Overview
Hyperthyroidism, the most common endocrine disease in cats, is a hypermetabolic state caused by excessive production and secretion of thyroid hormones. In addition to being vital for growth and development, thyroid hormone controls the metabolic rate and energy expenditure of nearly every organ in the body.
Epidemiology
Signalment
Age
Mean age of affected cats is 13 years (range, 8 months to 24 years).1
Causes & Risk Factors
Similar to toxic nodular goiter in humans, 97% of cats with hyperthyroidism have benign adenomatous nodular hyperplasia.2
Both lobes of the thyroid gland are typically involved.
Possible risk factors include iodine deficiency; iodine content of canned food; fish-, liver-, or giblet-flavored canned food; fire-retardant chemicals; and bisphenols in pop-top cans.1,3,4 These environmental or dietary endocrine disruptors may stimulate genetically predisposed thyrocyte development into hyperplastic and adenomatous nodules that become functionally autonomous. Over time, some tumors may undergo malignant transformation into carcinomas. 2
Clinical Presentation
Cats diagnosed via routine laboratory testing may have minimal to no clinical signs.
Otherwise, clinical signs include weight loss and poor body condition, polyphagia, vomiting, polyuria and polydipsia, diarrhea, weakness, and voluminous stool.5
Restlessness, skin changes, and respiratory signs are also common1
Lethargy and anorexia may be seen with severe hyperthyroidism and/or concurrent disease (eg, occult hyperthyroidism).1,5
Physical examination findings include palpable thyroid nodule (Figure 1), weight loss, heart murmur, tachycardia, and increased nail growth.5
Less common abnormalities include retinal hemorrhage, retinal vessel tortuosity, retinal detachment, dyspnea, and ventral neck flexion.1,5

FIGURE 1 Visible thyroid nodule on the neck of a cat
Differential Diagnoses
Differentials include renal disease, diabetes mellitus, GI lymphoma, exocrine pancreatic insufficiency, inflammatory bowel disease, liver disease, and heart disease.
Comorbidities (eg, cardiac disease, renal disease, GI disease), either concurrently or secondary to the hyperthyroid state, are also common in this older population of cats.2
Diagnostics & Diagnostic Findings
Definitive Diagnosis
Diagnosis should be pursued based on supportive signalment, patient history, and examination findings.
Hyperthyroidism is usually diagnosed via documentation of elevations in serum concentrations of total thyroxine (tT4), a highly specific and sensitive test for diagnosis of feline hyperthyroidism.
Serum thyroxine (T4) levels alone are diagnostic in >90% of cats with hyperthyroidism.6
Measurements of total triiodothyronine (tT3) concentrations are not helpful and have no role in the diagnosis of hyperthyroidism, as 30% of cats with hyperthyroidism have a normal tT3.6
If hyperthyroidism is suspected and tT4 is within the laboratory reference interval, tT4 concentrations may need to be rechecked up to several weeks later, as concentrations may fluctuate in and out of the normal range.
A high-normal tT4 in a middle-aged to older cat should indicate suspicion for hyperthyroidism.
Concurrent disease may also suppress thyroid levels (effect of nonthyroidal illness).1
Additional tests to consider include free thyroxine (fT4) concentration measurement (See Free Thyroxine), triiodothyronine (T3) suppression testing, nuclear scintigraphy, and thyroid-stimulating hormone measurement.
The T3 suppression test involves administration of liothyronine (25 micrograms/cat PO every 8 hours) for 2 days, with an additional dose administered the morning of day 3. Blood should be drawn at baseline and 2 to 4 hours after administration of the final dose for tT3 and tT4 measurement.
The tT4 concentration in cats with hyperthyroidism is >2 micrograms/dL and <1.5 micrograms/dL in healthy cats.
Values between 1.5 and 2 micrograms/dL are nondiagnostic.
The T3 suppression test is useful for diagnosis of mild hyperthyroidism in cases in which tT4 and fT4 are nondiagnostic; however, it may be difficult for pet owners to administer the pills for 3 consecutive days, and failure can result in a false-positive diagnosis.
Nuclear scintigraphy is typically performed at specialized centers (eg, university hospitals, referral facilities).
Technetium-99m is commonly used, is trapped and concentrated in the thyroid, and has a short half-life.
Uptake is compared with uptake in the zygomatic salivary glands.7
Ectopic tissue (<5% of cats with hyperthyroidism) and metastatic tissue can also be detected.7
Thyroid-stimulating hormone can be measured via canine assay or a newer assay optimized for cats.8
If results are normal, hyperthyroidism is less likely.8
Free Thyroxine
fT4 represents the unbound portion of T4 and is the hormonally active portion (<1% of the total).
Measurement is only recommended using a modified equilibrium dialysis technique that separates the bound from the unbound fraction.
Up to 12% of clinically ill, euthyroid cats also have increased fT4 concentrations.6,9
Relevant Laboratory Tests
Minimum Database
CBC results show normal to elevated RBCs, packed-cell volume, and mean corpuscular volume in up to 50% of cats with hyperthyroidism.1,5
Alkaline phosphatase and alanine aminotransferase activities are mildly to moderately elevated in 75% of cats.1
Urine specific gravity is <1.035 in 50% of cats with hyperthyroidism.10
Fructosamine concentrations are decreased below the normal range in 50% of cats with hyperthyroidism because of accelerated protein turnover.1
Fructosamine may not be useful for monitoring diabetes or distinguishing between stress hyperglycemia and diabetes with concurrent hyperthyroidism.1
Thoracic radiographs may show cardiomegaly, pulmonary edema, or pleural effusion.
Abdominal radiographs can help identify comorbid conditions.
Ancillary Testing
Echocardiography and electrocardiography are useful for investigation of cardiac abnormalities found on physical examination and thoracic radiographs.
Blood pressure measurement should be part of the evaluation of every cat with hyperthyroidism.
Ten percent to 20% of cats with hyperthyroidism are hypertensive, and 20% to 25% of normotensive cats with hyperthyroidism become hypertensive following treatment.1
Treatment should be instituted if systolic blood pressure is repeatedly >160 mm Hg or there is evidence of end-organ damage.
Treatment
Hyperthyroidism can be definitively treated with both radioactive iodine and surgery or controlled with drug therapy or a therapeutic diet.
Treatment should be tailored to the needs of each patient, household, and owner.
Definitive therapy is generally optimal, but pharmacologic or dietary therapy may be preferred depending on patient age and comorbidities. Definitive therapy prevents disease progression and possible development of large thyroid cysts and carcinomas.
Methimazole
Methimazole is readily available, reliable, convenient, and inexpensive short-term but is potentially toxic and requires daily administration, and disease control is dependent on compliance.
Methimazole blocks synthesis of T4 and T3 by inhibiting thyroid peroxidase, disrupting iodination of tyrosine residues on thyroglobulin, and preventing the coupling of diiodotyrosine and monoiodotyrosine.
The typical starting dose is 2.5 mg/cat PO every 12 hours, but some mildly affected cats may be controlled with 1.25 mg/cat PO every 12 hours or 2.5 mg/cat PO every 24 hours.
Less than 5% of adverse effects (eg, leukopenia, thrombocytopenia, hepatopathy, myasthenia gravis) are life-threatening.1
Agranulocytosis may be immune-mediated.
Other adverse effects include eosinophilia, lymphocytosis, self-induced excoriations (up to 15%), positive antinuclear antibody result, vomiting, and anorexia (up to 20%).1
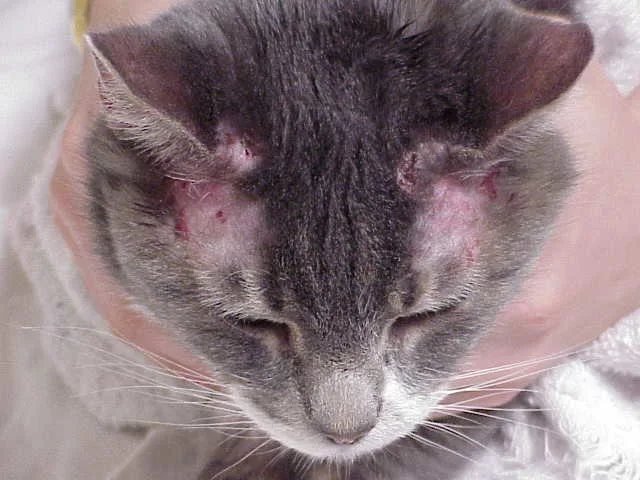
Vasculitis may cause skin excoriations (Figure 2).
Adverse effects occur within the first 3 months of therapy. CBC, platelet count, serum chemistry profile, and tT4 should be checked every month for 3 months, then every 3 to 6 months.
The goal of treatment is tT4 concentrations in the lower half of the reference interval within 1 month.
If tT4 is not decreasing, administration problems, infrequent or inadequate dose, and thyroid carcinoma (rare, <3%) should be ruled out.7
Various formulations are available.
For cats in which oral administration is difficult, methimazole can be formulated as a pluronic lecithin organogel for transdermal use.11
A branded, small, coated pill is available in 2.5 mg and 5 mg sizes and is FDA-approved for use in cats.
A branded 5 mg/mL oral solution is palatable and FDA-approved for use in cats.
Special precautions are required to handle methimazole, especially in pregnant individuals. It is important to wear gloves, wash hands after handling, not crush or split tablets, and dispose of unused product in the trash.


FIGURE 2 Methimazole drug reaction in a cat; self-induced excoriation on the head (left) and excoriation between the toes (right) can be seen.
Radioactive Iodine
Radioactive iodine is curative, is noninvasive, and results in a rapid response.
Radioactive iodine is actively taken up by hyperplastic thyroid tissue, destroys diseased tissue, and spares atrophied normal tissue.
A median dose of 1.9 mCi (reference interval, 1-10.6 mCi) was shown to reduce the frequency of posttreatment hypothyroidism and azotemia.12
Hospitalization varies widely, depending on the agency licensing the facility.
Disadvantages include expense, availability, need for short-term hospitalization, and limited contact with the patient for 2 weeks posttreatment.
Treatment is successful in 94% of cats.
Two percent of cats become hypothyroid, 1.5% remain hyperthyroid, and 2.5% relapse within 1 to 6.5 years of treatment.
Cats should be monitored for hypothyroidism and azotemia starting 2 weeks posttreatment.
Thyroidectomy
Multiple techniques (ie, extracapsular, intracapsular, modified intracapsular, staged thyroidectomy; Figure 3) have been described to remove the thyroid glands.
Approximately 70% of cats have bilateral involvement.7
Scintigraphy may be helpful to localize ectopic thyroid tissue and identify the ≈5% of cats that do not benefit from surgery.7
Surgery is beneficial, curative, and usually permanent. Recurrence is possible if surgery is incomplete or unilateral thyroidectomy is performed.
Risks include damage to recurrent laryngeal nerves and hypoparathyroidism; disadvantages include anesthesia risks in cats with concurrent heart and kidney disease.
Cats that become hypothyroid and azotemic postoperatively should be treated.

FIGURE 3 Surgical excision of a thyroid nodule
Nutrition Management
A prescription thyroid care diet that is iodine restricted can limit synthesis of thyroid hormones and is effective in >80% of cats, with 50% achieving thyroid values in the low end of the normal range by 60 days13; however, clinical signs of hyperthyroidism may not improve, and success depends on readiness of the cat to eat this diet and avoid all other food, treats, supplements, and well water.
A thyroid care diet can be considered for cats in which methimazole therapy was not successful and definitive therapy is not an option.
tT4 concentrations and serum kidney values should be monitored 4 weeks after the diet is initiated; tT4 should be decreased after 4 weeks and normal within 8 weeks.
If concentrations remain elevated, dietary history (including water source) should be evaluated.
Monitoring & Follow-up
Hypothyroidism is common posttherapy and, if accompanied by azotemia, is associated with shorter survival times.14
Kidney values and tT4 should be monitored every 2 to 4 weeks for up to 3 months following definitive therapy and every 3 to 6 months for cats receiving methimazole.
If hypothyroidism is accompanied by azotemia, levothyroxine may help improve renal blood flow and glomerular filtration rate.15
Prognosis
Prognosis is excellent in cats with uncomplicated hyperthyroidism and varies in cats with severe hyperthyroidism or when concurrent disorders are present.
Outcome depends on successful management of thyroid complications and comorbid disease.
Average survival after successful treatment is 2 years but depends on the age of the cat and the treatment modality.
Hyperthyroidism & Renal Disease
Hyperthyroidism and renal disease are common in older cats and frequently occur concurrently. Hyperthyroidism can mask renal disease because of increased renal blood flow and glomerular filtration rate and lower muscle mass. With treatment, the true state of kidney function is revealed. Twenty five percent of cats with hyperthyroidism may become mildly to moderately azotemic posttreatment. If a cat becomes hypothyroid posttreatment, azotemia can worsen. How azotemia development affects survival is uncertain, but studies have shown no significant difference between azotemic versus nonazotemic euthyroid cats.14,15 In a study, however, survival time of cats that became azotemic and hypothyroid following treatment was shorter compared with nonazotemic cats.14
Predicting which cats with hyperthyroidism will become azotemic with treatment is difficult. Pretreatment creatinine, BUN, and symmetric dimethylarginine at the high end of the reference interval, as well as urine specific gravity <1.035, are suggestive of pre-existing renal disease.2
Treatment (eg, surgery, radioiodine therapy) with methimazole prior to definitive treatment for hyperthyroidism can reveal the extent of renal disease, but clinical delineation may require 3 to 6 months of therapy.2