Isoflurane & Sevoflurane: Mechanics & Effects
Patrick M. Burns, BVSc, MANZCVS, DACVAA, University of Montreal
Part 1 of this 2-part series on inhalant anesthesia offers a review of the pharmacologic effects and mechanisms of these agents. Part 2 will describe application and follow-up protocols.
Profile
Mode of Action1-3
The exact mechanism of inhalant anesthetic agents is still unknown.
There is potentiation of the GABAA and glycine receptors, as well as inhibition of the acetylcholine and glutamate receptors.
Inhalant anesthetics bind to the amphiphilic cavities in the proteins of cell membranes, causing conformational changes to receptors and transmembrane proteins.
There is a lack of synaptic transmission; this neuronal transmission interruption causes anesthesia.
Major Pharmacodynamic Effects
Central Nervous System
The principal effects of inhalant anesthetics result in a state of general anesthesia with hypnosis, unconsciousness, amnesia (in humans), muscle relaxation, and immobility.
Immobility is caused principally at the level of the spinal cord.
Isoflurane and sevoflurane have been demonstrated to be neuroprotective.3
Sevoflurane can better preserve the autoregulation mechanisms for brain vasculature; it is preferred over isoflurane for patients with neurologic disease.4
Cardiovascular System
All inhalant anesthetic agents produce an agent- and dose-dependent reduction in myocardial contractility, systemic vascular resistance, and cardiac preload with subsequent reductions in mean arterial pressure (MAP) and cardiac output in a dose-dependent manner.
The most prominent effect at clinically pertinent minimum alveolar concentration (MAC) values is vasodilation caused directly by effects on vascular smooth muscle and indirectly by a reduction in sympathetic tone.5
This is dose dependent and may result in hypotension.
At higher levels of anesthesia, negative inotropic effects are produced by changes in calcium availability and subsequent interaction with the actin-myosin cross-bridging.
Sevoflurane has less of an effect on the autoregulation of the microcirculation of the brain and heart when compared with isoflurane.4
Respiratory System
The dose-dependent depression of respiratory function is similar in both inhalant anesthetics.
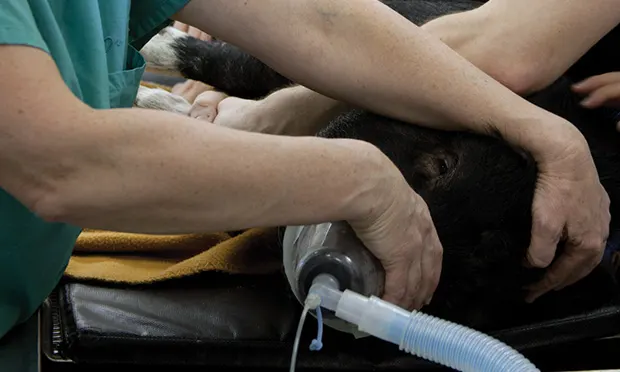
Sevoflurane causes less bronchospasm than isoflurane, making it ideal for chamber or mask induction (Figure 1).6

Mask induction of a potbellied pig. Sevoflurane is the inhalant anesthetic of choice when using an anesthetic chamber or mask. After anesthesia is stable, a change over to isoflurane to reduce the costs of anesthesia may be preferable.
Renal System
Sevoflurane can be degraded by soda lime to compound A, which is nephrotoxic.7
To minimize the risk for forming compound A, the newer calcium hydroxide-based CO2 absorbents may be used; however, they have a lower absorbent capacity and are more costly.7
Low-flow anesthesia (ie, a low oxygen flow rate of less than 500 mL/min) should be avoided.1,6
Pharmacologic Profile
Isoflurane and sevoflurane are pharmacodynamically similar.
Sevoflurane may be preferable in patients with certain heart or brain conditions.
Sevoflurane has a lower blood–gas coefficient, which translates to a clinically faster response time to changes in concentration.
Major factors that influence anesthetic uptake are anesthetic delivery to the lungs, blood–gas solubility, cardiac output, alveolar-to-venous anesthetic partial pressure difference, and tissue type.
Minimum Alveolar Concentration
The MAC of an anesthetic agent necessary to prevent movement in response to a supramaximal noxious stimulus in 50% of patients exposed.8,9
It is used to help determine the percentage of anesthetic agent to use.
For most species, the MAC of isoflurane and sevoflurane is about 1.3% and 2.3%, respectively.6
There is an inverse relationship between potency and MAC and between MAC and the blood–gas coefficient.
Factors that can cause an increase in MAC requirements: anxiety, hyperthermia, thyrotoxicosis, and central nervous system stimulants
Factors that can cause a decrease in MAC requirements: hypothyroidism, hypothermia, hypotension, sedatives, analgesics, and pregnancy
Biotransformation of Anesthetics
0.2% of isoflurane is metabolized.1,7
<3% of sevoflurane is metabolized.1
Inspired & Alveolar Anesthetic Concentrations
The fraction alveolar concentration (FA) equilibration with the fraction inspired concentration (FI) signifies a steady state between the breathing circuit and the patient.
The end-tidal agent concentration (ETA) is used as a surrogate measure of the anesthetic concentration of the brain, which is the true measure of anesthetic depth.
Effect of Changes to the Ventilation
The principal driving force that influences the anesthetic concentration in the brain is the FA.
A stable FA implies that a steady state has been achieved between the alveolar space and all other compartments of the body (eg, blood, brain, muscles, fat).
A FA:FI approaching 1 indicates a steady state with the other tissue compartments.
How quickly the FA:FI ratio achieves a steady state is dependent on the ventilation of the patient and the uptake of the anesthetic agent.
Increasing the ventilation of the patient when using a more soluble anesthetic such as isoflurane has a greater effect on the rate of increase in the FA:FI when compared with sevoflurane.
The uptake (the proportion of isoflurane absorbed by the pulmonary blood flow) of isoflurane is greater.
With isoflurane, if ventilation is doubled, uptake can be doubled, assuming cardiac output remains the same.
As sevoflurane is relatively insoluble it will quickly achieve an equilibrium between all the tissue compartments. Changes to the alveolar ventilation have less of an effect on the FA:FI ratio as compared to isoflurane.
Factors Influencing Anesthetic Uptake
Solubility
The relative solubility of an anesthetic agent between two different phases at a steady state is described by the partition coefficient.
The blood–gas partition coefficient λ describes the interaction between the blood and the alveolar gas.
Isoflurane (λ = 1.4) has a higher blood–gas partition coefficient than sevoflurane (λ = 0.65).
At a steady state (ie, when the partial pressure is the same in each phase), more isoflurane is contained in the blood than the alveolar gas by a factor of 1.4.
The uptake of isoflurane is thus greater than sevoflurane.
The time required for isoflurane to obtain a steady FA:FI ratio will be longer, which translates to a longer induction time for isoflurane, assuming normal ventilation–perfusion equilibrium.
Cardiac Output
The higher the cardiac output, the higher the rate of uptake.
This is a result of more blood being in contact with the alveolar space with each minute.
This effect lowers the FA:FI ratio.
The corollary of this is the increased blood flow to other tissue compartments other than the brain, which also slows the rate of accumulation of the anesthetic agent in the brain.
Alveolar-to-Venous Partial Pressure Anesthetic Gradient
As blood flows through the various tissue compartments, the tissue absorbs the anesthetic agent as a function of relative solubility.
The greater the tissue absorption, the lower the venous partial pressure of the anesthetic agent.
This results in a larger alveolar-to-venous gradient, which slows the rate of increase in the FA:FI ratio.
The high solubility in the other tissue compartments, especially fat, slows the rate of recovery because of the release of the anesthetic agents from these tissues back into the blood.
The principal difference between isoflurane and sevoflurane is the blood–gas partition coefficient (Table).
Tissue Groups
The vessel-rich group (ie, brain, heart, splanchnic organs) has a relatively low mass (10% of body mass) but receives a high percentage of the cardiac output (75%).1,2,4
These organs will receive more anesthetic faster as compared to other organs where the blood flow is lower and the tissue mass is greater.
After approximately 2 minutes, sevoflurane attains its equilibrium between the brain and blood (assuming normal ventilation and cardiac output in mammals).
Isoflurane takes 4–8 minutes to equilibrate.
Percentage of Anesthetic Agent Used
Increasing the percentage of the anesthetic agent at the start of anesthesia also increases the FI of the anesthetic agent.
Doubling the percentage of anesthetic used does not result in doubling the rate of increase in the FA:FI ratio because of the anesthesia-induced respiratory depression.
Rebreathing Circuits
The gas inspired by a patient when using a rebreathing circuit is a mixture of fresh and exhaled gas, which is recycled and mixed again with fresh gas flow.
Uptake of anesthetic into the bloodstream slows the increase in the FA:FI ratio as it prolongs the time to equilibrate for FA.
By using a fresh gas flow greater than the respiratory minute ventilation, the inspired gas will always be the same as the output of the vaporizer; however, this is wasteful and environmentally deleterious.
Higher flow rates also dry out the airways, so lower fresh gas flows are used.
Two confounding problems slow the rate of increase of the anesthetic concentration in the circuit.
The lower fresh gas flow slows the rate of change in anesthetic concentration within the circuit.
The binding of volatile anesthetics onto the surface of the tubing of the circuit, CO2 absorber, and uptake of anesthetic by the patient slows the rate of increase of the circuit anesthetic concentration.
In General
When comparing isoflurane and sevoflurane using their pharmacokinetic profiles, the major difference is the blood–gas solubility coefficient.
Changes in anesthetic concentration are more rapid with sevoflurane, but the MAC is higher when compared with isoflurane.
Currently, sevoflurane is more expensive to use, because a higher fresh gas flow is recommended to prevent the formation of compound A when using a rebreathing circuit.
Sevoflurane is the agent of choice for chamber and mask inductions and when a faster recovery is required.
Sevoflurane may also have advantages over isoflurane in anesthesia for patients with brain disease.

In anesthesia of cold-blooded species, sevoflurane may be preferable to isoflurane because of the shorter recovery period (Figure 2).
Figure 2. In anesthesia of cold-blooded species, sevoflurane may be preferable to isoflurane because of the shorter recovery period.
FA = fraction alveolar concentration, FI = fraction inspired concentration, ETA = end-tidal agent concentration, GABAA = class A γ-aminobutyric acid, MAC = minimum alveolar concentration, MAP = mean arterial pressure