Blepharitis (ie, inflammation of the eyelids) is common in cats and dogs and can be accompanied by swelling of the eyelids, thickening or irregularities of the eyelid margins, erythema of the eyelid skin, alopecia (ie, periocular hair loss), conjunctival hyperemia, and/or ocular discharge. Eyelid skin can also become ulcerated, crusty, flaky, and/or lichenified. Blepharitis can be unilateral or bilateral and may affect the entire superior and/or inferior eyelids or just a focal area. Self-trauma leading to excoriations and secondary infection can complicate the condition.
Discussion
Determining the underlying cause of blepharitis can be challenging, as this condition is often nonspecific and can be associated with systemic conditions (eg, environmental allergies, infectious diseases). Eyelids are composed of skin with modified oil glands (ie, meibomian glands) and lined with a mucous membrane (ie, palpebral conjunctiva) and can therefore be affected by etiologies that lead to generalized dermatitis, as well as localized problems (eg, drug reactions, local bacterial or fungal infections, impacted/inflamed oil glands [eg, chalazia, meibomitis]). Immune-mediated disease is common and may result in inflammation of the eyelids, either as part of a generalized condition (eg, pemphigus foliaceus) or limited to the periocular skin. Primary or secondary neoplasia can affect the eyelids; secondary or paraneoplastic processes can also be associated with eyelid disease.
Signalment and a thorough patient history, including current medications or previous dermatologic problems, are important for determining differential diagnoses in patients with blepharitis. Diagnosis and treatment can be difficult in cases in which no obvious cause is found via skin scraping, cytology and culture and susceptibility testing, or histopathology. Treatment is often focused on controlling inflammation and managing suspected infectious or other complicating etiologies and may be protracted, as recurrence is common in patients with presumed immune-mediated blepharitis.
Canine Juvenile Pyoderma

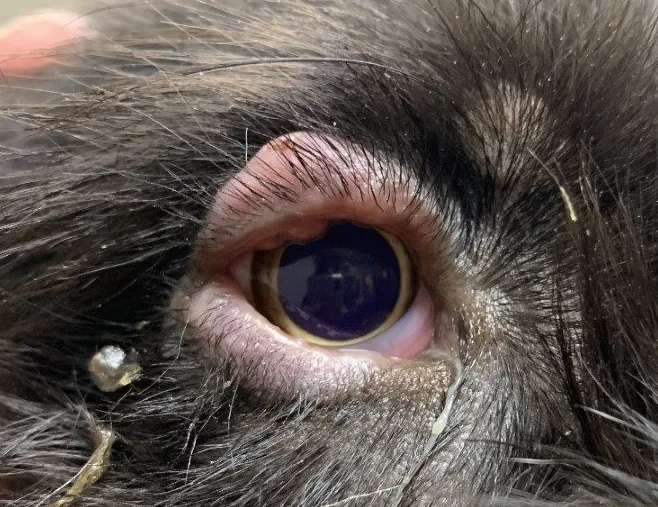
A 5-month-old crossbreed dog was presented for marked bilateral eyelid swelling and ocular discomfort. Purulent blepharitis as part of canine juvenile pyoderma syndrome was suspected based on eyelid appearance and patient age. A local staphylococcal infection resulting in a severe hypersensitivity reaction and inflammatory response was also suspected. A systemic antibiotic (doxycycline, 5 mg/kg PO every 12 hours for 3 weeks) and prednisone (1-2 mg/kg PO every 24 hours, slowly tapered over 6 weeks) were administered, and clinical signs resolved. An Elizabethan collar was also recommended to prevent self-trauma.
In many cases of blepharitis suspected to have a bacterial component, systemic antibiotics are preferred over topical antibiotics, as topical antibiotics safe for the ocular surface do not possess adequate skin penetration. Oral doxycycline is a common choice for treatment of blepharitis, partly due to its immunomodulatory and broad-spectrum antibacterial properties. In addition, doxycycline is preferred as a first-line antibiotic when appropriate as a part of antimicrobial stewardship to prevent bacterial resistance to other drugs (eg, fluoroquinolones, third- or fourth-generation cephalosporins).
Patients with canine juvenile pyoderma syndrome are often presented with blepharitis in addition to more generalized skin lesions (eg, pyogranuloma, abscessation) on the head and local lymphadenopathy. Other possible differentials include fungal or parasitic blepharitis and local contact dermatitis. Fine-needle aspiration of lesions with cytology, culture and susceptibility, skin scrapings, or tissue biopsy may aid in diagnosis.
Chalazion With Conjunctival Inflammation

A 4-year-old terrier crossbreed was presented for intermittent squinting and rubbing of the right eye. The eyelids were everted during examination to check the palpebral conjunctiva for abnormalities (eg, ectopic cilia [ie, abnormal hairs growing from the conjunctival surface], chalazia [ie, impacted meibomian glands that may become secondarily infected with bacteria (hordeolum) and cause pain and swelling]). Several small, yellow–tan lesions in the palpebral conjunctiva appeared to be chalazia. Warm compresses to the eyelids and a topical ophthalmic antibiotic ointment containing dexamethasone were applied every 8 hours for 2 weeks to resolve discomfort and allow expression of meibomian gland material (ie, meibum, oily sebaceous material) through the eyelid margin openings.
Impacted eyelid glands are not always painful, but local secondary bacterial infection can lead to discomfort and self-excoriation that causes conjunctival hyperemia and swelling.
Bilateral Lipogranulomatous Conjunctivitis & Blepharitis


A 10-year-old domestic shorthair cat was presented for chronic, progressive bilateral eyelid swelling and ocular discharge of 2-years’ duration. Topical 0.1% dexamethasone ophthalmic solution was applied every 12 hours. Although there was initial improvement, the eyelids continued to slowly worsen. Eversion of the eyelids showed yellow–tan pustules along the palpebral conjunctiva, severely thickened eyelids, and irregular eyelid margins. Conjunctival biopsy revealed lipid-laden granulomatous hyperplasia and fibrosis with adjacent lymphoplasmacytic and neutrophilic inflammation.
Lipogranulomatous conjunctivitis may occur secondary to meibomian gland damage and associated leakage of meibum into the surrounding tissue, resulting in severe inflammation. This condition may be associated with ultraviolet light exposure and is more common in white or lightly pigmented cats. Surgical debulking followed by topical and/or systemic immunomodulatory drugs (eg, cyclosporine) may help, but this condition can be challenging to manage, and recurrence is common. Cicatricial entropion or ectropion can also occur in chronic cases, potentially leading to ulcerative keratitis and other problems (eg, chronic epiphora, discomfort).
Keratoconjunctivitis Sicca With Secondary Infectious Blepharitis

A 9-year-old Labrador retriever was presented for mucoid discharge, mild conjunctivitis, and depigmentation and swelling of the eyelid margins of the right eye. A Schirmer tear test revealed moderately low tear production (right eye, 10 mm/minute; left eye, 17 mm/minute; normal, >15 mm/minute). Cytology of the eyelid margins showed numerous cocci bacteria and yeast organisms (Figure 1). Keratoconjunctivitis sicca (ie, dry eye) with secondary bacterial infectious blepharitis was diagnosed. Treatment with a topical antibiotic (ophthalmic oxytetracycline ointment every 6 hours for 2 weeks), daily warm compresses, and ocular hygiene wipes was initiated, and eyelid appearance improved. Long-term topical ophthalmic 0.2% cyclosporine ointment was administered to the right eye every 12 hours, resulting in improved quality and quantity of the tear film.


(A) Malassezia spp yeast (2 × 4 mm; arrow) next to an epithelial cell; (B) cocci bacteria within a neutrophil (0.5 mm; arrow)
Feline Eosinophilic Dermatitis

A 6-year-old domestic shorthair cat was presented for periocular alopecia, erythema, and crusts of 3-months’ duration. Cytologic analysis of the lesions obtained via gentle skin scraping with a #10 scalpel blade revealed numerous eosinophils, which are typically associated with immune-mediated or allergic disease, insect bite hypersensitivity, or parasites. Monthly parasite preventives were up to date. Mild feline eosinophilic granuloma complex was therefore suspected. Oral prednisolone (initially, 1 mg/kg every 24 hours for 10 days, tapered to 0.5 mg/kg every 24 hours for 10 days, followed by 0.5 mg/kg every 48 hours 5 times) was administered.
Periocular lesions resolved by the 3-week follow-up, but lesions recurred 4 months after prednisolone was discontinued. Similar lesions were also seen on the skin of the ventral abdomen. Oral prednisolone was re-administered for 3 weeks (at the same dosages as listed previously) in conjunction with oral cyclosporine modified microemulsion (7 mg/kg every 24 hours for 4 weeks, decreased to 7 mg/kg every 48 hours) for long-term management. Baseline CBC, serum chemistry profile, and electrolytes were obtained prior to cyclosporine therapy, and kidney/liver panels were recommended every 3 to 4 months for monitoring. This maintenance immunomodulatory therapy controlled signs of periocular and generalized dermatitis.
Flea Allergy Dermatitis


A 3-year-old domestic shorthair cat was presented for periocular dermatitis mainly involving the eyelid skin. Lesions were also noted behind the ears, and the patient was extremely pruritic. Lesions were suggestive of allergic skin disease, which can be related to fleas, food, or the environment and may have similar skin reaction patterns. Parasite preventives were not up to date, and live fleas were found on examination. Oral prednisolone (initially, 1 mg/kg every 24 hours for 10 days, tapered to 0.5 mg/kg every 24 hours for 10 days, followed by 0.5 mg/kg every 48 hours 5 times) was administered due to the intensity of the pruritus, observed self-excoriation, and severity of skin lesions. Regular monthly parasite control was prescribed for long-term management. Clinical signs resolved.
In cases of severe flea infestation, environmental flea control may also be recommended.
Demodicosis-Associated Blepharitis

A 1-year-old crossbreed dog was presented for nonpruritic periocular alopecia and erythema with crusting and flaking of the skin. Skin scraping revealed numerous cigar-shaped organisms (likely Demodex canis mites [ie, mange mites]). A spot-on topical (2.5% moxidectin, 10% imidacloprid) medication was administered weekly for 4 treatments,1 then monthly for long-term parasite maintenance. Erythema and crusting of the skin resolved in 3 to 4 weeks. Periocular hair grew back after several months.
Other options for treatment of demodicosis include isoxazoline products.2,3
Immune-Mediated Blepharitis

A 3-year-old Samoyed was presented for chronic thickening of the left eyelid, alopecia, hyperpigmentation of the skin, and crusty/ulcerated lesions that progressively worsened over the previous 6 months. Prior treatment with ivermectin (unknown dosage and route) for suspected demodicosis did not result in improvement, and skin scraping with cytology revealed scant numbers of cocci bacteria. A systemic antibiotic (doxycycline, 5 mg/kg PO every 12 hours for 3 weeks) and prednisone (1 mg/kg PO every 24 hours, tapered over several weeks) were administered for suspected immune-mediated blepharitis possibly associated with local staphylococcal hypersensitivity. Clinical signs improved but did not resolve. Cyclosporine (5 mg/kg PO every 24 hours for 30 days, tapered to every 48 hours) and niacinamide (ie, vitamin B3; 500 mg/dog PO every 8 hours, ongoing) were added, leading to further improvement and long-term control of the suspected immune-mediated condition.
Immune-mediated blepharitis may typically be bilateral, but unilateral presentation is not uncommon. Other possible differentials include fungal or parasitic blepharitis, local (contact) hypersensitivity, and allergic dermatitis. Skin biopsy may be recommended in unresponsive cases.
Allergic- or Atopic Dermatitis-Induced Blepharitis

An 8-year-old Labrador retriever was presented for bilateral eyelid swelling, moderate conjunctival hyperemia, and facial pruritus. The patient had a history of chronic licking of the feet and seasonal allergies previously attributed to pollen. Differentials included fungal or parasitic blepharitis, local (contact) hypersensitivity, and allergic or atopic dermatitis. Atopic dermatitis was presumptively diagnosed based on patient history of systemic allergies. Treatment with a combination of systemic immunomodulatory therapies included short-term anti-inflammatory prednisone (0.5 mg/kg PO every 24 hours, tapered over 3 weeks), long-term oclacitinib (0.5 mg/kg PO every 12 hours for 2 weeks, then every 24 hours), and monthly lokivetmab injections. Long-term treatment is required to control allergic skin disease. The patient improved after several months of treatment.
Systemic control of environmental allergies with allergen-specific immunotherapy, oral Janus kinase inhibitors (eg, oclacitinib maleate) or anti-interleukin-31 injections (eg, lokivetmab, a monoclonal antibody acting against the cytokine interleukin-31), antihistamines, or corticosteroids are often necessary to control periocular signs. Topical therapy with ophthalmic medication alone is typically limited in efficacy.
Local Drug Reaction Blepharitis

A 4-year-old rat terrier was presented for ulcerated and swollen eyelids ≈6 months after receiving treatment with a compounded ophthalmic formulation of 2% cyclosporine in corn oil for unilateral dry eye in the right eye. An antibiotic–corticosteroid combination eye drop was administered but did not result in improvement. Inflammatory cutaneous drug reaction (ie, drug eruption, contact dermatitis) to the corn oil component of the cyclosporine ophthalmic was thus suspected. Treatment for dry eye was changed to an aqueous-based tacrolimus-containing ophthalmic formulation (tacrolimus 0.03% compounded ophthalmic aqueous solution). Clinical signs improved in 3 to 4 weeks.
Squamous Cell Carcinoma of the Eyelids


Inflammation and ulceration of the eyelid skin or eyelid margins, especially in white or color dilute cats, is a common neoplastic change seen with periocular squamous cell carcinoma, which also occurs in darkly pigmented cats. Differentials include infectious (fungal, bacterial, protozoal, viral) or parasitic blepharitis, immune-mediated blepharitis, local (contact) hypersensitivity, and allergic or atopic dermatitis.
When possible, an incisional biopsy is recommended prior to surgical resection and adjunctive therapy (eg, cryotherapy, local radiation). Surgery that involves resection of >25% of the eyelid margin requires complex blepharoplastic procedures (eg, sliding skin graft [ie, H-plasty], rotational graft, lip-to-lid procedure) to recreate the resected eyelid margin.