Jaw Fractures in Dogs & Cats: Diagnostic Methods, Treatments
Jonathan Miller, DVM, MS, DACVS (Small Animal), Eclipse Specialty & Emergency Pet Care, Whippany, New Jersey
Pharyngostomy tube placement in a dog
Orthopedic referral is not always feasible or even necessary. There are many opportunities to practice your orthopedic skills in general practice. Explore our Fractures clinical portal to learn more about managing fractures in dogs and cats.
Background & Pathophysiology
Facial trauma from motor vehicles, bites, or falls can result in maxillary and/or mandibular fractures. These fractures represent 2% of all fractures in dogs and 15% of those in cats.1,2 In older patients, bone resorption can lead to self-induced or iatrogenic fractures with minimal trauma during dental procedures.
History & Clinical Signs
Patients with jaw fractures have typically experienced recent motor vehicular trauma, animal bites, blunt force trauma, or falls (including high-rise syndrome). Some fractures may not be evident to the pet owner until food prehension difficulties arise. Many fractures are discovered based on the patient’s inability to close the mouth, visible malocclusion, pytalism, and/or bleeding from the mouth.
Diagnosis
A thorough oral examination with the patient under general anesthesia is the most straightforward diagnostic technique. Palpation of the symphysis, horizontal body of the mandible, vertical ramus, temporomandibular joint, maxillary arcade, and hard palate is the first step to determine further diagnostics. Whereas open fractures can usually be observed, more caudally located fractures can be difficult to observe; presence of blood in the mouth should raise suspicion. Symphyseal separation is typically straightforward to palpate; however, the clinician should always look for a second fracture using general or dental radiography. Standard orthogonal views may be supplemented with oblique views to reduce confusion due to superimposition of teeth and bones. The maxilla can be assessed with these methods but is often best evaluated with CT if multiple fracture areas are suspected. Radiography can be used to evaluate fracture orientation, fracture number, tooth viability, bone quality, osteomyelitis, and tumor formation.
Other body systems should be assessed for damage secondary to any primary trauma. Common injuries include brain trauma, cranial nerve damage, and pneumothorax; thus, a thorough physical examination and cardiopulmonary stabilization should be performed prior to treatment for facial fractures.
Want to hear more?
We sat down with Dr. Miller to further discuss jaw fractures. Listen to his episode of Clinician's Brief: The Podcast here.
Treatment
General anesthesia is required for fracture treatment, and local anesthetic blocks are advantageous. IV antibiotics should be administered in patients that have open fractures. Intubation with a short endotracheal tube and pharyngostomy are useful for evaluating occlusion during fracture surgery; in the former, the connection between the tube and anesthesia hose is located in the mouth, allowing for brief, intermittent disconnection with closure of the mouth to assess interdigitation of the maxillary and mandibular teeth. A pharyngostomy tube can be placed caudal to the mandible through a separate skin and pharyngeal incision (Figure 1) or through an incision ventrolateral to the tongue.3

Pharyngostomy tube placement in a dog
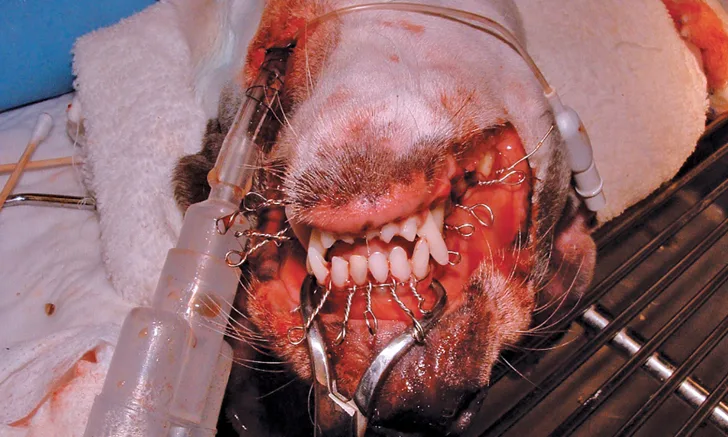
Symphyseal separation can be repaired by passing 22- to 18-gauge wire through a hole in the ventral midline skin to encircle the base of the mandibular canine teeth (Figure 2). The wire should be tightened to ensure stability of the symphysis while occlusion is observed to maintain proper spacing between the mandibular and maxillary canine teeth. The cerclage wire should be cut with sufficient wire protruding to enable removal after 6 to 8 weeks. The metal twist may be covered by a dollop of bone cement, acrylic, or a pencil eraser to prevent self-trauma.

Lateral radiograph showing placement of a mandibular symphyseal wire in a dog
When managing fractures of the mandibular body, the surgeon’s goal is to provide stability to achieve bone union, whereas the dentist’s goal is to maintain tooth viability and proper occlusion. For example, a surgeon may want to place cerclage wires near the tooth root in the ventral mandible to secure good-quality bone at the tension surface, whereas a dentist might prefer an intraoral technique to preserve the root and relinquish a biomechanically superior location for implant placement. With proper planning, these goals can be balanced with a variety of methods. Interfragmentary wiring can be performed by placing 24- to 18-gauge wire throughout the length of the mandibular body; typically, >1 wire should be placed perpendicular to the fracture line for stability (Figure 3). Simple straight-line fracture configurations are best for this technique. In cases involving comminution of the mandible, plates or external fixators can be useful (Figures 4 and 5). These are typically placed on the lateral aspect of the mandible with careful avoidance of the tooth roots.
When fracture lines between intact teeth are observed, interdental wiring with 26- to 20-gauge wire at the gingival line of each tooth can be useful as a supplement to other techniques. Acrylic is commonly added over the teeth–wire construct. The teeth should first be scaled, polished, and acid etched, then acrylic should be applied over the teeth–wire construct while ensuring occlusion (Figure 6).4,5 Bone healing may be prolonged if tooth extraction or root canal is required.4 The acrylic and wires can be removed once bone healing is evident, typically 6 to 8 weeks after injury.

FIGURE 3A
Lateral radiographs of a caudal mandibular body fracture (A) and placement of 2 interfragmentary wires (B) in a dog
In cats and small dogs with caudal body or ventral ramus fractures, bonding of the 4 canine teeth is a viable treatment option. Bonding prevents the entire mandible from moving so that a fracture in any location will heal. It is most often used with caudally located fractures for which there are fewer repair options. However, the application often gets overpowered and fails in medium and large dogs, for which other methods are needed. The canines should be scaled, polished, and acid etched, then acrylic should be applied while the mouth is open in a manner that would enable intake of gruel. The acrylic should be removed in 6 to 8 weeks. In older dogs with small rostral mandibular fractures, partial mandibulectomy is an excellent treatment strategy with no potential for nonunion or bone infection.
When financial considerations preclude the fracture assessment and treatment plan, a tape muzzle can be used. The face should be cleaned and dried and any open fractures sutured closed. Tape should then be applied in a circular pattern over the muzzle to allow an oral opening sufficient for intake of gruel. Another piece of tape should be placed under the ears and around the back of the head and secured to the muzzle tape (Figure 7). An Elizabethan collar should be used to prevent the patient from removing the muzzle. Pet owners should be advised to clean the tape muzzle, although it can be easily replaced if necessary. A sufficiently large nylon muzzle may alternatively be used.

Dog with tape muzzle in place
Prognosis & Clinical Follow-Up
Postoperative treatment includes pain management (eg, fentanyl or hydromorphone immediately, followed by an oral NSAID with tramadol or gabapentin) and 1 to 2 weeks of antibiotic treatment (eg, amoxicillin/clavulanic acid, clindamycin) for open fractures. In addition, the patient should be provided soft food for 2 to 4 weeks, during which time toys and hard treats should be withheld. Follow-up radiography should be performed 6 to 8 weeks posttreatment to assess fracture healing. Jaw fracture treatment has a complication rate of 34% to 60%.1,2 Malocclusion and infection are the most common complications; implant failure, malunion, and nonunion may also occur. Nonunion can be treated with further stabilization surgery and bone grafting.
Editor's note: This article was originally published in May 2020 as "Jaw Fractures."