Chronic Superficial Keratitis in Dogs
Anja Welihozkiy, DVM, DACVO, BluePearl Veterinary Partners, Sarasota, Florida
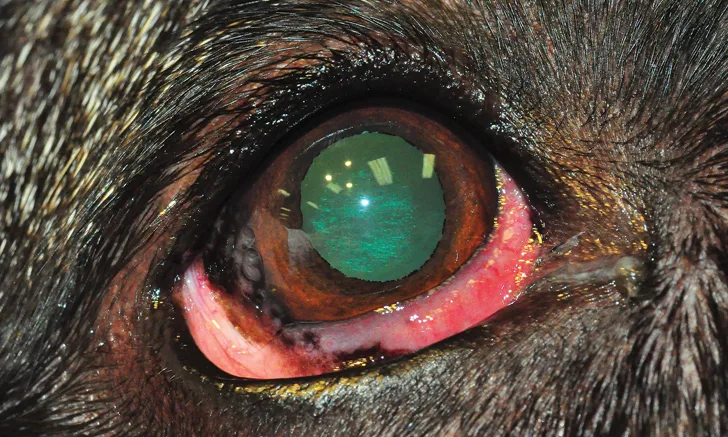
Chronic superficial keratitis (CSK)—also known as German shepherd pannus, Überreiter’s syndrome, or degenerative pannus—is a progressive, usually bilateral, and potentially vision-threatening disease of the canine cornea.1,2 It is characterized by chronic inflammation of the corneal epithelium and anterior stroma, which results in neovascularization, pigmentation, and opacification.1 Atypical pannus (ie, plasmoma), an inflammatory process of the nictitating membrane, has also been described.2
Clinical History & Signalment
Large breeds—in particular German shepherd dogs, shepherd crossbreeds, border collies, and greyhounds—are predominantly affected; however, CSK can occur in dogs of any size and breed.2 Age of onset is an important prognostic indicator. The condition typically progresses rapidly in young dogs (ie, 1-5 years of age); lesions may be less severe in animals affected later in life (ie, >4-5 years of age).2


Left eye of a 9-year-old neutered male German shepherd dog. Thickened nictitans (ie, plasmoma) and lateral corneal infiltration can be visualized (A). Right eye of the same dog; nictitans swelling and lateral invasion of cornea can be noted (B). Photos courtesy of Tammy Miller Michau, DVM, MS, MSpVM
Physical Examination Findings
CSK manifests initially at the temporal or inferior temporal limbus as a hyperemic, vascularized conjunctival lesion.2 Early changes in the cornea are characterized by limbal neovascularization and pigmentation, which advance centrally as the disease course continues.2 Chronic tissue changes are characterized by progressing moderate-to-severe corneal neovascularization, with infiltration of fleshy granulation tissue into the anterior stroma and proliferation of limbal melanocytic pigment invasion (Figure 1).2,3 Lipid infiltrates may also be noted in the clear cornea 1 to 2 mm in front of the leading edge of the lesion.2
As the disease advances, neovascularization often begins at the temporal limbus and extends centrally (Figure 2).2 The dorsal limbus is only involved late in the disease process; however, the entire cornea may eventually become vascularized, pigmented, and opaque, which can lead to visual impairment.2,4,5

Eye of a 6-year-old spayed German shepherd dog. Diffuse corneal infiltration can be noted. Photo courtesy of Tammy Miller Michau, DVM, MS, MSpVM
Histopathologic Diagnosis & Pathogenesis
The clinical lesion is histopathologically characterized by fibrovascular tissue in the corneal stroma that is accompanied by lymphocytes and plasma cells as well as migration of limbal pigmented cells.2 Infiltrating CD4+ lymphocytes are the predominant cells found in patients with CSK, which suggests that CSK has an immune-mediated pathogenesis.1
An increase in major histocompatibility complex class II antigen expression has been identified in the central corneal epithelium and stroma in dogs with CSK and is indicative of an autoimmune nature of the disease.6 In another study, an identified major histocompatibility complex class II risk haplotype was found to be strongly associated with chronic CSK in German shepherd dogs; animals with the risk haplotype were 2.7 times more likely to develop CSK, and animals that were homozygous for this specific haplotype were 8 times more likely. This further suggests that CSK is an immune-mediated disease with a genetic basis.7
High altitude and increased exposure to sunlight appear to intensify clinical signs in dogs that may have a genetic predisposition for developing CSK, as ultraviolet radiation may modify cornea-specific antigens, which initiate the cell-mediated inflammation.3,8
Clinical Diagnosis
In most cases, signalment and clinical appearance of the corneal lesions are sufficient for CSK diagnosis. However, major differential diagnoses can include pigmentary keratitis, keratoconjunctivitis sicca, chronic irritation, and/or chronic granulation tissue from previous corneal wounds.2
Treatment & Long-Term Management
CSK can generally be controlled through medical or surgical means (see Treatment at a Glance), but it cannot be cured. A standard treatment protocol has not been established, and the goal for all described therapies is to stall disease progression.2,8,9 Owners should be advised that lifelong therapy is necessary and that disease severity and prognosis are also dependent on factors such as age of onset, altitude, sun exposure, and genetic predisposition.2,8
Treatment at a Glance
Mild-to-Moderate Cases2
Long-term topical cyclosporine (0.2%-2% q12h) or tacrolimus (0.02%-0.03% q12h)
With or without an additional topical corticosteroid (eg, dexamethasone [0.1%], prednisolone acetate [1%] q6-8h) slowly tapered over few weeks to months2
Moderate-to-Severe Cases2,4,10
Topical medications as for mild-to-moderate cases; consider higher frequencies
Subconjunctival corticosteroid injections
Advanced treatments with strontium-90, soft x-rays (15 kV), and/or keratectomy
Long-term control of mild-to-moderate cases can often be managed with topical therapy (ie, cyclosporine [0.2%-2% q12h] or tacrolimus [0.02%-0.03% q12h] with or without an additional corticosteroid [eg, dexamethasone 0.1%, prednisolone acetate 1%]). The topical corticosteroid should be started at a higher frequency based on the individual case and case severity, then slowly tapered over time.2 One study demonstrated that topical pimecrolimus (1% q8h) may be an effective therapy for moderate-to-total regression of CSK lesions.5
For patients with an insufficient or delayed response to topical medication, subconjunctival corticosteroid injections may be necessary to control disease. Patients treated with long-term topical anti-inflammatory drugs should be monitored closely by the owner for signs of ocular discomfort, discharge, redness, and behavior changes and regularly examined by a veterinarian (ie, complete ophthalmic examination) to prevent corneal ulcerations or corneal infections.
Beta irradiation with strontium-90 2,10 and radiation therapy with soft x-rays (15 kV)4 have been described as safe and effective forms of treatment in patients that have severe CSK unresponsive to medical therapy (ie, drop application and subconjunctival injections) alone.
In patients with severe CSK that are unresponsive to medical therapy—and, where available, radiation therapy—surgical intervention may be considered. Superficial keratectomy may be required for patients with blinding disease; however, opacification recurrence should be expected. All of the treatment methods described (ie, medical therapy as well as radiation) should be considered following a keratectomy to prevent or delay recurrence.2
Making husbandry changes such as canine protective eye wear and limiting sun exposure during high UV radiation times should be considered, as ultraviolet-blocking contact lenses have not been shown to be successful or advantageous in CSK treatment.9
Conclusion
CSK is an immune-mediated disease process that can be challenging to treat and cannot be cured; delay of disease progression or stabilization of the corneal pathology should be considered a therapeutic success.9 A standard protocol has not been determined, but lifelong therapy is required.9
Take-Home Messages
CSK is an immune-mediated disease that likely has a genetic basis.7
German shepherd dogs, border collies, and greyhounds appear to be predisposed.2
CSK can be a potentially blinding disease in severe cases.2
Onset usually occurs at 3 to 5 years of age but may occur at any age. CSK can be more difficult to control in dogs affected at a young age.2
UV-light exposure and high altitude may contribute to disease severity.3,8
Lifelong therapy with immunosuppressive and immunomodulating agents is required.2