Enucleation & Pharmacologic Ciliary Body Ablation of the Eye
Anja Welihozkiy, DVM, DACVO, BluePearl Veterinary Partners, Sarasota, Florida
Although the primary goals in ophthalmology are to preserve vision and maintain a healthy globe, salvage procedures such as enucleation or ciliary body ablation (CBA) may be necessary in some cases.
Enucleation
Enucleation is the most commonly performed orbital surgical procedure in veterinary medicine.1 Globe enucleation is indicated in painful and irreversibly blind eyes with severe ocular pathology. Such pathologies may include intraocular neoplasia unamenable to other forms of surgical and/or medical treatment, uncontrollable endophthalmitis or panophthalmitis, unregulated glaucoma, perforating ocular trauma, and severe ocular trauma with intraocular hemorrhage.1-3 Enucleation may also be indicated in cases in which the owner cannot provide long-term treatment to maintain comfort in a patient with a diseased eye.3
The most common immediate postoperative complications of enucleation are hemorrhage, orbital swelling, hemorrhagic discharge from the wound, and periorbital skin bruising. Cold compresses, pressure bandages, and patient sedation are usually sufficient to control hemorrhage.1 Long-term complications can include draining fistulas that may result from incomplete removal of secretory tissue (eg, conjunctiva with its goblet cells, nictitating membrane gland) and/or the lacrimal caruncle at the medial canthus.1
Ciliary Body Ablation
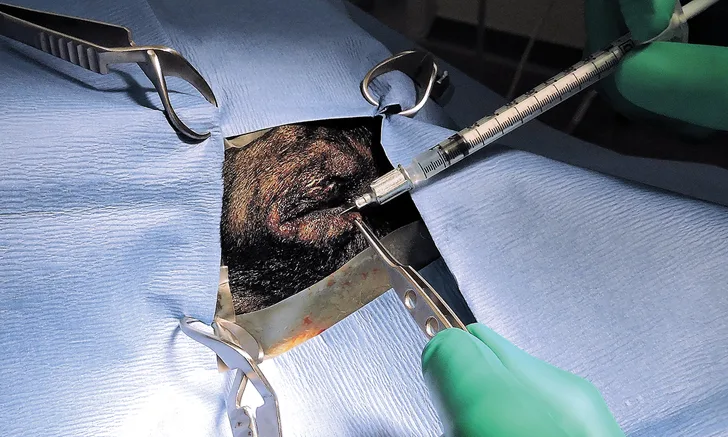
In CBA, the ciliary body is ablated via injection of a cytotoxic drug—most often gentamicin, though cidofovir use has been described in a study4—into the vitreous chamber to eliminate aqueous humor production and achieve low intraocular pressure (IOP) readings.
In contrast to enucleation, a pharmacologic CBA is indicated only to treat and provide comfort in end-stage blind, glaucomatous eyes in cases in which medical and other potential therapies (eg, surgery) for primary glaucoma have failed. CBA is not indicated in cats because of risk for intraocular sarcoma development.5 It is imperative that CBA only be used in dogs with uncontrolled primary glaucoma and in otherwise disease-free eyes.6
A recent study showed a 39.5% likelihood of post-CBA intraocular tumor formation in dogs.6 If tumor formation is detected, subsequent enucleation and histopathologic evaluation should be recommended. It is unclear if gentamicin causes tumor formation or if the injection augments a potential pre-existing intraocular tumor.6 Globe evaluation may have been incomplete in this study (none of the globes underwent ocular ultrasonography); malignant or premalignant processes may have been present before drug injection.6
According to the literature, CBA has an approximate success rate of 65% to 86%.1,7 Cosmetic outcome is variable. All dogs will develop cataracts, the cornea often becomes fibrotic, and phthisis bulbi (ie, shrinking of the globe) will occur at varying degrees. Intraocular hemorrhage is the main immediate complication, and some dogs require long-term treatment for intraocular inflammation. Heavy sedation or short-acting general anesthesia is required.
Evisceration
An evisceration procedure involves removal of all intraocular content through a limbal or scleral incision and replacement with an appropriately sized silicone sphere. Cosmetic results are usually acceptable. The main indication is end-stage primary glaucoma that has become unresponsive to medical or surgical therapy. Globes with intraocular infection or neoplasia are not candidates for a successful evisceration with an intraocular prosthesis procedure.
Step-by-Step: Enucleation
Subconjunctival Enucleation with Intraorbital Prosthesis Placement
With globe enucleation, the eye, eyelid, third eyelid (including lacrimal gland), and conjunctiva are excised. The transpalpebral and lateral approaches to enucleation minimize exposure of the orbit to contaminants of the ocular surface, intraocular infections, and/or neoplasms.1-3 The subconjunctival approach is the simplest, fastest, and most frequently used technique.1-3
What You Will Need
Sterile drapes, gown, and gloves
Extraocular pack with Mayo scissors, tenotomy scissors, Bishop-Harmon forceps, Brown-Adson forceps, enucleation scissors, Derf needle holder, suture scissors, and enucleation scissors (with or without an eyelid speculum)
Sterile orbital prosthesis
Sterile gauze
4-0 or 5-0 absorbable and nonabsorbable suture
Step 1
Clip and prepare the periorbital skin and eyelids for aseptic surgery. Using a diluted aqueous povidone–iodine solution (5%-10%), copiously lavage the conjunctival sac and globe surface.
Author Insights
Povidone–iodine solutions are used in ophthalmologic procedures to avoid corneal and conjunctival ulcerations. In enucleation, it is important to protect the contralateral eye from surface injury.
A preoperative retrobulbar block and eyelid block with a sodium channel blocker may improve intra- and initial perioperative analgesia and decrease the need for initial postoperative rescue analgesia.8

Step 2
After draping the periocular region, perform a lateral canthotomy. (A) Use Mayo scissors to facilitate increased globe exposure, and remove 3 to 5 mm of the inferior and superior eyelid margin. (B) Using Brown-Adson tissue forceps, grasp the nictitating membrane, including its lacrimal gland, then protract and dissect at the base. Blot with gauze sponges and apply digital pressure to control hemorrhage.
Author Insight
Removing the inferior lid before the superior lid is recommended, as doing so can prevent (sometimes moderate) hemorrhaging on the second lid incision.

Step 3
With tenotomy scissors, incise the bulbar conjunctiva and Tenon capsule at the 12 o’clock position approximately 5 mm posterior to the limbus. Using blunt dissection, continue the dissection plane between the sclera and Tenon capsule deeper into the orbit and in the medial and lateral direction to create a 180° to 360° perilimbal incision. Identify and incise the insertions of all extraocular muscles at their tendinous insertions. Avoid incising the muscle bellies, as this can cause unnecessary hemorrhage.

Step 4
After excising all major rectus muscles, displace the globe, which should be more mobile, in the anterior direction. Avoid excessive anterior traction on the globe, as this can cause a reduction in heart rate (ie, oculocardiac reflex), damage to the optic chiasm (particularly in cats and dolichocephalic dogs), and subsequent blindness to the contralateral eye.3
Use enucleation scissors to sever the optic nerve and retractor bulbi muscle close to their scleral attachments. Diffuse, often mild hemorrhage may occur; control this by placing 1 to 2 surgical sponges in the orbit for a short period, then carefully remove them without dislodging initial clot formation.
Author Insights
Ligation of the canine optic nerve is not necessary before globe removal. The nerve does not contain a central retinal vein as described in the human literature.
If hemorrhage continues after a few minutes of digital pressure, a hemostatic agent (eg, gelatin sponges) can be placed in the orbit.

Step 5
Remove the remaining conjunctiva and lacrimal caruncle. (A and B) Inspect the orbit for remaining conjunctival tissue and abnormalities. Close the wound with or without intraorbital prosthesis placement. (C) If needed, use silicone or methyl methacrylate spheres to prevent postoperative skin depression into the orbit. Sphere diameters vary from 12 to 28 mm, depending on orbit size. (D) After placement, the sphere should fit into the orbit without causing excessive pressure on the remaining orbital content.
Author Insight
Contraindications for intraorbital prosthesis placement are bacterial infections and neoplasms in the orbit.1-3

Step 6
(A, B, and C) Close the wound using 4-0 or 5-0 absorbable suture material and a combination of simple interrupted and simple continuous suture patterns. Close the lid incision in a routine fashion using 4-0 to 5-0 nonabsorbable suture. Postoperative analgesia is advised.

Step-by-Step: Ciliary Body Ablation
CBA is performed by injecting a cytotoxic drug into the posterior segment of the globe. The ciliary body (ie, the structure responsible for aqueous humor production) will be destroyed.
What You Will Need
Sterile gloves
Eyelid speculum
Bishop-Harmon forceps
25-g and 30-g needles
1-mL syringe
Tonometer
Step 1
Using a diluted aqueous povidone–iodine solution, aseptically prepare the conjunctival surface and periocular surface.
Step 2
Place an eyelid speculum, and use small forceps to stabilize the globe. Using a 30-g needle, perform an anterior chamber aqueocentesis at the dorsal limbus to decrease preinjection IOP and to allow aqueous humor to exit during the injection.
Author Insight
Care should be taken not to lacerate the iris during needle insertion, as this will likely cause unsightly intraocular hemorrhage. The needle should be inserted in a bevel-up fashion, pointing slightly toward the central cornea.

Step 3
Use a 1-mL syringe with a 25-g needle to inject a combination of 30 to 40 mg of gentamicin and a long-acting steroid (eg, dexamethasone ≤1 mg, triamcinolone ≤2 mg) into the posterior segment (vitreous). Do not exceed the maximum dose (based on the individual patient) of either medication. Alternatively, inject a long-acting steroid subconjunctivally. Insert the needle approximately 6 mm posterior to the limbus and direct it caudally to avoid the lens and the vascular ciliary body.

Step 4
Assess IOP immediately postinjection (target, <15 mm Hg). Remove any additional aqueous humor if IOP is >30 mm Hg. Quickly taper topical antiglaucoma medications.
Follow-Up
Discontinue topical antiglaucoma medications within 2 weeks of the procedure. Use oral anti-inflammatory drugs, additional pain medication, and a topical antibiotic for 1 to 2 weeks postinjection. Measure IOP 2 to 4 weeks postprocedure, once topical antiglaucoma medications have been discontinued.
CBA = ciliary body ablation, IOP = intraocular pressure