Canine Perioral Dermatitis
Jennifer Schissler, DVM, MS, DACVD, Colorado State University
Profile
Definition
Perioral dermatitis (PD) is inflammation of the maxillary or mandibular cutaneous or mucocutaneous tissues.
PD has diverse clinical presentations and causes and may be noted as a singular clinical entity or among generalized dermatologic or systemic signs.
Systems
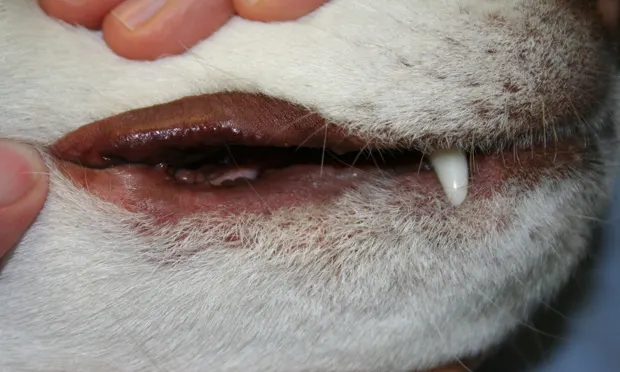
PD is not limited to lip fold intertrigo (ie, bacterial and Malassezia spp overgrowth; Figure 1); rather, it is a potential manifestation of focal or generalized cutaneous conditions.
Conditions include hypersensitivities, immune-mediated dermatopathy, infection, hepatopathy, periodontal disease, and neoplasia.

Lip fold intertrigo in a dog
Signalment & Causes
See Handout: Causes of Perioral Dermatitis for causes and presentations.
Some causes have known breed and age associations.
Risk Factors
Redundant lip folds can predispose patients to intertrigo.
Any primary cause of PD poses risk for secondary bacterial or Malassezia spp infection.
Chronic use of topical or systemic glucocorticoids poses risk for demodicosis.
Sun exposure can pose a risk for pemphigus foliaceus and discoid lupus erythematosus (Figure 2).

Discoid lupus erythematosus in a dog
Pathophysiology
Cutaneous or mucocutaneous inflammation can occur from causes that prompt erythema, pruritus, and primary lesions (eg, papules, pustules, vesicles, bullae), followed by secondary lesions (eg, erosions, ulcerations, crusts, alopecia).
The resulting skin barrier disruption predisposes patients to secondary bacterial and Malassezia spp overgrowth.
The microenvironment of a deep, redundant lip fold predisposes patients to intertrigo.
Severe periodontal disease with ptyalism may predispose to secondary perioral infection, particularly with deep lip folds.
Pruritus and malodor are common.
History
Signalment and clinical signs should be noted and history recorded:
Degree, location, and seasonality of pruritus
Duration and progression of lesions
Previous treatments and response
Dietary history
Physical Examination
Cutaneous examination (eg, of the footpads, interdigital spaces, and nasal planum) should be completed.
Otoscopic and ophthalmic examinations should be performed.
The oral cavity, mucous membranes, and mucocutaneous junctions should be examined.
Lymphadenopathy should be assessed and lymph nodes palpated.
Diagnosis
Definitive Diagnosis
Definitive diagnosis is achieved via history, examination, and appropriate diagnostics.
Secondary infections should be resolved, as they can confound clinical and histopathologic features of the primary cause.
Histopathology is required for diagnosis of immune-mediated disease, superficial necrolytic dermatitis, zinc-responsive dermatitis (Figure 3), and cutaneous epitheliotropic lymphoma (Figure 4).
Patients with nonseasonal perioral pruritus may require an 8-week prescription or home-cooked elimination diet to differentiate atopic dermatitis (Figure 5) from cutaneous adverse food reaction (CAFR).

Zinc-responsive dermatitis in a dog



Cutaneous epitheliotropic lymphoma in various canine patients

Atopic lip fold dermatitis with cheilitis and secondary Staphylococcus spp infection
Cytology
Acetate tape preparation (only for dry lesions) and impression smear of exudates should be performed to assess for bacteria, Malassezia spp, and presence of acantholytic keratinocytes.
Fine-Needle Aspiration
Nodules and enlarged lymph nodes should be aspirated.
Deep Skin Scrape
Deep skin scrape or pluck for Demodex spp (Figure 6) should be performed in all cases.
If patient compliance impedes the performance of a deep skin scrape, several representative areas (~100 hairs per sample) can be plucked and examined with mineral oil and a coverslip.1

Perioral and facial demodicosis in a dog
Cultures
Dermatophyte culture is indicated if lesions are consistent (see Handout: Causes of Perioral Dermatitis) and secondary infection and Demodex spp have been ruled out.
Bacterial culture is indicated if clinical and cytologic response to antimicrobial therapy is lacking.
Culture nodular or ulcerative lesions if bacteria are found on cytology; culture superficial lesions if intracellular rods are found.
Elimination Diet Trial
A strict novel or hydrolyzed diet or home-cooked novel diet should be prescribed for a minimum of 8 weeks to differentiate CAFR from nonseasonal atopic dermatitis.
Diet should be rechallenged to confirm the diagnosis.
Histopathology
Vesiculobullous presentations (Figure 7) and lesions that remain after resolution of secondary infection should undergo biopsy.
Multiple lesions representing all stages of disease should be sampled.

Mucous membrane pemphigoid in a dog
Additional Diagnostics
Serum biochemistry profile and abdominal ultrasonography are recommended to support diagnosis of superficial necrolytic dermatitis.
CBC, serum biochemistry profile, fecal flotation, and urinalysis are recommended in cases of adult-onset generalized demodicosis to screen for underlying systemic disease.
Treatment
Lip Fold Intertrigo
Daily use of topical antiseptic and drying agents should be initiated.
2% acetic acid, 2% boric acid, and antimicrobial-based wipes and solutions are appropriate for maintenance therapy.
Acid- and alcohol-based topical medications are not recommended for erosive or ulcerative lesions.
If erosions, ulcers, crusts, nodules, or depigmentation are present, systemic antimicrobial therapy is indicated (see Bacterial Infection & Mucocutaneous Pyoderma).
Cheiloplasty is curative in patients that have lip fold intertrigo (with no other underlying cause) and are refractory to maintenance therapy.
Bacterial Infection & Mucocutaneous Pyoderma
Topical therapy is recommended in all cases.
Systemic antimicrobial therapy is recommended for erosive or ulcerative, crusting, and depigmentation presentations.
If cocci are found on cytology, appropriate empirical choices include:
Clindamycin at 11 mg/kg PO q12–24h
Cephalexin at 22–30 mg/kg PO q12h
Cefpodoxime at 5–10 mg/kg PO q24h
Cefovecin at 8 mg/kg SC q14d up to 2–3 times
Amoxicillin–clavulanate at 13.75 mg/kg PO q12h
Solutions and wipes containing 2% acetic acid, 2% boric acid, or 2%–4% chlorhexidine may be used daily and maintained q3–7d after resolution.
Avoid acid or alcohol-containing products if erosions are present.
Shampoos containing 2.5% benzoyl peroxide or 2%–4% chlorhexidine may be used 2–3 times weekly.
For mixed infections and ulcerative lesions, silver sulfadiazine cream should be considered.
Mupirocin ointment is most appropriate for methicillin-resistant Staphylococcus spp infections.
Malassezia spp Infection
These infections should be treated topically.
Solutions and wipes containing 2% acetic acid, 2% boric acid, 2%–4% chlorhexidine, 2% miconazole, or 1%–2% ketoconazole may be used q24–48h until resolved, then maintained 1–2 times weekly.
Focal, dry presentations should be treated with daily applications of ointments with 1% clotrimazole, 1%–2% miconazole, 1% terbinafine, 4% thiabendazole, or nystatin.
Shampoos with 1%–2% ketoconazole, 2% miconazole, 2%–4% chlorhexidine, or 2.5% benzoyl peroxide may be used 2–3 times weekly.
Adjunct systemic therapy for generalized or severe multifocal presentations should be initiated:
Ketoconazole at 5–10 mg/kg PO q24h
Itraconazole at 5–10 mg/kg PO q24h
Fluconazole at 10 mg/kg PO q24h
Terbinafine at 30 mg/kg PO q24h
Dermatophytosis
These infections should be treated systemically and topically (see Malassezia spp Infection).
Lime sulfur may be used for generalized presentations.
Immune-Mediated Conditions*
Mild focal presentations may be managed with 0.1% topical tacrolimus (Protopic) and/or doxycycline and niacinamide.
Typically severe presentations initially require prednisolone at 2 mg/kg q24h.
A secondary immunomodulator may be administered as a steroid-sparing agent or to achieve remission.
Immunomodulating agents include azathioprine, cyclosporine A, mycophenolate, and chlorambucil.
Diagnosis, condition severity, and potential adverse effects will influence treatment choices.
Juvenile cellulitis (Figure 8) is treated with prednisolone as sole therapy.
For mild cutaneous drug eruptions, discontinuation of the drug alone may be sufficient.

Juvenile cellulitis in a dog
Vitiligo
No treatment is required or reliably effective.
Focal Demodicosis
Treatment is not recommended; lesions are expected to resolve within 4–8 weeks.
Generalized Demodicosis
Treatment options include:
Amitraz dips q14d
Ivermectin at 0.3–0.6 mg/kg PO q24h
Milbemycin oxime at 1–2 mg/kg PO q24h
Doramectin at 0.6 mg/kg PO or SC q7d2
Topical 10% imidacloprid and 2.5% moxidectin q7–14d3 (off label)
Epitheliotropic Lymphoma*
Therapies include prednisolone as well as oral, injectable, and topical chemotherapeutic agents.
Consultation with a veterinary oncologist is recommended.
Superficial Necrolytic Dermatitis
Treatment includes topical antimicrobial therapy and IV and/or oral amino acid supplementation to manage dermatologic lesions.
Hepatopathy is treated symptomatically, and surgery or octreotide may be considered for pancreatic glucagonoma.4
Prognosis for survival is poor to grave.
Zinc-Responsive Dermatosis
Lifelong supplementation with zinc gluconate at 5 mg/kg PO q24h, zinc sulfate at 10–15 mg/kg PO q24h, or zinc methionine at 1.7 mg/kg PO q24h is required; additional topical or oral glucocorticoid therapy may be needed.
Hypersensitivity
CAFR is controlled via restrictive diet.
Treatment options for atopic dermatitis include but are not limited to:
Immunotherapy
Cyclosporine A
Antihistamines
Fatty acids
Adjunct topical antiinflammatory and/or antimicrobial therapy
Follow-Up
Requirements depend on cause.
For infections, recheck clinical and cytologic response in 2–3 weeks to ensure topical and/or oral therapy is effective.
In General
Relative Cost
Cost can vary.
Lip fold intertrigo (diagnosis and treatment): $–$$
Cheiloplasty for lip fold intertrigo: $$$$
Zinc-responsive dermatosis (diagnosis and management): $$–$$$
Generalized demodicosis management: $$–$$$$
Immune-mediated disease (diagnosis and management): $$$–$$$$$
Superficial necrolytic dermatitis (diagnosis and management): $$$$–$$$$$
Cost Key
$ = <$100
$$ = $100-$250
$$$ = $250-$500
$$$$ = $500-$1,000
$$$$$ = >$1,000
(Actual costs will have regional variations)
*A complete discussion of therapy is beyond the scope of this text.