Pruritus & Pinnal Hair Loss in a Beagle
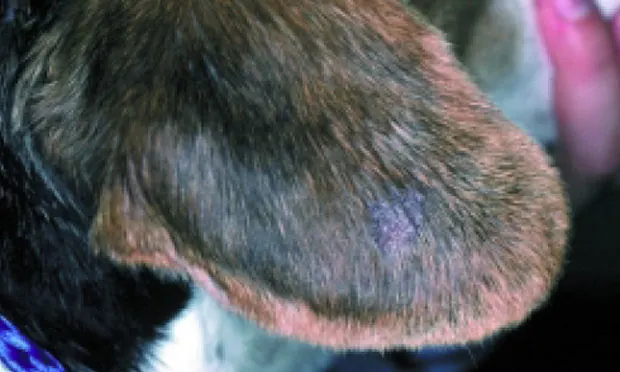
History. In August, an 18-month-old, neutered male beagle was presented for evaluation of generalized pruritus and hair loss on the distal pinnae of both ears. The dog freely roamed the owner's farm. According to the owner, the hair loss began 2 months ago and has slowly progressed to involve both ear flaps. The pruritus only developed in the past 2 weeks. The owner has no other pets.
Examination. Physical examination was otherwise normal. The hair on the lateral aspect of both pinnae was thin, and mild crusting and scaling were noted, especially on the ear margins. When the ears were manipulated, the dog exhibited an itch-scratch reflex. A diffuse papular eruption was present on the ventral abdomen, but no other dermatologic abnormalities were found.
Laboratory Tests and Diagnostic Evaluation. Otic examination of the horizontal and vertical canal was normal. Ear swabs were negative for mites, and cytologic evaluation revealed rare Malassezia organisms per high-power field (40×). Superficial and deep skin scrapings of the ventral abdomen and ear margins were negative for mites. Wood's lamp examination was also negative. The ear flaps were wiped with alcohol, and then a fungal culture was obtained using a toothbrush to collect spores and incubated in-house for 10 days at room temperature. Impression smears of the skin revealed large numbers of cornified epithelial cells but no bacteria or yeast organisms. While the results of the dermatophyte culture were pending, the dog was treated with ivermectin 200 µg/kg PO Q 2 WK for 6 weeks. The results of the dermatophyte culture are shown in Figure 1. At a 6-week reevaluation, pruritus persisted and hair loss had worsened. At this visit, a skin biopsy was obtained from the ear flap and the papular eruption on the ventral abdomen. The initial report revealed diffuse folliculitis and furunculosis (Figure 2). Special stains were ordered. The ear tips were recultured but the alcohol-wipe step was omitted. The sample was sent to a reference laboratory for culture.
Diagnosis. Trichophyton species infection. (See Figure 4.)
Interpretation and Treatment. The lack of response to what seemed to be appropriate therapy was a clear indication that a skin biopsy was needed to diagnose the skin disease. Folliculitis and furunculosis are commonly caused by demodicosis, bacteria, and dermatophytes. Special stains were indicated in this case to help determine whether a microbial infection was the cause of the folliculitis/furunculosis. For dermatophytes, routine histopathology and special stains cannot identify which pathogen is causing the skin disease. A repeat culture, which was incubated at higher temperatures for a longer period, was needed. There is increasing evidence that dermatophyte cultures should be incubated at 75° to 80° F; the usual recommendation is room temperature, which can vary tremendously.2 This dog was seen in August and room temperature in the clinic varied from 65° to 68° F. For this reason, some Trichophyton species can be difficult to culture in house. In addition, cultures are often swarmed by contaminants, and pathogens can be missed.
Pending results of the dermatophyte culture, the dog was treated with a systemic and topical antifungal drug. Microsporum canis and Trichophyton species infections are more difficult to treat than M. gypseum, which is a soil contaminant. In this case, itraconazole (10 mg/kg PO Q 24 H) and twice-weekly lime sulfur sponge rinses (8 oz/gal) were successful.3 The source of the Trichophyton species infection was never identified, but this organism can be isolated from rodents, pocket pets, and large animals. One species, T. rubrum, is a common source of human dermatophytosis.
Ask yourself...• The initial history and clinical presentation suggested what diagnosis?• On the basis of the skin biopsy findings, what is your diagnosis now? How did the special stain help?• Why wasn't the organism isolated the first time the samples were cultured?• How would you treat this dog?
Did you answer....• Sarcoptes scabiei was most compatible with the history, pruritus, papular eruption on the ventral abdomen, and itch-scratch reflex on ear manipulation. Given that the skin scrapings were negative, the only way to diagnose scabies would have been via a "response to treatment" trial. Sarcoptic mange mites can be very difficult to find; anecdotally they are estimated to be found in less than 1 out of 10 cases.1• Dermatophytosis. The intense inflammatory response can make it difficult to identify dermatophytosis via regular H&E staining. The special stain shown in Figure 3 is a periodic acid-Schiff stain, demonstrating the presence of glycogen and mucoproteins containing neutral polysaccharides. Fungal cell walls contain these polysaccharides, hence all fungi stain bright red with periodic acid-Schiff stain.1• Possible explanations include the following: loss of sample via aggressive wiping with alcohol, wrong technique for sampling the skin (plucking hairs may have been more successful), incubation period too brief, incubation temperature too low.• Systemic and topical antifungal treatment until there are three negative fungal cultures. Concurrent decontamination of the environment.
TAKE-HOME MESSAGES• Several samplings may be needed to identify dermatophyte infection.• Skin biopsy specimens revealing folliculitis and/or furunculosis should raise the suspicion of demodicosis or an infectious agent.• Dermatophyte cultures should be allowed to grow for at least 21 days.• In-house dermatophyte cultures should be incubated at temperatures between 75° to 80° F.