Chronic Progressive Weakness in an Older Dog
A 7-year-old, 38.6-kg, castrated Doberman pinscher was presented with a 3-month history of progressive pelvic limb weakness.
History
Figure 1. Neck position suggestive of discomfort.

The owners reported that the dog appeared uncoordinated and was stumbling on both pelvic limbs. The dog held its neck slightly lower than normal (Figure 1), but the owners did not think the dog was in pain.
One year earlier, the dog had undergone a staged bilateral tibial plateau leveling osteotomy for bilateral pelvic limb lameness caused by cranial cruciate ligament disease. Recovery had been uneventful. Vaccinations were current, and the dog appeared otherwise healthy.
Related Article: Weakness & Exercise Intolerance in a Dog
Physical Examination
The dog was alert and responsive and was not dehydrated. At normal stance, however, the pelvic limbs became more crouched with time. The dog had good overall muscle tone, but muscle mass was decreased over the scapulae bilaterally. The nails on both pelvic limbs appeared abnormally worn, with dorsal digital excoriation more prominent on the left. A medial buttress was noted on palpation of the stifle in both pelvic limbs.
Gait analysis disclosed a long stride in the pelvic limbs and a short, choppy stride in the thoracic limbs. The pelvic limbs crossed over when the dog turned, and the left pelvic limb occasionally scuffed the ground on the cranial aspect.
Marked delay in return of the pelvic limbs to normal position was noted when the digits were turned over while supporting the dog’s weight, suggestive of proprioceptive dysfunction. No proprioceptive abnormalities were noted in the thoracic limbs.
Hopping was slow in both pelvic limbs; a localized tremor and decreased weight bearing, especially on the left side, were noted when the test was performed on the thoracic limbs. No cranial nerve deficits were present.
Related Article: Intervertebral Disk Herniation
Withdrawal reflexes were decreased in the pelvic limbs. Thoracic limb reflexes appeared intact, but patellar reflexes were difficult to elicit. The dog resisted lateral neck flexion in both directions, and dorsal neck flexion caused the dog to sit down and vocalize abruptly. Palpation of the thoracolumbar spine did not elicit a painful response.
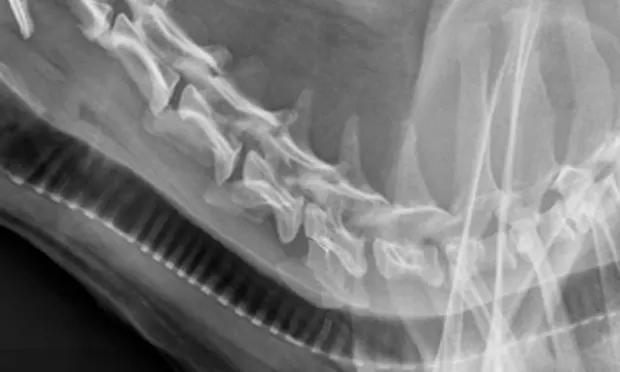
Figure 2. Lateral cervical radiograph demonstrating a collapsed disk space at C5-C6 (arrow).

Diagnostics
CBC, serum biochemistry profile, and urinalysis results were within reference ranges. Thoracic and abdominal radiography disclosed no abnormalities. Radiographs of the cervical spine showed normal vertebral bone densities and soft tissue structures. The C5-C6 intervertebral disk space appeared narrow with some opacity within the canal (Figure 2).
MRI of the cervical spine disclosed dorsal and ventral compression of the spinal cord at the level of the C5-C6 disk space (Figure 3).
Figure 3. Sagittal cervical spinal MRI showing dorsal and ventral compression of the spinal cord at the C5-C6 disk space.

ASK YOURSELF...
Based on neurologic-examination findings, where would the neurologic lesion be localized?
What differentials are consistent with lesion localization in this dog?
What could survey radiography of the spinal column disclose about these diagnoses?
Based on MRI results and the dog’s current neurologic status, what treatment(s) would be indicated?
Diagnosis
Disk-associated cervical spondylomyelopathy (wobbler syndrome)
Preliminary Diagnosis
The MRI results were consistent with dorsal and ventral compression resulting from disk-associated wobbler syndrome. In addition to a chronic type-2 disk herniation or protrusion, there was dorsal compression resulting from the dorsal vertebral laminae and hypertrophy of the interarcuate ligament. Disk disease was noted on MRI based on the decreased intensity of the C5-C6 and C6-C7 disks, indicating loss of water content.
Treatment
For 6 weeks, the dog had strict at-home rest (cage rest when the owners were absent). Prednisone at 0.5 mg/kg PO q12h was prescribed for 7 days at a tapering dose. The owners were instructed that if the dog needed to be walked, a body harness should be used rather than a neck collar and leash.
Outcome
Follow-up examinations at 2 and 6 weeks showed increased pelvic limb strength. The dog held its head higher and appeared more comfortable. A mild gait deficit was still present in all limbs, but coordination was improved. At 3 months, the dog continued to improve, but its level of activity was more restricted than before onset of signs.
DID YOU ANSWER?
The lesion was localized to the caudal cervical spinal cord, more specifically to the C6-T2 spinal cord segments. The C6-T2 segments give rise to the radial, median, and ulnar nerves of the brachial plexus; disease of these segments can give rise to reduced thoracic limb reflexes and severe neurogenic atrophy of the major muscle groups. The dog was tetraparetic, despite pronounced weakness in the pelvic limbs. This can be common in large-breed dogs, as the spinal cord pathways to the pelvic limbs are more superficially located than the thoracic limb pathways; compressive lesions affecting the cervical cord can sometimes cause pelvic limb signs to be apparent first. The dog had decreased withdrawal reflexes, proximal muscle atrophy, and decreased stride length in the pelvic limbs, which is consistent with a lower motor neuron lesion (C6-T2 spinal cord). The thoracic limbs had intact reflexes and increased stride length, which are consistent with an upper motor neuron lesion (cranial to L4). The patellar reflexes could not be assessed appropriately because of previous cruciate surgeries and associated osteoarthritis.
The differential diagnosis for this lesion localization in an older large-breed dog with chronic progressive signs includes type-2 disk disease (chronic disk protrusion), cervical spondylomyelopathy (wobbler syndrome), diskospondylitis, infectious or sterile meningomyelitis, and vertebral or spinal cord neoplasia. Trauma would not be a consideration, as this dog had a chronic progressive history, which would also rule out fibrocartilaginous embolic myelopathy.
Survey radiography of the cervical spine would assist diskospondylitis evaluation, which would appear as lysis of the end plates adjacent to the affected disk space. Vertebral neoplasia can sometimes be identified by the presence of associated lysis; however, ≥50% of the bone structure would need to be affected for this lysis to be visible. Narrowed disk spaces, narrowing and opacity of the intervertebral foramen, and mineralized material in the vertebral canal may suggest disk disease diagnosis. Although changes in the shape of cervical vertebrae (ie, more triangular) are compatible with wobbler syndrome, this is not a sensitive finding.<sup1sup>
Medical treatment can be successful in up to 50% of cases, especially if the dog is ambulatory at assessment.1-5 However, ≥20% of patients may continue to deteriorate neurologically when treated conservatively.4 One study indicated that ≤62% of patients treated in this manner can do poorly and require euthanasia.6 Treatment may include strict rest and short-term anti-inflammatory medications (analgesics if necessary). If the dog shows improvement after 6 weeks of strict rest, slow introduction back to a long-term reduced and controlled exercise regimen is advised. Neck collars and leashes should be avoided. If the dog fails to respond to this therapy or is more severely affected initially, surgery should be considered; the specific surgical technique can vary depending on surgeon’s preference and specific abnormalities evident on imaging.7,8 Approximately 80% of dogs improved with surgery.7 Recurrence and surgical morbidity can be concerns.7
SIMON R. PLATT, BVM&S, MRCVS, DACVIM (Neurology), DECVN, is professor of neurology at University of Georgia. Dr. Platt is president of the ACVIM neurology specialty and coeditor of BSAVA Manual of Canine & Feline Neurology and Manual of Small Animal Neurological Emergencies. He completed an internship in small animal medicine and surgery at University of Guelph and a residency in neurology and neurosurgery at University of Florida. He earned his veterinary degree from University of Edinburgh.