Postintubation Tracheal Tears in Cats
Jane E. Quandt, DVM, MS, DACVAA, DACVECC, University of Georgia
Tracheal tears commonly occur in cats following dental procedures,1 often due to overinflation of the endotracheal tube cuff; this is typically done to prevent fluid or debris from leaking around the endotracheal tube.1 Low-volume, high-pressure cuffs may be more likely to cause tears than are high-volume, low-pressure cuffs. Other causes of tracheal tears include trauma, improper endotracheal tube placement and/or size, injury from an endotracheal tube stylet, and failure to deflate the cuff when repositioning and/or extubating.2,3 In 2 feline case series (n = 16 and n = 20), 2 cats had tracheal ruptures induced by a stylet; all other cases of tracheal rupture were caused by cuff overinflation.2,4 In intubated cats, approximately 1.6 ± 0.7 mL of air is needed to form an airtight seal; more than 6 mL of air in the cuff can increase the risk for tracheal rupture.2
Ruptures are often linear tears of the trachealis muscle. Tears extending into the carina typically have a poorer prognosis.2 Most commonly, tears are longitudinal, 2 to 5 cm in length, extrathoracic, and located in the dorsal longitudinal trachealis muscle or dorsolateral aspect of the trachea at the junction of the tracheal rings.2,4 In a feline cadaver study, ruptures were linear and located at the attachment of the trachealis muscle to the tracheal cartilage, which was also located directly over the enlarged cuff.2 In the cadavers, the trachealis muscle split from the left side of the trachea and rolled to the right, which suggests there is less support on the left side of the trachea in cats.2
Clinical Signs
The endotracheal tube should be inspected after every extubation. If blood on the endotracheal tube and/or aberrant swelling or crepitus in the neck region—potentially extending to the sternal area—are present, a tear could be involved.3 Clinical signs generally develop 4 hours to 6 days after the anesthetic episode2 because the mediastinum, which tightly covers the trachea, may prevent air from escaping until coughing and tracheal irritation develop, which then allows air to escape.2 Subcutaneous emphysema is evident in all tracheal tear cases due to the migration of air into the mediastinum and subsequently into the subcutaneous tissues.1,2,4 It has been reported in 100% of tracheal tear cases.5,6 Other clinical signs of tracheal tears include anorexia, coughing, noise from the upper airway, tachypnea, expiratory dyspnea, gagging, exertional cyanosis, exercise intolerance, and muffled heart sounds.1,4 Fever may also develop as a sign of possible sepsis, in which case antibiotic therapy should be instituted.2 In tracheal tear cases, air dissects along connective tissue planes in the cervical area and surrounds the trachea; air then travels into the mediastinum, which can cause pneumomediastinum.4 Pneumothorax may develop if pressure is high enough to rupture the mediastinum.1 Tension pneumothorax may develop if the tracheal defect acts as a one-way valve.4,5

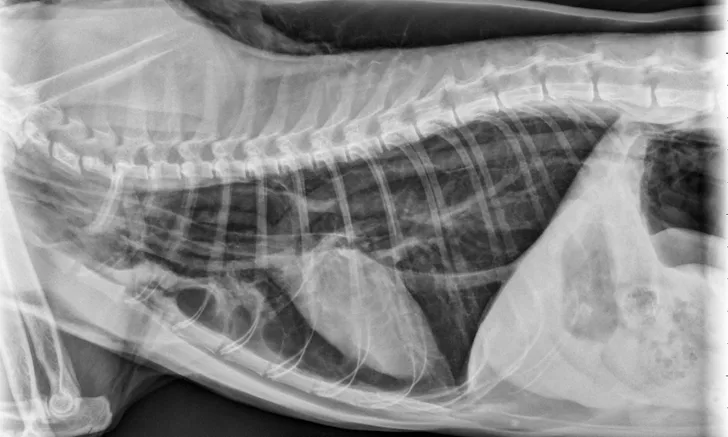
Figure 1 Radiographic image of a cat with a tracheal tear and severe subcutaneous emphysema
Diagnosis
Radiography can be used to diagnose tracheal tears (Figures 1 and 2). If a tracheal tear is present, thoracic radiographs may reveal pneumomediastinum, subcutaneous emphysema, pneumoretroperitoneum, hyperinflated lung fields, a gas-filled pseudo-airway at the level of the rupture, focal narrowing of the tracheal lumen, and/or pneumothorax if the mediastinum has been perforated due to air pressure.3
CT can also be used to diagnose a tracheal tear. CT can provide the location and extent of the tear, define and differentiate soft tissue structures, and provide secondary reconstruction of the planes that may help determine the length of the tear as well as provide valuable information for surgical planning.3
Locating the Tear
Tracheoscopy can be used to determine the most appropriate treatment approach (eg, whether surgery is necessary) and to observe the rupture. During tracheoscopy, the cat should not be intubated, as this may obscure the lesion and, if the scope is placed through the endotracheal tube, obstruct the endotracheal tube. An injectable anesthetic technique, such as hydromorphone (0.1 mg/kg IV) and propofol (4 mg/kg IV) titrated to effect with oxygen insufflation, has been used for tracheoscopy.5 Injectable anesthesia can be used during tracheoscopy but must be carefully titrated to effect to avoid apnea. Ketamine (1-2 mg/kg titrated to effect) combined with a benzodiazepine (eg, diazepam, midazolam [0.2 mg/kg IV]) or alfaxalone (1-3 mg/kg IV titrated to effect) can also be used. Oxygen insufflation should be provided to help prevent hypoxemia.
However, if the patient cannot be ventilated, referral to a tertiary care center should be considered. Once the lesion has been identified, before surgery, the patient should be intubated for oxygen and ventilator support.5 The endotracheal tube should be smaller than the tracheal lumen, and extreme caution should be used when intubating patients with a suspected or confirmed tear. Ideally, the anesthetic plane should be light enough that the patient maintains spontaneous respiration. If possible, positive pressure ventilation should be avoided to prevent further emphysema and pneumothorax. If the patient does not breathe, assisted breathing should be provided with minimal pressure (≤10 cm H2O) to provide adequate ventilation.1 The endotracheal tube must pass the tear site.
Treatment
Patients with mild tears and no more than moderate dyspnea can be treated with conservative medical management2,3 consisting of cage rest and possible oxygen supplementation. Resolution of clinical signs can range from 2 days to 5 weeks.2 Sedative administration may help prevent vocalization.4 Potential sedatives for such cases include butorphanol (0.2-0.4 mg/kg IV), midazolam (0.25 mg/kg IV), acepromazine (0.01-0.03 mg/kg IV or IM), buprenorphine (0.01-0.02 mg/kg IV), and opioid–tranquilizer combinations.
All cats with severe respiratory compromise should be treated surgically.4 Immediate surgery is required in patients with severe dyspnea, open-mouth breathing despite oxygen treatment, or worsening subcutaneous emphysema.4
If possible, in patients with a tracheal tear confirmed before anesthesia, the ventral cervical area and the right thoracic wall should be clipped; this allows for a shorter preparation time while the patient is anesthetized. The surgeon should be present during intubation in case a tension pneumothorax develops and emergent surgery is needed. The anesthetic plan should include a smooth IV induction technique and intubation with an endotracheal tube lumen that is smaller than normal to avoid interference on the trachea during surgery. However, the endotracheal tube should still be long enough to pass below the tear.1,5,7 In cases in which the tear extends to the carina, there is a higher mortality rate during surgery.2,7,8 Cats can be intubated for surgery, although an injectable technique may be preferred.
Of note, death can occur during surgery in cases in which it is not possible to ventilate the cat due to the distal location of the tear.2,5,8 Tracheal tears may allow for the inhalant to escape from the respiratory tract and into the surrounding environment; this will expose team members to the inhalant and can make it difficult to maintain an appropriate anesthetic plane. Once the tear has been repaired, the cuff can be inflated until no gas is detected escaping from around the endotracheal tube when a positive pressure of 15 cm H2O is applied via rebreathing bag compression.5 If using an injectable anesthesia, inflating the cuff may not be necessary unless positive pressure ventilation is required, but cuff placement should be avoided near the area of the repaired tear.
A ventral midline approach should be used, as it may be necessary to split the first several sternebrae to repair ruptures in the thoracic inlet. All reported tears have occurred at the junction of the tracheal rings and trachealis muscle.6 The trachea can be repaired with simple interrupted or simple continuous sutures with absorbable or nonabsorbable material.2,4 When performing surgical repairs, care should be taken to protect the recurrent laryngeal nerves during tracheal exposure.3
Resolution of subcutaneous emphysema can take 1 to 6 weeks (average, 2 weeks).4 Resolution is slow because absorption of air depends on the diffusion gradient of nitrogen, which is small.4 To speed the absorption, treatment with 95% oxygen over 4 hours has been used in humans and may be helpful in cats.4 This treatment decreases the partial pressure of nitrogen in the blood and promotes diffusion of nitrogen from the interstitium into the blood4; however, this is not commonly performed in cats because of the difficulty of providing 95% oxygen via methods other than intubation and anesthesia.
Prevention & Conclusion
For any procedure, an appropriately sized endotracheal tube should be used in cats requiring intubation; for most patients, this will be a tube approximately 3.5 to 4.5 mm in diameter. All air should be removed from the cuff before intubation. The cuff should be inflated incrementally with 0.5 mL of air until pressure on the reservoir bag increases to 15 to 20 cm H2O and no audible amount of air or only a small amount of air escapes around the endotracheal tube. A 3-mL syringe should be used for cuff inflation. During a dental procedure, the cuff is commonly overinflated to prevent water from entering the lungs; this should be avoided to prevent possible tracheal tearing. Ruptures of greatest length tend to be associated with high-volume, low-pressure endotracheal tubes.2 Using the back pressure on the inflation syringe and assessing the size of the pilot balloon are not reliable indicators of cuff size or pressure.2 In addition, it is critical to disconnect the anesthetic circuit when changing a patient’s position and to deflate the cuff before extubation.3
Most tracheal tears in cats are iatrogenic and occur with cuff overinflation, as seen with dental procedures. This injury can be avoided with proper cuff inflation and postural drainage. Suction can be placed in the pharyngeal region to collect fluid.9 The pharynx can be packed with sponges to prevent aspiration and replaced when they become saturated.9 The sponges must be removed at the end of the procedure and before extubation to prevent possible laryngeal occlusion. When the dental procedure is complete, the mouth and pharyngeal area should be examined to make sure no sponges are left in place.
Tracheal tears can be life threatening and difficult to repair but can be prevented. Team members should pay appropriate attention to endotracheal tube size, cuff inflation, and patient positioning.