Canine Interdigital Follicular Cysts
Darren Berger, DVM, DACVD, Iowa State University
You have asked...
What do I need to know about diagnosing and treating interdigital follicular cysts on my canine patients?
The expert says…
Pododermatitis is a generic term to describe inflammatory conditions that afflict dogs’ paws and is a common reason to seek a veterinarian’s opinion. A number of different conditions are known to cause canine pododermatitis (see Medical Conditions Associated with Pododermatitis in Dogs).1,2 Although pododermatitis in many of these conditions represents a clinical manifestation of a more extensive disease, some dogs have lesions confined strictly to their paws. Interdigital follicular cysts are a common reason for a dog to be presented with lesions confined only to the feet. The condition is often mistaken for foreign body or nonresolving pyoderma and can be a source of frustration for owners and veterinarians.
Medical Conditions Associated with Pododermatitis in Dogs
Acral lick dermatitis
Atopic dermatitis or cutaneous adverse food reaction
Demodicosis
Deep pyoderma
Deep or systemic mycoses (eg, phaeohyphomycosis, blastomycosis) Malassezia dermatitis
Dermatophytosis
Hepatocutaneous syndrome
Hookworm dermatitis
Idiopathic hyperkeratosis
Interdigital follicular cysts
Leishmaniasis
Neoplasia (eg, squamous cell carcinoma)
Pemphigus complex
Systemic lupus erythematosus
Vasculitis
Zinc-responsive dermatosis
Clinical Signs
Interdigital cysts sometimes present as noticeable dorsal lesions accompanied by licking, chewing, or lameness, while in other cases, the condition is perceived by owners as simply a cosmetic flaw. Lesions are usually first noted in young adult dogs (1-3 years of conformational age) and appear to be more common in American Staffordshire terriers and bull terriers, retrievers, and dogs with conformation deformities.3,4 At physical examination, dorsal interdigital erythema, swelling, nodules, hemorrhagic bullae, or draining tracts are seen (Figure 1). The dorsal interdigital lesion directly corresponds to an area of alopecia, erythema, edema, and comedone formation on the ventral palmar or plantar surface skin between the digital and metacarpal and tarsal pads. Interdigital follicular cysts most often occur on the front paws between the fourth and fifth interdigital space.5 However, lesions may occur anywhere, affect more than 1 interdigital space, or occur symmetrically depending on the underlying conformational disturbance.

FIGURE 1 Swelling and hemorrhagic bullae formation in the dorsal interdigital space commonly encountered with cases of interdigital follicular cysts. Image courtesy of J.O. Noxon, DVM, DACVIM, Iowa State University
Interdigital Follicular Cysts: What Are They & Why Do They Occur?
The current understanding is that interdigital follicular cysts form secondarily to abnormal friction or trauma to the ventral interdigital webbing associated with congenital (varus or valgus deformity) or acquired anatomic deformities.4,5 The abnormal friction or wear creates thickened, edematous, or callus-like changes to the interdigital skin, which results in plugging of follicular openings and comedone formation. Keratin production within the plugged follicular lumen persists and results in follicular dilation and cyst formation.5 Further complicating the issue, dogs have compound hair follicles (multiple hair shafts arising from 1 opening), so a single plugged follicular opening can result in multiple cysts. As a result, follicular cysts may be present in multiple layers of the ventral interdigital skin, and each is prone to rupture. Follicular rupture results in keratin, hair, and bacteria being released into the dermal space, which incites a pyogranulomatous foreign body (eg, broken hair shaft) reaction along with secondary deep pyoderma. Concurrent deep pyoderma and foreign body reaction leads to incomplete resolution of lesions with antimicrobial therapy alone; inflammation re-occurs quickly once glucocorticoid therapy is discontinued. Repeated rupture of the follicular cysts results in fistulous tract formation, which drains into the dorsal interdigital space. The presence of this dorsal clinical lesion commonly results in the misinterpretation that these lesions originate at this site.5
Diagnosis
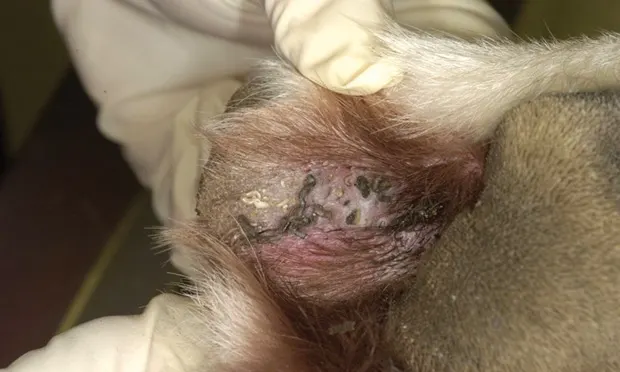
Interdigital follicular cysts are usually diagnosed based on clinical presentation and physical examination findings. In addition, a dermatologic minimum database (cytology, skin scrapes, and trichogram) should be performed to eliminate other primary or confounding causes of the patient’s clinical presentation. To help support a diagnosis, dorsal surface or ventral skin may be pressed or squeezed, which may result in white-to-gray keratin material being extruded from the small cysts that have formed (Figure 2). Exercise caution when attempting this in a nonsedated patient as it normally elicits a pain response.4 Biopsy with histopathology can be used to help confirm a diagnosis of interdigital follicular cysts in difficult or confusing cases. Biopsies need to be obtained from the ventral palmar or plantar surfaces because this is where interdigital follicular cysts originate.

FIGURE 2 Corresponding palmar surface to the lesions shown in Figure 1, showing extruded white-to-gray colored keratin material from follicular cysts following pressure applied to the dorsal surface. Image courtesy of J.O. Noxon, DVM, DACVIM, Iowa State University
Treatment
Addressing lesions surgically is preferred at this time.4,5 Partial or total fusion podoplasty has been previously described as a treatment method for chronic, nonresolving interdigital dermatitis but should only be considered a salvage procedure.6 Concerns with this type of surgical management are postsurgical complications such as dehiscence, lameness, or, specifically with partial podoplasty, an alteration to conformation and development of new lesions at a different interdigital site.
Surgical Ablation
The preferred treatment method for interdigital follicular cysts is surgical ablation with a CO2 laser. The method for performing this procedure is well-documented and results in roughly a 70% first-time success rate.4,5,7 It is recommended that those not familiar with or trained to perform this procedure refer cases to individuals who have experience in this area, as clinical success is dependent on skill level. Following surgical ablation, the treated area is allowed to heal via second intention (Figure 3). Postsurgical care consists of systemic and topical antimicrobials, nonsteroidal anti-inflammatory drugs, exercise restriction, and frequent bandage changes (every 2-3 days for the first 2 weeks, followed by weekly bandage changes for the next month). Recurrence is not uncommon and repeat procedures may be needed to permanently address the condition.

FIGURE 3 Patient several weeks postoperatively demonstrating second intention healing following surgical ablation with a CO2 laser. Image courtesy of J.O. Noxon, DVM, DACVIM, Iowa State University
Medical Management
Medical management can be attempted in cases of early lesion development or when surgical intervention is not an option. In cases of interdigital follicular cysts, products (eg, gels, lotions, wipes) containing benzoyl peroxide or salicylic acid may be beneficial because of their follicular flushing and keratolytic properties. Products should be used daily to every other day to break down and prevent comedone formation. Additionally, antimicrobial and glucocorticoid therapy may be beneficial in resolving secondary infections and inflammation associated with ruptured cysts, but neither will resolve the condition or prevent further episodes. Overall, medical therapy tends to be of limited effectiveness in most cases and is unlikely to be beneficial in chronic relapsing cases where scarring has occurred.