Ask the Expert: How should common human medication intoxications be treated in veterinary patients?
Accidental ingestion of human prescription medications, over-the-counter drugs, recreational substances, and dietary supplements is a common veterinary emergency and a leading reason pet owners and veterinary team members contact animal poison control centers. Common ingestions include over-the-counter and prescription anti-inflammatory drugs, psychotropic medications (eg, stimulants, antidepressants), marijuana, and vitamin D supplements. Effective diagnostic, monitoring, and treatment plans are important for affected patients, and, even in cases in which the agent or mechanism is not known, applying key principles of toxic exposure management and promptly addressing life-threatening abnormalities are essential for positive patient care and outcomes.
General Approach
For suspected or known ingestion, the specific formulation, dose, and nonactive ingredients should be obtained, as many nonactive ingredients (eg, xylitol) can be toxic and multiple formulations of medications are often available. Asking the owner careful questions may help reveal a potential toxic exposure. (For example, Are there any prescription or recreational medications in the household? Tell me about the formulations of these medications. Are there any artificial sweeteners or extended-release medications?) Consultation with a veterinary poison control center is often recommended, particularly with complex or atypical cases, because of the wide variation of available doses and formulations.
Many toxins can result in life-threatening problems. Initial stabilization of the airway, breathing, and circulation, as well as assessment for neurologic problems, are imperative.
Although decontamination typically involves induction of emesis followed by administration of a binding agent (eg, charcoal, cholestyramine), adverse effects or contraindications are possible. In addition, charcoal is not effective for many toxic exposures (eg, antifreeze, hydrocarbons), and the timing of exposure may not warrant administration of a binding agent. In subclinical patients presented <4 hours after ingestion, apomorphine or ropinirole may be beneficial for emesis induction in dogs, and dexmedetomidine or hydromorphone can be used in cats1; however, success of emesis in cats is inconsistent. When indicated, alternative decontamination methods (eg, gastric lavage) can be performed, but the patient should be anesthetized and intubated to provide comfort and limit risk for aspiration pneumonia.
General supportive care depends on clinical signs and may include antiemetic therapy, IV fluid therapy, cardiovascular monitoring (eg, blood pressure, electrocardiogram), oxygen therapy, or other supportive care. Some specific medications used for human medication intoxications are listed in Table 1.
Contraindications for Inducing Emesis
Many patient- and toxin-related contraindications to induction of emesis are possible. Emesis induction is not necessarily a benign procedure and can result in aspiration pneumonia, vagal events, or choking. Patient dehydration and unwillingness to ingest food, water, or binding agents (potentially exacerbating the effects of a toxin) are possible but often minimal.
Contraindications may include respiratory distress (eg, brachycephalic airway syndrome), inability to protect the airway (eg, laryngeal paralysis), seizures or neurologic impairment, bradycardia, weakness, esophageal or other GI disease (eg, inability to open the mouth to expel contents), and recent surgery.
Toxin-related reasons to avoid emesis induction include rapid absorption that may limit effectiveness of emesis and ingestion of products that may be corrosive or sharp. Dangers like the ones associated with zinc phosphide are also possible for veterinary team members.
Contraindications for Inducing Emesis
Patient Considerations
Respiratory distress and/or disease
Seizures
Neurologic impairment
Weakness
Inability to protect airway
GI and/or abdominal disease
Toxin Considerations
Corrosives
Acid substance
Alkali substance
Sharp objects
Potential danger to staff
Previous significant vomiting
Underlying disease causing predisposition to aspiration (eg, laryngeal paralysis, megaesophagus)
NSAID & Acetaminophen Ingestion
NSAIDs interrupt prostaglandin production by inhibiting cyclooxygenase and can result in decreased blood flow to renal and GI systems; local ion trapping may also exacerbate gastric ulcers. Liver and platelet function may be affected by large-quantity or chronic ingestion. Severe ingestions can result in neurologic signs. Toxicosis severity and treatment duration may be impacted by dehydration, time between exposure and decontamination, specific medication ingested, and pre-existing hepatic, renal, or GI disease. Vomiting and diarrhea secondary to GI irritation are the most common signs but may not be evident with acute exposure.
Accidental NSAID ingestion untreated for >8 hours can cause risk for acute renal failure and GI ulceration. In patients that have ingested large doses, decontamination, rehydration with fluids (if indicated), and provision of twice-maintenance IV fluids for ≥48 hours are routinely recommended to prevent renal injury. Anecdotally, the value of more than maintenance fluids has been questioned for many renal toxicities; however, administration of twice-maintenance fluids for ≥48 hours is routinely recommended by veterinary poison control centers, as elimination of many NSAIDs is through the kidneys.
GI protectants (eg, misoprostol, H2-blockers, proton pump inhibitors, sucralfate) may be beneficial. Misoprostol can help maintain GI blood flow. Proton pump inhibitors and H2-blockers can help reduce gastric acid; sucralfate coats the ulcerated region and should be administered if a GI ulcer is suspected.
Simple renal injury may respond to fluids and medications; oliguria and anuria require intensive patient monitoring and treatment. Liver injury has been reported with some NSAID ingestions and may warrant further therapy.2 Baseline serum chemistry profile and daily monitoring for at least 48 to 72 hours are recommended. Intravenous lipid emulsions may have some benefit for large overdoses that result in neurologic signs and for some specific drugs.3 If available, extracorporeal therapies (eg, therapeutic plasma exchange, charcoal hemoperfusion) can be useful in the acute setting to remove the toxin or if oliguria or anuria develop.4
Acetaminophen (ie, paracetamol) differs from NSAIDs in that it primarily inhibits cyclooxygenase-3 and thus does not typically cause GI ulceration; however, the metabolites can induce significant hepatocellular damage and oxidative injury to RBC membranes. Cats are particularly susceptible to acetaminophen toxicity because of their limited glucuronidation capacity.
Following standard decontamination, liver enzyme activity and CBC should be closely monitored. In patients with clinical signs of toxicity (eg, methemoglobinemia, hepatic injury), treatment often includes N-acetylcysteine, S-adenosylmethionine, and supplementation with silymarin and vitamin C.5 Severe cases may require oxygen therapy and, in some instances, blood transfusions.
Antidepressant Ingestion
Most antidepressant medications work via reuptake inhibition or altered transport of serotonin, norepinephrine, or dopamine (see Common Psychotropic Medications). Many of these drugs are rapidly absorbed and are available in extended-release or long-acting formulas.
Clinical signs of toxicosis can vary depending on the medication. Selective serotonin reuptake inhibitors (SSRIs) can result in serotonin syndrome, affecting the cardiovascular (eg, hyper- or hypotension, tachycardia), GI (eg, vomiting, diarrhea), and neurologic (eg, sedation, agitation, ataxia, tremors, seizures) systems.6
Common Psychotropic Medications
Monoamine oxidase inhibitors
Selegiline
Noradrenergic and specific serotonergic antidepressants
Mirtazapine
Norepinephrine-dopamine reuptake inhibitors
Bupropion
Norepinephrine reuptake inhibitors
Atomoxetine
Viloxazine
Serotonin-norepinephrine reuptake inhibitors
Duloxetine
Venlafaxine
Tricyclic antidepressants
Amitriptyline
Clomipramine
SSRIs
Fluoxetine
Paroxetine
Sertraline
Citalopram
Escitalopram
Stimulants
Dexmethylphenidate
Dextroamphetamine
Dextroamphetamine and amphetamine
Lisdexamfetamine
Methylphenidate
Standard decontamination is recommended but should be avoided in patients with clinical signs because of risk for aspiration. Supportive care for clinical signs is the mainstay of therapy. Fluid therapy does not enhance elimination but may help correct dehydration and acidosis; sodium bicarbonate may be administered to patients with severe acidosis. Passive and/or active cooling may be necessary for hyperthermic patients.
Propranolol or esmolol can be used for supraventricular tachyarrhythmias; norepinephrine or epinephrine can be used for hypotension.6-8 Benzodiazepines should generally be avoided with many of these medications; sedation may be accomplished with acepromazine or butorphanol. Methocarbamol has been recommended as an alternative therapy for tremors. Phenothiazine use remains controversial. Seizures can be treated with levetiracetam, phenobarbital, or propofol. Although not specifically studied in toxicologic overdoses, status epilepticus not responsive to levetiracetam and/or barbiturates may be responsive to propofol or inhalant (isoflurane) anesthesia.8-13 Specific therapy includes serotonin antagonism with cyproheptadine but is only indicated for a single dose and only when signs are present.
Stimulant Ingestion
Amphetamines are stimulants commonly used for obesity, attention-deficit/hyperactivity disorder (ADHD), and other disorders in humans. Stimulants inhibit norepinephrine and dopamine reuptake in the brain. Clinical signs are neurologic (eg, agitation, shaking/trembling, circling, seizures, disorientation, coma, death), cardiovascular (eg, tachycardia, hypertension, potential reflex bradycardia), and GI (eg, vomiting, abdominal pain) effects. Rhabdomyolysis, hyperthermia, and disseminated intravascular coagulation occasionally occur.
Standard decontamination should be used judiciously because of possible inability to protect the airway. Intravenous fluids can be helpful for dehydrated patients and may help improve urinary excretion. Keeping the patient in a quiet, dark room to minimize stimulation may help.
Additional treatment (Figure 1) should be supportive and for clinical signs. Phenothiazines (eg, acepromazine) are first-choice agents for excessive stimulation and may also be used for treatment of hypertension and hyperthermia. Butorphanol may be useful in some patients. Use of benzodiazepines in patients with stimulatory signs is controversial and generally avoided, as neurologic adverse effects can be exacerbated; however, benzodiazepines may be used for seizures. Levetiracetam, phenobarbital, and propofol are common first-choice agents for seizures.8-14 Excessive muscle fasciculations may also be treated with methocarbamol. IV fluids and cooling may be necessary for patients with elevated body temperatures. IV lipid solutions may be considered for specific medications because some ADHD medications are lipophilic.15


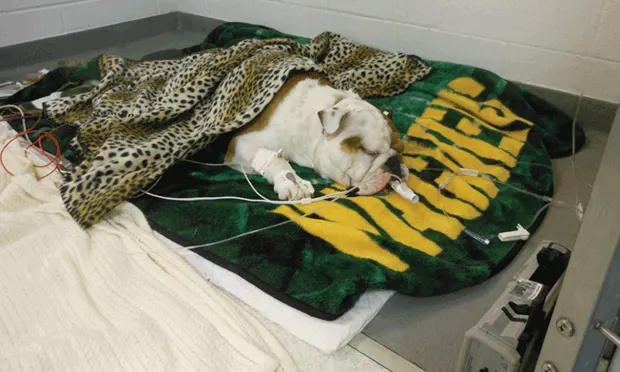
A 1-year-old intact male bulldog presented after ingestion of dextroamphetamine and amphetamine. The patient was hyperthermic and tachycardic and developed seizures. Sedation, antiepileptic medications, and a beta blocker were administered to control signs. Endotracheal intubation and intermittent oxygen supplementation were required because of heavy sedation (A). After 36 hours, the patient was normothermic, had a normal heart rate, and no longer had seizures (B). Several days after presentation, the owner reported the dog was doing well.
Marijuana Ingestion
Marijuana (Cannabis sativa) contains delta-9-tetrahydrocannnabinol (THC), which alters neurotransmitter activity, and is available as a legal prescription or recreational substance for humans in some states. Veterinary patients that ingest marijuana are typically presented with altered mental status, ataxia, and dilated pupils; potential agitation, seizures, and/or coma may result in death. Additional signs can include vomiting, diarrhea, arrhythmias, tachypnea, and incontinence. In dogs, over-the-counter urinary tests are unreliable for diagnosis.16
Decontamination should be avoided when altered mental status is present, and emesis is often unrewarding. Supportive care is the mainstay of treatment. Because renal elimination of THC is minimal, the benefit of diuresis is questionable; fluids may be used for dehydration. Benzodiazepines can be used safely for agitation, seizures, and tremors; monitoring body temperature, respiration, and heart rate is essential. Most patients recover uneventfully within 24 to 96 hours; however, ingestion of large quantities may require aggressive supportive care.
Although research on IV lipid infusions is minimal, success has been reported, and this treatment is often considered in patients with severe neurologic signs.17 Extracorporeal therapy has been reported in a severely affected dog.18
Vitamin D Ingestion
Vitamin D3 (ie, cholecalciferol) is available as a sole supplement, in multivitamins (which may also contain toxic levels of iron, xylitol, and vitamin A), and in rodenticides. Initial clinical signs (8-12 hours after ingestion) are vague and include lethargy, vomiting, diarrhea, and inappetence resulting in hypercalcemia and renal failure (occurring 36-48 hours after ingestion), which can cause polyuria, polydipsia, weakness, hematemesis, and arrhythmias. Mineralization of tissues occurs with persistent hypercalcemia, especially in GI, kidney, and neurologic tissues.
Decontamination should be initiated immediately, as vitamin D3 has a prolonged action and treatment can be challenging and costly if hypercalcemia develops. When decontamination is not possible or is incomplete, IV lipid emulsion may help prevent hypercalcemia, as vitamin D is fat soluble. Cholestyramine is typically recommended in cases of large, acute doses.
Ionized calcium levels should be monitored every 24 hours for 5 to 7 days. When ionized hypercalcemia is present, therapies (eg, 0.9% saline diuresis, corticosteroids, salmon calcitonin) may need to be combined. Furosemide is only recommended if bisphosphonates are not available and should only be used in hydrated patients, as dehydration can potentially worsen azotemia. Bisphosphonates (eg, pamidronate, zoledronate) inhibit osteoclast function and have prolonged activity, making these drugs a good alternative if other therapy is unavailable or ineffective.
Difficult topics and alternative approaches to care can be tough to communicate with clients. Use Top 5 Tools for Communicating in Tough Situations to better understand how these 5 tools can help you hold your own in tough situations.
Show empathy
Use personality and behavior assessments
Be aware of body language
Listen respectfully
Be confident