Poorly Controlled Pruritus in an Atopic Dog
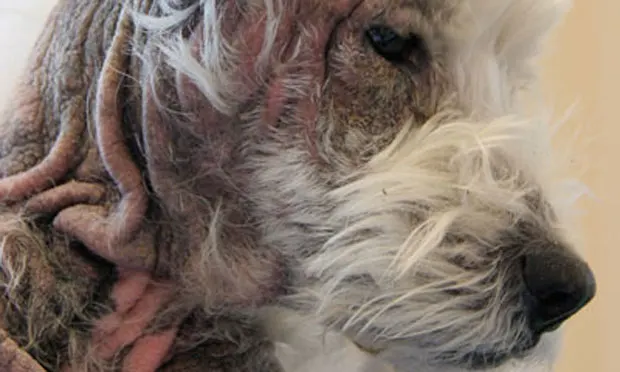
A 6-year-old, 8-kg neutered male West Highland white terrier with intense pruritus was presented for evaluation.
History. The dog had a 5-year history of nonseasonal generalized pruritic skin disease that had previously improved with oral (prednisone) and injectable (dexamethasone and triamcinolone) glucocorticoids, as well as oral antibiotics (cephalexin). Two previous allergen-specific IgE serologic tests had been performed, and allergen-specific immunotherapy had been instituted without sustained clinical improvement. Royal Canin Hypoallergenic HP 19 (royalcanin.us) diet had been fed exclusively for the previous 12 months. Additional clinical signs included frequent soft feces (several times per week), flatulence, and increased defecation (3–4 times per day).

Dermatologic Examination. Dermatologic examination findings included severe alopecia; hyperpigmentation; and lichenification with moderate erythema, yellow scale, and multifocal serous crusts extending from the periocular areas to the ventral and lateral aspects of the cervical area (Figure 1 above: _Periocular, facial, and cervical lesions), axillae, entire ventrum, and all aspects of the limbs (Figure 2; Lesions evident on the ventral abdomen, inguinal areas, and hindlimbs)_. Multifocal areas of alopecia, erythema, and serohemorrhagic crusts with heavy adherent scale were present over the dorsal and lateral aspects of the chest. Erythema and moisture were present within the interdigital spaces, as well as the palmar and plantar aspects between the foot pads.
Figure 2; Lesions evident on the ventral abdomen, inguinal areas, and hindlimbs.
Physical Examination. Physical examination findings revealed mild peripheral lymphadenopathy.
Diagnostic Testing.
Superficial and deep skin scrapings:
Negative for Sarcoptes and Demodex mites
Skin cytologic testing:
Impression smear beneath crust showed moderate degenerate neutrophils and cocci bacteria (often intracellular), mild macrophages (0–2/oil-immersion field), and erythrocytes
Acetate tape preparation from several sites showed findings similar to those of impression smear, with large numbers of Malassezia organisms (> 10/oil-immersion field)
Flea combing: Negative
Laboratory Analysis. A complete blood count, serum biochemical profile, total thyroxine level, urinalysis, evaluation for fecal ova and parasites, and a Giardia enzyme-linked immunosorbent assay were performed. The only abnormalities were a mild increase in globulins (3.9 g/dL; reference range, 1.6–3.6 g/dL), absolute neutrophilia (neutrophil count, 16,709; reference range, 2060–10,600), monocytosis (monocyte count, 1085; reference range, 0–845), and eosinophilia (eosinophil count, 1519; reference range, 0–1200).
Related Article: Pododermatitis
Ask Yourself...
What is your treatment plan for this patient?
A. Treat the bacterial and yeast infections with appropriate systemic and topical antimicrobial therapy and rule out scabiesB. Begin immunomodulatory therapy with systemic glucocorticoids or cyclosporineC. Recommend an intradermal skin test to further evaluate for airborne allergyD. Perform another food elimination dietary trialE. A and D
Correct answer:E. Treat the bacterial and yeast infections with appropriate systemic and topical antimicrobial therapy and rule out scabies; perform another food elimination dietary trial
There were several possible causes of pruritus in this dog, including allergic skin disease (atopy, adverse reaction to food, flea allergy dermatitis), infectious skin disease, and occult ectoparasitism (sarcoptic mange). Clinical and cytologic evidence confirmed skin infections due to bacteria (cocci, most likely Staphylococcus pseudintermedius) and yeast (Malassezia species), both of which contribute to severe pruritus.
The first step in treating the superficial skin infection is to determine the degree of residual pruritus that may be attributable to other causes. Bacterial pyoderma and yeast dermatitis require a minimum of 3 to 4 weeks of systemic antibiotic and antifungal therapy, respectively. However, in severe cases, treatment lasting up to 6 weeks is not uncommon. Shampoo therapy is an important adjunct to resolving infection, improving the condition of the skin, and reducing the risk for recurrent infection. Although concurrent glucocorticoid or cyclosporine therapy may decrease pruritus, it is not indicated in the presence of infection, may slow resolution, and can interfere with determination of the underlying cause.
The age at onset, breed, previous response to glucocorticoid therapy, and results of allergen-specific IgE serologic testing all may support or raise suspicion of an underlying diagnosis of atopy. Although I prefer intradermal skin testing alone, or in combination with serologic testing, this test could not be performed in this patient due to the poor condition of the skin.
Related Article: Canine Scaling Disorders
Initial Therapeutic Plan. A 30-day course of cefpodoxime, 7 mg/kg PO Q 24 H (Simplicef, pfizerah.com), and fluconazole, 5 mg/kg PO Q 24 H, was initiated. Bathing in a shampoo containing 2% chlorhexidine and miconazole (Malaseb, tevaanimalhealth.com) was recommended twice weekly. Topical selamectin (Revolution, pfizerah.com) was prescribed monthly to prevent heartworms and rule out scabies.
A home-cooked, balanced, food elimination dietary trial with rabbit and sweet potato was initiated because of the gastrointestinal signs; improvement in gastrointestinal and skin signs may not be evident until after the diet is fed exclusively for 10 to 12 weeks.
Reevaluation at 2 Weeks. The dermatologic examination revealed clinical improvement and the owner reported reduced skin odor and pruritus. Flatulence had also become less frequent. Repeat skin cytologic testing revealed that the yeast and bacterial infections were resolving.
Because evidence supported underlying atopic dermatitis, therapy with cyclosporine, 5 mg/kg PO Q 24 H (Atopica, ah.novartis.com), was initiated. The owner was advised to continue the other medications and the food elimination dietary trial as previously prescribed.

Reevaluation at 6 Weeks. The patient’s condition continued to improve, with no evidence of infection, near-resolution of skin lesions, and noticeable hair regrowth . Generalized pruritus was reduced by 80%. Fecal consistency and frequency also normalized. The cyclosporine dose was reduced to 5 mg/kg PO Q 48 H.

_
Figures 3 and 4; Clinical improvement with near resolution of skin lesions and noticeable hair regrowth 6 weeks after initiation of treatment
_

Long-Term Follow-Up. The patient was subsequently reevaluated 12 weeks after initiation of the food elimination dietary trial. There were no significant findings on dermatologic examination (Figure 5: Complete resolution of skin lesions at completion of food elimination dietary trial__).
Further attempts to reduce the cyclosporine therapy resulted in increased pruritus and the dog was reevaluated to rule out skin infection as a cause or consequence of pruritus. A food challenge was performed by reintroducing Royal Canin Hypoallergenic HP 19; a marked exacerbation in pruritus was reported within 2 days of the dog consuming the diet. These signs resolved within 5 days of returning to the home-cooked rabbit and potato diet. The dog was subsequently maintained on Royal Canin Veterinary Diet Rabbit and Potato formula, without incident.
Long-term control of infection and pruritus was very effective with the combination of once- to twice-weekly shampoo therapy, oral cyclosporine, allergen-specific immunotherapy, and avoidance of dietary indiscretion. Individual challenge with select proteins was not pursued in this case, but I feel that allergy to soy hydrolysate was probably involved in this patient’s adverse reaction to food.
Discussion. An estimated 5% of all dermatoses in dogs and 10% to 15% of all allergic skin conditions are caused by adverse reactions to food. Concurrent gastrointestinal signs, including intermittent vomiting, loose stool, chronic diarrhea, increased number of bowel movements, and borborygmus are reported in 10% to 15% of cases.1 A Swiss study documented a higher incidence of gastrointestinal signs in 31% of dogs with adverse food reactions.2 Concurrent allergic diseases (atopy or flea allergy dermatitis) are diagnosed in 20% to 30% of patients with food allergy.3,4
Intradermal skin, patch, and food-specific IgE testing are not of value in the diagnosis of cutaneous adverse reaction to food because of their low sensitivity and specificity. The gold standard for diagnosis is observance of improvement or resolution of clinical signs after feeding an elimination diet for 8 to 12 weeks, followed by recurrence of clinical signs (often pruritus) when the patient is challenged with previously consumed food items.
An appropriate elimination diet should consist of a novel protein and carbohydrate source that the affected patient has not previously consumed. Although feeding a commercially available diet often enhances owner adherence, many dermatologists feel that home-prepared diets are more reliable in the diagnosis of food allergy.
With hydrolyzed diets, the protein source—usually a common protein such as chicken or soy—is degraded into peptides and amino acids by enzymes to reduce, but not eliminate, the allergenicity of proteins.5 A recent study demonstrated that a variable proportion (up to 50%) of dogs will exhibit worsening of clinical signs when fed hydrolysate diets derived from proteins that are involved in their adverse reaction to food.6 Therefore, these diets are probably best used in cases where there is no suspicion of hypersensitivity to the diet’s individual components.
Take-Home Messages
• Patients with concurrent bacterial and Malassezia yeast infections may be intensely pruritic and require both systemic antibiotic and antifungal therapy.• A thorough diagnostic investigation, including evaluation for concurrent allergic skin disease and secondary skin infections as well as ruling out scabies by treatment (even if superficial skin scrapes are negative), is critical in any patient with poorly controlled atopic dermatitis.• A dietary trial with multiple diets, including a home-cooked diet, may be needed to diagnose an adverse reaction to food accurately.