Prognosticating in Dogs With Heatstroke
Elke Rudloff, DVM, DACVECC, Lakeshore Veterinary Specialists, Glendale, Wisconsin
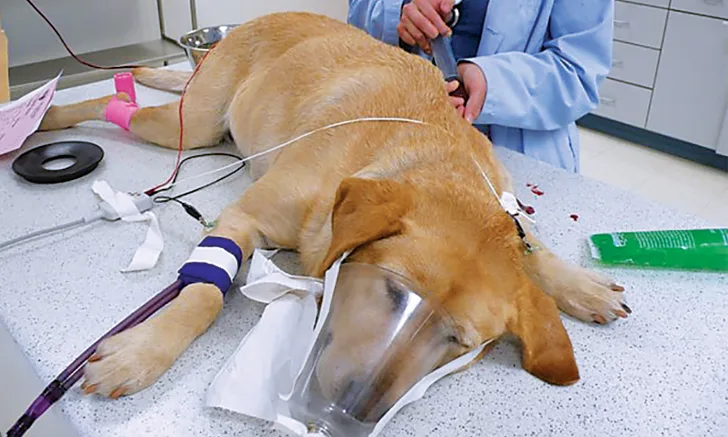
A young Labrador retriever with heatstroke after being taken jogging on a hot (90°F) and humid day. The dog was hosed off with cool water at home before presentation; rectal temperature on presentation was 105.5°F.
In the Literature
Bruchim Y, Kelmer E, Cohen A, Codner C, Segev G, Aroch I. Hemostatic abnormalities in dogs with naturally occurring heatstroke. J Vet Emerg Crit Care (San Antonio). 2017;27(3):315-324.
The Research …
Heatstroke is a serious, life-threatening condition that is reported to result in mortality (natural and euthanasia) in more than 40% of cases.1-4 Heatstroke is a concern for both owned and tactical-use dogs. Research to identify prognostic markers, which clinicians could use to advise owners about treatment or euthanasia in affected dogs, is ongoing.
Heatstroke commonly causes both a hyper- and hypocoagulable state; development of overt bleeding and microthrombi are unpredictable.2,5 Because of the dynamic nature of the coagulation pathway and its unpredictable effects, it is difficult to know if and when coagulation derangement treatment is indicated.
The authors of this study, which investigated whether specific coagulation tests can confer a prognosis, have published the most information investigating the pathophysiology, prognostic markers, and outcomes in dogs with heatstroke.2,3,5
All but one of the 30 dogs in this study received fresh frozen plasma; 90% were male dogs. These points should be taken into consideration when results are evaluated. It is unclear whether the prophylactic treatment with fresh frozen plasma affected outcome. Alterations in prothrombin time, activated partial thromboplastin time, total protein C activity, and fibrinogen concentrations appeared to be associated with outcome at 12 to 24 hours postpresentation. There were no admission coagulation test results that could be used for prognosis at treatment onset.
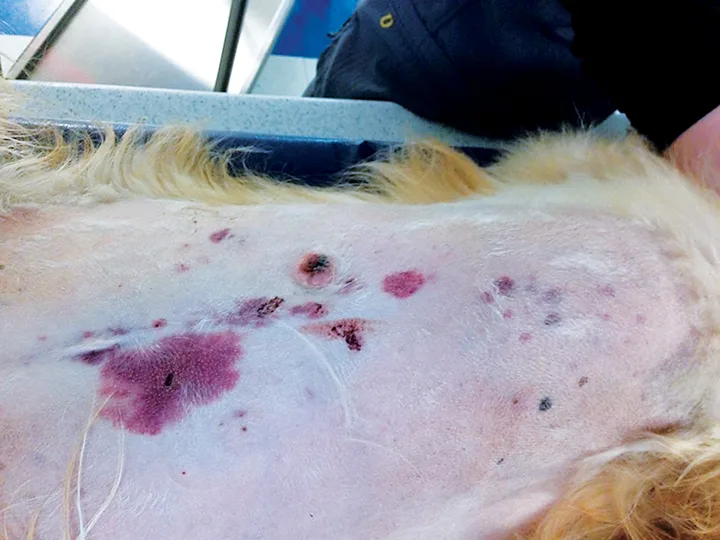
Petechiae and ecchymosis that developed in an older, overweight crossbreed dog within 4 hours of presentation. The dog had been left in a car in 80°F heat for 30 minutes, and its body temperature on presentation was 106.4°F.
… The Takeaways
Key pearls to put into practice:
Because of the incidence of hemostatic defects and the need for repeated blood sampling, placement of a blood-sampling catheter in heatstroke patients could reduce the need for percutaneous needle sticks and potential blood vessel damage.
Although the variables tested in this study are not all readily available without access to a 24-hour comprehensive diagnostic laboratory, most emergency clinics have the capability to monitor prothrombin time and partial thromboplastin time in-house.
Prothrombin time and activated partial thromboplastin time are ideally monitored every 6 to 12 hours for at least 48 hours. Increased clotting times from baseline and after 12 hours may be associated with increased mortality.