Intervertebral Disc Disease at a Glance
Loretta J. Bubenik, DVM, MS, Diplomate ACVS, Louisiana State University
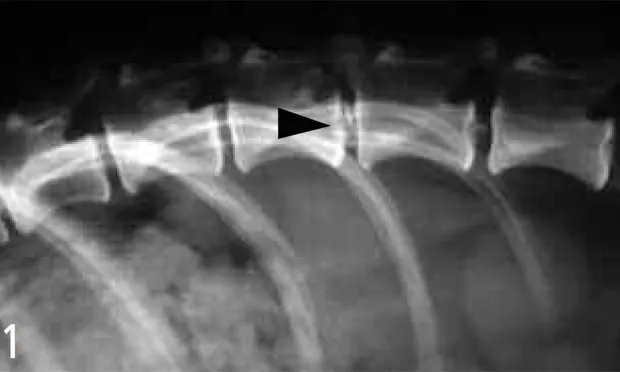
Note the mineralized disc at T13-L1. The disc may or may not be causing the clinical signs the dog had been experiencing. Further imaging would be needed to evaluate for spinal cord compression; however, the presence of the mineralized disc indicated disc degeneration, which predisposes to herniation.7
Profile
Definition
Systems. Intervertebral disc disease is a degenerative process of the intervertebral disc that causes loss of normal disc architecture and function, resulting in disc bulging or herniation into the spinal canal.1,2
Genetic Implications. Commonly affects chondrodystrophic breeds, especially dachshunds, through multifactorial inheritance.3
Incidence/Prevalence. Approximately 2% of the canine population is affected; with 73% of cases occurring in chondrodystrophic breeds.4,5 Dachshunds have the highest prevalence (25% vs < 10% for others).4
Signalment
Species. Most commonly affects dogs, but can occur in cats.
Breed Predilection. Breeds affected in addition to dachshunds include beagles, cocker spaniels, Shih Tzus, Pekingese, Lhasa apsos, Welsh corgis, and poodles.4
Age and Range. Most common in animals 2 to 7 years of age; peak incidence at 5 years,6 but can affect animals of any age.
Gender. No predilection.
Causes
Disc degeneration is the main cause of the disease, but traumatic disc herniation also occurs.2
Risk Factors
Breed and the presence of calcified disc.7-9 The relationship between obesity and disc disease has not been proven.7-9
Pathophysiology
Intervertebral discs function as shock absorbers and stabilizers of the spine. They consist of the outer annulus fibrosus, which encases the softer nucleus pulposus.
In chondrodystrophic breeds, the disc undergoes degeneration over time (chondroid metaplasia), but many changes are present early in life.2 Such changes are characterized by loss of water and proteoglycans and alterations in glycosaminoglycan content, resulting in a harder, more cartilaginous nucleous pulposus and a weakened annular ligament.10 As degeneration progresses, normal function is lost and sudden extrusion of disc matter can occur (Hansen type I lesions).
In nonchondrodystrophic breeds, degeneration usually occurs later in life and involves fibrous metaplasia of the disc instead of the cartilaginous changes noted for chondrodystrophic breeds.2 Nonchondrodystrophic disc disease is usually characterized by disc bulging (Hansen type II lesions) rather than extrusion.
Signs
Severity and type of signs depend on the rate of disc extrusion/protrusion, volume of compressive mass/cord compression, and lesion location. The faster the disc matter extrudes and the more compressed the spinal cord, the more severe the clinical signs.
Cervical region: Signs are most commonly attributed to pain (stiff forelimb gait, lowered head, guarded neck, cervical and shoulder muscle spasms). Nerve root irritation is common and can cause lameness of one or both limbs (root signature). Paresis or paralysis is less common but does occur.
Thoracolumbar: Varying degrees of spinal pain, back arching, ataxia, nonambulatory paresis, and paralysis occur with thoracolumbar (T-L) lesions.
Nonspecific clinical signs of disc herniation include exercise intolerance, diminished appetite, vocalization, and gait alteration. Urinary dysfunction may be present.
Grades based on neurologic status:
Grade I: Spinal pain with no neurologic deficits.
Grade II: Mild to moderate ambulatory paresis with conscious proprioceptive deficits.
Grade III: Nonambulatory paresis +/- urine retention.
Grade IV: Paralysis with urine retention. This grade can further be divided into IVa-sensory function still intact; and IVb-complete sensory and motor paralysis.
History
Variable and may be nonspecific. May have a history of spinal pain or ataxia. Recent history might include sudden onset of ataxia, paresis, paralysis, spinal pain, and/or vocalization after jumping/running. An obvious inciting incident may not be present. Decreased appetite, lethargy, exercise intolerance, lack of social interaction, or reluctance to participate in usual activities might be noted.
Physical Examination
General examination is often normal, although other problems might be found.
Neurologic examination should include cranial nerve and mentation evaluation, myotactic reflexes of all four limbs, gait and strength assessment, panniculus, conscious proprioception, withdrawal reflexes, crossed extensor reflexes, spinal palpation, and sensory evaluation when paralysis is present.
Cervical disc herniation is often only associated with cervical pain, although neurologic deficits do occur. Deficits might include gradations of conscious proprioception deficits, tetraparesis, tetraparalysis, root signature, and/or respiratory compromise. Forelimb reflex character may be upper or lower motor neuron or normal depending on lesion location. Hindlimb reflex character will be lower motor neuron or normal.
Thoracolumbar disc herniation is more likely to cause neurologic deficits. Forelimb reflexes and function should be normal. Hindlimbs can exhibit varying degrees of conscious proprioception deficits; paresis; paralysis; and in rare cases, root signature. Reflex character to the hindlimbs is usually upper motor neuron, because herniation near the T-L junction is most common; but the character of reflexes can be lower motor neuron for more caudal spinal lesions or they may be normal.
Animals with little if any limb function are unlikely to have conscious control of urination. Inappropriate urination or inability to urinate signifies a problem. Bladder reflex changes are usually upper motor neuron in character, but can be lower depending on the location of the spinal lesion.
Pain Index
The degree of pain associated with disc herniation can range from absent to severe; it is the predominant clinical sign for cervical disc herniation. Potential sources of pain include radiculitis, meningeal irritation, and the intervertebral disc. Signs include reluctance to move, arched back, stiff neck, holding up a limb, muscle spasms, and vocalization.
Diagnosis
Definitive Dx
Diagnosis is supported by signalment, history, and examination. Appropriate hematologic, serum chemistry, urine, CSF, and imaging studies should be done to assess health and rule out other diseases. Blood analysis can show evidence of recent steroid administration, dehydration, or stress, but is often normal. CSF evaluation is often normal but can show elevated protein without pleocytosis or changes consistent with spinal trauma. Radiographic signs consistent with disc herniation include narrowing/ wedging of the disc space, collapse of articular facets, narrowing of the intervertebral foramen, and/or mineralized matter within the vertebral canal. Disc mineralization is common; it supports disc degeneration but not necessarily herniation (Figure 1). Myelography, computed tomography, or magnetic resonance imaging is necessary to localize the lesion or aid in diagnosis of problems other than disc disease.
Differential Dx
Diskospondylitis, meningitis, myelitis, spinal fracture/luxation, cervical vertebral instability, atlantoaxial subluxation, hemivertebra, neoplasia, cysts, cauda equina disease, fibrocartilaginous emboli, intracranial disease, degenerative myelopathy, severe osteoarthritis, and bilateral cranial cruciate rupture.
Postmortem Findings
Disc matter in the spinal canal +/- spinal cord swelling/compression at the site of herniation. Varying degrees of spinal cord degeneration.
Treatment
Treatment is based on grade of neurologic dysfunction. Surgery or conservative management is used to treat the disease.
Grade I: Conservative management with pain medication is appropriate. Most animals in this condition will respond to cage rest. Consider surgery if pain does not resolve or worsens.
Grade II: Conservative management is appropriate. Consider surgery if worsening is noted.High-grade II: If the animal is weakly ambulatory, consider conservative management, but monitor the animal serially for worsening. Evaluation by a specialist would be beneficial since surgery may be the best option. If the animal improves over the first 24 to 48 hours, then conservative management can be continued. If the animal does not improve or worsens, surgery is recommended.
Grade III to Grade IVa: Surgery is recommended.
Grade IVb: If spinal decompression is achieved within the first 24 to 48 hours of sensory loss, recovery might be improved. Because it is difficult to know when sensation was lost, surgery is often done at the time of presentation to offer the best chance of recovery, even though the prognosis is questionable.

Dogs that have permanent loss of limb function can have a good quality life in a cart if care can be maintained by the owner. The dog adjusts easily to using the cart and can get around very well.
Conservative Management
Strict confinement for 4 to 6 weeks; thereby allowing sufficient time for the disrupted annular ligament to seal and decrease the chance of further herniation at the problem site. Keep the patient in a crate big enough only to turn around, eat, and drink. Use a harness rather than a collar to walk dogs with cervical disease. Keep nonambulatory animals in a well-padded, clean area to help prevent decubital ulcers and urine scald, and bathe as needed. Loss of conscious urination will require manual bladder emptying to maintain adequate bladder decompression. The number of bladder expressions per day is dependent on the amount of urine produced by the dog-three to four times a day is a good start. Urine dribbling between manual expressions can indicate inadequate bladder management and number of expressions per day should be increased; failure to maintain adequate bladder decompression can result in permanent bladder atony. Range-of-motion exercises help maintain muscle and joint health, and standing/balancing exercises encourage limb use and build strength. Nonambulatory animals should not be allowed to drag themselves around. A cart is a good option for animals with permanent loss of mobility as long as the owner can provide appropriate care (Figure 2).
Client Education
Owners should be warned against allowing prematurely increased activity. They should also be made aware that the disease can recur at the same site or at another site. Client education about the disease should begin before recurrence.

A spinal cord exposed through hemilaminectomy. Note the extent of central compression of the spinal cord over the disc space. The purpose of this surgery is to decompress the spinal cord by removing the disc material causing the compression. Surgical decompression allows a normal blood supply to return to the compressed area and neurologic recovery to begin.
Surgery
Animals with severe neurologic deficits, that do not respond to or worsen with conservative management, or that have recurrent episodes should be considered surgical candidates. The surgical approach depends on the site of disc herniation, but the goal is to decompress the spinal cord. Ventral slot is the method of choice for cervical disc herniation while hemilaminectomy is preferred for T-L herniations (Figure 3). All animals undergoing surgical decompression should be cage-rested for 4 weeks to allow healing.
Medications
Drugs/fluids: For radiculitis associatedwith cervical disc disease, prednisolone at a tapering dose of 0.2 to 1 mg/kg over 5 to 7 days can be useful. For muscle spasms, methocarbamol (15 to 20 mg/kg PO Q 8 H) or diazepam (1.1 mg/kg PO Q 8 H) can be used. NSAIDs or opioids can be used for pain control according to the labeled directions; NSAIDs should not be combined with steroids.
Contraindications: Dexamethasone should not be used to treat disc disease and has been linked to severe gastrointestinal bleeding and colonic perforation in cases of spinal cord injury.11 Long-term steroid administration is not recommended.
Alternative therapy: Acupuncture may be a reasonable alternative for managing the pain associated with chronic intervertebral disc disease.
Follow-Up
Patient Monitoring
Animals should be monitored for recurrence and/or worsening of clinical signs. Animals with sensory loss should be monitored for self-mutilation.
Prevention
Limiting running and jumping has been suggested to prevent occurrence, but the value of this has not been proven. Disc fenestration has not been proven to prevent future disc herniation and is not routinely offered unless combined with spinal cord decompression. Laser or chemical disc ablation has been tried, but further work is necessary before conclusions can be drawn.
Complications
Ascending-descending hemorrhagic myelomalacia is a rare complication associated with disc herniation. Permanent loss of function is expected and most animals die of respiratory failure due to loss of diaphragm function as myelomalacia progresses. The disorder is characterized by a change in myotactic reflexes from upper to lower motor neuron in character, progressive loss of panniculus, and loss of function in previously normal forelimbs.
In General
Relative Cost
Conservative treatment with minimal diagnostics averages $300.00. Surgical cost varies; $2,000 to $4,000 and above is an estimated range for surgery.
Prognosis
Nonambulatory animals that undergo surgical decompression recover faster and more completely than those treated conservatively.12-14 For animals that have sensory function, prognosis is favorable, with expected recovery rates of 70% to 100%.12-16 Animals with complete sensory loss have a guarded to fair prognosis. Recovery is unpredictable (0 to 75% recovery rates16-19), but recovery may occur with time and patience. The prognosis for asensory dogs can worsen the longer treatment is delayed or the longer they go without regaining sensation.16-19 Recurrence occurs in approximately 6% of dogs that undergo surgical decompression, and dachshunds are more likely to have recurrence (10% vs 3% for other breeds),7 but recurrence may approach 20%.20 Recurrence may be higher in dogs treated conservatively. 21