Chronic Pruritus in a Household of Cats
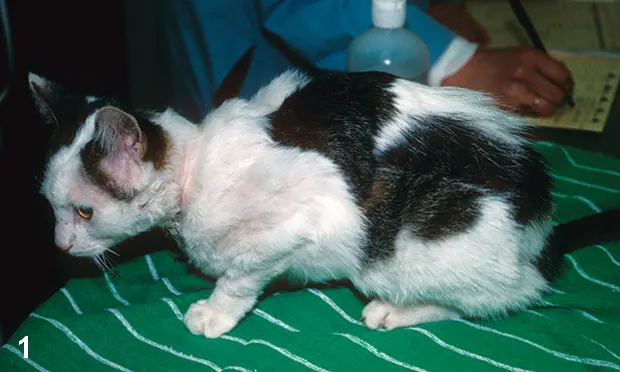
Ed, a 9-month-old, castrated, domestic short-haired cat, was presented for evaluation of chronic pruritus of 3 months’ duration.
History
Ed’s owner, involved in breeding and showing Devon rex cats, had 7 intact female cats between 1 and 8 years of age. All cats lived indoors and never left home except for shows or breeding. All were mildly to severely pruritic; Ed was the most severely affected (Figure 1).
Vaccination status was current, but flea control was not used (to avoid potential focal hair loss). The owner did not report any skin lesions on her own body but did mention that pruritus had developed in all cats about 4 weeks after Ed had been adopted at a cat show at 5 months of age; Ed and the 2 cats present at a show had been kept separate for 10 days to ensure none had contracted an upper respiratory infection. The owner reported that all cats had GI complications (eg, constipation, hairballs) and was concerned they had a food allergy; she provided a fecal specimen from a community litter box for testing.
Physical Examination
Except for a large colon filled with fecal material, Ed’s physical abnormalities were strictly dermatologic. Palpation of the dorsal aspect of the hair coat revealed stubbly hairs compatible with barbering. Patchy hair loss was present on the lateral thorax, along with a large focal area of apparently noninflammatory alopecia on the ventral abdomen; close inspection revealed follicular plugging. Excessive scaling was present throughout. The owner indicated that the other cats’ dermatologic signs mostly resembled Ed’s.
Related Article: Diagnosis of Demodicosis in Dogs & Cats
Laboratory Testing
Fecal flotation was conducted on the litter box sample

(Figure 2); mites were evident.
ASK YOURSELF...Based on fecal flotation findings, what is the best diagnostic recommendation?A. Treat Ed for mites and, if there is a positive response, treat the other cats.B. Conduct a Wood’s lamp examination and fungal culture on Ed, and pending those results, initiate treatment.C. Conduct a Wood’s lamp examination and fungal culture on Ed, and initiate treatment.D. Conduct a Wood’s lamp examination and fungal culture on Ed, and initiate treatment for Ed and the other cats after they have been examined.
Correct Answer:D. Conduct a Wood’s lamp examination and fungal culture on Ed, and initiate treatment for Ed and the other cats after they have been examined.
Related Article: Treatment of Demodicosis in Dogs & Cats
Findings & Diagnostic Implications
The fecal flotation showed several Demodex gatoi mites. Unlike other Demodex spp mites in cats and dogs, this mite is highly contagious, and the hallmark clinical sign is pruritus.1,2 D gatoi mites can be difficult to find for many reasons:
Small, translucent mites can be overlooked on a skin scraping.
Mites may not be prevalent where the cat is grooming, possibly explaining why mites are found on fecal flotation and not on skin scrapings; hair pluckings from difficult-to-groom areas may prove more fruitful.
Because pruritus is presumably a hypersensitivity reaction, even a few mites can cause intense pruritus.
There are several major causes of pruritus in cats (eg, parasites, infections, allergies). In a survey of more than 500 cats with chronic pruritus, the most common cause was flea allergy dermatitis.3 The second most common causes included feline demodicosis and dermatophytosis, emphasizing the need to perform response-to-treatment trials in cats with chronic pruritus and conduct core diagnostics (eg, skin scrapings, hair pluckings, flea combings, fungal culture) to rule in or out other causes. Of the survey cats diagnosed with allergic skin disease, approximately 12% had food allergy.3 That Ed and his housemates all had pruritus from food hypersensitivity is unlikely; the GI signs are likely secondary to pruritus and overgrooming.
Outcome
The history, timeline, and owner description were highly indicative of contagious disease—in this case, feline demodicosis from D gatoi infestation. Recommendations for contagious skin diseases include treating all in-contact animals. Also, the remaining 7 cats should all be examined before treatment to ensure that no complicating medical problems will make a one-size-fits-all treatment inappropriate, to obtain accurate body weights, and to corroborate that all cats are similarly affected. Legal issues regarding examination of the other cats are self-evident.
All the cats were treated with lime sulfur q1wk for 6 weeks. The owner reported a noticeable decrease in pruritus after 1 week.
Recommended Diagnostics
Excluding the feline dermatology mantra that “it is ringworm until proven otherwise,” this case presented two reasons to conduct a Wood’s lamp examination and fungal culture: lesions developed after introduction of a kitten into the household and after reintroduction of two cats that had been at a show; both are common opportunities for introduction of contagious diseases.
Although fungal culture is definitive, a Wood’s lamp examination may reveal positive fluorescence with direct examination, confirming the diagnosis (or possibly revealing multiple diagnoses). Wood’s lamp examinations are usually inexpensive and can be performed on all cats at examination.
Arguably, all cats should have a sample cultivated for fungal infection; however, after 3 months of cohabitation, fungal culture of a sample from Ed will likely be representative. Examination of the other cats and owner constraints can help determine the need for additional cultivation; if treatment fails, this can be revisited. Starting lime sulfur treatment while waiting for culture results can be beneficial.
The Take-Home
D gatoi (a short, blunted mite) infestation is a common differential for any cat with chronic pruritus, especially cats with symmetric alopecia. Mite infestation should be ruled out by response-to-treatment trial before allergy testing or food trial is pursued.
This species is highly contagious and should be suspected in cats that are at risk or in households with multiple pruritic cats.
Infestations are often diagnosed via response-to-treatment trials.
Another well described species of mites in cats is D cati (long and slender).
D cati is not contagious and is usually associated with other medical problems (eg, diabetes mellitus, immunosuppression, excessive glucocorticoid use).
Presence of this mite should prompt examination for underlying illness.
A third morphologically distinct mite (longer than D gatoi but shorter and wider than D cati) has been described in cats.4-6 Determining whether this is a new species will require molecular testing. It has been seen in association with D cati and D gatoi infestations and underlying illnesses.
KAREN MORIELLO, DVM DACVD, is clinical professor of veterinary dermatology at University of Wisconsin–Madison and coeditor of the Journal of Veterinary Dermatology. Her clinical research interests include contagious skin diseases, particularly feline dermatophytosis. Dr. Moriello received the 2005 American College of Veterinary Dermatology Award for Excellence for outstanding contributions to service and education and the 2006 Ida Kittleson Award from the Dane County Humane Society for her time and energy contributions in the care of shelter animals with skin disease. She earned her degree from University of Illinois.