Noninvasive Blood Pressure Monitoring: A Review
Monitoring of systolic and diastolic blood pressure is an important part of overall patient assessment. Blood pressure measurement identifies hypertension and hypotension and is an important monitoring tool during anesthesia and in critical care.
Hypertension is a valuable clinical sign to detect disease, even at an early stage. While no data yet exist that define nonfatal endpoints as a result of hypertension (eg, retinal detachment), identification of hypertension through blood pressure measurement may assist the practitioner in assessing risk of target organ damage and limiting further progression of disease. In addition, detection of hypotension in animals with heart disease allows the practitioner to assess response to medications and adjust medication dosages.
Noninvasive blood pressure measurement is based on the Riva-Rocci method: A peripheral artery is occluded completely by an inflated cuff and then the cuff is gradually deflated. When the pressure in the cuff is low enough to allow blood flow, it is defined as the systolic blood pressure measurement.

Conventional oscillometric unit
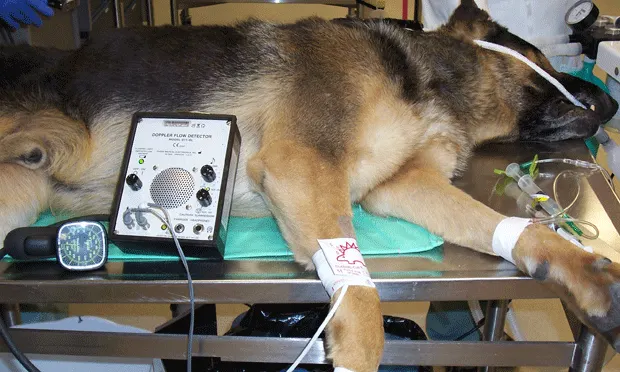
Doppler UltrasoundThe first noninvasive blood pressure measurement technology on the market was Doppler ultrasound. It is based on the Doppler shift effect—the change of frequency due to moving blood cells and movement of the arterial wall. The return of an audible pulse wave is supposed to equal systolic arterial pressure (SAP). Diastolic arterial pressure (DAP) generally cannot be determined reliably.
There are concerns regarding Doppler accuracy in detecting SAP. In cats under anesthesia, it has been shown that SAP determined via Doppler ultrasound correlated more closely with mean arterial pressure than SAP.1
Conventional OscillometryBoth conventional and high-definition oscillometry are based on arterial wall motion (oscillations). Initially oscillometry was rather inaccurate and not very sensitive, complicating its use in veterinary medicine. However, as it is microprocessor based, it improved as this technology improved over time.
Conventional oscillometry measures mean arterial pressure (MAP) and pulse rate, and calculates SAP and DAP. Most of these devices are relatively accurate within a range of 70 to 160 mm Hg (linearity range) but tend to underestimate higher and overestimate lower pressures. In low-pressure situations, these units may not provide a reading.
High-Definition OscillometryWith high-definition oscillometry (HDO), SAP, DAP, MAP, and pulse rate are measured, but other information beyond blood pressure is also gathered. Its 32-bit processor and PC software allow visible real-time measurements and analysis. In addition, features include:
-Assessment of initial blood pressure reading; then individual adjustment of all measurement parameters to maximize subsequent readings
-Gain function to increase sensitivity, allowing detection of weak pulses
-Pulse-dependent deflation rate (faster with higher heart rates) to cope with high and low heart rates.
In animals with high heart rates, such as cats or ferrets, readings can be obtained in as little as 8 seconds. Additionally, the real-time projection of oscillations (pulse wave analysis) allows the practitioner to determine if the rhythm is regular and may also provide information on cardiac output and arterial elasticity.
Accuracy has been proven in different animals against direct line/telemetry. Due to its entire linearity (not limited to 70–160 mm Hg) even the lowest pressure situations can be measured. Although the units can be used without a computer, it is highly recommended that one be used so the examiner can visualize the reading versus receiving only a numerical result.
Technology Learning CurvesHandling of the different devices has become easier as the technology has become more advanced.
The most experience and intensive training is needed for Doppler devices because blood pressure values obtained can be significantly influenced by the examiner. Cuff selection and placement, maximum inflation pressure, and deflation rate are determined by the operator. These factors all influence the accuracy of the readings obtained. However, its accuracy as a flow meter is less operator-dependent.
With conventional oscillometry, the examiner’s predominant task is to keep the animal calm for up to 2 minutes (depending on the unit). HDO is as easy to use as conventional oscillometry and due to the pulse-adapted deflation rate; the examiner only has to keep the animal calm for a short time. In addition, readings can be taken at the base of the tail of a standing or moving animal. Since every single heart beat can be visualized on a computer screen, artifacts can be noted while the reading is being taken.

Measuring Against the Gold Standard
There is some debate about validation of indirect blood pressure measurement devices in veterinary medicine. Many times these devices are compared to direct blood pressure measurement, but direct blood pressure management is not a gold standard either—the pressures determined vary depending upon technique and which artery is used.
In one study an indirect blood pressure monitor had better agreement with an arterial catheter in the dorsal pedal artery than with another direct arterial line in the lingual artery.2 Even though indirect blood pressure measurement devices may not have perfect agreement with a “gold standard,” they are the only practical way to measure blood pressure in clinical practice. There is no debate that hypertension can be seen in small animal practice and has very serious consequences.
Economic ImpactThe noninvasive blood pressure measurement units discussed in this article are available for less than $3000. Considering the many indications for measuring blood pressure, it is one of the most cost-effective units in a veterinary practice.

HDO reading with hypotension (119/59; hypotension compensated with a pulse rate of 144) and impaired arterial elasticity (high presystolic amplitudes) in a 4-year-old Schnauzer with hypothyroidism

HDO curve in a dysrhythmic 6-year-old bulldog with no clinical signs; overall blood pressure is in the normal range, but the disrhythmic situation leads to differences in diastolic filling and consequently in Frank–Starling-influenced contractility, leading to a fluctuating cardiac output situation (high and low amplitudes)
NONINVASIVE BLOOD PRESSURE MONITORING: A REVIEW • Beate Egner & Anthony Carr
References1. A comparison of indirect blood pressure monitoring techniques in the anesthetized cat. Caulkett NA, Cantwell SL, Houston DM. Vet Surg 27:370-377, 1998.
Accuracy of an oscillometric blood pressure monitor during phenylephrine-induced hypertension in dogs. McMurphy RM, Stoll MR, McCubrey R. AJVR 67:1541-1545, 2006.