Canine Obesity-A Treatable Condition
Sherry Lynn Sanderson, DVM, PhD, DACVIM, DACVN, University of Georgia

Obesity remains the most common nutritional health problem in dogs. Adipose tissue was long considered metabolically inert, and its primary role in disease was attributed to stress on the joints and increased workload on the heart. However, the understanding of how obesity contributes to health problems has recently grown. Adipose tissue is now known to be metabolically active and is a major endocrine organ in the body. In addition to secreting hormones, adipose tissue produces protein signals and factors called adipokines, and many adipokines are linked to inflammation and the inflammatory response.1-5 Thus, obesity is considered a chronic inflammatory disease, and many obesity-related risks can be attributed to this inflammatory state.
Profile
Definitions
Obesity is the excessive accumulation of adipose tissue and occurs when dogs are > 20% above ideal weight. Dogs 10% to 20% above ideal weight are considered overweight.
Genetic Implications. Obesity genes have not been found in dogs, but a genetic component to obesity in certain breeds is likely.
Incidence/Prevalence. The number of overweight or obese dogs in the U.S. has reached epidemic proportions. An estimated 24% to 44% of U.S. dogs are overweight or obese, and about 50% of dogs age 5 to 10 years are overweight or obese.
Signalment
Breed Predilection. Some breeds are predisposed to obesity, including Labrador retrievers, miniature schnauzers, dachshunds, shelties, cocker spaniels, beagles, basset hounds, and Cairn terriers.
Gender. Obesity is more common in females than males, and neutered females are almost twice as likely to be overweight or obese as intact female dogs.
Risk Factors
The most common risk factor for obesity is overeating and lack of adequate exercise.
Age: Metabolic rate decreases as a dog ages; lean muscle mass decreases and fat mass increases.
Neutering: Gonadectomy increases the incidence of obesity in dogs.
Endocrine disorders: Hypothyroidism and hyperadrenocorticism are the most common endocrine causes of obesity in dogs.
Drugs: Corticosteroids and phenobarbital increase appetite.
Pathophysiology
Obesity is characterized by chronic inflammation; inflammation increases as adipose tissue expands.
Adipose tissue is a major endocrine organ that produces hormones and protein factors and signals called adipokines. The expression, production, and release of adipokines increases with obesity:1-5,6
Cytokine-like adipokines-leptin & adipsin:
In normal individuals, leptin triggers the hypothalamus to decrease appetite and reduce food intake and stimulates diet-induced thermogenesis.
Obese individuals can become leptin resistant (leptin is no longer effective at downregulating food intake or increasing metabolic energy expenditure).
Leptin is elevated in obese dogs, and levels increase as body condition score (BCS) increases.7-11
Inflammatory cytokines-Interleukin (IL)-1b, IL-6, IL-10, & tumor necrosis factor-a (TNFa): TNFa promotes inflammation and causes insulin resistance by blocking activation of insulin receptors.
Chemokines-IL-8 & monocyte chemotactic protein-1 (MCP-1): MCP-1 contributes to inflammation by attracting macrophages.
Acute phase proteins-haptoglobin, plasminogen activator inhibitor-1, & serum amyloid A:
Adiponectin, an antiinflammatory adipocyte hormone, is decreased in obese humans and dogs.12
Obesity-associated inflammation extends beyond adipose tissue. The liver is affected by fatty infiltration and adipose-derived inflammatory mediators that cause activation of inflammatory signaling pathways in the liver, including Kupffer cell activation. This activation helps further produce inflammatory mediators and recruit other immune cells, and may play a role in hepatic insulin resistance.13
Persistent, low-grade inflammation and increased oxidative stress secondary to obesity may also play a role in many chronic diseases, such as osteoarthritis and diabetes mellitus.
Signs
History. The owner should provide a thorough diet history: quantity and frequency of feeding of all pet foods, snacks, treats, and human foods.
Physical Examination. Body weight and BCS should be recorded at each visit. Abnormalities on physical examination can vary-common findings include joint pain, lameness, and exercise intolerance.
Diagnosis
Definitive Diagnosis
Body weight plus BCS provide an efficient and effective way to diagnose obesity. Two BCS systems are available:
5-point scale (1 = very thin; 3 = ideal; 5 = obese)
9-point scale (1 = very thin; 4-5 = ideal; 9 = obese)
Both systems use the same variables to assess BCS:
Ribs should be easily felt (slight fat cover); individual ribs are not visible.
Overhead view should show a well-proportioned lumbar waist.
Side view should show abdominal tuck in front of the hind legs.
Tail base should have a smooth contour; bones should be felt under a thin layer of fat.
Laboratory Findings
Obese dogs should be screened for hypothyroidism before starting a weight loss program, even those without obvious clinical signs. Other tests may be warranted on the basis of clinical signs.
Treatment
Obesity management programs should have 2 goals:
Short-term: Lose weight and reach ideal BCS
Long-term: Maintain ideal BCS once the weight loss program is completed.
A traditional obesity management program consists of caloric restriction in combination with exercise.
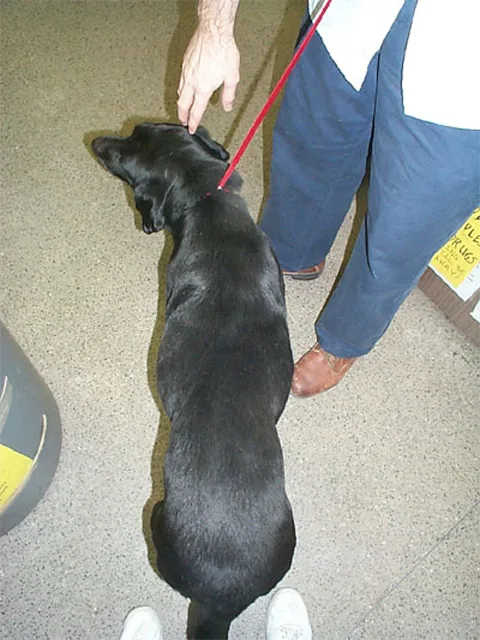
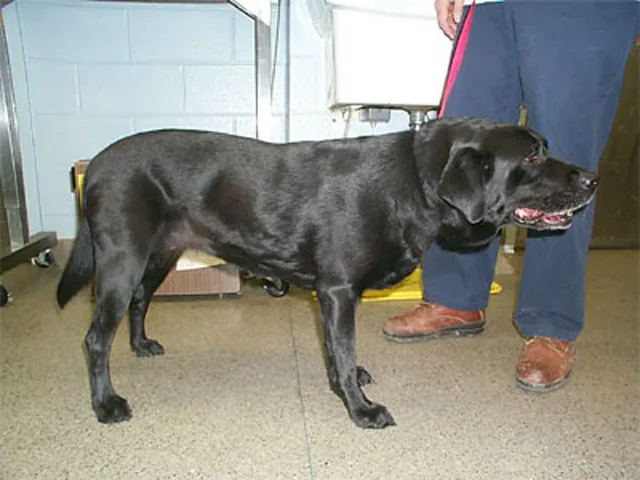
Step 1: Acknowledge that obesity is present. On physical examination, Eppie weighs 96.5 lb (43.4 kg) and has a body condition score (BCS) of 8 (based on 9-point scale) (Figures 1 and 2). The rest of the physical examination is unremarkable.


Eppie at the beginning of her weight loss program. She weighed 96.5 pounds, and BCS was 8/9.
Step 2: Obtain thorough diet history from owner (see Signs). Eppie has been consuming a “light” commercial dry dog food for the past year, but has continued to gain weight. Her owner is uncertain about the exact quantity of food she is feeding. Eppie also receives dog treats, but they are not given consistently every day.
Step 3: Form a partnership with the owner. Success of a weight loss program largely depends on the client's acceptance of the need for weight loss and willingness to perform the tasks necessary to achieve it. Lifestyle changes are necessary; however, keep in mind the importance of maintaining the owner-animal bond with any change in lifestyle.
Step 4: Correct and control any underlying diseases. Eppie is screened for hypothyroidism and results are within the reference range.
Step 5: Induce a negative energy balance. The most effective way to do this is to combine energy restriction with exercise. Exercise is many times a forgotten component of a weight loss program; however, the beneficial effects on metabolic rate make it critical. Because it is difficult for the owner to increase the amount of Eppie’s exercise, the Canine Club at the University of Georgia College of Veterinary Medicine arranges a schedule to walk Eppie regularly.
Step 6: Calculate caloric requirements. Two methods can be used to calculate a starting point for caloric intake:
Method 1
1 x resting energy requirement (RER):
RER = 70 (body weightkg0.75)*
Method 2
Multiply maintenance energy requirements (MER) by 0.6 (60%):
MER = 1.6 x RER
OM = 60% (MER)
Although both methods give slightly different kcal/day, this difference is clinically insignificant. Initial caloric calculations are only starting points; they may need to be modified according to an individual dog's response.
Step 7: Choose an appropriate diet for weight loss. Most pet food companies that make therapeutic diets also make a diet intended for weight loss programs (Table). Avoid starvation diets.
Starvation diets restrict not just calories but also every nutrient. Dogs, like humans, have daily requirements for certain nutrients, and starvation fails to provide these nutrients. In addition, starvation decreases intestinal mass and surface area, which can interfere with absorption of nutrients and increase the risk for bacterial translocation.
Net weight loss with starvation programs is roughly equivalent to that with restricted caloric intake, but it comes at a much higher cost to the patient.
Starvation is considered inhumane by most clients and veterinarians, and destroys the client-veterinarian partnership needed for successful weight loss. If clients do not feel good about the weight loss program, they may refuse to participate or discontinue it prematurely.
Short- and long-term successes are important components of a weight loss program. Starvation does not provide the owner with the tools to modify lifestyle on a long-term basis.

Step 8: Divide total daily caloric intake into 2 meals. Meal size and frequency influence postprandial thermogenesis in dogs.14 Thermogenesis is increased by feeding multiple small meals rather than 1 large meal (ie, it takes calories to digest food). Two smaller meals may provide better satiety than 1 large meal.
Step 9: Allow treats (this is part of the human-animal bond). Provide low-calorie treat options (Table) and limit the amount of treats to <10% of the dog's total calorie intake.
Step 10: Decide on a rate of weight loss. Because of lack of uniform sizes of dogs, it is better to recommend a percentage loss of body weight per week than a standard quantity for all dogs. A weight loss rate of 1% of body weight per week is safe.
Step 11: Weigh the dog at least once every 2 weeks. This frequency allows early detection of weight loss slowing or plateauing. It also prevents the owner from investing time and money in a program that is not working. Frequent weight checks provide an opportunity to celebrate successes with owners and motivate them to continue with the program.
Outcome—Were the goals achieved?Eppie achieved the short-term goal of losing weight to reach an ideal BCS. She also achieved the long-term goal of maintaining an ideal BCS for over 2.5 years (Figures 3 and 4)
Eppie 2.5 years after starting her weight loss program. She weighs 63.7 pounds, and BCS is 5/9.
Lack of owner compliance is the single most important factor in the failure of weight loss programs.15
Owner frustration with lack of results can cause dissatisfaction with the program and decreased motivation to continue.
Some owners have experience with an unsuccessful weight loss program and are unwilling to try the same approach again.
Other owners feel guilty about restricting caloric intake in their dog and find adherence difficult.
Some dogs develop undesirable behaviors, such as stealing food or getting into the garbage, when calories are restricted.
Pharmacologic Approach
Dirlotapide (Slentrol)
This selective intestinal microsomal triglyceride protein inhibitor works primarily by blocking the assembly and release of some chylomicrons from intestinal epithelial cells into the lymphatics. This results in the release of chemical mediators (peptide YY and glucagon-like peptide-1) that act as potent appetite suppressants by stimulating the satiety center in the hypothalamus. This effect accounts for about 90% of the action of this drug.
The remaining 10% of the drug's effect is due to excretion of trapped triglycerides in the intestinal epithelial cells when the cells are sloughed. Fat is broken down normally in the gastrointestinal tract and undergoes normal absorption into the enterocytes.
Dirlotapide comes in a liquid form that is administered orally Q 24 H. The drug has a neutral flavor and is generally well accepted by dogs. It is effective with most complete and balanced diets.
The most commonly reported side effects with dirlotapide are vomiting, diarrhea, and lethargy. Mild to moderate elevations in alanine and aspartate aminotransferase occur in some dogs, but levels usually return to normal after discontinuation of drug therapy.
Dirlotapide is contraindicated in:
All cats
Dogs with liver disease
Dogs receiving long-term corticosteroid therapy.
The safety of dirlotapide in dogs has been evaluated for 1 year.
In General
Relative Cost
Costs varies depending on the size of the dog.
Yearly costs of a traditional or pharmacologic weight loss program are ~$, which is considerably lower than cost of surgery to repair a torn ligament ($$$).
Costs will increase if underwater treadmill sessions are indicated.