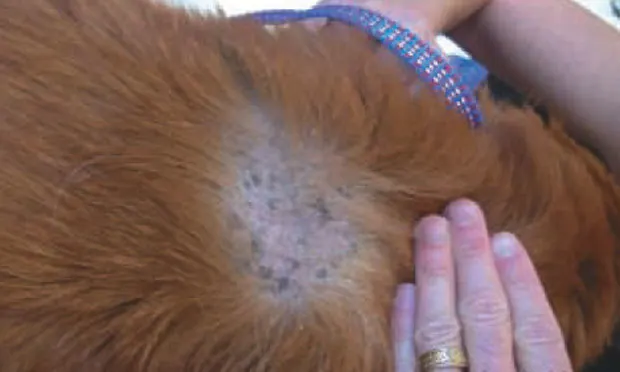
Ginger, a 9-year-old spayed female golden retriever/basset hound mix, was presented for evaluation of "greasy," odiferous dermatitis.
History. Previously, Ginger had been evaluated and treated for seborrhea secondary to atopy, hypothyroidism, and infection. Otitis and pruritus were present historically as well as currently. The clinical signs had been relatively well controlled with a combination of allergen-specific immunotherapy, soloxine, and bathing 2 to 3 times weekly with a miconazole/chlorhexidine shampoo, but occasional exacerbations required corticosteroids and systemic antimicrobial agents.
Examination. Ginger exhibited generalized erythema and thin hair coat. Patches of more obvious erythema and nearly complete alopecia were present over the rump and bilaterally on the thoracic wall. An erythematous, mildly proliferative, waxy dermatitis was present on Ginger's ears, shoulders, and neck (See PDF for Figures 1 through 3). The skin and hair coat had a waxy texture that most veterinarians would describe as "greasy seborrhea."
Laboratory Analysis.Cytology of the skin and ears revealed large numbers of cocci and yeast organisms. Multiple skin scrapings were negative for parasites.
ASK YOURSELF ...
What is the etiology of this patient's clinical signs?
A. Bacterial and yeast infections
B. Allergies
C. Hypothyroidism
D. All of the above
Correct answer: D All of the above
The seborrhea is probably associated with and complicated by multiple coexisting causes.
Discussion. Traditionally, "seborrhea" had been used as a term for a distinct diagnostic entity that was further classified as either primary or secondary. However, the terms cornification orkeratinization defect are becoming the preferred terminology when discussing what was once called "primary seborrhea." Most patients with clinical signs of seborrhea have at least one underlying cause.
"Seborrhea" remains a clinically useful, descriptive word. It is often combined with adjectives used to characterize the appearance of the skin and hair as either "greasy" (oleosa) or "dry" (sicca).
Client education is important to emphasize the need to identify and control diseases that may cause seborrhea. It is equally important for the veterinarian to determine the ability of the client to physically and financially manage these patients and to work within these abilities. Often a delicate balance must be achieved with regard to maintenance therapy, but exacerbating factors, such as parasites, microbial overgrowth, allergy flare-ups, or missed baths, can cause significant setbacks in the patient's therapy.
Diagnosis. Ginger had multiple primary and secondary factors contributing to the seborrhea. The history, physical examination, and laboratory findings were quite compatible with bacterial and yeast infections secondary to the previously diagnosed hypothyroidism and atopy.
Additional historical information indicated that Ginger's hair coat remained "mildly greasy" unless she was bathed frequently; basset hounds are predisposed to cornification defects, so such a defect may have also been present.
The client related that she had been able to control Ginger's dermatitis by providing optimum care until the medical needs of a human family member disrupted the entire household's routine. She sought veterinary care to provide short-term relief of pruritus and odor while planning to reinitiate the previously successful long-term maintenance therapy.
Treatment. For short-term relief of the severe pruritus, dexamethasone SP was administered subcutaneously at a dose of 0.22 mg/kg; a phytosphingosine-containing microemulsion spray (Douxo Seborrhea Micro-emulsion Spray; Sogeval, www.sogevalus.com) was applied in the examination room as odor control and to demonstrate it as an option to frequent bathing.
A 21-day course of cefpodoxime, 5 mg/kg Q 24 H PO (Simplicef; Pfizer, www.pfizerah.com); a 14-day course of fluconazole, 5 mg/kg Q 24 H PO; and a 10-day course of a topical gentamicin, mometasone, and clotrimazole otic suspension (Mometamax; Schering-Plough Animal Health, www.sch-plough.com), along with use of an existing otic cleaning agent at the client's home were initiated. Thyroid replacement therapy and allergen-specific immunotherapy were reinstated for long-term control of the hypothyroidism and allergies. For topical therapy, a combination of the client's existing miconazole/chlorhexidine shampoo (Malaseb; IVX Animal Health, www.ivxanimalhealth.com) and the phytosphingosine spray were recommended.
Long-term follow-up over the next 18 months demonstrated that the client was again able to control Ginger's clinical signs with a combination of allergen-specific immunotherapy, thyroid replacement therapy, and topical use of twice-weekly phytosphingosine spray and twice-monthly miconazole/chlorhexidine shampoo. The use of phytosphingosine spray allowed the client to conveniently pursue regular application of therapy.
Take-Home Messages · Seborrhea is often associated with multiple contributing or coexisting causes that should be addressed.
· Frequent bathing can facilitate management of seborrhea but may not be practical for all clients. Topical sprays can be a more convenient and cost-effective option.
· According to the American College of Veterinary Dermatology Task Force on Canine Atopic Dermatitis, allergen-specific immunotherapy is the only available treatment option that has the potential to result in partial or complete remission of canine atopic dermatitis without the further need of additional antiinflammatory drugs.
TX at a glance
· Short-term relief of pruritus:Dexamethasone SP (0.22 mg/kg SC)
· Medium-term therapy:-21 days of cefpodoxime (5 mg/kg Q 24 H PO)- 14 days of fluconazole (5 mg/kg Q 24 H PO)- 10 days of gentamicin/mometasone/clotrimazole otic suspension- Otic cleansing at home
· Long-term systemic therapy:- Thyroid replacement- Allergen-specific immunotherapy
· Long-term topical therapy:Frequent baths with miconazole/chlorhexidine shampoo were tapered, but not discontinued. Phytosphingosine spray was substituted for many of the baths.
For related articles, see the following:Scaling & Crusting Skin DiseaseTopical Therapies for Skin DiseaseCanine Atopic Dermatitis
GREASY & ODIFEROUS DERMATITIS • Dunbar Gram & Chris Cook
Suggested ReadingKeratinization defects. In Scott DW, Miller WH, Griffin CE (eds): Muller & Kirks's Small Animal Dermatology, 6th ed- Philadelphia: WB Saunders, 2001, pp 1025-1036.The ACVD Task Force On Canine Atopic Dermatitis (XIX): General principles of therapy. Olivry T, Sousa CA. Vet Immunol Immunopathol 81:311-316, 2001.
Other ResourcesAllergen-specific immunotherapy:www.greerlabs.com