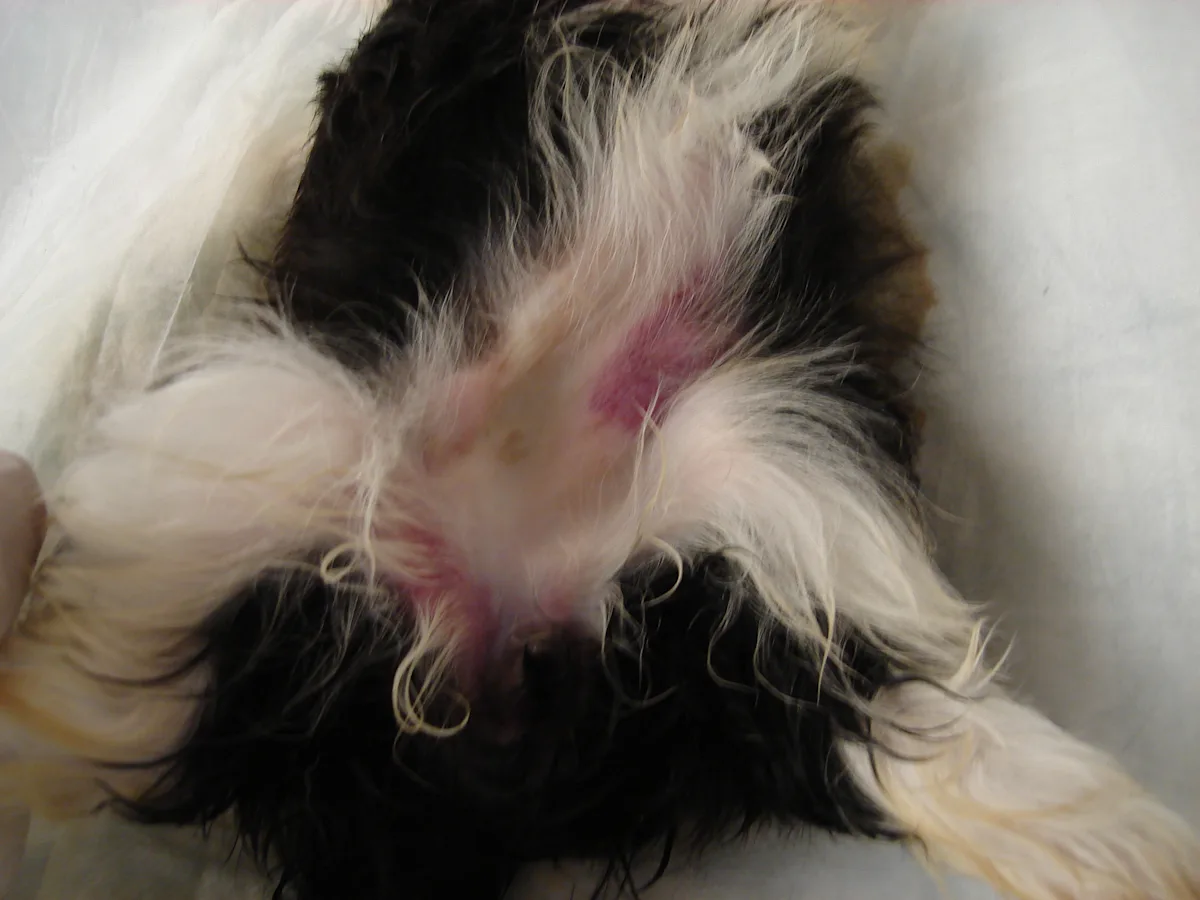
FIGURE 2 Contusions in the perianal (A) and 2 ventral abdominal (B) regions
Laboratory Results
Forensic examination was performed on the first deceased puppy, and samples were obtained; necropsy was performed on both.
Ask Yourself
Of the following 5 approaches, which 3 are best in a case of suspected sexual abuse in an animal?
A. Question the history with regard to the cause of any anorectal or genital injury.
B. Perform a forensic examination and collect samples.
C. Complete a routine physical examination, obtaining rectal temperature, pulse, and respiration before swabbing.
D. Treat superficial wounds aggressively.
E. Report the case to law enforcement.
Best Answers: A, B, E Question the history with regard to the cause of any anorectal or genital injury, perform a forensic examination and collect samples, and report the case to law enforcement.
Sexual abuse should be a differential in any case involving urogenital injury. Sexual acts with animals include any contact with or involving the animal’s anorectal area or genitalia. Signs include rectal and/or vaginal prolapse, anorectal or genital abrasions or lacerations, broken os penis, or bruising at the perineum or tail base.
Staff at private and emergency veterinary facilities are usually the first responders to animal cruelty. How the initial examination and treatment are handled can directly impact the ability of law enforcement and forensic professionals to collect and document critical evidence. This is especially true in cases of sexual abuse. If a veterinarian suspects that a patient has been sexually abused, proper evidence collection is essential for law enforcement to prosecute the perpetrator.
In most cases, veterinarians can perform the initial examination and swab collection, although some choose to turn the case over to forensic professionals and law enforcement from the outset. Some jurisdictions may require that law enforcement or crime scene personnel be present during evidence collection. Every effort should be made not to contaminate or destroy evidence before a forensic examination is performed and samples are collected (see Goals of Forensic Veterinary Examination and Performing a Forensic Examination).
Outcome
Both puppies originated from the same home, even though they were presented to different practices on different days. Necropsy findings in both puppies were consistent with sexual abuse: severe dilation of the anal tissue with lacerations and contusions to the perineum and ventral abdominal regions. There were proximal and distal rectal tears with concurrent peritonitis.
Forensic examination, including internal and external rectal and vaginal swab collection, was performed on the first puppy, but no usable evidence was found, and the case was not prosecuted. The emergency clinician treating the second puppy used spermicidal jelly on the thermometer, and the rectum was heavily lavaged with chlorhexidine to address the rectal wounds. Because of the potential contamination and destruction of evidence, no forensic examination could be pursued for the second puppy.
The Take-Home
Any history or suspicion of sexual abuse should be taken seriously.
Sexual abuse should be a differential in any case of genital/anorectal injury or trauma.
When sexual abuse is suspected, every effort should be made to preserve and collect forensic evidence before initiating any treatment or action that could alter forensic information.
Systemic stabilization of the patient should begin immediately, based on the patient’s condition.
Performing a Forensic Examination
Physical Examination
1. Perform a complete head-to-tail examination, looking for injuries: abrasions, bruises, pattern injuries, lacerations, bite marks, burns, head trauma, blunt force injuries, injuries to the ears (grabbing), ligature and/or binding marks (around muzzle or limbs), toenail injuries, strangulation-type injuries, and tail injuries (especially near the base). If more than 120 hours have passed since the suspected assault, look for evidence of healing/healed injuries.
2. Use a black light or alternative light source to look for semen, saliva, vomit, or blood; collect samples via swabs.
3. Take photographs of the entire animal, including all injuries, before and after shaving or cleaning. Acquire photographs with and without measurements.
4. Diagram all injuries.
5. Collect toenail scrapings, swabs, and clippings. All areas where physical or fluid (ejaculate) contact was possible should be swabbed, taking appropriate measures to prevent contamination:
Swab body surfaces using a sterile swab moistened with a drop of sterile water. When swabbing mucous membranes, it is not necessary to moisten the swab.
Hold the swab at a 45° angle, concentrating the contact area to the top of the swab.
Dry the swabs. If using a swab dryer, dry swabs for 1 hour before packaging. If a swab dryer is not available, place swabs in a cardboard swab box and keep them at room temperature for 24 hours before refrigeration or freezing. Special swab collection units, known as rape kits, are available.
Label each box with the location of the swabbed area. Check with the local crime laboratory for specific packaging guidelines.
Place boxes in a paper evidence bag.
Check with local reporting law enforcement agencies for packaging and chain of custody requirements.
6. Swab teeth and gums for foreign DNA or other material; collect a buccal DNA swab, as the animal may have bitten or scratched the perpetrator.
7. Obtain blood and urine samples. The animal may have been drugged, and the perpetrator’s sperm may be present in the urine of female victims.
8. Collect fecal samples if the animal defecated after the assault.
9. Examine the genital area (male and female), beginning externally and working inward; if alive, the patient should be sedated.
Collect rectal, vaginal, penile, and/or cervical samples via swabs (externally, then internally).
Examine for foreign bodies.
Use a sterile otoscope for a light source or a human (juvenile) sterile clear plastic vaginal speculum.
Consider obtaining cultures for Neisseria gonorrhoeae or Chlamydia trachomatis.
10. Obtain whole-body radiographs, with specific attention to the base of the tail and coccygeal area.
Acknowledgment: Special thanks to Dr. Melinda Merck, the Series Editor and a forensic veterinary consultant who actively assists animal cruelty investigators.