Labored Breathing: Hairballs, Parasites, or Worse?
Luna, a 4-year-old spayed domestic long-haired cat, was presented for emergency examination with respiratory distress.
History
Luna primarily stayed indoors, was current on her vaccines, and tested negative for FeLV/FIV. Her owners reported a history of hairballs, for which she received daily over-the-counter remedy.
Her family was remodeling its home and put Luna in the unfinished basement for safety. Luna seemed fine the night before presentation; however, the following morning she was hiding, refusing to eat, and breathing hard.
Physical Examination
During examination, Luna was quiet but responsive with an increased respiratory rate of 72 breaths/min with nostril flaring and increased expiratory effort. Crackles (best auscultated by eliciting a cough through tracheal palpation) and wheezes were heard in all lung fields. Heart rate was 180 bpm with no murmurs or gallop rhythms. Her temperature was 101°F.
The rest of the examination was unremarkable.
Progression
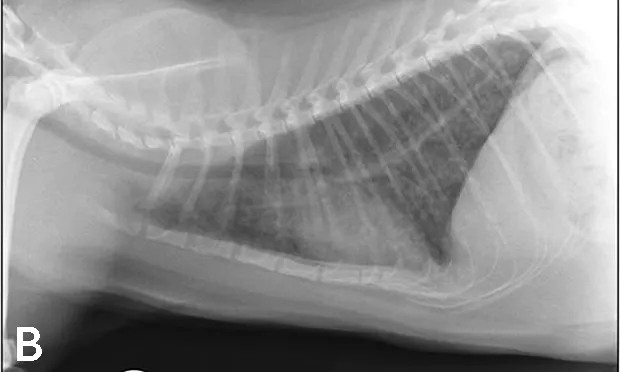
Luna was placed in an oxygen-enriched cage, and thoracic radiographs (Figure 1) were taken.

Figure 1. Thoracic radiographs taken at presentation.
Ask Yourself...What is your initial assessment and treatment plan for Luna? Assume she will continue to receive supplemental oxygen.
A. Luna has aspiration pneumonia from vomiting hairballs; antibiotic therapy should be provided.B. Luna has congestive heart failure; diuretic therapy is warranted.C. Luna has lower airway disease; bronchodilator (albuterol or terbutaline) and glucocorticoid therapies are warranted.D. It is unclear what Luna has developed; a keyhole lung biopsy is advised to determine the best course of action.
Correct Answer:C. Luna has lower airway disease; bronchodilator (albuterol or terbutaline) and glucocorticoid therapies are warranted.
Luna’s clinical signs and radiograph findings were most consistent with lower airway disease (ie, feline asthma). While asthma implies reversible bronchoconstriction, some cats with lower airway disease have more inflammatory changes and less reversible airway changes.
In Luna’s case, several clues suggested that her distress was from allergic airway disease. Often, owner complaints of hairballs are in reality a cough. When owners describe their cat as trying to cough up a hairball, it is prudent to establish that hairballs are produced. This clarifies whether coughing is confused with attempts to emit hairballs.
Luna’s signs worsened after exposure to a dusty environment, although airway disease had been present for some time.
During examination, crackles and wheezes are common in lower airway disease. Adventitial lung sounds, consistent with fluid in the alveoli and airway, are not specific for congestive heart failure (CHF). In addition, cats with CHF are usually hypothermic and, subsequently, relatively bradycardic. With Luna, respiratory effort was mostly expiratory, typical of airway disease but not always appreciated at examination.
Radiographic findings consistent with airway disease include donuts and tram lines, which are supportive of bronchial thickening and hyperinflation from expiratory flow limitation. Some cats with lower airway disease also have a collapsed middle lung lobe (Figure 2).

Figure 2. Cat with collapsed middle lung lobe (arrow) in addition to lower airway disease.
Luna was at an appropriate age for lower airway disease. Because lower airway disease is an allergic/inflammatory condition, most cats are identified at approximately 2 to 10 years of age. In very young or elderly cats, careful search for different underlying conditions is strongly advised.
Further Diagnostics
Parasite TestingLungworm and heartworm infections may cause similar signs. Lungworm infection, most common in young cats with exposure to outdoors and intermediate hosts, may cause clinical and radiographic signs

(Figure 3) similar to lower airway disease. Infection may be evaluated with a Baermann fecal sedimentation, or larva may be observed with airway cytology samples (Figure 4). Heartworm disease should be tested (via heartworm antigen and antibody test) in any cat with airway signs.
F__igure 3. Signs of lungworm infection that presented with signs similar to lower airway disease.
Figure 4. Lungworm larvae observed within airway cytology sample.
Airway CytologyAirway cytology from cats with asthma is typically eosinophilic, but it may be neutrophilic. When necessary, a blind bronchoalveolar lavage (BAL) may be performed and is useful for retrieving fluid to evaluate for evidence of airway inflammation and to exclude other causes of pulmonary disease (eg, infection, neoplasia). The decision to perform BAL analysis and testing is based on clinician assessment; this testing provides helpful information and should be considered.
ResultsLuna tested negative for heartworm and lungworm infection. Following stabilization, airway cytology was performed, evaluated, and documented 43% eosinophils, considered supportive of lower airway disease.
Follow-Up
Luna was diagnosed with lower airway disease and treated with terbutaline (0.01 mg/kg SC) and dexamethasone (0.5 mg/kg IV). She improved rapidly, which is the expected response, and was transitioned to prednisolone (1 mg/kg PO q12h for 14 days, then q24h indefinitely) and sent home with rescue albuterol therapy for administration during crisis. Routine use of b2-agonists should be avoided and given only when necessary. Glucocorticoid therapy is the mainstay for feline lower airway disease and may be administered either orally or via aerosol.
Many cats need long-term therapy to control clinical signs. Additional recommendations include limiting aeroallergens, avoiding dusty kitty litters, and avoiding smoking and heavy perfumes/cleaning products in the house.
BAL = bronchoalveolar lavage, CHF = congestive heart failure
Take-Home Messages
Coughing may be misinterpreted as hairballs.
Bronchointerstitial patterns are common radiographic abnormalities.
Parasitic diseases should be excluded.
Elderly cats with suspected airway disease should be aggressively evaluated for a different underlying cause, such as upper airway mass or pulmonary neoplasia.
Long-term glucocorticoids and improved environmental hygiene is advised for affected cats.
ELIZABETH ROZANSKI, DVM, DACVIM (Small Animal) & DACVECC, is associate professor of emergency and critical care medicine at Tufts University. Her area of interest is respiratory disease. She completed her internship at University of Minnesota and her residency in emergency and critical care at University of Pennsylvania. Dr. Rozanski earned her degree in veterinary medicine at University of Illinois.
Related articlesDiagnostic Challenges of Feline Heartworm DiseaseFeline Asthma and Bronchitis