Cloudy Eye in a Labrador Retriever
Mary Rebecca Telle, DVM, University of Wisconsin-Madison
Gillian J. McLellan, BVMS, PhD, DVOphthal, DECVO, DACVO, MRCVS, University of Wisconsin–Madison
THE CASE
A 7-year-old spayed Labrador retriever crossbreed is presented for a 5-day history of an intermittently red, cloudy left eye. The owner states that the patient had previously been diagnosed with allergic conjunctivitis and has had intermittent flare-ups. The patient has reportedly been coughing for 3 days and, although still eating and drinking, her appetite is decreased. Her BCS is 7/9, which is consistent with previous visits.
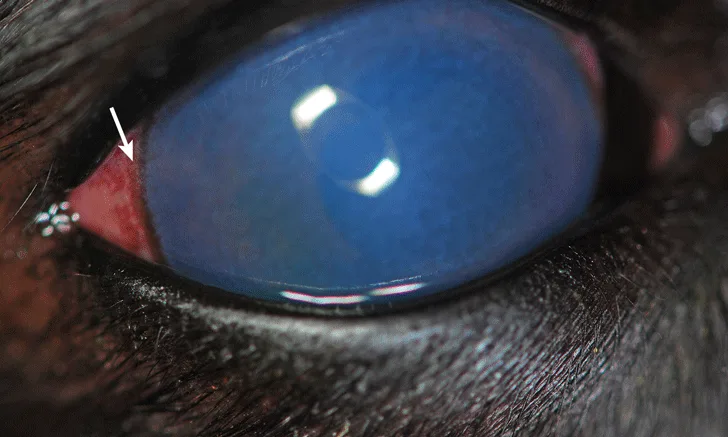
On general physical examination, mild mandibular lymphadenopathy, moderate dental tartar, rectal temperature of 103.8°F (39.9°C), and a tense abdomen on palpation were noted. An initial ophthalmologic examination of the left eye reveals blepharospasm; absent menace response; questionable dazzle reflex; a fixed, mid-range pupil with subtle dyscoria and no apparent direct pupillary light reflex or consensual pupillary light reflex from the left to the right eye; pronounced episcleral injection and conjunctival hyperemia; mild edema, and suspected moderate aqueous flare (Figure 1). Although a tapetal reflex is visible, the fundus in the left eye cannot be visualized by indirect or direct ophthalmoscopy. The right eye appears normal.


The affected eye showing (A) pronounced conjunctival hyperemia (arrow) and moderate-to-severe corneal edema, as well as (B) episcleral injection (arrow) and a mid-sized pupil with slight dyscoria (arrowheads)
What are your next steps?
Conclusion
This case highlights the challenge of determining whether glaucoma is primary or secondary, especially if owners are financially constrained or unable to accept referral. In addition, many cases of PACG exhibit a degree of inflammation and pigment dispersion, which can further complicate the clinical picture. This case illustrates the importance of recognizing that primary glaucoma may be encountered in any breed, including crossbreed dogs.
IOP = intraocular pressure, PACG = primary angle closure glaucoma, STT = Schirmer tear test