Pain Management in an Arthritic Senior Cat
Sheilah A. Robertson, BVMS (Hons), PhD, DACVAA, DECVAA, DACAW, DECAWBM (WSEL), CVA, MRCVS, Lap of Love Veterinary Hospice, Gainesville, Florida
History
Josh, a 12-year-old neutered male domestic shorthair cat, was presented for his annual wellness examination. Josh was adopted at 2 years of age into an indoor multicat household; all cats in the household were free-fed the same diet. Dental cleaning was performed with the patient under general anesthesia one year prior.
Physical Examination
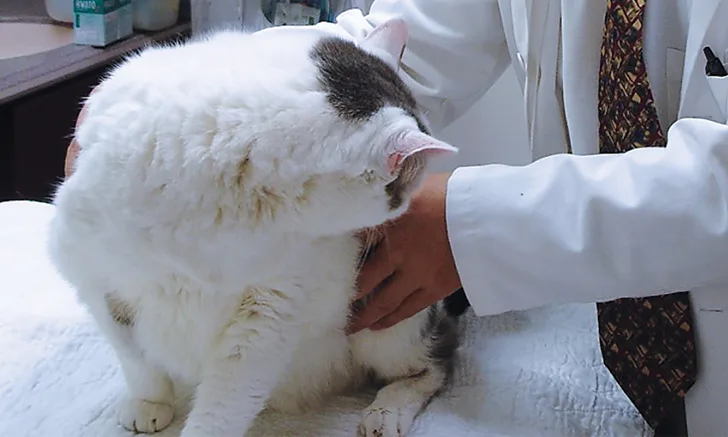
Josh weighed 15.9 lb (7.2 kg), 0.9 lb (0.4 kg) of which had been gained over the past 12 months. BCS was 7 out of 9 as compared with 6 out of 9 the previous year; sarcopenia was evident, particularly over hips and thighs (Figure 1). His coat looked unkempt.

Apparent muscle loss over the hips
A conversation with the owner revealed that Josh had become less active, appeared to sleep more, and had changed his sleeping location from the window ledges to the floor or under the bed. The owner also described Josh as being less social with the other household cats.

A taut muscle band is palpated in the left dorsal midlumbar area, which causes the patient to turn and tense further.
Josh would not walk freely around the examination room, so gait observation was not possible. He would not jump from the examination table, even when coaxed by the owner or in response to a treat placed in his carrier. He was, however, friendly and allowed a physical examination. During a full orthopedic examination,1 he resisted extension of his pelvic limbs and right elbow. A taut muscle band (trigger point) was palpated over the left dorsal midlumbar area (Figure 2); palpation resulted in apparent pain (ie, a fast turn, stare, further tensing of lumbar muscles). The owner was asked to take videos at home (see Videos).
Diagnostics
Diagnostics included blood work (ie, CBC, serum chemistry profile, total T4); urinalysis; blood pressure measurement; and radiography of the elbows, pelvis, stifles, and spine (with patient sedated). In addition, the owner was asked to complete a Feline Musculoskeletal Pain Index (FMPI) questionnaire.
Feline Musculoskeletal Pain Index
The Feline Musculoskeletal Pain Index (FMPI; see Suggested Reading) questionnaire can be used to assess mobility impairment. The questionnaire consists of 17 questions, with a maximum score of 68. Higher scores indicate less mobility impairment.2
Results showed elevated BUN (43 mg/dL [15.4 mmol/L]; normal, 15-36 mg/dL [5.4-12.8 mmol/L]), serum creatinine (2 mg/dL [177 μmol/L]; normal, 0.6-1.9 mg/dL [53-168 μmol/L]), and urine protein:creatinine ratio (0.6; normal, <0.5); urine specific gravity was decreased (1.029; normal, 1.035-1.060). Systolic blood pressure (measured 4 times using the Doppler instrument before sedation) ranged from 150 to 160 mm Hg. FMPI score was 26 out of 68.
Diagnosis
Stage 2 chronic kidney disease (CKD)3
Sedation was needed to allow the team to manipulate the affected joints so that multiple radiographic views with the patient in different patient positions could be obtained. Adequate sedation was achieved with dexmedetomidine (3 μg/kg IM) and butorphanol (0.2 mg/kg IM), which also provided good muscle relaxation. Another orthopedic examination was performed while the patient was sedated; range of motion was normal in all joints.
Based on clinical and radiographic findings (Figures 3-6), degenerative joint disease (DJD) involving the hips and elbows bilaterally and the right stifle, with myofascial pain in the dorsolumbar area, was diagnosed.4

FIGURE 3
Lateral (A) and dorsoventral (B) views of the pelvis. Figure A shows a moderate amount of the smoothly marginated, bridging, bony proliferations surrounding the 2nd through 5th coccygeal vertebrae. A moderate amount of kyphosis is present on the tail, centered in the bony proliferation. A mild amount of irregularly marginated bony proliferation is present surrounding the facet joint of the C5-C6 intervertebral disk space. Figure B shows poor coverage of the right femoral head by the acetabulum. A moderate amount of irregularly marginated bony proliferation is present on the cranial and caudal aspects of the acetabulum and femoral neck. There is decreased soft tissue associated with the left pelvic limb as compared with the right. A small osteophyte on the left cranial acetabulum can be noted. Image courtesy of Dr. Karen Perry. Interpretation: Chronic, healed caudal vertebral fracture, C2-C4. Moderate, right coxofemoral osteoarthritis and mild left coxofemoral osteoarthritis
Treatment & Long-Term Management
CKD and DJD are common diseases affecting older cats. One study has reported that their co-occurrence may be as high as 68%.5 It is important to discuss with owners that neither is curable and that the focus of treatment is on patient comfort and quality of life.
The owner was encouraged to discontinue free feeding and feed Josh separately from the other cats. A commercially available renal diet was suggested; the food was to be gradually mixed with the current food over 2 weeks with accurate calculation of caloric requirements. Josh’s estimated ideal body weight was 12.8 lb (5.8 kg; see Suggested Reading for tools to help formulate caloric requirements).
Treatment at a Glance
Weight loss
NSAIDs
Diet change
Dietary supplements
Physical modalities
Meloxicam (0.02 mg/kg PO q24h, based on an estimated lean body weight of 6 kg) was administered. The efficacy of meloxicam in cats with DJD with and without stable CKD has been reported.6-10 Long-term oral meloxicam use is extra-label in the United States but is licensed for this purpose in other countries. Retrospective studies have shown no impact on progression of stable CKD nor on longevity in cats receiving meloxicam9,10; however, large, well-designed, prospective studies are needed. The safety (but not efficacy) of robenacoxib in cats with DJD and CKD has been reported.11 Cats that had CKD and a subgroup that had IRIS stage 2 and 3 CKD were included in this one-month prospective placebo-controlled trial; overall, there were no differences in reported adverse effects or changes in clinical chemistry and hematology results between the treatment and placebo groups, including the cats with CKD.
Gabapentin (12.5 mg/kg PO q12h) was administered. Gabapentin is used in humans with neuropathic pain and is widely used in dogs and cats to treat chronic pain despite the lack of large clinical studies. Some case reports support its use in cats with chronic musculoskeletal disease.12,13 Gabapentin is renally excreted. Some recommendations have been made for dosing and dose intervals based on serum creatinine.14 The effects in Josh may be unpredictable (eg, increased somnolence); therefore, the dose and dosing interval may require changes over time.
Additional Treatment
Education sheets on DJD and long-term use of NSAIDs in cats were provided to the owner,7 and various additional treatments were implemented to decrease the patient’s joint pain. Josh received dietary supplements containing glucosamine hydrochloride, avocado/soybean unsaponifiables, and Boswellia serrata extract, all of which may be beneficial to humans and animals with joint disease. The owner was shown how to palpate for trigger points and gently massage these areas using a soft rubber brush. Environmental modifications (eg, placing steps) were made to facilitate ascending and descending elevated locations (eg, window ledges).
The owner was encouraged to add a drinking fountain for the cats to increase water intake and raise the source of water from floor level to make it more accessible. Josh also engaged in therapeutic exercise (eg, walking to receive food [from the overall daily ration]).
Based on temperament, Josh was a suitable candidate for acupuncture, but the owner declined.
Follow-Up
Results from blood work repeated 2 weeks after starting meloxicam showed no significant changes. The FMPI score had improved to 53 out of 68. Body weight was unchanged.
Josh was not apparently sedate from the gabapentin, and no changes in dose or dosing interval were made. The owner stated that feeding Josh separately was unsuccessful; Josh would only eat a small amount when on his own and ate the other cats’ food when let out, which is a common issue in multicat households. The owner was willing to explore the use of microchip or RFID-activated pet feeders.
Follow-up was scheduled for 8 weeks later, at which time the patient showed improvement based on the FMPI score and owner feedback.
Prognosis & Outcome
Prognosis for this patient is good; weight loss is likely to be of great benefit. If the CKD is unstable or progresses, acupuncture should again be suggested, and other options may be available if NSAID therapy is discontinued (see Options for Future Therapy).
Options for Future Therapy
Grapiprant is a prostaglandin E2 (PGE2) EP4 receptor antagonist. It is currently available for use in dogs and may one day be available for cats.15 NV-02, a felinized antinerve growth factor monoclonal antibody treatment, is undergoing trials in cats.16
Key Takeaways
CKD and DJD frequently coexist in cats. Neither is curable, but treatment can be initiated to improve patient quality of life.
Many treatment options—both pharmacologic and nonpharmacologic—exist, and new options are likely forthcoming.
CKD = chronic kidney disease, DJD = degenerative joint disease, FMPI = Feline Musculoskeletal Pain Index