Pancreatic Biopsy
J. Brad Case, DVM, MS, DACVS, University of Florida
W. Alex Fox-Alvarez, DVM, MS, DACVS-SA, Community Care Veterinary Specialists, Gainesville, Florida
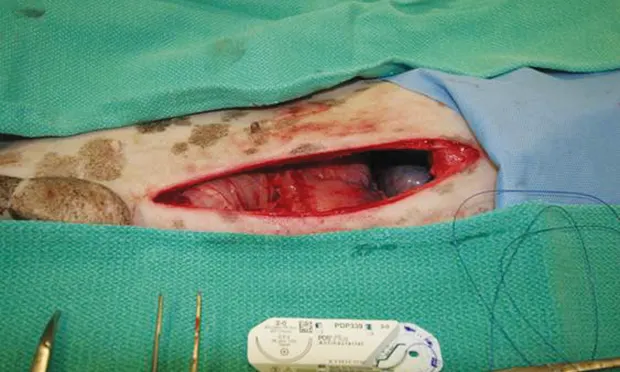
Antemortem diagnosis of pancreatic disease is a challenge. Histopathology remains the gold standard of diagnosis for pancreatic neoplasia and pancreatitis. Pancreatic biopsy provides a definitive diagnosis of pancreatitis, assuming a representative sample is obtained. An open or laparoscopic approach can be made to collect samples.
Open approaches require only standard surgical equipment and allow easy manipulation of tissue and visualization of the entire pancreas (important when sampling focal disease involving the left limb). However, open surgery results in greater tissue injury and pain compared with a laparoscopic approach and may not be favored by some clients or in some cases.
Studies in both human and veterinary medicine have demonstrated laparoscopic procedures to have less tissue trauma and systemic inflammation, lower pain indices, and reduced patient convalescence when compared with analogous procedures performed using an open approach. This decrease in the healing and inflammatory demand postoperatively may be particularly important in patients with delayed healing from metabolic derangements, such as hypoproteinemia, secondary to their pancreatic disease. While this approach provides a magnified, illuminated view of the right limb of the pancreas, the left limb of the pancreas is difficult to evaluate laparoscopically and may require dissection of the omental bursa and repositioning of the patient (beyond the scope of this article). In addition, laparoscopy requires the use of specialized equipment and may take slightly longer to perform for learning practitioners; however, once the procedure can be completed with confidence, the time required can be comparable with that for an open method.
When biopsying the pancreas, if not targeting a specific lesion, the distal aspect of the right or left limb of the pancreas is preferred to decrease the risk for damaging important vascular and pancreatic structures. Care should be taken to avoid major blood vessels (eg, caudal pancreaticoduodenal artery and its branches).
Pancreatic biopsy is a safe procedure. Despite concerns for adverse sequelae after pancreatic biopsy, studies suggest that significant clinical or biochemical abnormalities are uncommon postoperatively.1-4 Patients should be monitored closely for signs of pancreatitis.
Related Article: Surgeon's Corner: Visceral Biopsy Technique
Step-by-Step: Guillotine Biopsy via Laparotomy
What You Will Need
Basic surgery pack (ie, needle holders, DeBakey thumb forceps, mosquito hemostats, Metzenbaum scissors)

STEP 1
Place patient in dorsal recumbency position and follow standard aseptic preparation.
Step-by-Step: Laparoscopic Biopsy
What You Will Need
Videolaparoscopy tower, camera, insufflation tubing, and light cable
2 5-mm trocars and cannulas
5-mm laparoscopic clamshell biopsy forceps
5-mm laparoscope 0°
5-mm laparoscopic blunt probe

FIGURE A
Videolaparoscopy tower
Both Methods
Sterile sample cups for separate diagnostic samples (histopathology, culture)
Culture media
10% formalin for histopathology
Microscope slides for impression cytology
Step-by-Step: Clamshell Biopsy Forceps Method via Laparoscopy

STEP 1
Position patient. Reverse Trendelenburg position (ie, dorsal recumbency, body tilted with head up and feet lower than head, at approximately 15 degrees) with leftward obliquity is the authors’ preferred position for descending limb pancreatic biopsy. Many endoscopists, however, prefer a right lateral approach as it provides an immediate view of the pancreas. The major disadvantage of the right lateral approach is the lack of ability to view the entire liver, which is often indicated given the possibility of concomitant inflammatory or neoplastic disease and limitations of ultrasonography.
The approach described here can provide excellent visualization of the duodenum, liver, extrahepatic biliary system, right kidney, and right limb of the pancreas. The left limb of the pancreas is challenging to view laparoscopically and should not be attempted without significant training and experience.