Pododermatitis
Karen A. Moriello, DVM, DACVD, University of Wisconsin–Madison
Profile
Definition
Pododermatitis describes any inflammatory skin disease that involves the paw.1 It is a common dermatologic problem associated with many underlying skin diseases.
Signalment
Species. Inflammatory lesions on the feet are more common in dogs than cats.
Breed Predilection. Dogs or cats at risk for dermatologic diseases involving the paw may be at increased risk for pododermatitis as a complication of the underlying disease.• Idiopathic sterile granulomas limited to the feet are common in English bulldogs, Great Danes, and dachshunds.1• Hyperkeratosis of the footpad can occur in dogs predisposed to disorders of cornification (eg, cocker spaniels). Familial footpad hyperkeratosis has been reported in Irish terriers, French mastiffs, kerry blue terriers, Labrador retrievers, golden retrievers, and mixed-breed dogs.2,3• Other breed-related predilections include zinc-responsive skin diseases of sled dogs (eg, Siberian husky, Alaskan malamute); Malassezia overgrowth is common in Devon rex cats.4-6
Risk Factors
• Dermatologic diseases that involve the paw or footpad are a risk factor for allergic diseases, immune-mediated diseases, diseases of cornification, parasitic diseases (demodicosis, hookworm dermatitis, Leishmania infection), metabolic diseases (eg, hepatocutaneous syndrome), and neoplastic diseases (eg, mycosis fungoides).• Dogs that dig, work (eg, hunting and aid dogs), or spend a lot of time outdoors are at risk for traumatic pododermatitis.• Dogs with conformational disorders and obesity are at risk for pododermatitis due to abnormal weight-bearing distribution and secondary increased friction between the skin and footpads.
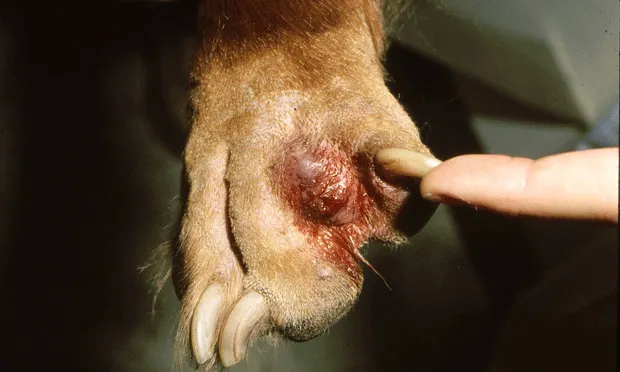
Figure 1. Interdigital furuncle
Pathophysiology
• The pathophysiology of pododermatitis varies depending on the underlying disease. Any disease, including chronic rubbing of opposed surfaces, that causes folliculitis and subsequent furunculosis can lead to chronic pododermatitis.• Some examples:- Demodicosis: Proliferation of mites-which results in secondary folliculitis, furunculosis, bacterial infection, and self-trauma-leads to inflammation of the dorsal, ventral, and interdigital areas.-Pemphigus foliaceus: Crusting of the footpads results from rupture of primary lesions (pustules) with secondary crusting.
Figure 2. Pododermatitis due to atopy. Note the hair loss due to licking of the dorsum of the paws.
Signs
History. Presenting client complaints vary by the disease and how observant the client is, but may include:• Foot licking and salivary staining• Redness• Bleeding paws or digits• Nail biting• Odor• Sloughing pads or nails• Lumps• Lameness• Changes associated with systemic illness (eg, anorexia, weight loss, vomiting).
A thorough dermatologic history should suggest clues to the cause.• Lesion location (footpad, haired portion, or both; interdigital or palmar/plantar aspects)• Number of paws involved (1 paw may indicate trauma or a foreign body, front paw involvement should prompt questions about whether the dog spends much time outdoors digging, working or hunting dogs or canine athletes usually have all 4 paws involved)• Seasonal versus nonseasonal, pruritic versus nonpruritic• Age of onset• Environment
Figure 3. Severe footpad crusting due to hepatocutaneous syndrome
History of the lesions and response to previous therapy can help narrow the differential diagnosis. Response to corticosteroids may suggest allergies, irritant reactions, and, with high doses, immune-mediated diseases. Bacterial or yeast infections of the feet are almost always due to an underlying cause; thus, response to antimicrobial therapy needs to be carefully assessed to best identify the underlying cause of the infections.
Physical Examination. A complete dermatologic examination and assessment of all 4 paws should be done. Sedation is recommended to obtain a thorough examination and core diagnostic tests.
• Salivary staining on paws suggests pruritus.• Interdigital erythema limited to the plantar surfaces may indicate irritant or allergic contact reaction.• Nodular lesions, thickening, and scarring of interdigital skin suggest previous deep pyoderma and furunculosis. This is common with foreign-body reactions to keratin and chronic pododemodicosis.• Interdigital furuncles are common with atopy and in dogs with conformational triggers of pododermatitis.• Nail bed debris or paronychia may be associated with Malassezia1,2 overgrowth.• Hair loss, scales, and abnormal nails suggest dermatophytosis.• Severe pododermatitis can be associated with regional lymphadenopathy.• Nodular lesions on the dorsum of the paw indicate tumors, sterile granuloma syndrome, and nodular dermatofibrosis.
Pain Index
Pododermatitis due to deep pyoderma and hepatocutaneous syndrome with subsequent cracking and splitting of the paws can be severely painful. Tramadol (5 mg/kg PO Q 8 to 12 H) is beneficial.
Diagnosis
Differential Diagnosis
Definitive diagnosis of the underlying cause involves a thorough history, careful clinical examination, interpretation of core diagnostic test results, and progression through a logical diagnostic evaluation. The most common diagnoses, based on predominant clinical presentation of pododermatitis, include:• Dogs:- Inflammatory/exudative lesions and/or interdigital furunculus (Figure 1): Bacterial pyoderma, dermatophytosis with or without concurrent Malassezia overgrowth, mycoses, deep mycoses, pemphigus foliaceus, demodicosis, diffuse foreign-body reaction, tick infestation- Pruritus (variable to severe): Malassezia overgrowth, hookworm dermatitis, Pelodera dermatitis, demodicosis, tick infestation - Erythema, moderate pruritus, salivary staining, dorsal hair loss: Atopy and food allergy with or without concurrent bacterial/yeast overgrowth (Figure 2), allergic contact reaction, demodicosis, tick infestation- Hyperkeratotic or crusted and fissured footpads: Cornification disorder, zinc responsive dermatosis, hepatocutaneous syndrome (Figure 3), pemphigus foliaceus, mycosis fugoides, Leishmania infection, systemic lupus erythematosis- Nodular: Foreign-body reaction to keratin or plant material (awns), neoplasia, nodular dermatofibrosis syndrome, sterile granuloma/pyogranuloma, demodicosis - Sloughing footpads:Vasculitis, trauma, hookworm dermatitis, Pelodera infection, erythema multiforme, toxic epidermal necrolysis, burns
• Cats:- Crusted footpads/nail beds: Dermatophytosis, pemphigus foliaceus, Notoedres- Hair loss and erythema: Dermatophytosis, Notoedres,food allergy, atopy, Malassezia infection - Foot chewing & nail biting: Malassezia infection,allergic causes, Notoedres- Puffy footpads, footpad ulcers, discolored footpads: Eosinophilic granuloma, neoplasia, plasma cell pododermatitis7
Laboratory Findings & Imaging
• Skin scrapings: Demodicosis and Pelodera infection (Long-standing cases of pododemodicosis may require diagnosis via biopsy because of scar tissue.)• Skin cytology: Bacterial or yeast overgrowth• Nail bed cytology: Brown exudate, usually indicating Malassezia organisms• Dermatophyte culture: Indicated if nail fold is involved or furunculosis is suspected • Bacterial culture: Indicated for deep, recurrent, or nonresponsive bacterial pyoderma• Fecal flotation: Hookworm dermatitis• Skin biopsy: Useful for definitive diagnosis of many diseases (Biopsy should be done for nodular, recurrent, or chronic pododermatitis to rule out demodicosis.)• Allergy or food trial: Indicated when history and clinical signs are compatible with allergies or when patients have nonseasonal pruritus or relapsing bacterial or yeast pododermatitis (Regardless of how compelling the history is for allergies, core diagnostic tests should also be performed.)• Radiography: Helpful to diagnose foreign bodies, fractures of digits, tumors• Ultrasonography of abdomen: Helpful in cases of dermatofibromas to rule out concurrent renal cyst adenocarcinomas8 • Complete blood count, serum biochemical panel, urinalysis: Useful when systemic disease is known or suspected.
Treatment
Successful treatment of pododermatitis depends on definitive diagnosis of the underlying cause. Unless complicated surgery is needed, most patients are managed as outpatients.
Medical Management
• Bacterial infections: Interdigital furunculosis usually requires at least 6 weeks of antibiotics depending on culture and sensitivity (especially given the increasing prevalence of methicillin-resistant Staphylo-cocci). Concurrent bathing in a medicated shampoo (benzoyl peroxide or a chlorhexidine and ketoconazole or miconazole combination) several times a week is beneficial. Topical application of mupirocin ointment to focal areas of abscessation can be helpful. Concurrent treatment may be needed for Malassezia coinfection.• Yeast overgrowth: In dogs, clipping the hair coat short aids in bathing of paws in a combination chlorhexidine and ketoconazole or miconazole combination at least twice a week. Concurrent administration of ketoconazole (5-10 mg/kg Q 24 H for 21-30 days) is recommended. If yeast overgrowth results from atopy or a disorder of cornification, 1% triamcinolone acetate spray can be applied topically to manage pruritus.
In cats, oral itraconazole (5 mg/kg Q 24 H for 30 days or given on a week-on/week-off basis) can be used. In an otherwise healthy adult cat, this should prompt a search for an underlying medical cause (eg, diabetes mellitus).
• Pruritus: If pruritus management of underlying atopy or food allergy is inadequate or if atopy is seasonal and the feet are a major target, topical 1% triamcinolone acetate spray is effective. In some cases, noninflammatory doses of oral prednisone (0.5 mg/kg PO) for short periods may be needed.
• Pododemodicosis: Conventional therapy for demodicosis with concurrent antimicrobial therapy is the treatment of choice. Treat the entire dog, not just the paws.
• Hyperkeratosis: In dogs with cornification disorders, hyperkeratosis of the footpads can be managed by veterinary "pedicure" (ie, trimming excessive hyperkeratosis). Clients report that soaking the paws and hydrating them before application of salicylic acid helps delay overgrowth. Propylene glycol can be used as an emollient, but clients need to be warned that it can be messy.
• Hepatocutaneous syndrome: Management of footpad problems associated with this disease is challenging. Footpads are thickened, crusted, fissured, and very painful. Secondary Malassezia infections are often a complication. Fluconazole (5 mg/kg Q 24 H) can be used and I also administer tramadol (5 mg/kg PO Q 8-12 H or as needed). Daily footpad soakings using warm, moist, or wet compresses wrapped around the paws for 10 to 15 minutes are helpful. Applying triple antibiotic ointment or administering concurrent antibiotics can be beneficial.
With IV administration of amino acid solutions weekly or every other week, footpad crusting often improves. Typically, a dog would be treated with 500 ml of 8% to 10% amino acid solution given by slow IV infusion over 12 to 24 hours. The solution must be mixed in with a saline or 5% dextrose solution; follow package directions. Once the patient improves clinically, treatment is repeated every 2 to 4 weeks and is only palliative.
• Feline plasma cell pododermatitis: There is no one "best" treatment. Some cases wax and wane. Some authors advocate changing the type of litter used.1 I treat patients first with doxycycline (10 mg/kg PO Q 24 H for 30 days); some patients need long-term treatment, others require pulse treatment, and some cases respond and do not recur. If treatment fails, consider oral prednisone (4.4 mg/kg PO Q 24 H); cyclosporine (5 mg/kg Q 24 H) is another option. Gold salt injections are another possibility, but complications include bone marrow suppression and renal disease. Surgical removal of part of the pad may be helpful if the area is limited; lameness is a complication.
Surgical
Surgical interventions are needed when foreign bodies are suspected. Surgical removal of plant awns or curettage of draining tracts may be needed. In rare cases of severe pododermatitis with chronic furunculosis and scar tissue, the interdigital webbing can be removed (fusion podoplasty).9 This uncommon procedure is limited to dogs with severe scarring. If there is an underlying undiagnosed cause (eg, atopy), the dog will continue to lick the remaining dorsum and ventrum of the paw.
Activity
If pododermatitis is caused by trauma or repeated activities associated with athletic training, the dog's environment or training should be altered to allow the paws to heal. Some dogs may need protective boots. Dogs with allergic pododermatitis may benefit from avoiding grass at certain times of the year, particularly when it is wet from morning dew.
Client Education
If the underlying cause is an incurable disease, the client needs to understand that pododermatitis will recur. Clients should be educated about how to monitor target clinical signs that indicate a starting or impending relapse. Dogs with chronic pododermatitis as a result of conformational problems will never be cured, and marked remission of clinical signs may not be possible.
Follow-Up
Patient Monitoring
The underlying disease dictates frequency of monitoring.
Prevention
It is difficult to prevent most causes of pododermatitis. Hookworm dermatitis and Pelodera infection can be prevented by routine use of anthelmintics and attention to sanitation. Prevention of traumatic injuries is difficult; the key is rapid recognition to prevent chronic disease.
Complications
In patients receiving systemic antifungal therapy, it is prudent to monitor liver enzymes before therapy and during therapy if the animal becomes ill. In my experience, hepatotoxicity is uncommon.
In General
Relative Cost
Treatment of a case of pododermatitis can vary from $ for simple cases of foreign-body removal and appropriate concurrent care to $$$$ for cases due to life-long (eg, atopy, disorder of cornification) or serious medical diseases (eg, immune-mediated condition, hepatocutaneous syndrome).