Anemia in a Cat
Kimberly Caruso, DVM, Antech Diagnostics, Irvine, CA
A 7-year-old, male, neutered Himalayan cat (Figure 1) presented to the emergency clinic for generalized lethargy noticed by the owner for the past few days. The animal is an indoor cat and lives with two other indoor cats. It had no previous medical history and vaccinations were not up-to-date. Vital signs included temperature 97.7ºF, heart rate 152 beats/min, and respiratory rate 40 breaths/min. Physical examination revealed a quiet, weak but alert cat. The patient was obviously tachypneic, with rapid, shallow breathing. Auscultation of the thorax revealed nothing noteworthy. Mucous membranes were a very pale pink. Blood was drawn for a CBC, and the results are presented in the accompanying table. A concurrent blood smear is shown as Figure 2. The results of whole-blood ELISA for FeLV and FIV were negative.
Table

FIGURE 1
Ask Yourself ...
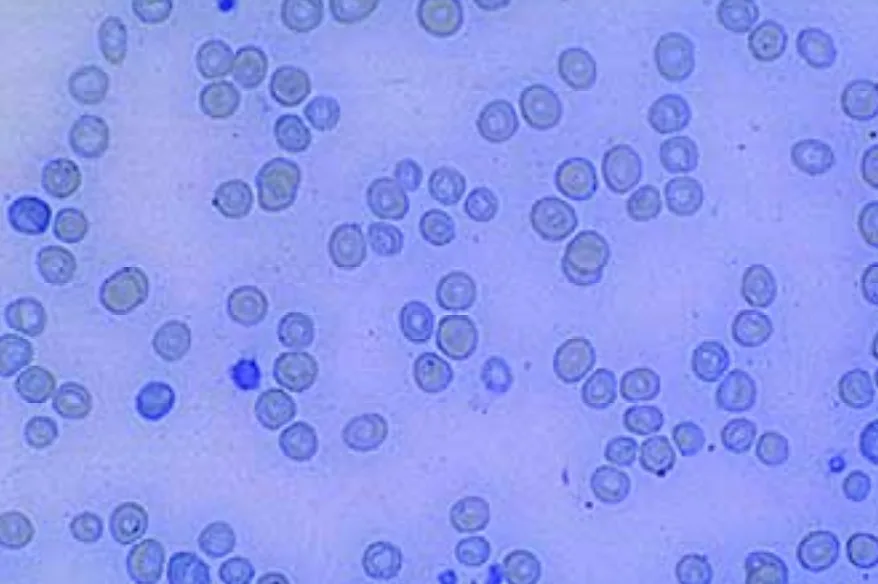
What morphologic changes are depicted on the blood smear?
What type of anemia is present?
What is the cause of the anemia? Is it acute or chronic?
What is the mainstay of treatment?
Diagnosis
Iron-deficiency anemia secondary to external parasitism
Cytologic evaluation
Microcytic hypochromic red blood cell indices are the hallmark of iron-deficiency anemia caused by iron depletion. Iron is necessary for hemoglobin synthesis. The amount of hemoglobin in the red blood cell is what signals for the turn-off of cell division. Without iron, hemoglobin cannot reach its maximal concentration within the blood cells. They continue to divide and become microcytic. With decreased hemoglobin production due to the lack of iron, red blood cells also become hypochromic (i.e., appear pale with a prominent central pallor). Anemia is regenerative in early iron deficiency, but as iron deficiency progresses into iron depletion, it becomes nonregenerative due to lack of iron for erythropoiesis (i.e., inadequate production).
Foundation
The most common cause of iron-deficiency anemia is chronic blood loss. It can also occur in young nursing animals because milk has a low percentage of iron. Some examples of chronic blood loss include internal and external parasitism, intestinal neoplasms, bladder neoplasms, gastrointestinal ulceration, and excessive removal of blood from blood donors. Further examination of the cat in this case revealed abundant flea dirt in the haircoat as well as numerous fleas. On further questioning, the owner reported a persistent flea problem for the past 2 months. Iron-deficiency anemia secondary to external parasitism with resultant chronic blood loss was diagnosed.
Treatment
The mainstay of treatment is to eliminate the source of blood loss and give the animal supplemental iron. A transfusion is indicated if anemia is severe. Typically, iron supplementation is continued until the HCT and MCV increase to levels within the normal reference ranges. The HCT is likely to return to normal more quickly than the MCV. The cat in this case was started on a flea control and oral iron supplementation program as well as being given a whole blood transfusion. It responded well and was discharged to the care of the regular veterinarian the next day.
Did You Answer ...
• Moderate anisocytosis (variation in red blood cell size) and minimal polychromasia. Many of the red blood cells are microcytic (smaller than normal) and hypochromic (increased central pallor/narrowing of the red-staining zone due to decreased hemoglobin content). Feline red blood cells normally have a minimal degree of central pallor.• Microcytic (decreased MCV), hypochromic (decreased MCHC), nonregenerative anemia (normal reticulocyte count, absence of polychromasia). Red blood cell distribution width is a measurement of variation in red blood cell size; and in this case, the increased width resulted primarily from the admixture of normocytes and microcytes. Cell distribution width is considered a better indicator of variation in red blood cell size than MCV.• Chronic iron deficiency is the cause. This type of anemia is most often associated with chronic blood loss-in this case, from long-term flea infestation.• Treatment involves eliminating the source of blood loss and giving supplemental iron and, if the anemia is severe, a transfusion.