Primary & Secondary Keratinization Disorders
Sandra Sargent, DVM, DACVD, Pittsburgh Veterinary Specialty & Emergency Center, Pittsburgh, Pennsylvania
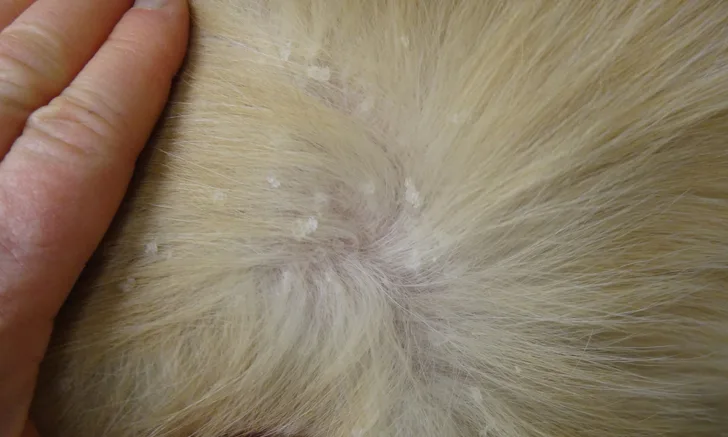
What is the difference between primary and secondary keratinization disorders?
Chronic seborrheic skin disease is aesthetically displeasing and can adversely affect the human–animal bond. Nonspecific descriptive terms such as seborrhea oleosa, seborrhea sicca, and seborrheic dermatitis are commonly used to describe seborrhea, but there is confusion around these terms. In veterinary medicine, seborrhea sicca is used to describe focal or diffuse scaling of the skin with the accumulation of white nonadherent scales and a dull dry coat. The opposite, seborrhea oleosa, refers to greasy skin and hairs.1 Many patients, however, have both flaky and greasy skin; thus, although these terms are descriptive, they may not be particularly helpful, as the conditions can be caused by a large number of underlying diseases.
Physicians use the term seborrheic dermatitis to refer to a chronic inflammatory disorder affecting areas of the head and trunk where, in humans, sebaceous glands are prominent.2 Veterinary clients may be frustrated when they present their pet for seborrhea treatment and are told that seborrhea is rarely a specific diagnosis but simply a descriptive term. They may fail to understand why a detailed history, examination, and further testing are necessary to determine the underlying cause.
When treating a patient with scaly or seborrheic skin, it is important to determine whether the scaling is a primary keratinization defect or secondary to another skin or internal disease. In primary keratinization disorders, the excessive scale is caused by a direct defect in one or more steps in stratum corneum formation. Secondary disorders (ie, those in which seborrhea develops as a result of another condition3) account for at least 80% of all seborrhea cases; it is critical to rule out such secondary disorders before diagnosing primary keratinization dermatoses.4
Most cases of secondary seborrhea have a good prognosis if the underlying cause is identified and treated successfully. Primary keratinization diseases are more difficult to control and usually require lifelong management, which is often labor-intensive and costly.
Secondary Disorders
Because they are common, secondary seborrheic disorders (Table 1) should be an immediate consideration on initial examination. Multiple conditions often occur simultaneously, and almost every dermatologic disorder can result in seborrheic signs.
Causes of secondary seborrhea in dogs5
A good dermatologic history discloses age of onset, seasonality, presence of pruritus, and whether any other pets or humans in the household are affected. Because diseases of other body systems can cause these dermatoses, the clinician should inquire whether other abnormalities such as polyuria, polydipsia, polyphagia, heat-seeking behavior, appetite changes, or weight gain or loss have been observed.
Physical examination of the skin and other systems can provide many clues for diagnosis. A minimum dermatologic database (eg, skin scrapings, impression cytology, fungal culture) should be collected. Secondary bacterial infections should be identified by recognizing lesions caused by infection (eg, papules, pustules, epidermal collarettes) and by sampling these lesions for microscopy.
Identified infections should be treated with appropriate oral and/or topical therapy. In older patients or those with signs consistent with internal disease, a CBC, serum chemistry profile, and thyroid hormone panel are important in ruling out internal secondary causes.
Primary Disorders
True keratinization defects (Table 2) are much less common in dogs and even more rare in cats; therefore, this discussion will focus on canine diseases. Many primary keratinization disorders are hereditary, so affected animals should not be bred.3
Primary keratinization defects4
Primary canine seborrhea has long been considered an inherited disorder of keratinization; it is most commonly recognized in the American cocker spaniel, English springer spaniel, West Highland white terrier, and basset hound.1 Diagnosis can often be complicated because many of these breeds are also commonly affected with allergic skin disease.1
A recent study questioned whether primary seborrhea is a true entity.3 As the role of Malassezia pachydermatis and staphylococcal infections have become more widely recognized, many cases that would have been labeled primary seborrhea in the past are now recognized as pyoderma, M pachydermatis dermatitis, allergic dermatitis, or sebaceous adenitis. Primary seborrhea may be an adaptive response rather than a true keratinization defect, and primary seborrhea may not be considered a true entity.3
If the more common causes of secondary seborrhea are ruled out and/or the signalment and history are consistent with a primary disorder, the following diseases, which result in similar clinical signs and can be easily confused, should be carefully considered:
Vitamin A-Responsive Dermatosis
This disorder is described primarily in the cocker spaniel, although it has also been reported in the Labrador retriever, miniature schnauzer, and Gordon setter.3 It is characterized by an adult-onset seborrheic skin disease with significant follicular plugging and casts as well as hyperkeratotic plaques. Ceruminous otitis is also common. The pronounced follicular plugging or casts is highly suggestive, although other causes (eg, hypercortisolism, sebaceous adenitis, demodicosis) can cause similar changes, and secondary infections can complicate diagnosis. Diagnosis is confirmed via biopsy and response to treatment with Vitamin A (ie, retinol).1
Ichthyosis
Ichthyosis is a congenital skin disease characterized by excessive hyperkeratosis on all skin surfaces, including pads. Ichthyosis has been recognized in a variety of breeds, including the golden retriever, West Highland white terrier, American bulldog, Jack Russell terrier, Norfolk terrier, and Cavalier King Charles spaniel.1
Most of these patients are obviously abnormal at birth or soon thereafter; however, in the golden retriever, lesions can be subtle and may not be recognized until adulthood.6,7 Large sheets of scale are seen on the hair shafts, and large adherent scales are seen on sparsely haired skin. The diagnosis can be confirmed by biopsy and, in some breeds, genetic testing.* Allergic skin disease is also common in these breeds, further complicating diagnosis and treatment.
Clients should be counseled that ichthyosis is incurable and can be difficult to manage, especially in more severely affected dogs. Many golden retrievers are more mildly affected, and, although the worst aspect for owners is a cosmetically displeasing skin and coat, this breed is at higher risk for secondary skin infections. Topical treatments and fatty acids remain the treatment of choice for all forms of ichthyosis.3
Schnauzer Comedo Syndrome
Schnauzer comedo syndrome is a follicular keratinization defect occurring exclusively in miniature schnauzers1; it is seen more commonly in young adults and is characterized by crusting and multiple waxy comedones located along the dorsal midline of the dog. The underlying cause is thought to be an inherited developmental defect in the hair follicle that results in abnormal keratinization with subsequent comedone formation, follicular plugging, and secondary bacterial folliculitis.1 Most affected dogs will respond to keratolytic and follicular flushing agents (eg, benzoyl peroxide shampoo). Secondary bacterial folliculitis should be controlled with antibiotic therapy.1 The condition is lifelong, but most cases can be controlled with chronic maintenance therapy.
Ear Margin Dermatosis
Ear margin dermatosis is characterized by subclinical, bilaterally symmetrical keratinization disorder confined to the ear margins. It is most commonly seen in dachshunds.8 Varying amounts of scale are found along the edge of the pinna. Follicular casts (ie, accumulation of keratinous debris around the hair shaft seen protruding from the follicular ostium or present when hairs are plucked and examined) may be prominent, and the underlying skin appears uninflamed. The condition typically occurs at an early age and waxes and wanes chronically with or without treatment. If the ear margins are intensely pruritic, sarcoptic mange should be considered. If more severe crusting, ulceration, or fissures are present, vasculitis should be considered and biopsies may be necessary for a definitive diagnosis. Because patients with ear margin dermatosis are typically subclinical, treatment may not be necessary, and aggressive treatment may worsen the condition.8 If desired, the scale and hair casts can be removed and kept at a minimum via application of topical keratolytic or moisturizing agents. A topical product containing phytosphingosine has been reported to be helpful.1
*Genetic testing for ichthyosis is available for golden retrievers (Optigen) and American bulldogs (University of Pennsylvania).