Sandy, a 16-year-old neutered male domestic shorthair cat, was presented for routine vaccination. The owner mentioned that the cat was showing signs of aging.
History. Sandy’s behavior at home had changed—he was less active (no hunting outside or jumping on counters) and sleeping more, less sociable with his owners, and had periods where he was urinating indoors.
Physical Examination. Sandy was thin (his weight had decreased from 6.1 kg to 5 kg since last year’s examination), with poor coat condition and some matted hair. He was reluctant to jump on or off the examination table. At rest his elbows were adducted slightly, and he resented flexion and extension of these joints. Clinical examination was otherwise unremarkable; hematology, serum biochemistry, and urinalysis values were within the reference ranges.
Ask Yourself
What is Sandy’s diagnosis and how would you manage the condition?
A. Normal changes with old age—no treatment
B. Osteoarthritis—no treatment necessary
C. Osteoarthritis—manage with nonsteroidal antiinflammatory drugs
D. Osteoarthritis—no treatment possible in cats
Correct Answer
C. Osteoarthritis—manage with nonsteroidal antiinflammatory drugs
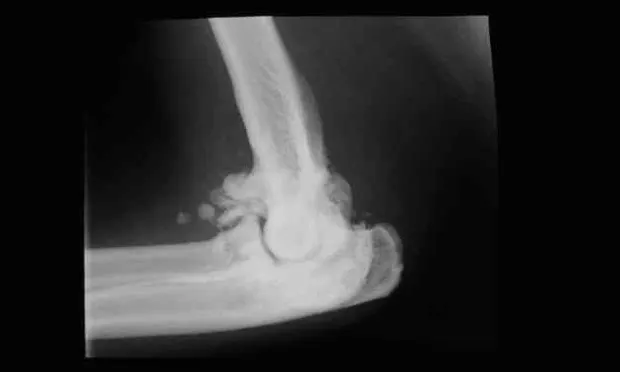
A high percentage of the aging cat population has radiographic or clinical signs of osteoarthritis.1 The elbow and hip appear to be the most affected joints.2 The cat may be stiff and reluctant to move or jump, but lameness is rare. Signs of pain may be difficult to appreciate in cats,3 and signs of chronic pain, such as reduced mobility, reduced activity, difficulty with grooming, and changes in temperament, may often be misinterpreted as signs of aging. Diagnosis is primarily established by history and clinical examination, with or without radiography (Figure 1).
(Figure 1. Osteoarthritis (with osteophytes) in a feline elbow. Courtesy Dr. Martin Owen, University of Bristol)
Treatment. Nonsteroidal antiinflammatory drugs (NSAIDs) are the mainstay of osteoarthritis treatment in both humans and dogs. These agents act by inhibiting the cyclooxygenase isoenzymes (COX-1 and COX-2). Older NSAIDs, such as aspirin, are more COX-1 specific and cause more side effects than the more COX-2–specific, newer NSAIDs. The main side effects are gastrointestinal ulceration and renal tubular damage. Because cats have decreased hepatic metabolism, they have a greater risk for toxicity; nonetheless, NSAIDs can be used in cats if appropriate protocols for dosing and monitoring are followed.4,5
No oral NSAID is licensed for long-term use in cats in the United States; therefore, the owner’s informed consent must be obtained before these drugs can be used. In the United Kingdom, meloxicam is licensed for long-term feline use and is the only NSAID licensed for use longer than 5 days.6 The guide dose is 0.1 mg/kg for the first day, with a maximum of 0.05 mg/kg Q 24 H thereafter. However, doses of 0.01 mg/kg or lower given every second or third day may provide good pain relief. Aiming for the lowest effective dose helps avoid adverse side effects.
Tepoxalin and carprofen have also been used in cats for acute pain management, but a recent review advises against their use for chronic pain management in cats until further safety and toxicity data become available.4
Monitoring. Before initial administration of an NSAID, assess hepatic and renal status and presence of gastrointestinal disease with history, clinical examination, serum biochemical profile, hematology, and urinalysis, plus other tests if indicated (eg, endoscopy of gastric mucosa, examination of feces for blood). Determine concurrent medications, including those owners may administer without prescription (eg, herbal remedies)—some may have adverse interactions with NSAIDs.7
During treatment, monitor for adverse events every 3 to 6 months, using a minimum database of body weight, fasting serum urea level, creatinine level, and urine specific gravity. Side effects are most common in geriatric animals and those with underlying renal or hepatic abnormality. A reduced dose given for extended intervals may be required; however, if major hepatic or renal disease is present, NSAIDs should be avoided.
It is important that owners recognize signs indicating possible toxicity (inappetence, vomiting, diarrhea, lethargy) and understand that they should not increase the dose without consulting their veterinarian.
Other Medications. Opioids (eg, morphine, codeine, buprenorphine, tramadol) are less effective than NSAIDs for chronic inflammatory pain. In severe cases, however, they may be helpful when given in addition to NSAIDs. They may also be beneficial when NSAIDs are contraindicated.
The safety and efficacy of nonopioid drugs used for chronic pain management, such as amantadine and amitriptyline, are unproven for use in feline osteoarthritis; however, they may be useful. In addition, glucosamine hydrochloride, chondroitin sulfate, manganese ascorbate, fatty acids, and acupuncture may also be helpful.
Acetaminophen is highly toxic in cats.
Lifestyle Changes. Lifestyle management, especially weight loss in overweight animals, is important. See the Box for articles on feline nutrition and weight loss.
Take-Home Messages1. Osteoarthritis in cats is a chronic, progressive, and potentially debilitating process that primarily affects older animals.2. Treatment is necessary to ensure good quality of life.3. NSAIDs are the mainstay of drug management, although none is licensed for long-term feline use in the United States.4. Lifestyle management may be beneficial.5. The effectiveness of treatment with other drugs, nutraceuticals, functional foods, or complementary therapies are currently unproven in cats but may be of benefit.
THE CREAKY OLD CAT • Louisa Slingsby
References1. Radiographic evidence of degenerative joint disease in geriatric cats: 100 cases (1994–1997). Hardie EM, Roe SC, Martin FR. JAVMA 220:628-632, 2002.
Feline osteoarthritis: A prospective study of 28 cases. Clarke SP, Bennett D. J Small Anim Pract 47:439-445, 2006.3. Pain management in cats—Past, present and future. Part 1. The cat is unique. Taylor PM, Robertson SA. J Feline Med Surg 6:313, 2004.
Nonsteroidal anti-inflammatory drugs in cats: A review. Lascelles BDX, Court MH, Hardie EM, Robertson SA. Vet Anaesth Analg 34:228-250, 2007.
Managing pain in feline patients. Robertson S. Vet Clin North Am Small Anim Pract 35:129-146, 2005.
Long-term safety, efficacy and palatability of oral meloxicam at 0.01-0.03 mg/kg for treatment of osteoarthritic pain in cats. Gunew MN, Menrath VH, Marshall RD. J Feline Med Surg 10:235-241, 2008.
Potential interactions between non-steroidal anti-inflammatory drugs and other drugs. Trepanier LA. J Vet Emerg Crit Care 15:248-253, 2005.