Laboratory Evaluation in Dogs & Cats with Chronic Kidney Disease

You have asked…
What do I need to know about laboratory measurement and reporting when diagnosing and treating chronic kidney disease?
The expert says…
Chronic kidney disease (CKD) is a major cause of morbidity and mortality in dogs and cats. The prevalence of CKD has been estimated to be 0.5% to 1.0% in dogs and 1% to 3% in cats1,2 and increases with age, especially in cats. As many as 30% to 50% of cats 15 years of age or older have CKD.3-5
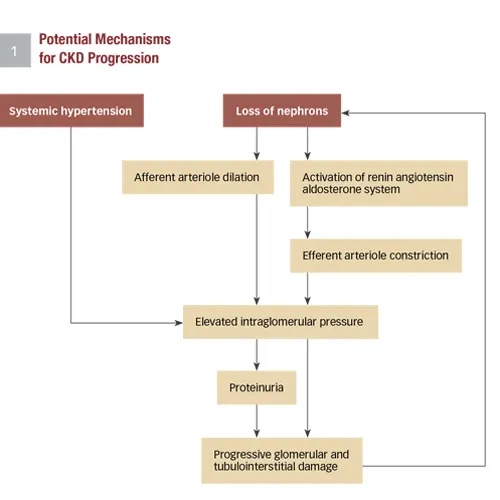
Nephron damage associated with CKD is usually irreversible and often progressive. Progressive loss of renal function in dogs tends to be common, linear, and relatively rapid compared with cats. Cats may have stable renal function for months to years and be relatively unaffected by CKD or may have slowly progressive disease over several years; stable cats may also experience an abrupt, unpredictable decline in renal function. Soft tissue mineralization, systemic hypertension, intraglomerular hypertension, and proteinuria have been associated with progression of CKD (Figure 1). Although it is not usually possible to improve renal function in CKD, it is logical to assume that early diagnosis can improve clinical outcomes. There is firm evidence for dietary treatment and increasing evidence that anti-proteinuric treatments can slow the progressive nature of CKD.
Early CKD Diagnosis
Serum Creatinine Concentration
Early nonazotemic CKD (International Renal Interest Society [IRIS] Stage 1) (Table 1A & 1B) can be diagnosed in dogs and cats with abnormal renal palpation or renal imaging findings, persistent renal proteinuria, or urine concentrating deficits. CKD is usually diagnosed based on persistent azotemia superimposed on an inability to form hypersthenuric urine. (Some cats with CKD retain the ability to concentrate urine.) Serum creatinine concentrations are used as a marker of glomerular filtration rate (GFR). Creatinine is produced from the nonenzymatic degradation of creatine and creatine phosphate in skeletal muscle; therefore, serum creatinine concentrations reflect muscle mass as well as GFR.
Serum symmetric dimethylarginine (SDMA) is derived from intranuclear methylation of L-arginine by protein-arginine methyltransferases and is released into the circulation after proteolysis. SDMA is eliminated primarily by renal clearance and represents a potential biomarker for diagnosing and monitoring CKD.10,11 In 2 recent longitudinal studies, SDMA concentrations increased above normal approximately 17 months prior to serum creatinine concentration increasing above reference range (serum creatinine concentration >1.8 mg/dL in a dog study and >2.1 mg/dL in a cat study).10,12 Interestingly, a serum creatinine concentration of >1.6 mg/dL occurred in the feline study, at nearly the same time the SDMA was increased above normal.10 Serum creatinine concentrations must be interpreted in light of the patient’s muscle mass, urine-specific gravity, and physical examination findings to rule out pre- and postrenal causes of azotemia. Dogs have large variations in muscle mass that will tend to increase the breadth of reference ranges.9 Despite these issues, longitudinal, consistent assessment of serum creatinine concentrations is an excellent tool to assess renal function and diagnose early CKD.Interpretation of serum creatinine concentrations can be influenced by analysis method (Jaffe’s reaction vs enzymatic; benchtop vs reference laboratory) as well as variations in reference intervals that can lead to false-positive or false-negative determinations of azotemia.6,7 Although reference ranges need to be individualized, many veterinary nephrologists suggest that renal azotemia begins with serum creatinine concentrations lower than most reference ranges (ie, 1.4 and 1.6 mg/dL in dogs and cats, respectively).<sup8 sup> The sensitivity of serum creatinine concentrations for the early diagnosis of azotemia or CKD is improved if a lower reference range is employed.
Related Article: Staging & Management of Feline Chronic Kidney Disease
Urine Protein/Creatinine Ratio (UP/C)
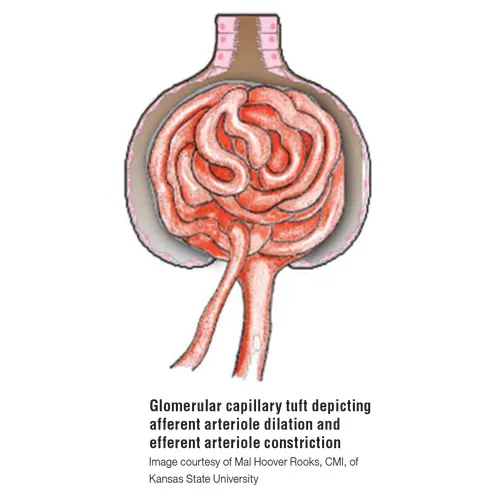
Proteinuria in dogs and cats with CKD can occur because of glomerular and/or tubular lesions. Glomerular proteinuria can be caused by loss of integrity of or damage to the capillary wall (eg, immune complex disease and X-linked hereditary nephropathy). It is also likely that increases in glomerular capillary pressure increase the amount of filtered plasma protein. Intraglomerular hypertension may result from loss of nephrons (afferent glomerular arteriole dilation and efferent arteriole constriction) and from systemic hypertension being transmitted into glomerular capillaries. Structural glomerular disease and CKD are often accompanied by systemic hypertension that can exacerbate intraglomerular hypertension and glomerular proteinuria. Tubular proteinuria occurs when reabsorption of protein from glomerular filtrate is compromised. Tubular proteinuria is typically of lesser magnitude than glomerular proteinuria. Reduced tubular reabsorption of protein can occur with tubulointerstitial injury and decreased numbers of functioning tubules. Whether caused by capillary wall lesions, tubular lesions, or intraglomerular hypertension, excessive protein in the glomerular filtrate may contribute to additional glomerular and tubulointerstitial lesions, and lead to loss of more nephrons. Proteinuric renal disease and systemic hypertension often coexist, and it can be difficult to separate effects of high systemic and intraglomerular pressures and proteinuria.
Diagnosing renal proteinuria in cats and dogs with CKD is a multistep process. Albumin is the major urine protein in dogs and cats, but specificity of dipstick screening for albuminuria is poor (especially in cats). Traditional dipstick-positive proteinuria should be confirmed with a more specific follow-up test (eg, sulfosalicylic acid turbidimetric test, UP/C [Table 2], or species specific albuminuria assays). The second step in assessment of proteinuria is to determine its origin (physiologic or benign proteinuria and pre- and postrenal proteinuria need to be ruled out). Renal proteinuria is persistent and associated with a benign or inactive urine sediment (hyaline casts may be observed in the urine sediment in cases of renal proteinuria). Persistent proteinuria is defined as at least 2 positive tests at 2-week intervals. Subsequently, via serial monitoring of the UP/C, it should be determined if the proteinuria is stable, increasing, or decreasing.
The current recommendation is to treat persistent proteinuria of renal origin with a renal diet (reduced dietary protein, phosphorus, and sodium, supplemented with N-3 fatty acids and alkalizing agents) and an angiotensin-converting enzyme (ACE) inhibitor. Borderline proteinuria warrants increased monitoring via the UP/C ratio. Note that borderline and even normal levels of proteinuria in cats have been associated with poor outcomes.
For example, in cats with naturally occurring CKD, relatively mild proteinuria (UP/C 0.2–0.4) increased the risk for death or euthanasia 2.9-fold compared with cats with UP/Cs <0.2.13 In a study of nonazotemic cats older than 9 years with CKD, 95 cats (median age 13) were followed for 12 months or until death or azotemia developed. Azotemia was defined as a serum creatinine concentration >2.0 mg/dL; 29/95 (30.5%) cats developed azotemia. Proteinuria at presentation (median UP/C of 0.19 vs 0.14) was significantly associated with development of azotemia in these geriatric cats.14 Finally, when 112 client-owned cats with stable CKD were compared with 101 client-owned cats with progressive CKD, median UP/Cs in the progressive group were higher than the stable group (0.27 vs 0.14).15 A 0.1 increase in UP/C was associated with a 24% increase in risk of CKD progression.15 It should be noted that overlap of UP/C values was present in these studies, and therefore clinical relevance in individual cats may be difficult to determine. Nonetheless, proteinuria is an important risk factor for the development of azotemia in cats and the progression of CKD in dogs and cats and should be monitored closely.
Related Article: Feline Chronic Renal Failure
Management of CKD
Systolic Blood Pressure
IRIS blood pressure substaging for dogs and cats with CKD is based on risk of target organ (ocular, neurologic, cardiac, and renal) damage (Table 3). Not long ago, indirect systolic blood pressure measurements >170–180 mm Hg were considered the threshold for hypertension. Despite inherent difficulties with indirect blood pressure measurement in dogs and cats, it may be appropriate to consider systolic hypertension to be present at lower pressures (>160 mm Hg).
In a recent study, 45 dogs with naturally occurring CKD were divided into 3 groups based on initial systolic blood pressure and were followed for up to 2 years. The groups were defined as: high (161–201 mm Hg), n = 14; intermediate (144–160 mm Hg), n = 15; and low (107–143 mm Hg), n = 16. The initial high-systolic blood pressure group had increased risk of uremic crisis and death compared with the low-pressure group (median survival <200 days vs >400 days, respectively).17 In cats with a remnant kidney-wrap model of CKD, systolic hypertension (mean pressure of 168 mm Hg) was associated with reduced GFR (1.34 vs 3.55 mL/min/kg), increased UP/C (1.2 vs 0.1), and increased glomerulosclerosis.18 Similarly, in dogs with the remnant kidney-wrap model of CKD, systolic hypertension (>160 mm Hg) was associated with reduced GFR, increased UP/Cs, and increased mesangial matrix accumulation, tubular lesions, fibrosis, and cellular infiltrates.19 Cats with progressive CKD had higher systolic blood pressures than did cats with stable CKD (155 mm Hg vs 147 mm Hg).15 Finally, in 69 cats with naturally occurring CKD, high time-averaged systolic blood pressure (159 mm Hg vs 136 mm Hg) was correlated with glomerulosclerosis and hyperplastic arteriolosclerosis.20
Serum Phosphorus Concentrations
Similar to serum creatinine reference ranges, serum phosphorus reference ranges vary among laboratories. This variability is caused in part by higher serum phosphorus concentrations observed in healthy, growing puppies and kittens. Soft tissue mineralization of the kidney causes irreversible nephron damage and is associated with CKD progression in dogs and cats. Cats with stable CKD had lower serum phosphorus concentrations than did those cats with progressive CKD (4.4 vs 5.1 mg/dL).15 Serum phosphorus concentration is a predictor of CKD progression in cats, with a 41% increase in the risk of progression for every 1.0 mg/dL increase in serum phosphorus concentration.15 In 80 client-owned cats with CKD, serum phosphorus concentrations correlated with renal interstitial fibrosis.20 In dogs with CKD, a serum calcium times phosphorus product >70 mg/dL was a poor prognostic indicator.21 These findings have prompted closer scrutiny of therapeutic targets for serum phosphorus in dogs and cats with CKD8 (Table 4).
Summary
Closer monitoring of serum creatinine and UP/C may facilitate early diagnosis of CKD in dogs and cats. Longitudinal assessment of these parameters provides better data than one-time evaluations. No laboratory test is perfect; trending laboratory data using the same test methodology tends to improve diagnostic sensitivity. Once CKD has been diagnosed, standard of care renoprotective treatment includes a renal diet, potentially in combination with one or more enteric phosphate binders for hyperphosphatemia, ACE inhibitors, or calcium channel blockers for proteinuria and hypertension. Tighter control of hyperphosphatemia, renal proteinuria, and systolic hypertension may improve treatment outcome.
ACE = angiotensin-converting enzyme, CKD = chronic kidney disease, GFR = glomerular filtration rate, IRIS = International Renal Interest Society, UP/C = Urine protein/creatinine ratio
GREGORY F. GRAUER, DVM, MS, DACVIM, is professor and Jarvis chair of medicine in the clinical sciences department at Kansas State University. His area of interest, research, and teaching is the small animal urinary system, a topic he lectures about at the NAVC Conference. He has served as professor and section chief of small animal medicine at Colorado State University and faculty member at University of Wisconsin–Madison, where he completed his internship and residency and earned his master’s. Dr. Grauer is a graduate of Iowa State University.
*Dr. Grauer has research projects funded by IDEXX and has been paid by IDEXX to attend meetings as a key opinion leader in his field.